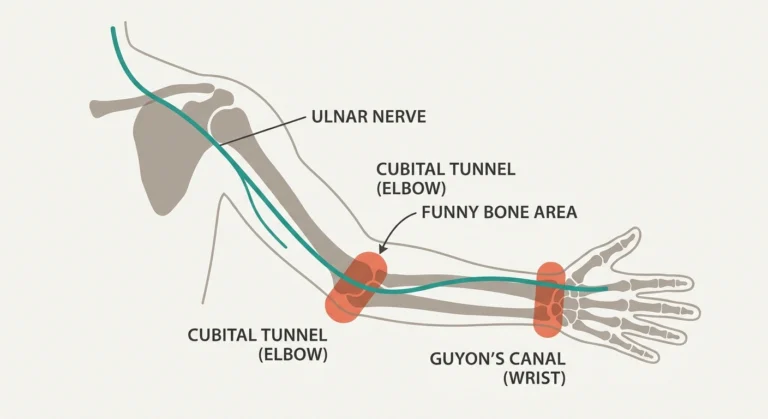
Lyme Disease and Neuropathy: The Nerve Damage Connection
Lyme disease enters the neuropathy conversation in two very different ways. In the clean version, a person gets Lyme, the infection affects the nervous system, and they develop numbness, shooting pain, weakness, or facial palsy that makes clinical sense. In the messy version, someone has chronic nerve symptoms years later and wonders whether Lyme explains everything. Those are not the same scenario, and treating them as identical creates confusion fast.
The reality is that Lyme disease can affect the peripheral nervous system. But the pattern, timing, and evidence matter. Early neurologic Lyme disease is well recognized. Some late peripheral neuropathy claims are more controversial, especially in North American literature. This article gives you the evidence-based middle ground: what Lyme-related nerve problems look like, how they are diagnosed, where recovery is common, and where over-attribution becomes a problem.
How Lyme Disease Can Affect Nerves
Lyme disease is caused by Borrelia infection transmitted by infected ticks. When the nervous system gets involved, symptoms may come from cranial nerves, peripheral nerves, nerve roots, or — less commonly — the central nervous system. The CDC highlights facial palsy, radiculoneuritis, meningitis symptoms, numbness, pain, and weakness as common neurologic patterns in early disseminated disease.
That means Lyme-related nerve problems often look different from the classic length-dependent peripheral neuropathy pattern you see with diabetes. Instead of a slow, symmetric stocking-glove spread, people may have severe shooting limb or trunk pain, facial weakness, or a more acute neurologic picture. If you need the classic baseline pattern for comparison, review what neuropathy feels like.
What Lyme Neuropathy Symptoms Can Look Like
- Sharp or shooting radicular pain in an arm, leg, or around the trunk
- Numbness or tingling in the limbs
- Weakness in affected areas
- Facial palsy or facial droop
- Meningitis-type symptoms such as headache, stiff neck, or light sensitivity when CNS-adjacent involvement is present
This matters because “Lyme neuropathy” is often used loosely online. Some of the most recognized neurologic Lyme presentations are radiculoneuritis and facial palsy rather than a quiet, chronic, symmetric foot neuropathy. The symptom map tells you a lot about whether Lyme is a strong fit or just one theory among many.
