When most people hear the word “neuropathy,” they think of tingling feet, burning hands, and numbness — the classic sensory symptoms that affect the nerves you can feel. But there's a whole other side of neuropathy that doesn't get nearly enough attention, and it can be far more disruptive to daily life than numbness alone. It's called autonomic neuropathy, and it affects the nerves that control the things your body does automatically — your heart rate, blood pressure, digestion, sweating, bladder function, and more.
I've met many people in our neuropathy community who spent months or even years dealing with mysterious symptoms — constant dizziness when standing up, unexplained digestive problems, episodes of drenching sweats or an inability to sweat at all — before anyone connected these issues to their neuropathy. If that sounds familiar, this article is for you. Understanding autonomic neuropathy is the first step toward managing it, and there's more that can be done about it than many people realize.
What Is the Autonomic Nervous System?
To understand autonomic neuropathy, it helps to understand the system it damages. Your nervous system is divided into parts that you consciously control (like moving your arm) and parts that operate on autopilot. That autopilot portion is your autonomic nervous system, and it quietly manages an astonishing number of functions every second of every day.
The autonomic nervous system controls your heart rate and blood pressure, keeping them adjusted whether you're lying down, standing up, or climbing stairs. It manages your digestive tract — the muscular contractions that move food through your stomach and intestines. It regulates your body temperature through sweating and blood vessel dilation. It controls your bladder and bowel function. It manages pupil size in response to light. It even plays a role in sexual response.
Your autonomic nervous system has two branches that work in balance: the sympathetic nervous system (your “fight or flight” response that speeds things up) and the parasympathetic nervous system (your “rest and digest” response that slows things down). When autonomic neuropathy damages the nerves in either or both of these branches, the affected automatic functions start malfunctioning — and the symptoms can be confusing because they seem to come from so many different body systems at once.
If you've been following the stages of neuropathy as it progresses, autonomic involvement often represents a more advanced phase where the damage extends beyond sensory nerves into the nerves controlling your body's background operations.
Did You Know?
The autonomic nervous system controls your heart rate, blood pressure, digestion, sweating, bladder function, and more — all without you thinking about it. When these nerves are damaged, the symptoms can seem unrelated and are often misdiagnosed for months or years.
Causes of Autonomic Neuropathy
The most common cause of autonomic neuropathy is diabetes — particularly when blood sugar has been poorly controlled over a long period. Researchers estimate that up to 50% of people with diabetes will develop some degree of autonomic neuropathy over time, though many cases are mild and go undiagnosed. The high blood sugar damages the small nerve fibers that serve autonomic functions, similar to how it damages the sensory nerves in your feet and hands.
But diabetes is far from the only cause. Autonomic neuropathy can result from:
Autoimmune conditions. Conditions like Sjögren's syndrome, lupus, rheumatoid arthritis, and celiac disease can trigger immune attacks against autonomic nerve fibers. Guillain-Barré syndrome is an acute autoimmune condition that can severely affect autonomic function.
Infections. HIV, Lyme disease, hepatitis C, and certain other infections can damage autonomic nerves. COVID-19 has also been associated with new-onset autonomic dysfunction (dysautonomia) in some patients.
Medications and toxins. Certain chemotherapy drugs, particularly vincristine and cisplatin, can damage autonomic nerves. Heavy alcohol use over years can also cause autonomic neuropathy alongside the more visible peripheral nerve damage.
Amyloidosis. This condition, where abnormal proteins build up in organs and tissues, frequently affects autonomic nerves and can cause severe autonomic dysfunction.
Hereditary conditions. Some forms of hereditary neuropathy include an autonomic component, such as familial amyloid polyneuropathy and hereditary sensory and autonomic neuropathy (HSAN).
Neurodegenerative diseases. Parkinson's disease, multiple system atrophy, and Lewy body dementia all involve autonomic nerve dysfunction as part of the disease process.
Idiopathic. In some cases, no clear cause can be identified — a frustrating reality that many in our community understand all too well. If you're interested in understanding the full range of what can trigger nerve damage, including vitamin deficiencies that cause neuropathy, exploring every possible contributor is worthwhile.
of people with diabetes may develop some degree of autonomic neuropathy over time
Cardiovascular Symptoms: When Your Heart and Blood Pressure Misbehave
Cardiovascular autonomic neuropathy is one of the most significant forms because it can have serious health implications. The autonomic nerves that control your heart and blood vessels normally make constant, invisible adjustments — speeding up your heart when you exercise, slightly raising your blood pressure when you stand up from sitting. When these nerves are damaged, those automatic adjustments become unreliable.
