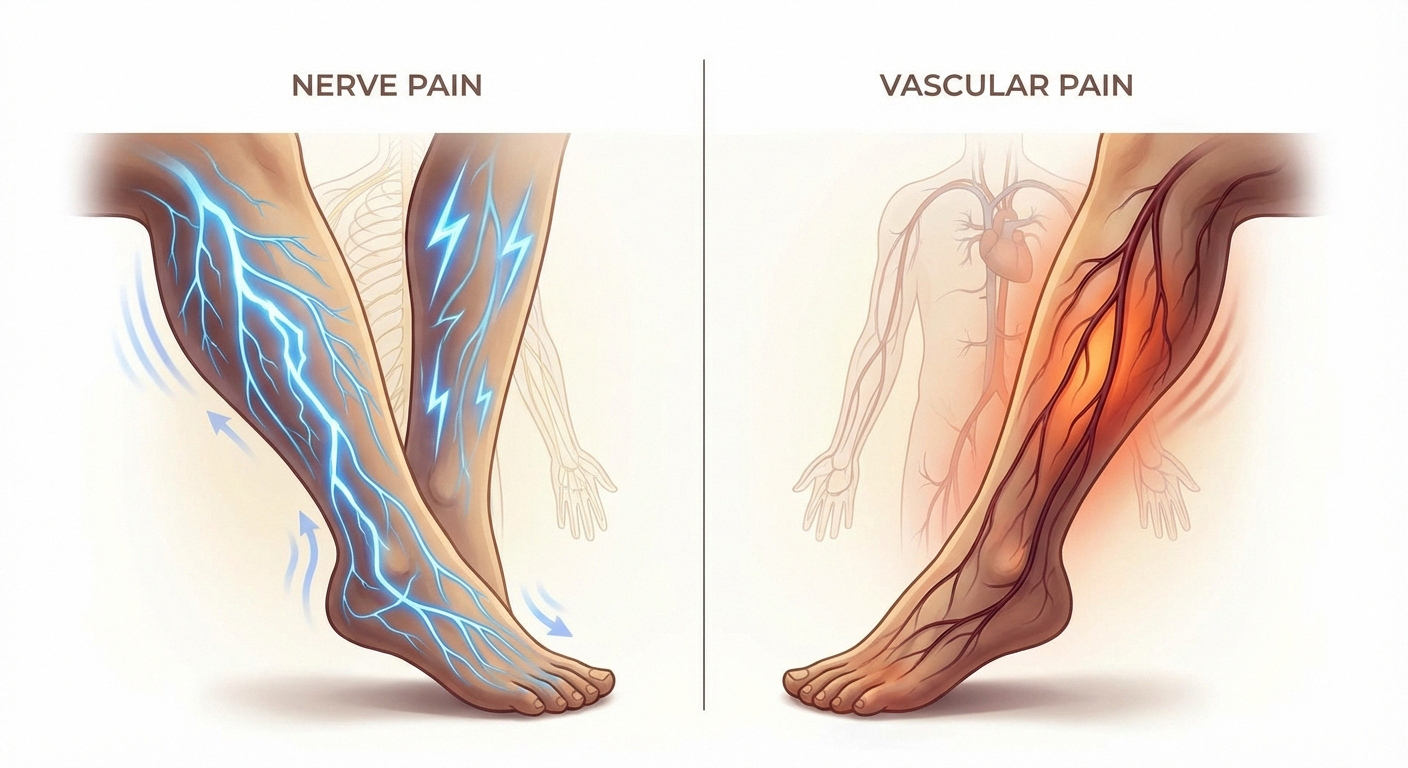
When dealing with chronic pain, it's easy to feel overwhelmed by all the terms doctors and specialists throw around. Two common types of pain that people experience are nerve pain (neuropathic pain) and vascular pain. Although they may feel similar at times—with sensations like burning, cramping, or numbness—their underlying causes, treatments, and implications differ significantly. For more, see our guide on neuropathy stages.
Nerve pain can also affect the upper body — learn about neuropathy in hands.
One of the most common nerve conditions is diabetic neuropathy.