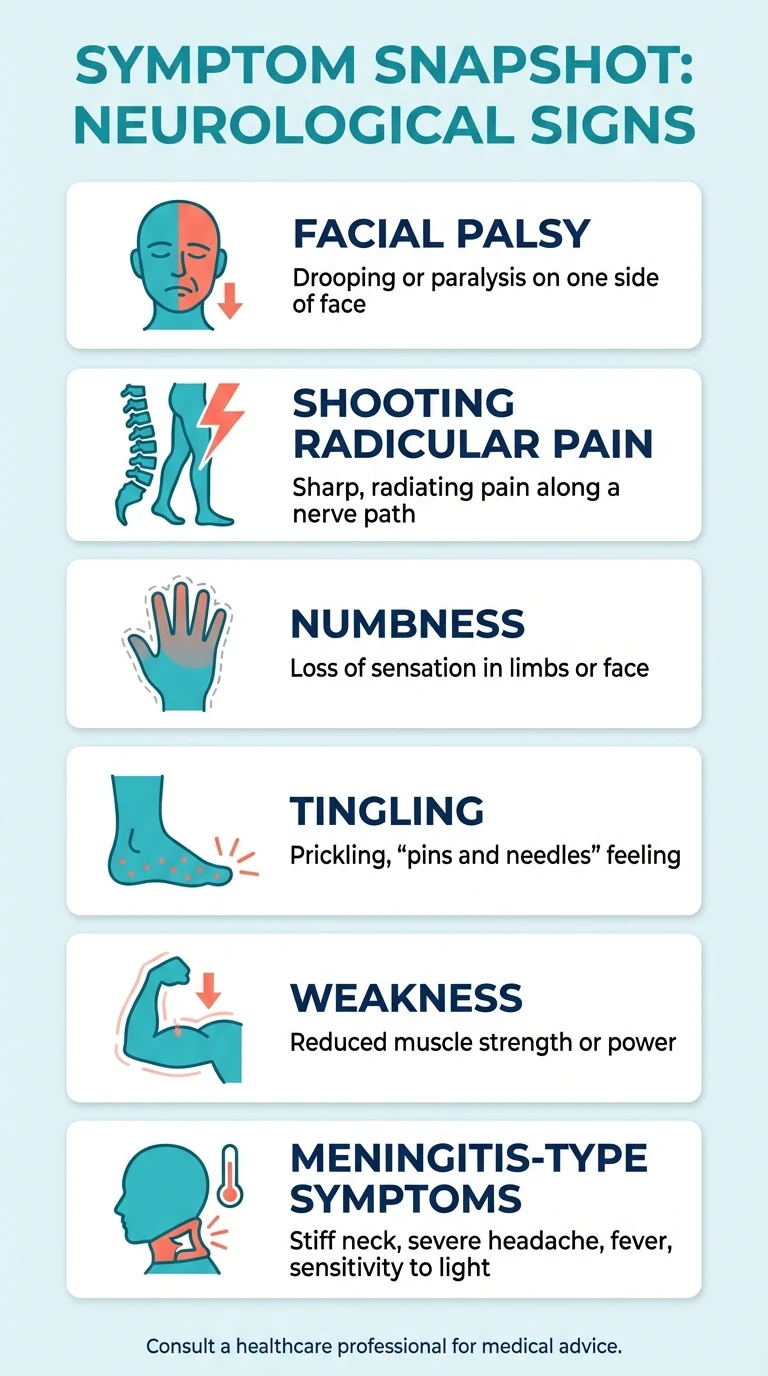
Common neurologic Lyme patterns
- Facial palsy
- Radicular pain
- Numbness and tingling
- Limb weakness
- Meningitis-type symptoms in some cases
Diagnosis: Exposure Risk, Pattern, and Proper Testing
The best Lyme-neuropathy workup starts with context. Do you live in or travel to an endemic area? Was there a tick bite, rash, flu-like phase, joint symptoms, or later neurologic pattern that fits? If the timeline and geography are weak, the odds change.

Diagnosis is a pattern problem
Lyme history, exposure geography, symptom timing, and proper two-step testing matter more than vague internet checklists.
From there, the CDC recommends two-step serologic testing. Neurologic exam matters too, and in selected cases clinicians may use EMG / nerve conduction studies or other testing to separate Lyme-related neuropathic patterns from conditions like toxic neuropathy, diabetic neuropathy, or idiopathic neuropathy. The key is not to skip straight from “I have tingling” to “it must be Lyme.”
Treatment and Recovery Outlook
The encouraging part is that many people with neurologic Lyme disease respond well to antibiotics. The CDC notes that most people recover fully, especially when treatment happens earlier. Facial palsy is usually treated with oral antibiotics, while Lyme meningitis or radiculoneuritis may be treated with oral or intravenous antibiotics depending on severity.

Recovery is still nerve recovery — which means it can lag behind the infection timeline. Pain may calm before sensation fully normalizes. Residual symptoms can hang around for a while even after the infection has been treated. That is one reason the bigger prognosis question always matters: see neuropathy prognosis and can neuropathy be reversed for the more general recovery rules.
