
Flying with Neuropathy: How to Survive Long Flights
I used to dread flying. Not the heights — the hours of sitting trapped in a metal tube while my feet burned and tingled like they were waking up from the world's longest sleep. One transatlantic flight left me hobbling through customs, wondering if travel was simply off the table with neuropathy.
It doesn't have to be. With the right preparation, long flights are survivable — and often more manageable than you'd expect. This guide covers everything from what happens to your nerves at altitude, to which seat to book, to exactly what to pack in your carry-on to make the journey bearable.
Why Flying Is Hard on Neuropathy
Understanding the mechanics helps you prepare more effectively. Several things happen on a plane that are particularly problematic for damaged peripheral nerves:
(vs 30–60% at home)
pressurized cabin
between walks
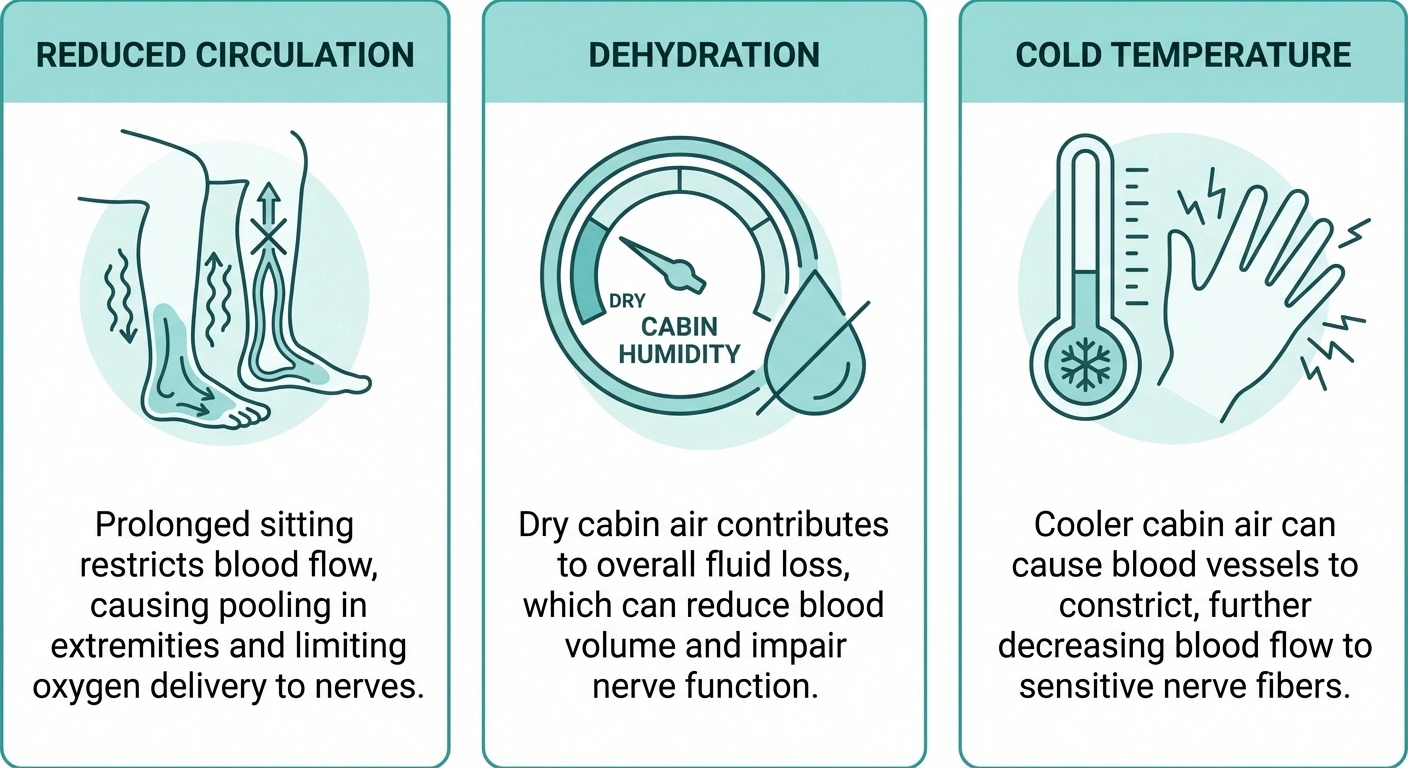
Prolonged Sitting Slows Circulation
When you sit still for hours, blood pools in the legs and feet. Circulation slows, reducing oxygen and nutrient delivery to already-compromised nerves. This is what makes neuropathy symptoms flare — the nerves are already working with reduced efficiency, and diminished circulation makes the situation worse. The typical airplane seat also puts your legs in a fixed position that may compress nerves at the back of the knee or hip, adding mechanical pressure to circulatory stress.
