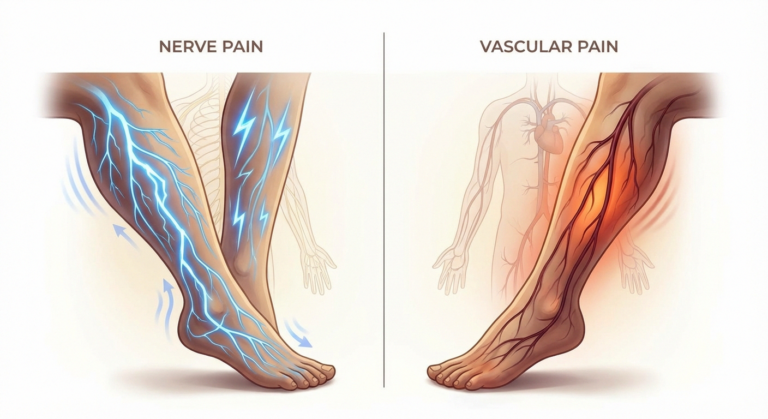
Neuropathy Diagnosis: Tests Your Doctor May Order and What They Mean
I still remember sitting in my neurologist's office, my feet buzzing with that familiar pins-and-needles sensation, wondering why is this happening to me? The doctor mentioned words like “nerve conduction study” and “electromyography,” and honestly, I felt overwhelmed. If you're at the beginning of your neuropathy diagnosis journey—or somewhere in the frustrating middle—I want you to know that understanding these tests can take so much of the anxiety away. After more than a decade of living with neuropathy and navigating the medical system, I've learned that knowledge really is power when it comes to advocating for yourself.
Getting a proper neuropathy diagnosis isn't always a straight line. It often involves multiple appointments, several different tests, and sometimes a fair amount of patience. But each test your doctor orders is a piece of the puzzle—helping to identify not just whether you have nerve damage, but what kind, how severe it is, and most importantly, what might be causing it. And that last part? That's the key to figuring out whether your neuropathy can potentially be reversed or at least managed more effectively.
Let's walk through the most common diagnostic tests together, so you'll know exactly what to expect and what the results may tell you.
Why Proper Diagnosis Matters
Here's something that surprised me early on: peripheral neuropathy isn't actually a single disease. It's a description of nerve damage that can have over 100 different causes. According to research, approximately 2.4% of the general population lives with some form of peripheral neuropathy, and that number rises to between 5% and 8% for people over 45. Among those with diabetes, the prevalence may be as high as 50%.
Why does pinpointing the cause matter so much? Because treatment depends entirely on it. If your neuropathy stems from a vitamin deficiency, addressing that deficiency may help slow or even reverse the damage. If it's related to diabetes, better blood sugar management becomes the cornerstone of your care plan. Without a thorough diagnosis, you're essentially guessing—and when it comes to nerve health, guessing can mean missing a window where intervention might make a real difference.
I've spoken with many people in my support group who went years without a proper neuropathy diagnosis. Some were told their symptoms were “just stress” or “part of aging.” Understanding the stages of neuropathy and catching it early can make a meaningful difference in outcomes. If your symptoms are progressing, don't wait—advocate for testing.
The Physical and Neurological Exam: Where It All Starts
Before ordering any specialized tests, your doctor will likely start with a thorough physical and neurological examination. This is actually more revealing than you might expect. During my first neurological exam, I was surprised by how much my doctor could learn just by tapping my reflexes, testing my ability to feel a tuning fork's vibration, and having me walk heel-to-toe across the room.
Here's what a typical neurological exam for neuropathy may include:
Reflex testing: Your doctor taps specific points (like your knee and ankle) with a small rubber hammer. Diminished or absent reflexes can indicate nerve damage.
Sensory testing: Using tools like monofilaments (thin, flexible fibers pressed against your skin), tuning forks, or pinprick tests, your doctor assesses your ability to feel light touch, vibration, temperature, and pain. This helps map out which types of nerve fibers may be affected.
Muscle strength testing: You'll be asked to push and pull against the doctor's hands in various positions. Weakness in specific patterns can suggest motor nerve involvement.
Balance and coordination: Walking tests, standing with eyes closed (Romberg test), and other balance assessments can reveal proprioceptive nerve damage—the nerves that tell your brain where your body is in space.
