
When your doctor first mentions pregabalin — or its brand name, Lyrica — you might feel a mix of hope and hesitation. I remember sitting in my neurologist's office years ago, listening to him explain yet another medication option for my neuropathy pain. By that point, I'd already tried several treatments with mixed results, so I understand the questions racing through your mind: Will this actually work? What will the side effects be like? How long before I notice a difference?
Pregabalin has become one of the most widely prescribed medications for neuropathic pain, and for good reason — it has a strong track record backed by clinical research. But like any medication, it's not a one-size-fits-all solution. In this guide, I'll walk you through everything I've learned about pregabalin for neuropathy — the benefits, the side effects, the realistic timeline, and the practical tips that can make a real difference in your experience with it.
Key Takeaway
Pregabalin (Lyrica) is one of the most well-studied medications for neuropathic pain. It calms overexcited nerve signals rather than masking pain, and may also improve sleep and reduce anxiety. Most people notice some benefit within 1-2 weeks, with full effects developing over 2-4 weeks as the dose is gradually adjusted.
What Is Pregabalin and How Does It Work for Neuropathy?
Pregabalin belongs to a class of medications called gabapentinoids. It was the first medication to receive FDA approval specifically for treating diabetic peripheral neuropathy and postherpetic neuralgia (nerve pain after shingles). It's also approved for fibromyalgia and as an add-on treatment for certain types of seizures.
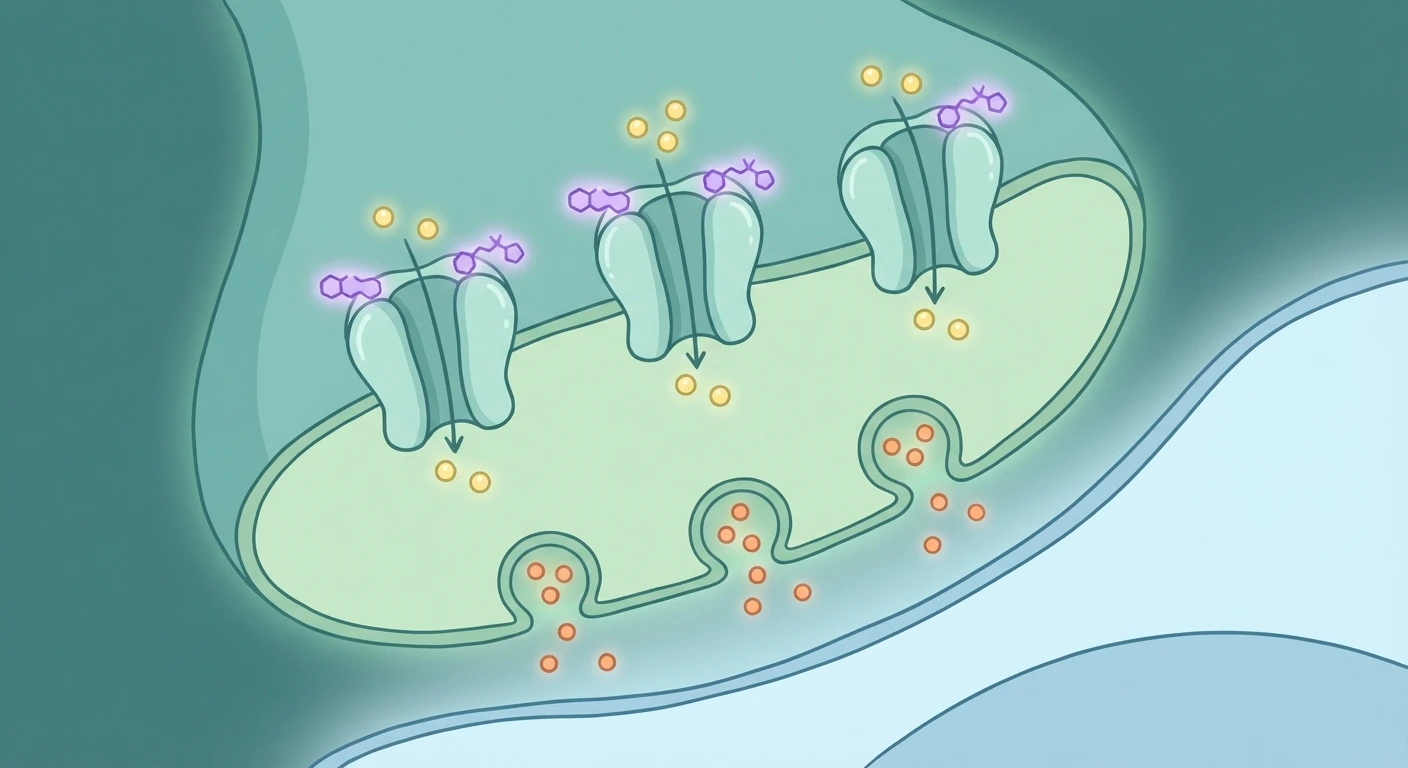
Here's what makes pregabalin interesting from a nerve pain perspective: it doesn't work the way traditional painkillers do. Instead of blocking pain at the site of injury, pregabalin works in your central nervous system. It binds to what scientists call the alpha-2-delta subunit of voltage-gated calcium channels in your brain and spinal cord. In simpler terms, it reduces the release of certain chemical messengers (neurotransmitters like glutamate, norepinephrine, and substance P) that overexcited nerves use to send pain signals.
Think of it this way: when you have neuropathy, your damaged nerves are essentially firing off pain signals when they shouldn't be — like a car alarm that goes off every time a breeze hits it. Pregabalin helps calm down that overactivity without completely numbing you. It turns down the volume on those misfiring signals, which is why many people find it helpful for the burning, shooting, and tingling sensations that come with different stages of neuropathy.