Cabin Pressure and Dehydration
Commercial aircraft cabins are pressurized to approximately 6,000 to 8,000 feet — lower than sea level, but low enough to affect circulation. Cabin humidity is also very low (typically 10 to 20%), which promotes dehydration faster than you'd normally expect. Dehydration reduces blood volume and thickens the blood slightly, further impairing circulation to peripheral nerves. If you add alcohol or excessive caffeine to the mix — both of which dehydrate — the effect compounds.
Temperature Changes and Sensitivity
Plane cabins get cold, especially on long overnight flights. For many neuropathy patients, cold temperatures amplify nerve sensitivity and increase burning or shooting pain. Having feet exposed to cold air vents or cold floors (if you remove shoes) can trigger significant flare-ups in people whose neuropathy is temperature-sensitive.
Choosing the Right Seat
This decision has a larger impact than any other single choice for a neuropathy flier. The Foundation for Peripheral Neuropathy specifically recommends booking a seat where you can stretch and move — and long flights without movement make symptoms significantly worse.
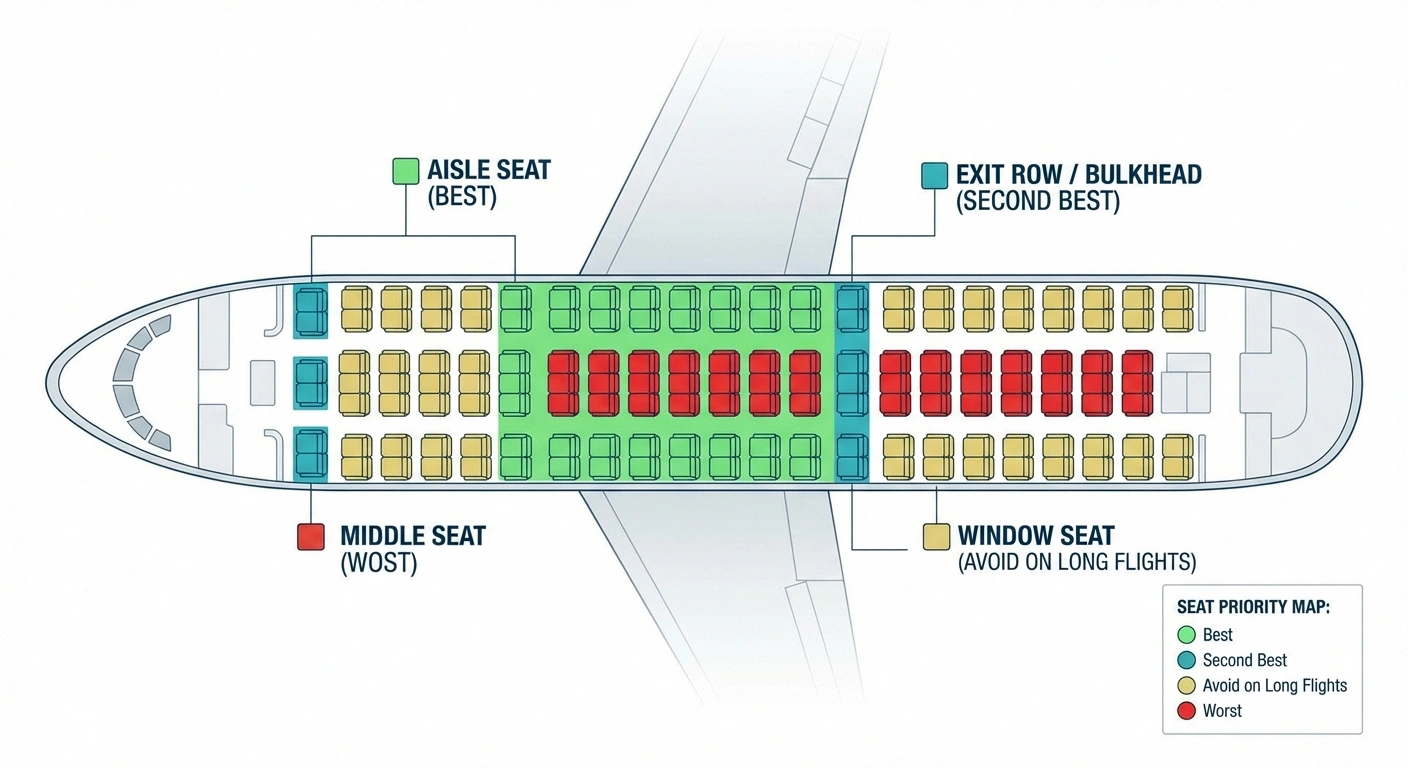
Here's the priority order:
- Aisle seat — the single most important choice. An aisle seat lets you stand and walk without disturbing anyone, allows you to stretch your legs into the aisle when the cart isn't passing, and eliminates the trapped feeling that makes neuropathy worse psychologically as well as physically.