This exam is completely painless and gives your doctor crucial information about which nerves may be affected—sensory, motor, or autonomic—and whether the pattern suggests a specific type of neuropathy. It also helps them decide which additional tests to order.
Nerve Conduction Study (NCS) and EMG: The Electrical Tests
If I had to name the test most closely associated with neuropathy diagnosis, it would be the nerve conduction study, usually performed alongside an electromyography (EMG). These are often done together in the same appointment and are sometimes referred to collectively as “electrodiagnostic testing” or simply “the nerve test.”
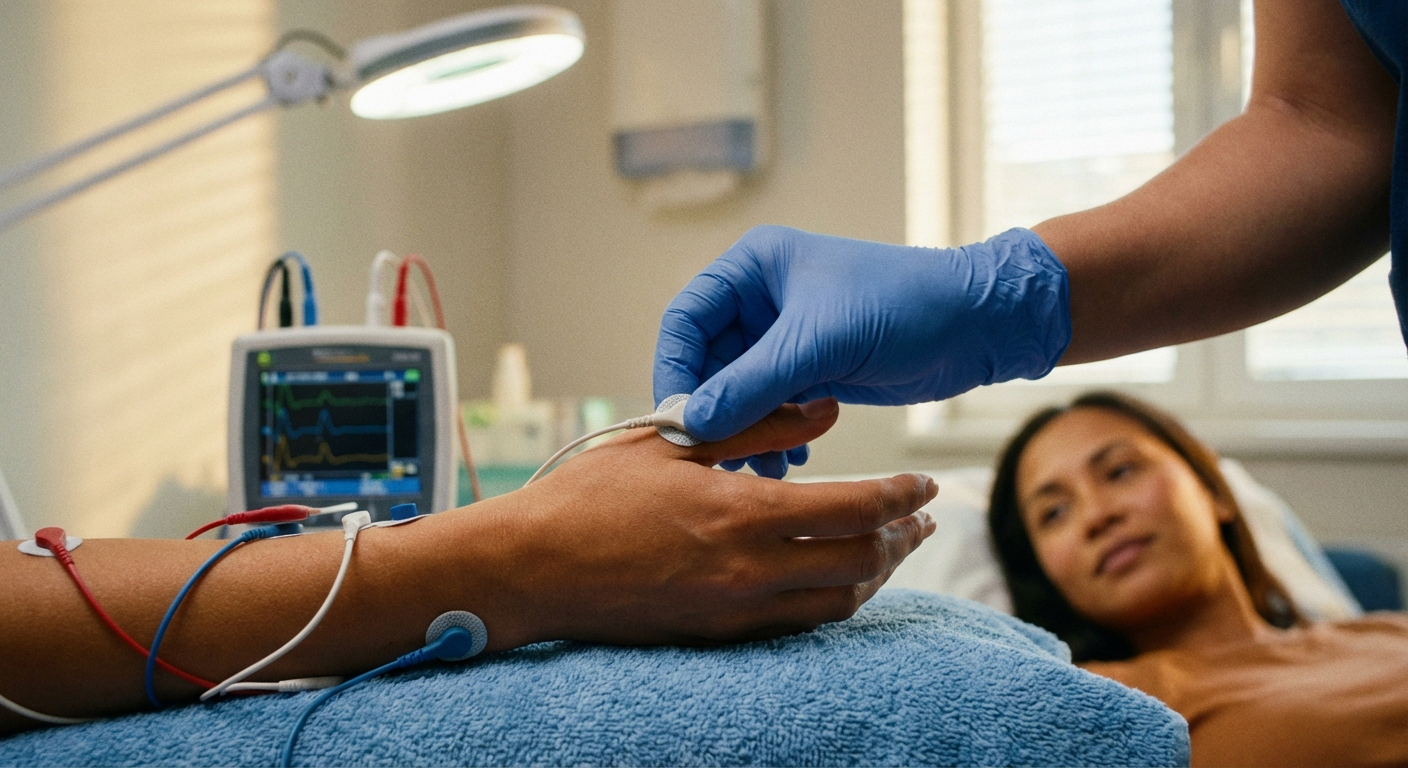
Nerve Conduction Study (NCS): During this test, small electrodes are placed on your skin over specific nerves. A mild electrical impulse is sent through the nerve, and the speed and strength of the signal is measured. Think of it like checking whether your electrical wiring is carrying a signal efficiently. Slow conduction speeds or weak signals may indicate damage to the myelin sheath (the protective coating around nerves), while reduced signal amplitude can suggest axonal damage (damage to the nerve fiber itself).
