
The question comes up more than you might think in our support groups: “I have neuropathy — can I still have a glass of wine with dinner?” It's a fair question, and it deserves a more nuanced answer than most articles provide. The relationship between alcohol and neuropathy isn't as simple as “all alcohol is bad” — but it's also more serious than many people realize.
Alcohol affects your nerves in two distinct ways: directly, as a neurotoxin that can damage nerve fibers, and indirectly, by depleting the vitamins your nerves need to stay healthy. How much alcohol it takes to cause problems depends on factors like how long you've been drinking, your nutritional status, your genetics, and whether you already have nerve damage from another cause like diabetes.
This article breaks down what the research actually tells us about alcohol and neuropathy — the amounts that seem to matter, how alcohol damages nerves, who's most at risk, and what you can realistically do if you enjoy a drink but also live with nerve pain.
How Alcohol Damages Your Nerves
Understanding how alcohol affects the nervous system requires looking at two separate but related mechanisms. Both contribute to nerve damage, and in many heavy drinkers, both are happening simultaneously.
of people with chronic alcohol use disorder develop some form of neuropathy
Direct Toxic Effects
Alcohol and its metabolites — particularly acetaldehyde — are directly toxic to nerve tissue. When alcohol is broken down in your body, it generates free radicals that cause oxidative stress on nerve cells. This damages the axons (the long fibers that carry signals) and can also degrade the myelin sheath (the protective coating around nerves that helps signals travel quickly).
Research has shown both axonal degeneration and demyelination in the nerves of chronic heavy drinkers. The damage typically starts in the longest nerves first — those reaching your feet and toes — which is why alcoholic neuropathy almost always begins in the lower extremities.
The direct toxic effect appears to be dose-dependent and cumulative. It's not one bad night that causes neuropathy — it's the ongoing, repeated exposure over months and years that gradually wears nerves down.
Nutritional Depletion
Alcohol interferes with your body's ability to absorb, process, and store several vitamins that are essential for nerve health — and this may be just as damaging as the direct toxic effects.
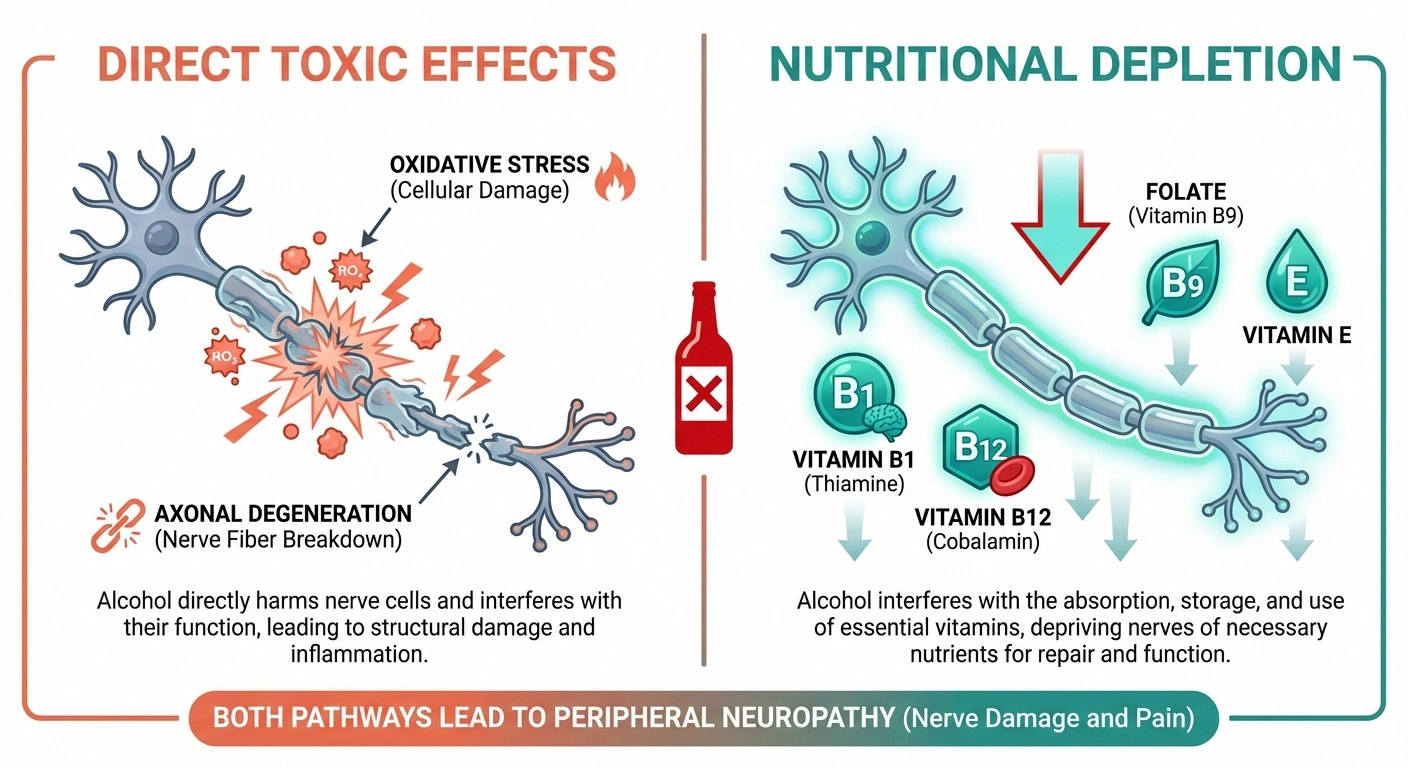
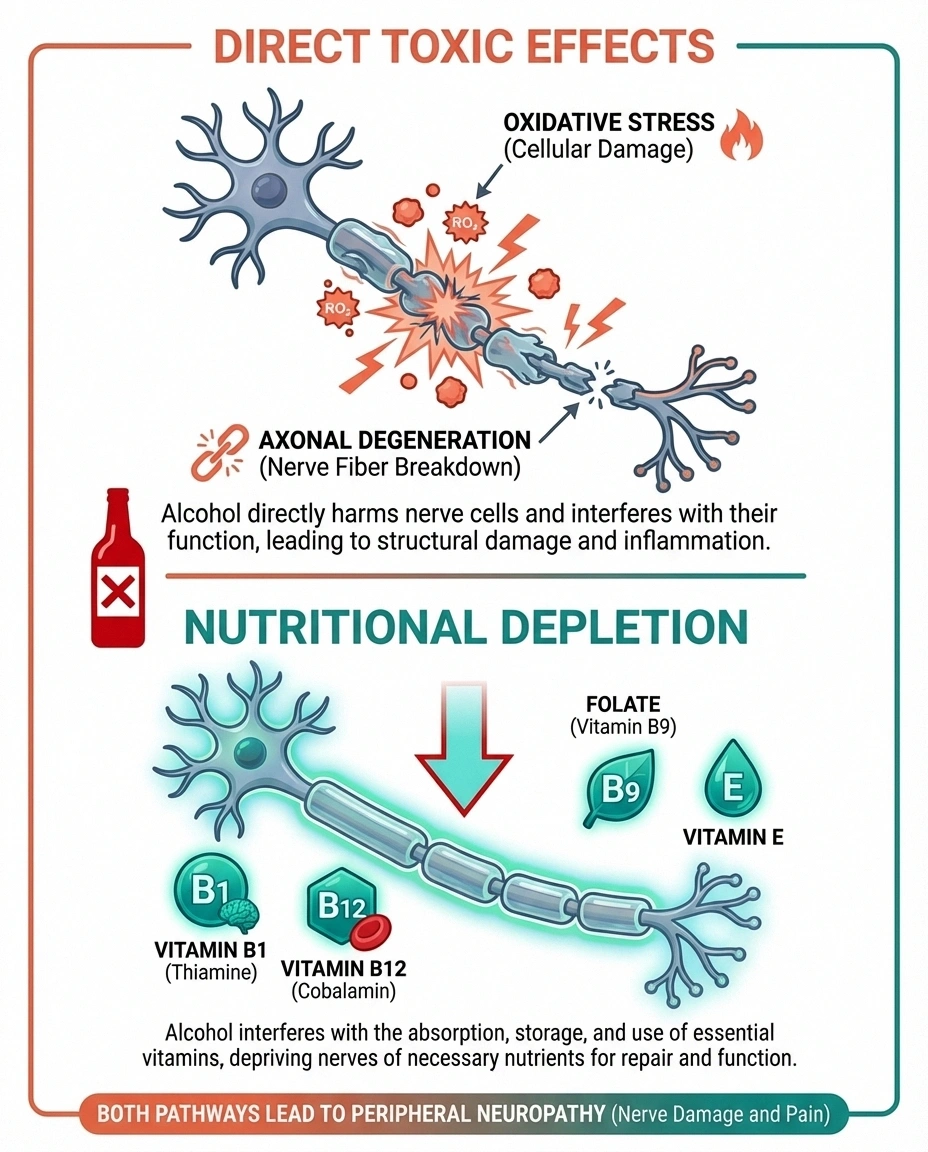
Thiamine (vitamin B1) is the most critical. Alcohol impairs thiamine absorption in the gut, reduces its storage in the liver, and increases its excretion. Thiamine is essential for energy metabolism in nerve cells — without it, nerves essentially starve. Severe thiamine deficiency can cause a condition called Wernicke-Korsakoff syndrome, but even moderate deficiency can contribute to peripheral neuropathy.