Orthostatic hypotension — a sudden drop in blood pressure when you stand up — is perhaps the most recognizable cardiovascular symptom. You may feel dizzy, lightheaded, or faint when transitioning from sitting or lying down to standing. In severe cases, you might actually black out. This happens because your damaged autonomic nerves can't quickly tighten your blood vessels to compensate for gravity pulling blood toward your legs when you stand.
Resting heart rate changes. Autonomic neuropathy can cause a persistently fast resting heart rate (tachycardia), often around 90-100 beats per minute, because the parasympathetic nerves that normally help keep your heart rate down aren't functioning properly. Alternatively, some people develop an inability to increase their heart rate appropriately during exercise, leaving them feeling exhausted and breathless with minimal exertion.
Exercise intolerance. The inability to properly adjust heart rate and blood pressure during physical activity can make exercise feel disproportionately difficult. This doesn't mean you should avoid activity — in fact, gentle exercises for neuropathy remain important — but it does mean you should work with your healthcare provider to find the right type and intensity.
Silent heart attacks. This is a particularly concerning aspect of cardiovascular autonomic neuropathy. When the nerves carrying pain signals from the heart are damaged, a heart attack may not produce the classic chest pain symptoms. Instead, people may experience unusual fatigue, shortness of breath, or nausea. If you have autonomic neuropathy, your doctor should be aware of this risk and monitor your cardiovascular health proactively.

Talk to Your Doctor
Cardiovascular autonomic neuropathy may mask heart attack symptoms. If you have autonomic neuropathy and experience unexplained fatigue, shortness of breath, or nausea, seek medical attention promptly — these could be signs of a cardiac event without the typical chest pain.
Digestive Symptoms: Gastroparesis and Beyond
The digestive tract is heavily controlled by autonomic nerves, and autonomic neuropathy can disrupt virtually every aspect of digestion. These symptoms are often among the most quality-of-life-affecting because eating is such a fundamental part of daily life.
Gastroparesis (delayed stomach emptying) is one of the hallmark digestive complications. When the autonomic nerves controlling your stomach muscles are damaged, your stomach can't contract effectively to push food through to the small intestine. This leads to feeling full after eating only small amounts, nausea, vomiting (sometimes of food eaten hours or even a day earlier), bloating, and abdominal pain. For people with diabetes, gastroparesis creates an additional challenge: it makes blood sugar control unpredictable because you can't reliably time how quickly food will be absorbed.
Alternating constipation and diarrhea occur when the nerves controlling intestinal motility are affected. Some people develop chronic constipation because the intestines can't push contents through effectively. Others experience sudden episodes of diarrhea, particularly at night (nocturnal diarrhea), which can be socially distressing and sleep-disrupting. Some people cycle between both.
Swallowing difficulty (dysphagia) can occur when the autonomic nerves controlling the esophagus are affected, leading to a feeling of food getting stuck or difficulty coordinating the swallowing process.
If you're working on a neuropathy-supportive diet, autonomic digestive symptoms can make this more challenging. Small, frequent meals rather than large ones are generally better tolerated, and working with a gastroenterologist alongside your neurologist may be necessary.
Sweating Abnormalities: Too Much, Too Little, or Just Wrong
Sweating is controlled entirely by your autonomic nervous system, and when those nerves are damaged, things get complicated. Some people develop anhidrosis — a reduced ability to sweat in certain areas or throughout the body. This is more than a comfort issue; sweating is how your body regulates temperature, and an inability to sweat properly can lead to dangerous overheating, especially during exercise or in hot weather.
Others experience the opposite: excessive sweating (hyperhidrosis), particularly in areas that still have intact autonomic nerves. This often creates a pattern called compensatory sweating, where you sweat heavily from the face, head, and upper body while your lower body remains dry. Gustatory sweating — profuse facial sweating triggered by eating, even foods that aren't spicy — is another common and socially embarrassing symptom.