Electromyography (EMG): After the NCS, your doctor may perform an EMG, which involves inserting a very thin needle electrode into specific muscles. This measures the electrical activity in your muscles both at rest and during contraction. Abnormal patterns can help distinguish between nerve damage and muscle disorders, and can show whether nerve damage is actively occurring or is an older, stable injury.
I won't sugarcoat it—the NCS involves small electric shocks that can feel uncomfortable, and the EMG needle isn't exactly pleasant. But both tests are generally tolerable and last about 30 to 60 minutes combined. The information they provide is invaluable.
What these tests can reveal:
• Whether you have neuropathy (and confirmation of clinical findings)
• Whether the damage is to large nerve fibers (these tests primarily assess large fibers)
• Whether the pattern is demyelinating or axonal
• Whether the neuropathy is generalized or focal (affecting specific areas)
• How severe the nerve damage may be
One important limitation: NCS and EMG only evaluate large nerve fibers. If your symptoms involve burning pain, temperature sensitivity, or autonomic issues—and your NCS comes back normal—it doesn't mean nothing is wrong. You may have small fiber neuropathy, which requires different testing. This was actually my experience, and it took additional testing to get the full picture.
Blood Tests: Searching for the Underlying Cause
Blood work is one of the most important parts of the diagnostic process because it helps identify why you have neuropathy. Your doctor may order a comprehensive panel that includes some or all of the following:

Fasting blood glucose and HbA1c: Since diabetes and prediabetes are the most common causes of peripheral neuropathy, these are usually the first blood tests ordered. HbA1c gives a picture of your average blood sugar over the past 2–3 months. Even mildly elevated blood sugar (prediabetes) can damage nerves over time.
Vitamin B12 and folate: B12 deficiency is a well-known and treatable cause of neuropathy. Interestingly, you can have low-normal B12 levels and still experience nerve symptoms. Some doctors will also check methylmalonic acid (MMA), which can be elevated even when B12 appears normal—catching deficiencies that standard B12 tests might miss.
Complete blood count (CBC) and comprehensive metabolic panel (CMP): These provide a broad overview of your general health, including kidney and liver function. Kidney disease and liver disease can both contribute to neuropathy.
thyroid-related neuropathy function tests (TSH, T3, T4): Both hypothyroidism and hyperthyroidism have been associated with peripheral neuropathy.
Inflammatory markers (ESR, CRP): Elevated inflammation markers may suggest autoimmune or inflammatory causes of neuropathy.
Serum protein electrophoresis (SPEP) and immunofixation: These tests look for abnormal proteins in the blood (monoclonal gammopathies) that can be associated with certain types of neuropathy.
Additional tests your doctor might order: Depending on your situation, this could include tests for Lyme disease, HIV, hepatitis B and C, vitamin D, copper levels, and specific autoimmune antibodies (like ANA or anti-ganglioside antibodies).
I've had my blood drawn more times than I can count at this point, and I'll say this: it's worth it. The blood work that finally identified a contributing factor in my case was a turning point in my treatment. Talk to your doctor about which tests are most appropriate for your specific symptoms.
Skin Punch Biopsy: The Small Fiber Detective
If your nerve conduction studies come back normal but you're still experiencing burning, tingling, or pain—especially in your feet—your doctor may recommend a skin punch biopsy. This was a game-changer for me personally, and it's become increasingly recognized as a critical diagnostic tool.