What the Research Says About Pregabalin's Effectiveness
One thing I appreciate about pregabalin is that there's a substantial body of clinical research behind it — far more than exists for many other neuropathy treatments. A major Cochrane review (the gold standard of medical evidence summaries) found that pregabalin at doses of 300 mg and 600 mg daily provides meaningful pain relief for a significant number of people with neuropathic pain conditions.
The numbers tell an encouraging story. In clinical trials for diabetic peripheral neuropathy, approximately 30-50% of patients treated with pregabalin achieved at least a 50% reduction in their pain — compared to about 20-30% of those taking a placebo. That might not sound dramatic at first, but a 50% pain reduction can be life-changing when you've been dealing with constant burning or stabbing pain in your feet.
A 2024 meta-analysis published in Frontiers in Pain Research compared pregabalin head-to-head with its older cousin, gabapentin. Both were found effective for neuropathic pain, but pregabalin showed some advantages: it had more predictable absorption (meaning doses are more consistent in their effects), and patients reported somewhat fewer episodes of nausea and vomiting compared to gabapentin.
Research has also shown that pregabalin may help with the sleep disruption that so many of us with neuropathy struggle with. When your neuropathy gets worse at night, the combination of pain relief and mild sedation from pregabalin can be genuinely helpful. Several studies noted improved sleep scores as a secondary benefit alongside pain reduction.
Benefits Beyond Pain Relief
While pain reduction is the primary reason doctors prescribe pregabalin for neuropathy, many people notice additional benefits that improve their overall quality of life:
Improved sleep quality. Neuropathy pain has a cruel habit of intensifying at night, right when you're trying to rest. Pregabalin's calming effect on nerve activity may help many people fall asleep more easily and stay asleep longer. In clinical trials, patients consistently reported better sleep scores, and some doctors intentionally prescribe the larger dose at bedtime to take advantage of this.
Reduced anxiety. Pregabalin is actually approved in some countries (though not the United States) for generalized anxiety disorder. Living with chronic neuropathy pain can understandably create or worsen anxiety, so this secondary benefit can be meaningful. Many people in support groups mention feeling generally calmer after starting pregabalin.