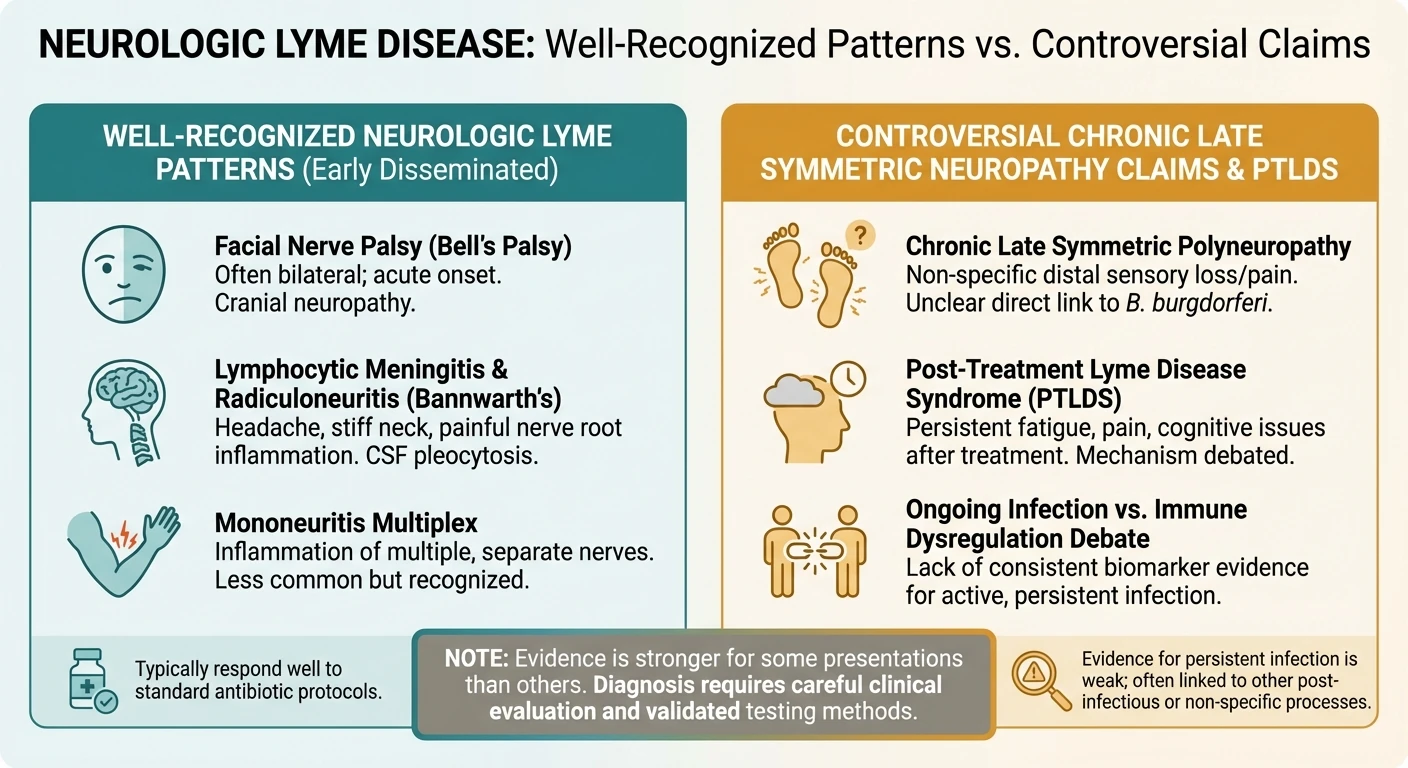
Where the Literature Gets Controversial
Here is the part that deserves honesty. Older studies described a mild chronic distal symmetric sensory neuropathy in late Lyme disease, but more recent appraisal argues that this entity in North America is controversial and may be far less established than many people assume. That does not mean Lyme never affects nerves. It means the strongest evidence is for recognized neurologic Lyme patterns, not for using Lyme as a catch-all explanation for every unexplained chronic neuropathy case.
Important nuance
Lyme can absolutely affect nerves. But late chronic symmetric distal neuropathy as a broad North American catch-all remains controversial, so keep the differential honest.
That distinction protects patients from two bad outcomes: missing real Lyme when it is present, and missing other causes because Lyme became the default story. Good medicine resists both errors.