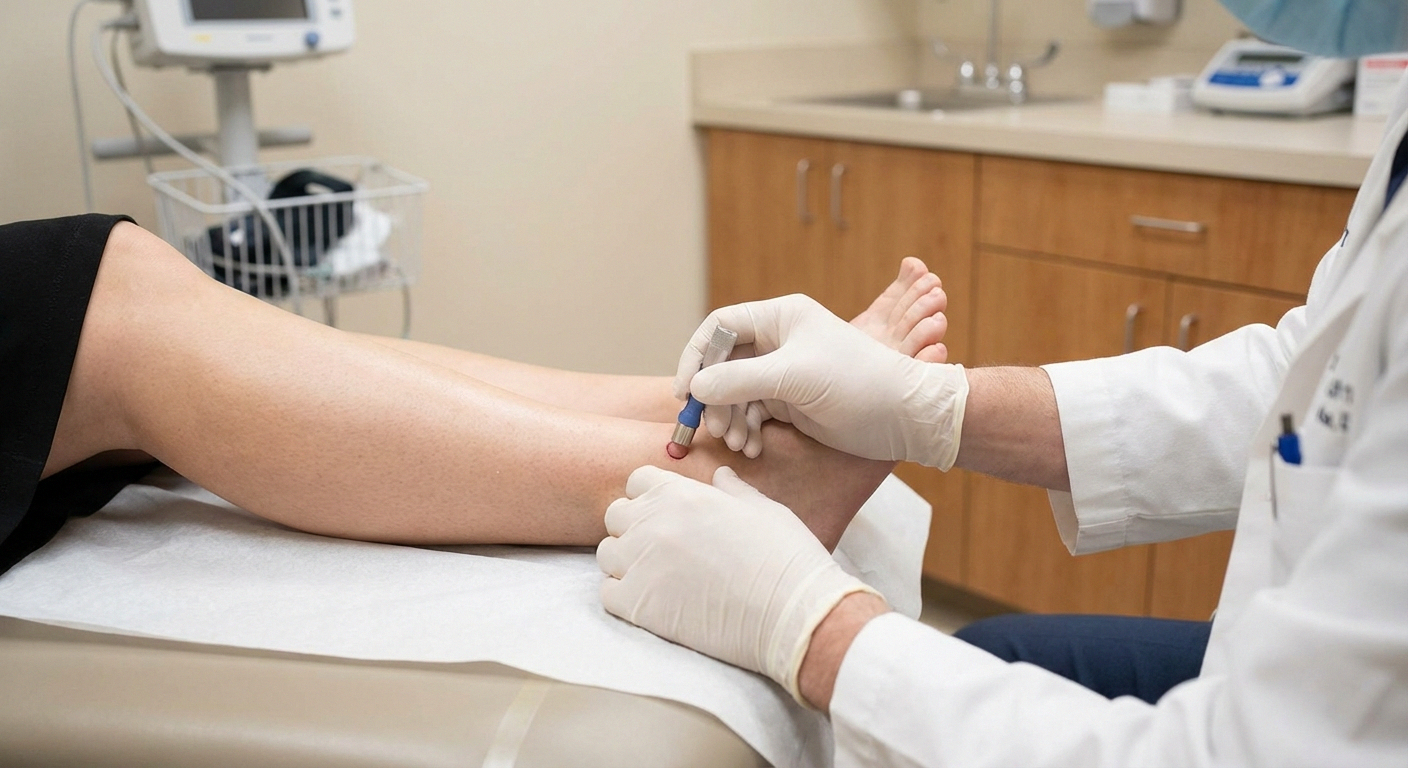
The procedure is simpler than it sounds. A small, circular tool (usually 3mm in diameter) is used to take a tiny sample of skin, typically from your lower leg near the ankle and sometimes from the upper thigh as well. The skin sample is then analyzed under a microscope to count the intraepidermal nerve fiber density (IENFD)—essentially, how many small nerve fibers are present in that area of skin.
The procedure itself is relatively quick—about 15 minutes—and involves only a local anesthetic. The small wound heals within a week or two. Most people describe the discomfort as minimal.
If your nerve fiber count is below the established age- and sex-matched norms, it confirms small fiber neuropathy. This diagnosis is significant because small fiber neuropathy can sometimes be associated with treatable conditions like autoimmune disorders, prediabetes, or certain vitamin deficiencies. It can also be repeated over time to track whether your condition is progressing or responding to treatment.