In this article, we'll break down the differences between nerve and vascular pain, discuss their causes, symptoms, and common treatment approaches, and help you understand when it's time to seek professional medical care.
Americans are estimated to have peripheral neuropathy — and millions more live with vascular circulation problems that cause similar pain
Browse all our understanding neuropathy guides for more articles like this one.
What is Nerve Pain?
Nerve pain, also known as neuropathy or neuropathic pain, is caused by damage or dysfunction in the nervous system. Instead of receiving normal signals from the nerves, the brain interprets abnormal signals as pain—even when no physical injury is present. The pain can feel electric, burning, or stabbing, and often appears in the hands and feet where nerve endings are densest.
Common Causes of Nerve Pain:
- Diabetes (diabetic neuropathy — the most common cause)
- Injuries (spinal cord injuries or physical trauma)
- Autoimmune diseases (like multiple sclerosis or lupus)
- Vitamin deficiencies (especially B vitamins B1, B6, B12)
- Heavy metal toxicity
- Infections (shingles, HIV)
🧠 Common Nerve Pain Symptoms
Burning, tingling, or pins-and-needles sensations (especially in feet and hands)
Sharp, shooting pains that seem to come from nowhere
Numbness or reduced sensitivity to touch or temperature
Allodynia — pain from stimuli that shouldn't hurt, like light touches or bedsheets
Muscle weakness or twitching in more advanced cases
For a deeper understanding of how to address nerve damage causes, explore strategies that may help reduce or even reverse neuropathy progression. If nerve pain becomes chronic and begins to interfere with daily life—like walking, sleeping, or holding objects—it's essential to see a healthcare provider. Left untreated, nerve pain can worsen and lead to permanent damage.
What is Vascular Pain?
Vascular pain occurs when blood flow to a certain area of the body is restricted. This reduced blood circulation deprives muscles and tissues of the oxygen they need, causing cramping, aching, and sometimes swelling. Unlike nerve pain, which can occur at rest, vascular pain often worsens with physical activity when oxygen demand increases—and may improve when you rest and reduce that demand.
Common Causes of Vascular Pain:
- Peripheral Artery Disease (PAD) — narrowing of arteries that supply the legs
- Deep Vein Thrombosis (DVT) — blood clots in deep veins
- Atherosclerosis — buildup of plaque in artery walls
- Raynaud's Disease — narrowing of blood vessels in extremities triggered by cold or stress
- Varicose veins — enlarged, twisted veins with poor circulation
- Claudication — leg pain during exercise due to inadequate blood supply
🩸 Common Vascular Pain Symptoms
Cramping or aching in the calves, thighs, or buttocks — especially during physical activity
Cold or pale extremities (feet or hands feel colder than the rest of the body)
Swelling in the legs or feet (especially at day's end)
Ulcers or wounds that are slow to heal — a serious warning sign
Since vascular pain is tied to poor circulation, treatments often focus on restoring proper blood flow through medications, compression therapy, exercise programs, and in severe cases, surgical interventions.
Key Differences Between Nerve Pain and Vascular Pain
Understanding exactly how these two types of pain differ can help you communicate more effectively with your doctor and pursue the right diagnosis sooner.