- Exit row or bulkhead seat — extra legroom reduces the compression on the back of the legs and allows you to fully extend your knees. Worth the extra cost for flights over 3 hours.
- Avoid window seats for long flights — being trapped against the window for a 10-hour overnight flight means you'll disturb two people every time you need to stand, which means you'll stand less often. The barrier to movement is the biggest problem.
- Avoid middle seats entirely — obvious, but worth stating.
When booking, check whether the airline offers disability seating — many will give you priority access to better seats if you disclose a mobility-related condition. You don't need a formal disability designation; neuropathy with walking difficulties qualifies.
What to Pack in Your Carry-On
Your carry-on is your neuropathy survival kit. These items make a measurable difference on long flights:

Compression Socks
Compression socks are the single most evidence-supported intervention for air travel with neuropathy. They improve venous return from the legs, reduce swelling, and maintain better circulation during prolonged sitting. The Mayo Clinic Connect specifically recommends compression socks for neuropathy patients on flights, noting that cabin pressure can cause swelling in the feet that makes symptoms worse.
Choose graduated compression socks with 15–20 mmHg for most patients, or 20–30 mmHg if you have significant edema. Put them on before the flight, not after you're seated. Make sure they aren't too tight — constriction can worsen nerve pressure.
Footwear That Protects Without Restricting
Wear comfortable, supportive shoes that you can easily slip off when seated. Tight laces or narrow toe boxes will increase nerve pressure during swelling. Once in your seat, you can remove shoes entirely if it's more comfortable, but keep socks on to protect your feet from cold floors and to avoid the hypersensitivity that bare foot contact with surfaces can cause in neuropathy patients.
Lumbar Support and Seat Cushion
A small inflatable lumbar cushion helps maintain neutral spinal positioning, reducing the nerve compression that comes from slouching for hours. Some patients also benefit from a seat cushion that redistributes pressure — airplane seats are notoriously flat and hard. These add bulk to your carry-on but are worth it for flights over four hours.
Your Medications in Original Containers
Carry all neuropathy medications in your carry-on, never in checked luggage. If your bag gets lost, you don't want to be overseas without gabapentin or your other pain medications. Bring slightly more than you'll need — flight delays and unexpected extensions happen. Carry a copy of your prescriptions in case you need to fill medication abroad.
Noise-Canceling Headphones or Ear Protection
Continuous noise is a stressor, and chronic stress sensitizes pain pathways. This is less obvious than the other items but genuinely matters for some neuropathy patients: reducing sensory overload from engine noise helps keep the nervous system less reactive during a long flight.
In-Flight Movement: The Most Important Variable
Movement is the most effective tool you have for managing neuropathy on a plane. The science is simple: movement pumps blood back toward the heart, counteracting the pooling that causes most in-flight neuropathy flare-ups.
Stand and Walk Every 30 to 60 Minutes
Set a reminder. Walk to the back of the plane, stand for a minute or two, and walk back. This takes 3 to 4 minutes but resets your circulation significantly. Don't wait until you're in pain — regular preventive movement is far more effective than reactive walking after symptoms have already spiked.