Imaging Tests: MRI, CT, and Ultrasound
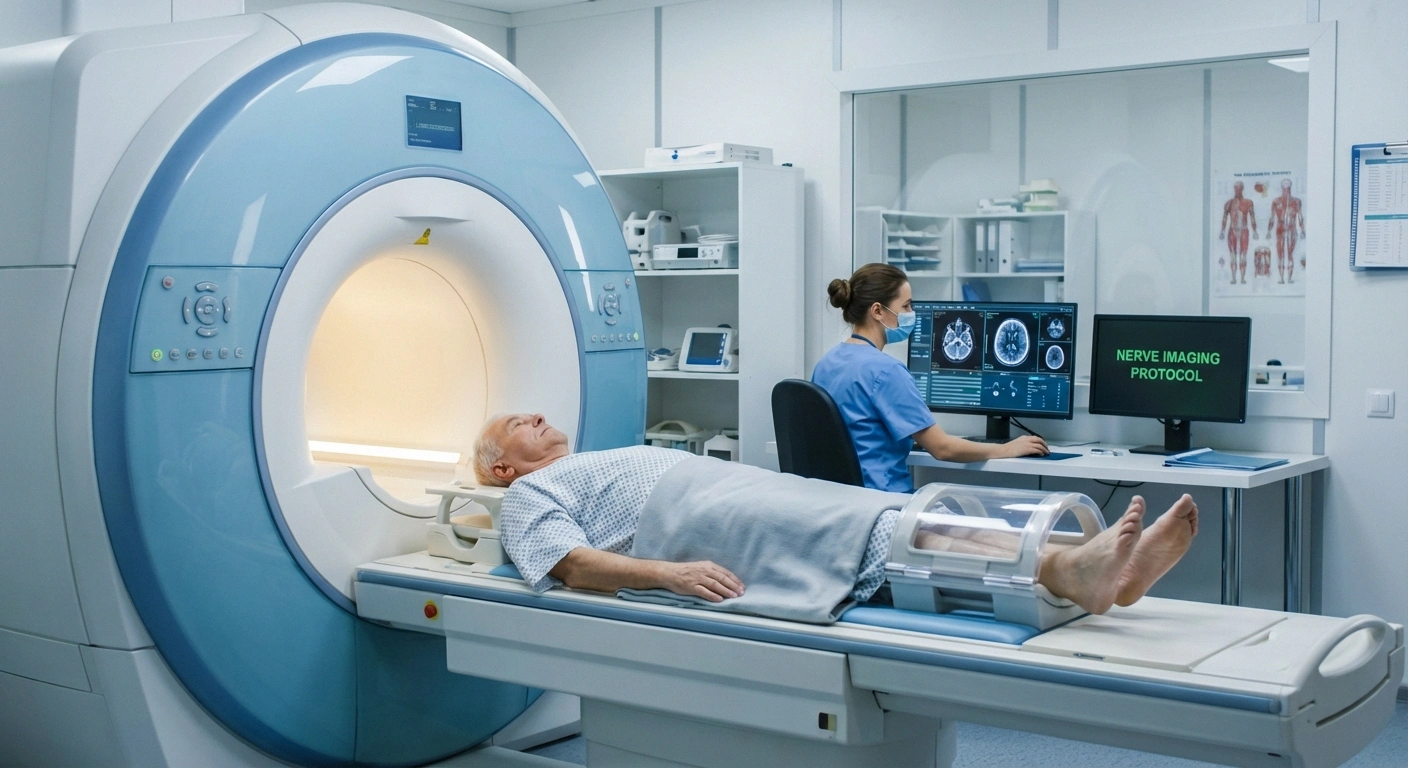
While imaging isn't always part of a standard neuropathy workup, there are situations where your doctor may order an MRI, CT scan, or nerve ultrasound. These tests don't diagnose neuropathy directly in most cases, but they help rule out structural causes of nerve compression or damage.
MRI (Magnetic Resonance Imaging): An MRI may be ordered to check for herniated discs, spinal stenosis, tumors, or other structural abnormalities that could be compressing nerves. If your neuropathy affects specific areas (like one arm or one side of your body), an MRI can help determine whether the nerve damage originates in the spine or in the peripheral nerves themselves. MRI neurography is a specialized technique that can sometimes visualize individual peripheral nerves in detail.
CT Scan: Similar to MRI but using X-ray technology, CT scans may be used when MRI isn't available or when looking for bony abnormalities that could affect nerves.