Some people experience both problems simultaneously in different body regions: unable to sweat from the waist down but drenching through their shirts from the upper body. This mixed pattern can be particularly confusing and is often not recognized as a neuropathy symptom.
Bladder and Urinary Symptoms
Autonomic neuropathy affecting the bladder can cause a range of urinary problems that significantly impact quality of life:
Difficulty sensing a full bladder. You may not feel the normal urge to urinate until your bladder is very full, leading to infrequent urination and bladder distension over time.
Incomplete bladder emptying. Weakened bladder muscles may not contract forcefully enough to empty completely, leaving residual urine that increases the risk of urinary tract infections — a common and recurrent problem for people with bladder neuropathy.
Overflow incontinence. When the bladder overfills because you can't sense fullness or empty completely, urine may leak without warning. This is understandably distressing and can lead to social isolation if not addressed.
Frequent urinary tract infections. The combination of retained urine and reduced sensation creates an environment where bacteria can thrive, leading to recurrent UTIs that may become more difficult to treat over time.
Sexual Dysfunction
Sexual function relies heavily on autonomic nerve signaling, and autonomic neuropathy can cause significant sexual dysfunction in both men and women. This is another area where many people suffer in silence because of the sensitive nature of these symptoms.
In men, autonomic neuropathy commonly causes erectile dysfunction — difficulty achieving or maintaining an erection sufficient for sexual activity. It can also cause retrograde ejaculation, where semen enters the bladder instead of exiting through the urethra. These issues affect an estimated 30-75% of men with diabetes who have autonomic neuropathy.
In women, autonomic neuropathy can cause vaginal dryness, decreased arousal, and difficulty reaching orgasm. These symptoms are often attributed to hormonal changes or aging rather than being correctly identified as neuropathy-related.
If you're experiencing sexual dysfunction alongside other neuropathy symptoms, please bring it up with your healthcare provider. These are medical symptoms, not personal failures, and there are treatments and strategies available.
Pupil and Vision Changes
Your pupils are controlled by autonomic nerves — they dilate in the dark to let in more light and constrict in bright conditions. When autonomic neuropathy affects these nerves, you may experience difficulty adapting to changes in lighting. Walking from a well-lit room into a darker hallway may temporarily leave you struggling to see, and oncoming headlights at night may seem unbearably bright. These changes are subtle but can affect your safety, particularly when driving at night.
Hypoglycemia Unawareness: A Hidden Danger for Diabetics
For people with diabetes, one of the most dangerous consequences of autonomic neuropathy is the loss of warning symptoms when blood sugar drops too low. Normally, your autonomic nervous system triggers sweating, shakiness, rapid heartbeat, and hunger when blood glucose falls — unmistakable signals that prompt you to eat something immediately. When autonomic neuropathy damages these pathways, a dangerous hypoglycemic episode can occur without any warning, potentially leading to confusion, loss of consciousness, seizures, or worse.
This is called hypoglycemia unawareness, and it's a serious safety concern that affects an estimated 25-40% of people with type 1 diabetes and a smaller but still significant percentage of those with type 2 diabetes who use insulin. If you have diabetes and autonomic neuropathy, talk to your doctor about adjusting your blood sugar targets and whether a continuous glucose monitor (CGM) might be appropriate to provide an external alert system that doesn't rely on your damaged nerves.