What to Do If You Think Lyme Is Affecting Your Nerves
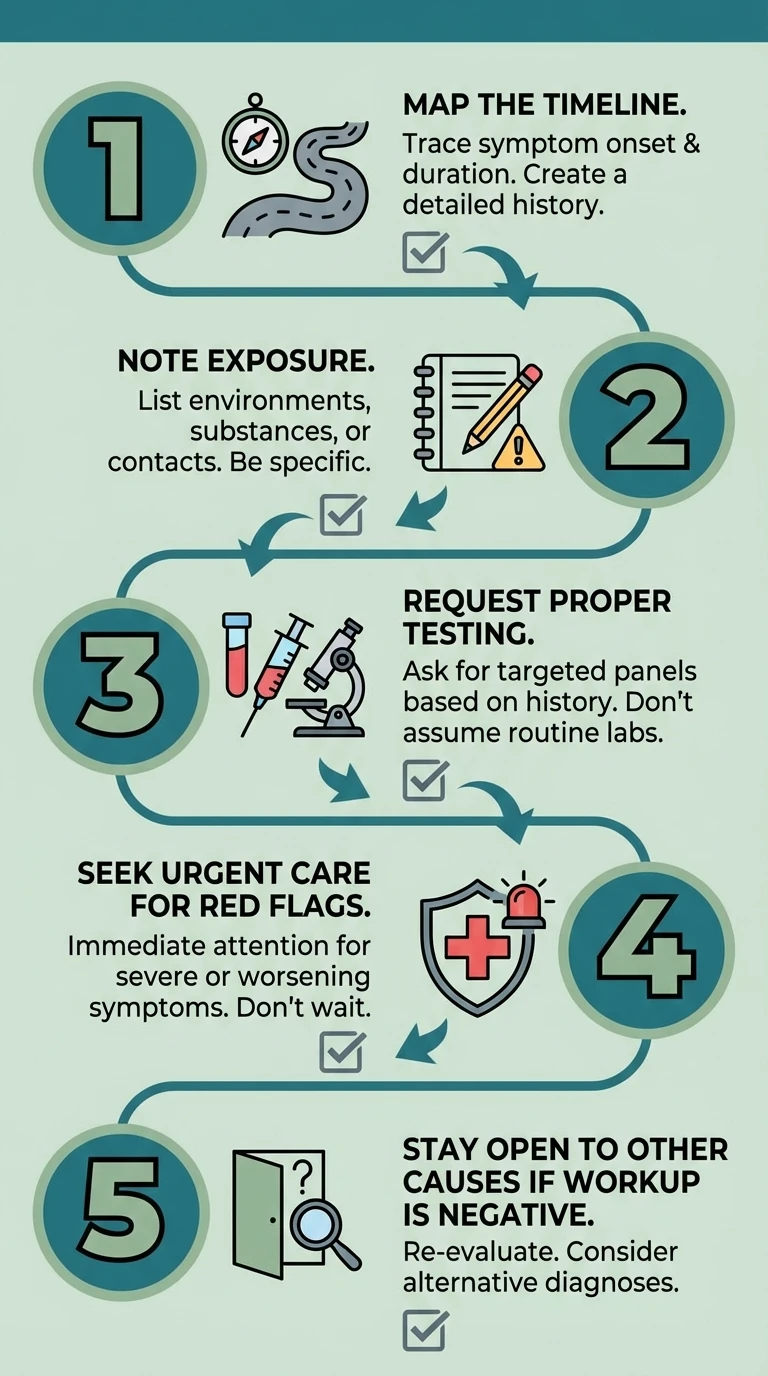
- Map the timeline: rash, tick exposure, early illness, then neurologic symptoms
- Tell your clinician where you live or traveled and when symptoms started
- Ask for proper Lyme testing rather than self-diagnosing from forums
- Get evaluated quickly if you have facial weakness, severe radicular pain, or meningitis-type symptoms
- If the workup is negative, stay open to other neuropathy causes rather than force-fitting the answer
The smartest frame is simple: Lyme disease can absolutely affect nerves, but the pattern should fit. If it does, treatment matters early. If it does not, keep the differential broad and return to a structured workup through diagnosis and cause-based evaluation.
Next moves
Frequently Asked Questions
Can Lyme disease cause neuropathy?
Yes. Lyme disease can affect peripheral nerves and may cause radicular pain, numbness, tingling, weakness, or facial nerve palsy. The timing and pattern matter, and not every burning or tingling symptom automatically means Lyme.
Is Lyme neuropathy permanent?
Not always. Many people improve with timely antibiotic treatment, especially in earlier neurologic Lyme disease. Delayed treatment can leave more persistent symptoms or residual nerve problems.
What does Lyme neuropathy usually feel like?
People may describe shooting radicular pain, numbness, tingling, weakness, or facial weakness. In some cases the pattern is more radiculoneuritis than a classic symmetric stocking-glove neuropathy.
How is Lyme neuropathy diagnosed?
Diagnosis usually relies on clinical history, exposure risk, symptom pattern, and recommended two-step Lyme serologic testing. In selected cases, neurologic exam, EMG, or other tests may help sort out what is happening.
Can chronic neuropathy years later definitely be blamed on Lyme disease?
Not automatically. Late or chronic distal symmetric Lyme neuropathy in North America is controversial in the literature, so it is important not to force every unexplained neuropathy into a Lyme story without evidence.