Relatively quick onset. Unlike some medications that take weeks to build up in your system, many people notice some improvement with pregabalin within the first week or two. Full benefits typically develop over 2-4 weeks as the dose is adjusted, but that initial glimmer of relief can be incredibly encouraging when you've been suffering.
Flexible dosing. Pregabalin comes in a range of capsule strengths (25 mg, 50 mg, 75 mg, 100 mg, 150 mg, 200 mg, and 300 mg), which allows for gradual dose adjustment. Your doctor can fine-tune your dose to find the sweet spot where you get the most benefit with the fewest side effects.
Understanding the Dosing Process
Getting the right dose of pregabalin is more of a journey than a destination — and understanding this process upfront can save you a lot of frustration. Here's what a typical dosing path looks like:
Starting dose: Most doctors begin with a low dose, typically 75 mg taken twice daily (150 mg total per day) or sometimes even lower at 25-50 mg at bedtime. Starting low helps your body adjust to the medication and minimizes early side effects like dizziness and drowsiness.
Titration phase: Based on how you respond, your doctor will gradually increase the dose over 1-2 weeks. The target therapeutic dose for diabetic neuropathy is usually 300 mg per day (100 mg three times daily), though some people do well at lower doses and others may need up to 600 mg per day.
Maintenance dose: Once you and your doctor find the dose that works, you'll typically stay at that level. The FDA-approved dosing range for diabetic neuropathy is 150 mg to 300 mg per day, divided into two or three doses.
An important note from the research: many patients are prescribed doses that are actually too low to be fully effective. A study published in the Postgraduate Medical Journal found that reluctance to increase the dose — often due to early side effects that would resolve — is one of the most common reasons patients don't get adequate relief from pregabalin. If you've been on a low dose for weeks without much improvement, it may be worth having a conversation with your doctor about careful dose adjustment rather than abandoning the medication.
of patients in clinical trials achieved at least 50% pain reduction with pregabalin
Common Side Effects: What to Realistically Expect
Let me be straightforward with you about side effects, because I think honesty serves you better than sugar-coating. Pregabalin does cause side effects in many people, especially during the first few weeks. The good news is that most side effects are manageable and tend to improve as your body adjusts.
Dizziness and drowsiness are the most commonly reported side effects, affecting roughly 20-30% of patients in clinical trials. These tend to be most noticeable in the first week and typically improve significantly by weeks 2-4. Many people find that taking the larger portion of their dose at bedtime helps manage this.
Weight gain is a concern for many people and affects approximately 5-15% of patients. The average weight gain in clinical trials was relatively modest (about 2-3 kg over several months), but it varies considerably. If you're watching your weight, working with your doctor on dietary strategies from the start — and maintaining the neuropathy-friendly diet habits we discuss elsewhere — can help minimize this.
Peripheral edema (swelling) in the feet and lower legs affects about 5-10% of patients. This is particularly worth monitoring if you already have circulation concerns. Mild ankle swelling doesn't necessarily mean you need to stop the medication, but it should be discussed with your doctor.
Dry mouth is reported by some patients. Staying well-hydrated and keeping water nearby can help manage this.
Blurred vision occurs in a small percentage of patients and is usually temporary. If it persists beyond the first couple of weeks, let your doctor know.
Cognitive effects — sometimes described as “brain fog,” difficulty concentrating, or feeling “fuzzy” — may affect some people, particularly at higher doses. In my experience talking with others in support groups, this side effect is very individual. Some people notice nothing, while others find it significant. Starting at a low dose and increasing gradually gives you the best chance of avoiding this.

Talk to Your Doctor
Never stop pregabalin abruptly. Sudden discontinuation can cause withdrawal symptoms including insomnia, nausea, headache, and in rare cases, seizures. Always work with your healthcare provider to create a gradual tapering plan if you need to stop the medication.