Getting Diagnosed: Tests for Autonomic Neuropathy
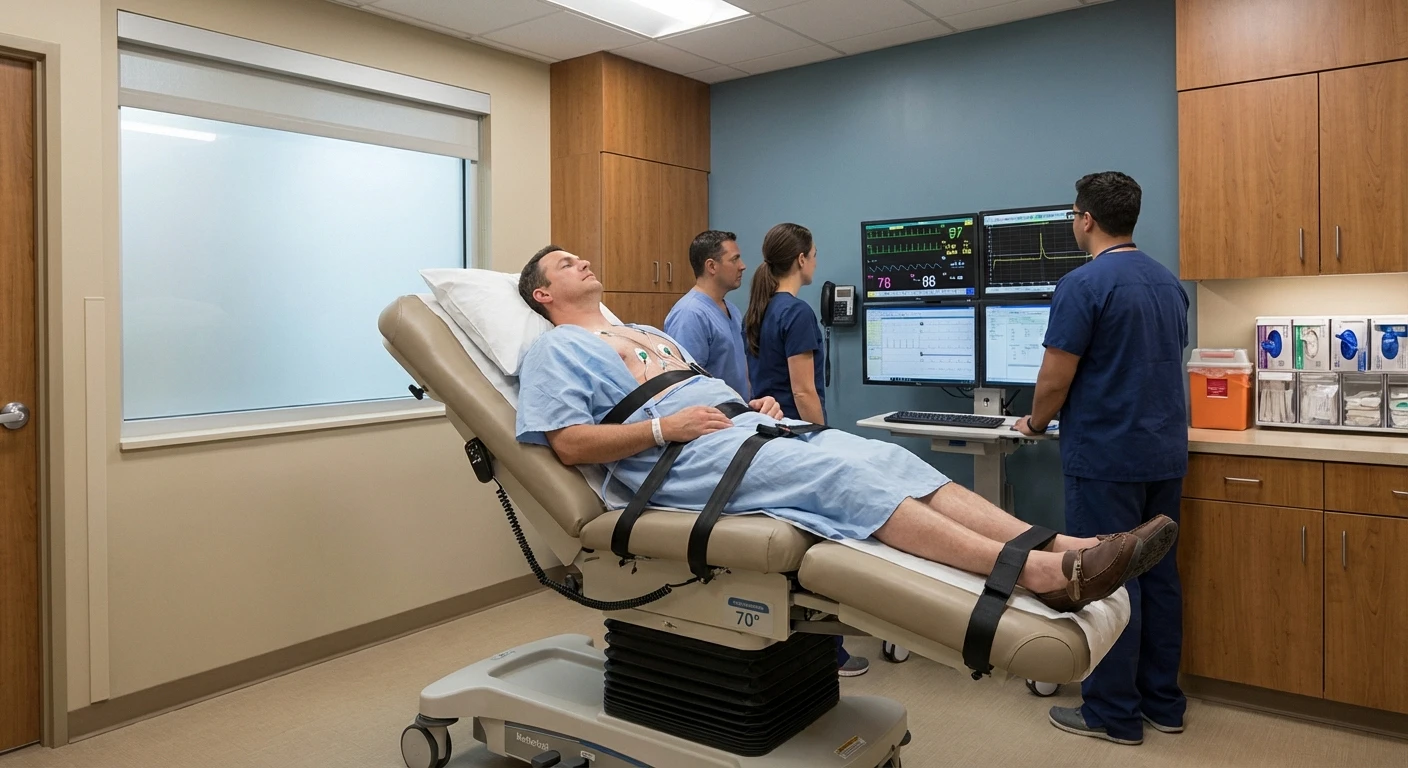
Diagnosing autonomic neuropathy requires specific tests that evaluate autonomic function directly — standard nerve conduction studies that diagnose peripheral neuropathy don't test autonomic nerves. Here are the key diagnostic tools your doctor may use:
Tilt table test. You lie on a table that slowly tilts you from horizontal to vertical while your heart rate and blood pressure are continuously monitored. This tests your cardiovascular autonomic function and can detect orthostatic hypotension and abnormal heart rate responses.
Quantitative sudomotor axon reflex test (QSART). This measures the nerve-controlled sweat response at specific body locations by applying a mild electrical stimulus and a chemical (acetylcholine) to the skin. Reduced or absent sweating in tested areas indicates autonomic nerve damage.
Thermoregulatory sweat test. You're placed in a warm chamber and coated with a powder that changes color when wet. This maps your entire body's sweating pattern and reveals areas where autonomic nerves are no longer triggering appropriate sweat production.
Heart rate variability testing. Your heart rate is monitored while you perform specific tasks like deep breathing and the Valsalva maneuver (bearing down). A healthy autonomic nervous system creates natural variations in heart rate during these activities — reduced variability suggests autonomic dysfunction.
Gastric emptying study. If gastroparesis is suspected, you eat a meal containing a small amount of radioactive material, and a scanner tracks how quickly the food leaves your stomach over several hours.
Bladder function tests (urodynamics). These measure how your bladder fills, stores, and empties urine, testing the autonomic nerve control of bladder function.