Nerve Ultrasound: This is a newer and increasingly popular tool. High-resolution ultrasound can visualize peripheral nerves directly, showing swelling, thickening, or structural changes. It's non-invasive, painless, and relatively affordable compared to MRI. Some specialists use it alongside nerve conduction studies for a more complete assessment.
Autonomic Testing: When Your Involuntary Nerves Are Affected
If you're experiencing symptoms like dizziness upon standing, abnormal sweating, digestive issues, bladder problems, or heart rate irregularities, your doctor may suspect autonomic neuropathy—damage to the nerves that control your body's involuntary functions. Specialized autonomic testing can help confirm this.
Quantitative Sudomotor Axon Reflex Test (QSART): This test measures your sweat response by applying a mild electrical current to stimulate sweat glands at specific locations on your body. Reduced or absent sweating can indicate small fiber or autonomic nerve damage. It's painless and takes about 30 minutes.
Tilt Table Test: You lie on a table that slowly tilts you from a flat position to nearly standing while your heart rate and blood pressure are monitored. This test evaluates how well your autonomic nervous system regulates blood pressure during position changes. An abnormal drop in blood pressure or excessive heart rate increase may indicate autonomic dysfunction.
Thermoregulatory Sweat Test (TST): A special powder that changes color with moisture is applied to your skin, and you're placed in a warm chamber. The pattern of sweating (or lack thereof) is mapped across your body, creating a visual representation of which autonomic nerves may be affected.
Heart Rate Variability and Deep Breathing Tests: These measure how your heart rate responds to deep breathing and the Valsalva maneuver (forcefully breathing out against resistance). Reduced heart rate variability can be an early sign of cardiac autonomic neuropathy.
Autonomic testing is typically performed at specialized centers, often affiliated with major medical institutions. If your doctor suspects autonomic involvement, don't hesitate to ask for a referral. The full battery of autonomic tests usually takes about 90 minutes to 2 hours and is generally not painful.
Genetic Testing: When It Runs in the Family
If your neuropathy started at a young age, progresses slowly, or if other family members have similar symptoms, your doctor may recommend genetic testing. Hereditary neuropathies, particularly Charcot-Marie-Tooth disease (CMT), are more common than many people realize—affecting approximately 1 in 2,500 people.
Genetic testing typically involves a simple blood sample that's analyzed for specific gene mutations associated with hereditary neuropathies. The most common hereditary neuropathy, CMT type 1A, is caused by a duplication of the PMP22 gene and can be identified through targeted genetic testing.
While knowing you have a genetic neuropathy doesn't change the fact that you have nerve damage, it can be important for family planning, connecting with specialized treatment programs, and avoiding unnecessary (and sometimes invasive) testing to find a cause that isn't there. It can also help you understand your likely prognosis and connect with condition-specific support communities.
For some people, the neuropathy diagnosis journey ends at idiopathic neuropathy—meaning no cause is identified despite thorough testing. If this happens to you, know that you're not alone and that treatment for symptoms and quality of life is still very much possible.
What to Expect at Your Appointment

Walking into a neurology appointment for the first time can feel intimidating. Here's what I wish someone had told me before my first visit, so you can feel prepared and make the most of your time with the doctor.
📋 What to Expect at Your Neurology Appointment
Gather your medical records, list of medications (including supplements), and write down your symptoms with dates of onset. Note any family history of neuropathy or neurological conditions.
Your doctor will ask detailed questions about your symptoms, when they started, what makes them better or worse, your medical history, medications, alcohol use, and occupational exposures.
Expect reflex testing, sensory evaluation (light touch, pinprick, vibration), muscle strength assessment, and balance and gait evaluation. Wear loose, comfortable clothing.
Based on the exam findings, your doctor may order blood work, schedule a nerve conduction study/EMG, or refer you for additional testing like a skin biopsy or imaging.
You'll typically have a follow-up appointment to review test results and discuss a treatment plan. Some results (like blood work) may come back within days, while others (like biopsy results) may take 2–4 weeks.
A few practical tips from my own experience: Bring a notebook or use your phone to take notes—you'll be processing a lot of information. If possible, bring someone with you for emotional support and an extra set of ears. Don't be afraid to ask your doctor to explain something in simpler terms. And remember, this appointment is the start of getting answers, not the end.