Serious Side Effects and Safety Considerations
While most side effects are mild and manageable, there are some important safety considerations to discuss with your healthcare provider:
Dependence and withdrawal: Pregabalin should never be stopped abruptly. Stopping suddenly can cause withdrawal symptoms including insomnia, nausea, headache, anxiety, and in rare cases, seizures. Your doctor will create a tapering schedule if you need to discontinue the medication — typically reducing the dose gradually over at least one week.
Suicidal thoughts: Like all anti-seizure medications, pregabalin carries an FDA boxed warning about a small increased risk of suicidal thoughts or behavior. While this risk is considered low, it's important to be aware of it and to tell your doctor immediately if you notice changes in your mood or thoughts.
Breathing concerns: In 2019, the FDA added a warning about the risk of respiratory depression when pregabalin is combined with opioids or other central nervous system depressants. If you take any opioid medications, sedatives, or anti-anxiety drugs, make sure your doctor knows before starting pregabalin.
Kidney function: Pregabalin is processed through the kidneys, so people with reduced kidney function need lower doses. Your doctor may check your kidney function before prescribing and adjust the dose accordingly.
Driving and operating machinery: Until you know how pregabalin affects you, be cautious about driving. The dizziness and drowsiness, especially in the first few weeks, can impair your ability to react quickly.
Pregabalin vs. Gabapentin: How Do They Compare?
This is one of the most common questions I hear from people in neuropathy support communities. Gabapentin (Neurontin) and pregabalin (Lyrica) are related medications that work similarly, but there are meaningful differences:
Absorption predictability. Pregabalin is absorbed more consistently than gabapentin. Gabapentin's absorption actually decreases as the dose increases (saturated absorption), meaning you don't always get a proportional increase in effect when you increase the dose. Pregabalin doesn't have this issue — its absorption is linear and predictable regardless of dose.
Dosing frequency. Pregabalin is typically taken two to three times daily, while gabapentin is usually taken three times daily. This might not seem like a big difference, but for those of us managing multiple medications, one fewer dose per day can simplify things.
Onset of action. Pregabalin may work slightly faster than gabapentin due to its more reliable absorption. Some studies suggest meaningful relief within the first week.
Cost. Generic pregabalin has become more affordable since Lyrica's patent expired, but gabapentin generics are still generally less expensive. If cost is a significant factor, this is worth discussing with your doctor and pharmacist.
Potency. Pregabalin is considered 2-3 times more potent than gabapentin on a milligram-for-milligram basis. A typical effective dose of pregabalin (300 mg/day) provides similar relief to gabapentin at higher doses (900-1800 mg/day).
The 2024 meta-analysis mentioned earlier found no overwhelming winner in head-to-head comparisons — both medications are considered first-line treatments for neuropathic pain. The choice often comes down to individual response, side effect tolerance, cost considerations, and your doctor's clinical experience. If you're interested in how various supplements for nerve health might complement your medication, that's another conversation worth having with your provider.
Practical Tips for Starting Pregabalin

After years of talking with others who have navigated the pregabalin experience, here are the practical tips that come up most often:
Start on a weekend or quiet day. The drowsiness and dizziness are typically worst in the first few days. If possible, time your first dose for a day when you don't need to drive or be at peak performance.
Take it with food. While pregabalin can be taken with or without food, taking it with a meal may slow absorption slightly and reduce the intensity of initial side effects.
Keep a symptom diary. Track your pain levels, sleep quality, side effects, and doses each day for the first month. This gives you and your doctor real data to work with when deciding about dose adjustments. A simple 1-10 pain scale jotted down morning and evening is enough.
Be patient with titration. It's tempting to want immediate results, but the gradual dose increase is there to protect you. Jumping to a higher dose too quickly almost always means worse side effects. Trust the process.
Set consistent times. Taking pregabalin at the same times each day helps maintain steady levels in your blood, which gives you more consistent relief. Setting phone alarms for your dose times can help establish the habit.