Treatment and Management Strategies
While there is no single medication that restores autonomic nerve function, many of the symptoms of autonomic neuropathy can be managed effectively — often dramatically improving quality of life. Treatment is typically symptom-specific:
For orthostatic hypotension: Standing up slowly (sit on the edge of the bed for a moment before standing), compression stockings to prevent blood pooling in the legs, increasing salt and fluid intake (with your doctor's approval), and medications like midodrine or fludrocortisone that help maintain blood pressure. Elevating the head of your bed by 4-6 inches can also help by reducing the blood pressure drop when you get up in the morning.
For gastroparesis: Eating smaller, more frequent meals. Choosing soft, low-fiber, low-fat foods that are easier to digest. Medications like metoclopramide or domperidone that help stimulate stomach contractions. In severe cases, dietary consultation with a specialist is essential to maintain adequate nutrition.
For bladder dysfunction: Timed voiding (urinating on a schedule rather than waiting for the urge), gentle abdominal pressure during urination, and in some cases, intermittent self-catheterization to ensure complete bladder emptying. Medications may help with specific bladder symptoms.
For sweating abnormalities: Glycopyrrolate or other anticholinergic medications for excessive sweating. For reduced sweating, avoiding overheating and staying in climate-controlled environments during extreme weather are practical strategies.
For sexual dysfunction: Phosphodiesterase inhibitors (like sildenafil) for erectile dysfunction. Vaginal lubricants and estrogen therapy for vaginal dryness. Open communication with both your healthcare provider and your partner is crucial.
Addressing the underlying cause is the most important long-term strategy. For diabetic autonomic neuropathy, strict blood sugar control can slow progression and may even partially reverse early damage. If an autoimmune condition is the cause, immunotherapy may help. If medications are contributing, your doctor may adjust them.
Supporting your overall nerve health through proper nutrition — including addressing any supplements that support nerve function — is a worthwhile complement to symptom-specific treatments.

Living with Autonomic Neuropathy: Daily Life Adjustments
Beyond medical treatment, several practical adjustments can make daily life significantly more manageable:
Carry water and salty snacks. Staying well-hydrated and maintaining adequate salt intake helps support blood pressure. Many people with autonomic neuropathy find that keeping electrolyte drinks or salty crackers available helps prevent dizziness episodes.
Dress in layers. If your temperature regulation is impaired, layers let you adjust quickly to prevent overheating or chilling. Moisture-wicking fabrics can help manage excessive sweating.
Plan your meals strategically. If you have gastroparesis, eat your larger meals earlier in the day when stomach motility tends to be better. Avoid lying down immediately after eating. Thoroughly chewing food and staying upright during and after meals can improve digestion.
Create bathroom routines. If bladder or bowel function is affected, establishing regular bathroom schedules (rather than waiting for urges that may not come) can prevent problems. Knowing where restrooms are when you're out can reduce anxiety significantly.
Wear a medical ID. If you have significant autonomic neuropathy — especially hypoglycemia unawareness or severe orthostatic hypotension — a medical alert bracelet or card can provide critical information to first responders if you become incapacitated.
Monitor regularly. Keep a symptom diary and check your blood pressure both lying down and standing (orthostatic readings). This data helps your doctor fine-tune your treatment and catch changes early. If you have diabetes, frequent blood sugar monitoring (or a CGM) becomes even more important with autonomic neuropathy.
Frequently Asked Questions About Autonomic Neuropathy
When to Seek Help
If you're living with neuropathy and experiencing any of the symptoms described in this article — persistent dizziness upon standing, unexplained digestive problems, unusual sweating patterns, bladder issues, or any of the other autonomic symptoms — bring these up with your healthcare provider. These symptoms are often not volunteered by patients because they seem unrelated to “nerve damage,” and they're not always asked about by doctors who may be focused on sensory symptoms.
Autonomic neuropathy may not always be preventable, but it is manageable. With the right combination of medical treatment, lifestyle adjustments, and awareness, you can maintain your quality of life and stay ahead of potential complications. You don't have to figure this out alone — your medical team, your community, and resources like this are here to help you navigate it.
What's Your Neuropathy Score?
Take our free 60-second assessment to get your personalized severity score and evidence-based recommendations.
Find Out Your Score