In-Seat Exercises
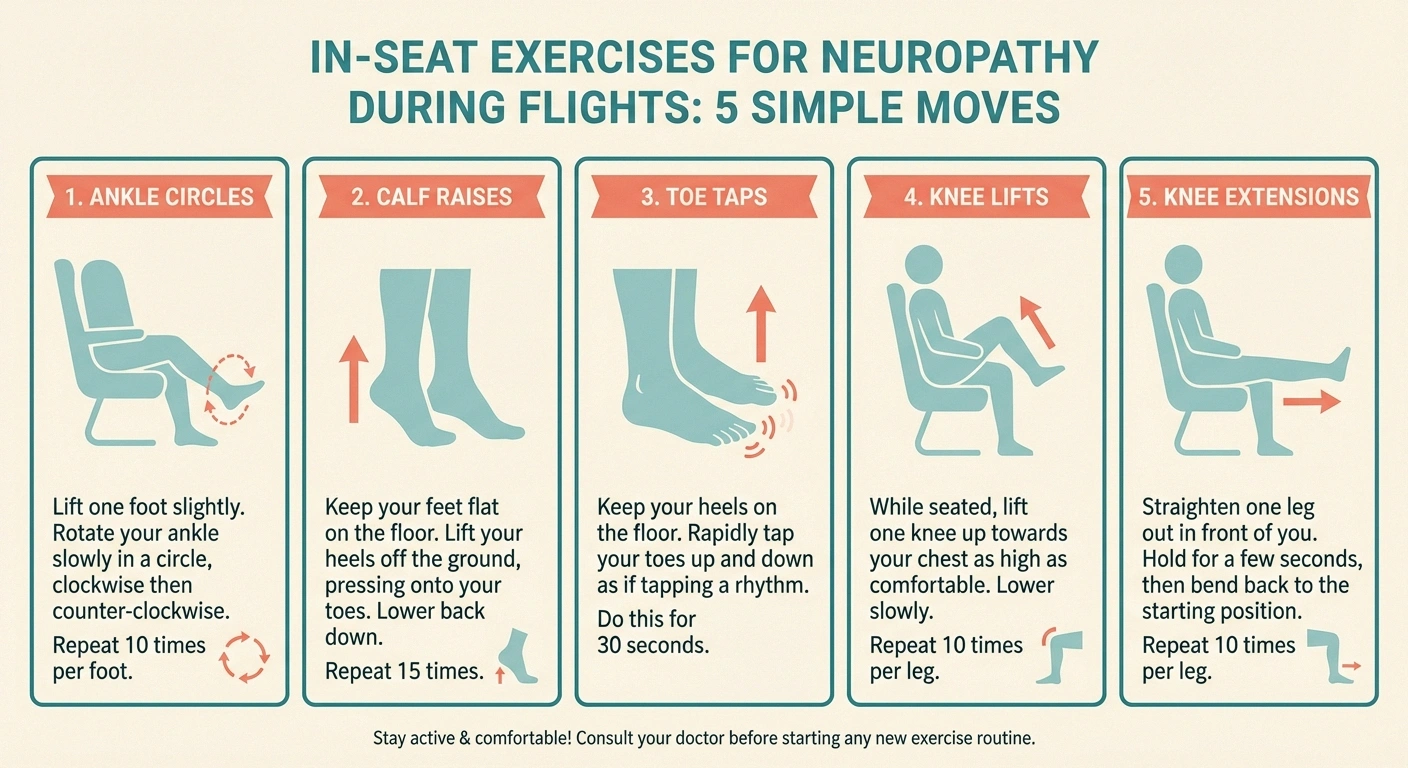
When walking isn't possible (seat belt sign is on, turbulence, sleeping passengers), do these seated exercises:
- Ankle circles — rotate each ankle clockwise and counterclockwise, 10 rotations each direction
- Calf raises — lift both heels off the floor while seated, hold for 2 seconds, lower. Repeat 15 to 20 times.
- Toe taps — tap your toes while keeping heels planted, alternating feet rapidly for 30 seconds
- Knee lifts — lift each knee toward your chest and hold for 10 seconds, alternating
- Knee extensions — extend one leg straight out, hold for 5 seconds, lower. Repeat 10 times per leg.
These exercises activate the calf muscle pump — the mechanism that pushes blood from the legs back to the heart against gravity. Doing them consistently every 30 to 45 minutes maintains circulation between walks.
Hydration and What to Eat on the Plane
Hydration is directly linked to neuropathy symptom intensity during flights. Dehydrated nerves are more electrically unstable and more prone to firing aberrantly. Aim for:

- At least 8 ounces of water per hour of flight time
- Bring your own water bottle to fill after security — don't rely on flight attendant service, which may not come often enough
- Avoid alcohol entirely on flights — it dehydrates and can significantly worsen neuropathy symptoms
- Limit caffeine to your normal intake — don't use coffee to compensate for sleep deprivation
For food, avoid salty airplane meals or snacks — sodium promotes swelling in the extremities, which worsens the nerve compression that long sitting already creates. Pack anti-inflammatory snacks: nuts, fruit, or a small sandwich from the terminal. If blood sugar management is part of your neuropathy care (as with diabetic neuropathy), maintaining stable glucose during the flight is especially important.
Temperature Management
Come prepared for cold. Pack warm socks, a light blanket or wrap, and wear layers you can remove or add. If cold temperatures reliably worsen your neuropathy, asking a flight attendant for an extra blanket early in the flight is better than waiting until you're already cold and symptomatic. Some patients find that warming gel packs (hand warmers) placed near the feet — not directly on the skin — help maintain warmth during cold flights.