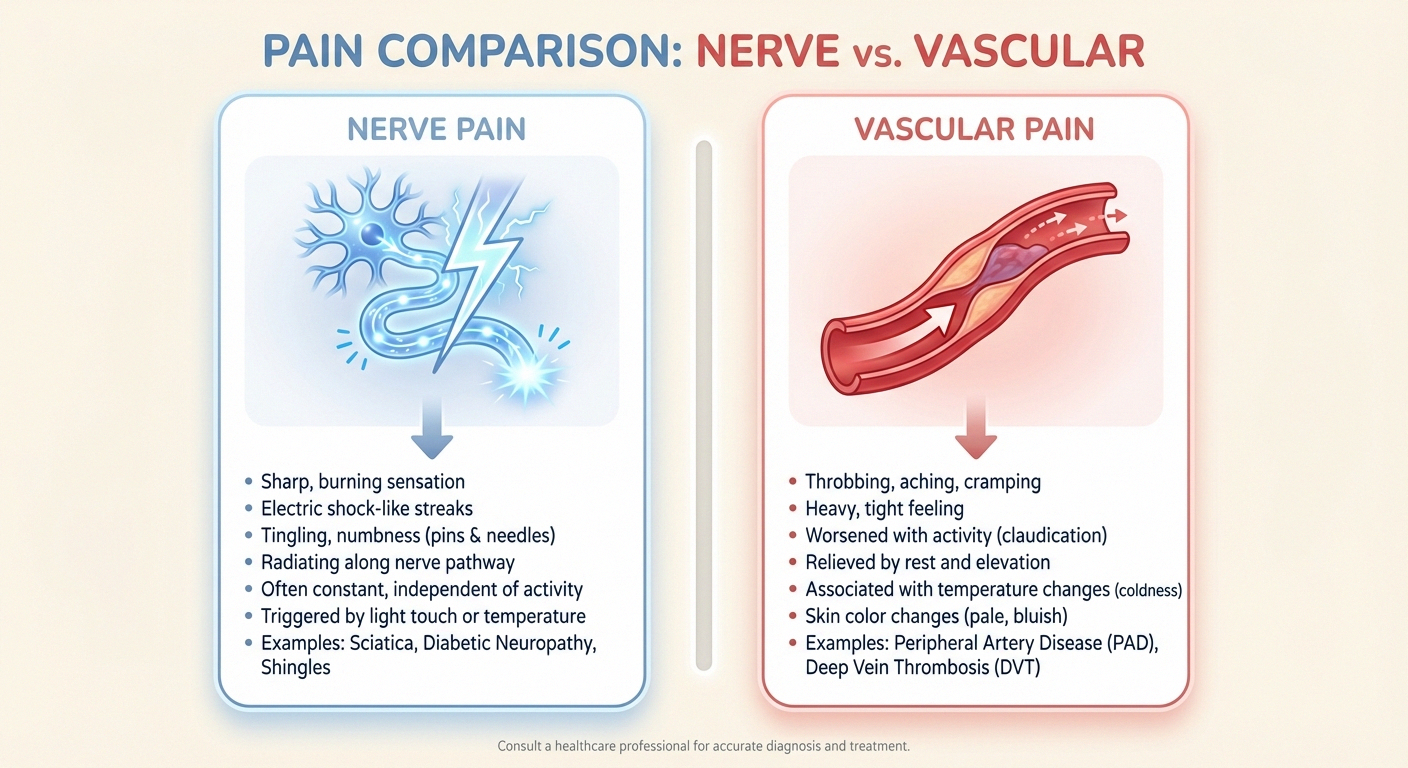
⚡ Nerve Pain
Cause: Damaged or dysfunctional nerves
Location: Specific nerve paths — often hands and feet
Sensations: Burning, tingling, electric, shooting
Triggers: Spontaneous, at rest, or from light touch
Treatment Focus: Calming and repairing nerves, addressing root cause
🩸 Vascular Pain
Cause: Restricted blood flow to tissues
Location: Larger regions — entire limbs, worsens with exertion
Sensations: Cramping, throbbing, aching, heaviness
Triggers: Physical activity, improves with rest
Treatment Focus: Improving circulation, reducing plaque buildup
Research Says
Diabetes is one of the most significant risk factors for both nerve pain and vascular pain. High blood sugar damages nerve fibers directly (causing diabetic neuropathy) while also damaging blood vessel walls (contributing to peripheral artery disease). Up to 50% of people with diabetes develop some form of neuropathy, and they are also 2–4 times more likely to develop PAD than the general population.
Treatment Options for Nerve Pain
Treating nerve pain typically involves a combination of lifestyle changes, medications, and supportive therapies. The right approach depends on identifying the underlying cause of the nerve damage.
1. Nutritional and Supplement Support
B vitamins—especially B1 (thiamine), B6, and B12—play a critical role in nerve health and repair. Deficiencies in these vitamins are a common and often overlooked cause of peripheral neuropathy. Explore a broader range of supplements for nerve pain relief to learn which nutrients may support nerve repair and reduce discomfort.