Questions to Ask Your Doctor
I firmly believe that the relationship between you and your doctor should be a partnership. You don't have to just sit there and nod—asking good questions can make a real difference in the quality of your care. Here are some questions I'd recommend bringing to your appointment:
• What type of neuropathy do you suspect I have?
• Which specific tests do you recommend, and what will each one tell us?
• Could my neuropathy be related to any of my current medications?
• Are there any treatable causes we should investigate?
• Based on my symptoms, should we test for small fiber neuropathy?
• How severe does my nerve damage appear at this point?
• What are my treatment options while we work on finding the cause?
• Should I see a specialist or consider a second opinion?
• How often should I have follow-up testing to monitor progression?
• Are there any lifestyle changes that might help manage my symptoms?
If your doctor doesn't seem open to answering your questions or dismisses your concerns, it may be worth seeking a neurologist who specializes in peripheral neuropathy. Your symptoms are real, and you deserve thorough investigation. Some people find that medications like gabapentin or pregabalin help manage symptoms while the diagnostic process continues—discuss these options with your healthcare provider.
🩺 Signs You May Need Diagnostic Testing for Neuropathy
If you're experiencing two or more of these symptoms, consider speaking with your doctor about diagnostic testing.
Comparing Neuropathy Diagnostic Tests
With so many possible tests, it can help to see them side by side. Here's a quick comparison of the most common neuropathy diagnostic tests:
⚡ Nerve Conduction Study / EMG
What it tests: Large fiber nerve function, muscle electrical activity
Duration: 30–60 minutes
Discomfort: Mild to moderate
Best for: Confirming neuropathy, determining type and severity
🩸 Blood Tests
What it tests: Underlying causes (diabetes, vitamins, thyroid, autoimmune)
Duration: 5–10 minutes (draw)
Discomfort: Minimal (needle stick)
Best for: Identifying treatable causes of neuropathy
🔬 Skin Punch Biopsy
What it tests: Small fiber nerve density (IENFD)
Duration: 15 minutes
Discomfort: Minimal (local anesthetic)
Best for: Diagnosing small fiber neuropathy when NCS is normal
🧲 MRI / Imaging
What it tests: Structural causes (compression, tumors, disc issues)
Duration: 30–60 minutes
Discomfort: None (may be loud or confining)
Best for: Ruling out structural causes of nerve compression
💧 Autonomic Testing
What it tests: Involuntary nerve function (sweat, heart rate, blood pressure)
Duration: 90 minutes – 2 hours
Discomfort: Minimal
Best for: Evaluating autonomic neuropathy symptoms
🧬 Genetic Testing
What it tests: Hereditary neuropathy gene mutations
Duration: Simple blood draw
Discomfort: Minimal
Best for: Suspected hereditary neuropathy (family history, early onset)
Frequently Asked Questions About Neuropathy Diagnosis

Putting It All Together: Your Diagnosis Journey
Getting a neuropathy diagnosis can feel like a marathon, not a sprint. I know how frustrating it is to wait for test results, to wonder what's causing your symptoms, and to feel like no one quite understands what you're going through. But here's what I've learned after more than a decade of navigating this path: every test brings you closer to answers, and answers are the foundation of effective management.
Remember these key points as you move through the diagnostic process:
Be your own advocate. If something doesn't feel right or a test comes back normal when you're clearly symptomatic, speak up. Ask about additional testing options like skin biopsy or autonomic testing. You know your body better than anyone.
Diagnosis is a process, not a single event. It's normal for the diagnostic journey to involve multiple appointments, several types of tests, and sometimes adjustments along the way. Each piece of information refines the picture.
Finding the cause matters. While symptom management is important (and your doctor should be addressing your comfort throughout the process), identifying the underlying cause gives you the best chance of slowing progression and potentially improving your condition.
You're not alone. Millions of people navigate the neuropathy diagnosis process every year. Support groups, educational resources, and patient communities can provide invaluable emotional support and practical guidance while you wait for answers.
I'm Janet, a patient advocate sharing over a decade of personal experience managing neuropathy. I'm not a medical professional, and this article is for informational purposes only. Always consult with your healthcare provider for medical advice tailored to your individual situation.
What's Your Neuropathy Score?
Take our free 60-second assessment to get your personalized severity score and evidence-based recommendations.
Find Out Your Score