Medication Timing on Long Flights
Talk to your neurologist before a long flight about whether any adjustments to your medication timing make sense. A few considerations:
- If you're crossing multiple time zones, you'll need a strategy for when to take medications that were previously timed to your sleep/wake cycle
- If your neurologist approves, taking your evening dose of gabapentin or a similar medication shortly before boarding a long overnight flight may reduce symptoms during the worst sleeping hours
- Topical treatments like lidocaine or capsaicin cream are useful for localized symptoms and don't cause the drowsiness that oral medications can
Never adjust medication timing without discussing it with your doctor first — especially for medications where timing affects seizure threshold or pain control stability.
At the Airport: Managing Before You Board
The airport experience matters as much as the flight. A few strategies:
- Request airport assistance — wheelchair service is available through the airline for people with mobility limitations. This isn't just for wheelchair users — anyone who needs assistance walking long distances through an airport qualifies. Request it when booking. There's no stigma, and it conserves energy for the flight itself.
- TSA medical accommodations — notify TSA screening that you have a medical condition affecting your legs and feet. You can request alternative screening methods if removing shoes is painful, and you're entitled to a private screening if needed.
- Arrive with a buffer — don't rush. Stress and physical exertion from rushing exacerbate neuropathy symptoms. Give yourself extra time so you can walk at your own pace, take breaks, and sit when needed.
- Walk before boarding — if you have time, walk slowly through the terminal rather than sitting at the gate. Moving blood before you're forced into a seated position helps.
After Landing: Recovery
Expect some post-flight symptom increase, especially after very long flights. Most neuropathy patients see improvement within a few hours of landing and resuming normal movement. To speed recovery:
- Walk as soon as you're off the plane — even slowly through the terminal
- Hydrate aggressively after landing
- Elevate your feet for 20 to 30 minutes when you arrive at your destination
- Gentle foot massage or a warm (not hot) foot soak can help reduce residual swelling and calm nerve activity
- Avoid the temptation to power through — rest on the first day if travel has been significant
For a therapeutic foot soak recipe that helps after long days on your feet (including travel days), we have a dedicated guide with neuropathy-specific ingredients.

Frequently Asked Questions
Is flying safe with peripheral neuropathy?
For most people with peripheral neuropathy, flying is safe with appropriate precautions. The main concerns are symptom flare-ups from prolonged sitting, dehydration, and cold — all of which can be managed. If you have severe autonomic neuropathy affecting heart rate or blood pressure, discuss flying with your neurologist first, as cabin pressure changes and dehydration may be more significant concerns.

How long is too long a flight with neuropathy?
There's no universal cutoff, but flights over 4 to 6 hours generally require more active management. Mayo Clinic Connect members with neuropathy report that flights under 3 to 4 hours are often manageable with basic precautions; flights over 6 hours require more intentional movement, hydration, and seat selection strategies.
Do compression socks help with neuropathy on flights?
Yes — this is one of the most consistently recommended interventions by neurologists and neuropathy advocates for air travel. Compression socks improve venous return, reduce swelling, and help maintain circulation during prolonged sitting. Choose graduated compression of 15–20 mmHg for most patients.
Can I bring my neuropathy medications on a plane?
Yes. You are allowed to bring prescription medications in your carry-on. Keep them in their original labeled containers. Liquid medications over 3.4 oz may need declaration at security. A letter from your physician stating your medications and medical condition can be helpful for international travel or if questioned.
What should I do if my neuropathy flares up during a flight?
Stand and walk the aisle as soon as you can safely do so. While seated, perform ankle circles and calf raises to pump blood back through the legs. Apply any topical treatment you have (lidocaine, capsaicin cream) if appropriate. Drink water. Adjust your position. If pain becomes severe and unmanageable, alert a flight attendant — they can assist with positioning accommodations and have basic medical supplies on board.
You Don't Have to Stop Traveling
Neuropathy changes how you travel — it doesn't have to end it. With an aisle seat, compression socks, consistent movement, and good hydration, most neuropathy patients can manage long flights comfortably enough to keep seeing the world.
The key is planning. The patients who struggle most are those who board a 12-hour flight with no preparation and wonder why it was terrible. The ones who thrive are those who treat the flight as a managed medical situation with a clear protocol — and follow that protocol even when they feel okay.
For more on keeping active and mobile with neuropathy, see our balance and fall prevention guide and our best shoes for neuropathy review — both relevant for travel days that go beyond just the flight. And for day-to-day living strategies, browse our complete natural remedies guide.
This article is for educational purposes only and does not constitute medical advice. Consult your neurologist before making changes to your medication regimen for travel.