2. Prescription Medications
- Anticonvulsants: Gabapentin and pregabalin are commonly prescribed to calm nerve signal misfiring.
- Antidepressants: Duloxetine and amitriptyline can help modulate pain signals in the nervous system.
- Topical Treatments: Lidocaine patches and capsaicin creams can provide targeted, localized relief.
3. Lifestyle Adjustments
- Maintain a balanced diet: Foods rich in omega-3 fatty acids and B vitamins can support nerve repair and reduce inflammation.
- Exercise regularly: Low-impact activities like swimming or walking can improve nerve function and reduce pain signals.
- Reduce alcohol consumption: Alcohol can directly damage peripheral nerves and worsen neuropathy symptoms.
- Control blood sugar: For diabetic neuropathy, stabilizing blood glucose is the most important step to slow progression.
You can also explore natural remedies for peripheral neuropathy pain as complementary approaches to conventional treatment.
Key Takeaway
Getting the right diagnosis is the most critical first step for nerve pain. Treatments for neuropathy differ significantly depending on the root cause—diabetic neuropathy is managed differently from vitamin-deficiency neuropathy or injury-related nerve damage. Always work with your healthcare provider to identify the specific cause before beginning any treatment plan.
Treatment Options for Vascular Pain
Since vascular pain is associated with restricted blood flow, treatments aim to restore circulation and prevent dangerous complications like blood clots or tissue damage.
1. Medications
- Blood thinners: Help prevent clots from forming or growing (e.g., warfarin, aspirin, newer anticoagulants).
- Cholesterol-lowering medications: Statins can reduce plaque buildup in artery walls.
- Vasodilators: Help widen blood vessels to improve circulation to affected areas.
2. Compression Therapy
Wearing compression stockings can help reduce swelling and improve blood return from the legs to the heart. You can also apply home remedies to reduce leg pain and improve circulation as part of a daily care routine.
3. Exercise Therapy
Structured exercise programs, especially walking to improve circulation, can help reduce symptoms of PAD and enhance blood flow safely. Regular walking stimulates the development of collateral blood vessels around blockages over time.
4. Surgical Interventions
In severe cases, procedures like angioplasty (widening of narrowed arteries) or bypass surgery may be necessary to restore adequate blood flow to affected limbs.
How to Know Which Treatment You Need
Knowing whether your pain is nerve-based or vascular in origin is essential—the wrong treatment won't help, and may delay getting the right care. Here are some clues:
- If your primary concern is burning, tingling, or pins-and-needles sensations—particularly at night or at rest—nerve-related causes and treatments are more likely to apply.
- If you are experiencing leg cramps that appear during walking and ease with rest, or cold, pale feet, vascular disease may be the underlying cause and should be evaluated promptly by a physician.
- If you have diabetes, you may be dealing with both simultaneously—and need evaluation for both conditions.
When to Seek Medical Attention

It's crucial to seek medical care if you experience any of the following warning signs:
See a Doctor If You Have:
- Severe or sudden pain that doesn't improve with rest
- Sores or wounds on your feet or legs that don't heal within a normal timeframe
- Persistent numbness or weakness affecting balance or daily function
- Swelling or redness in the legs — potential signs of deep vein thrombosis (DVT), which is a medical emergency
- Sudden, dramatic change in color or temperature of a limb
Finding Relief from Nerve and Vascular Pain
Understanding the differences between nerve pain and vascular pain can guide you toward the right treatments and lifestyle changes. While nerve pain often requires calming inflamed nerves, addressing nutritional deficiencies, and managing the underlying cause, vascular pain necessitates improving blood flow and preventing further blockages.
For those seeking to manage nerve pain naturally, lifestyle adjustments and targeted nutritional support can provide meaningful additional relief alongside conventional medical treatment.
Ultimately, the best course of action is to work with a healthcare professional who can identify the underlying cause of your pain and create a tailored treatment plan. Early diagnosis and proper treatment are the most reliable paths to regaining control and improving your quality of life.