Don't give up too early. Research shows many patients abandon pregabalin before reaching an adequate dose. If you're tolerating it reasonably well but not getting enough relief, talk to your doctor about increasing the dose rather than stopping.
Stay active. Gentle exercises for neuropathy can complement pregabalin's effects. Movement helps maintain nerve function and may enhance the medication's benefit.
Who Is Pregabalin Best Suited For?
While pregabalin can be helpful for many types of neuropathic pain, research and clinical experience suggest it may be particularly well-suited for:
Diabetic peripheral neuropathy. This is the condition pregabalin was first approved for, and the evidence base is strongest here. If diabetes is the underlying cause of your neuropathy, pregabalin has solid research supporting its use.
Postherpetic neuralgia. The burning, stabbing pain that can persist after a shingles outbreak responds particularly well to pregabalin in clinical trials.
People who haven't responded well to gabapentin. Because of pregabalin's more predictable absorption, some people who didn't get adequate relief from gabapentin do better on pregabalin. It's not guaranteed, but it's a reasonable next step.
Those with significant sleep disruption. If nighttime neuropathy pain is your biggest challenge, pregabalin's combined effect on pain and sleep can be especially valuable.
People who benefit from anxiolytic effects. If anxiety accompanies your chronic pain (which is very common), pregabalin's calming properties may provide dual benefit.
When Pregabalin Might Not Be the Best Fit
Pregabalin isn't ideal for everyone. Your doctor might consider alternatives if you:
Have significant kidney impairment (doses need careful adjustment, and some kidney conditions make it impractical). Are taking opioid medications (the respiratory risk increases with combination use). Have a history of substance use disorder (pregabalin has some potential for misuse and is classified as a Schedule V controlled substance). Are concerned about weight gain and have diabetes or metabolic syndrome that makes weight management critical. Need to maintain peak cognitive performance for work or safety-sensitive activities.
In these situations, your doctor might recommend alternatives such as duloxetine (Cymbalta), topical treatments like neuropathy creams, or other approaches depending on your specific situation.
Combining Pregabalin with Other Treatments

Pregabalin is often most effective as part of a broader management approach rather than as the sole treatment. Many healthcare providers recommend combining it with:
Topical treatments. Using a nerve pain cream on your feet while taking pregabalin orally targets pain from both directions — locally and centrally. This combination is generally safe and can allow for lower oral doses.
Physical activity. Regular, gentle exercise has its own nerve-supporting benefits and may enhance pregabalin's effects. Walking programs, water therapy, and stretching routines all complement medication-based management.
Nutritional support. Addressing any nutritional deficiencies — especially B vitamins and alpha-lipoic acid — supports overall nerve health while pregabalin manages the pain signals. Making sure you're not dealing with any vitamin deficiency that could worsen neuropathy is a smart parallel strategy.
Stress management. Chronic pain and stress feed off each other. Mindfulness practices, gentle yoga, warm baths, or neuropathy foot soaks can complement your medication and improve your overall quality of life.
Frequently Asked Questions About Pregabalin for Neuropathy
The Bottom Line on Pregabalin for Neuropathy
Pregabalin is one of the best-studied medications for neuropathic pain, with solid evidence supporting its effectiveness for conditions like diabetic peripheral neuropathy and postherpetic neuralgia. It works differently from traditional painkillers by calming overactive nerve signals rather than masking pain, and it may offer additional benefits for sleep and anxiety.
Like any medication, it comes with trade-offs. Side effects are common in the first few weeks but usually manageable, and finding the right dose takes patience and communication with your healthcare provider. The key is to give it a fair trial — starting low, increasing gradually, and reaching an adequate therapeutic dose before deciding whether it works for you.
If you're considering pregabalin, have an open conversation with your doctor about your complete health picture, your other medications, and your goals for pain management. And remember — medication is usually most effective as one piece of a broader approach that includes staying active, supporting your nerves nutritionally, and managing stress. Whatever you decide with your healthcare team, know that you're not alone in navigating these choices.