Other vitamins affected by alcohol include B12, B6, folate, and vitamin E — all of which play roles in nerve maintenance and repair. Heavy drinkers are also more likely to have poor diets overall, compounding the nutritional problem.
This dual mechanism — direct toxicity plus nutritional depletion — is why alcohol-related neuropathy can be so difficult to untangle. Scientists have debated for decades whether the nerve damage comes primarily from the alcohol itself or from the resulting malnutrition. The current consensus, supported by a thorough review published in the journal Muscle & Nerve, is that both contribute significantly.
How Much Alcohol Is Too Much for Your Nerves?
This is the question everyone wants answered — and unfortunately, there isn't a single clear threshold that applies to everyone. But the research does give us some useful guidance.
Research Says
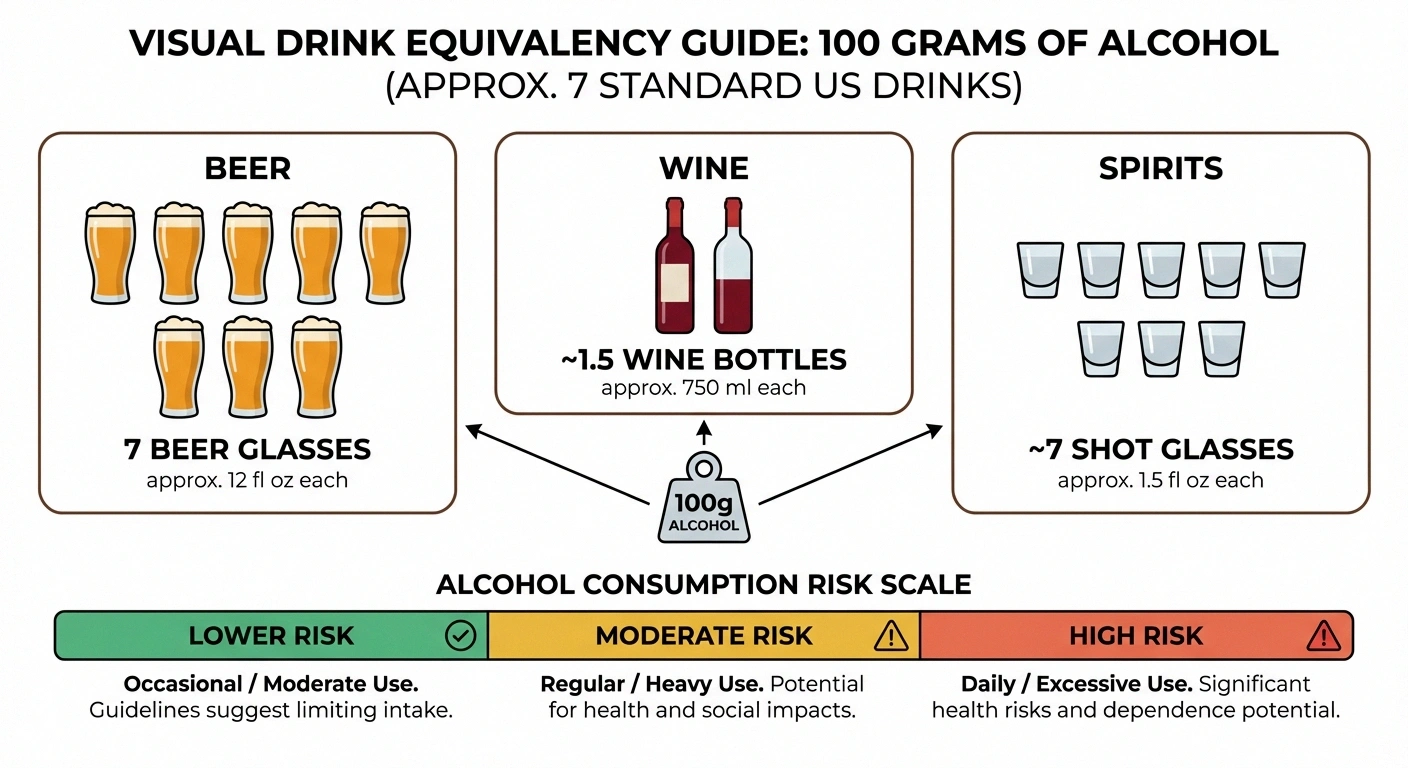
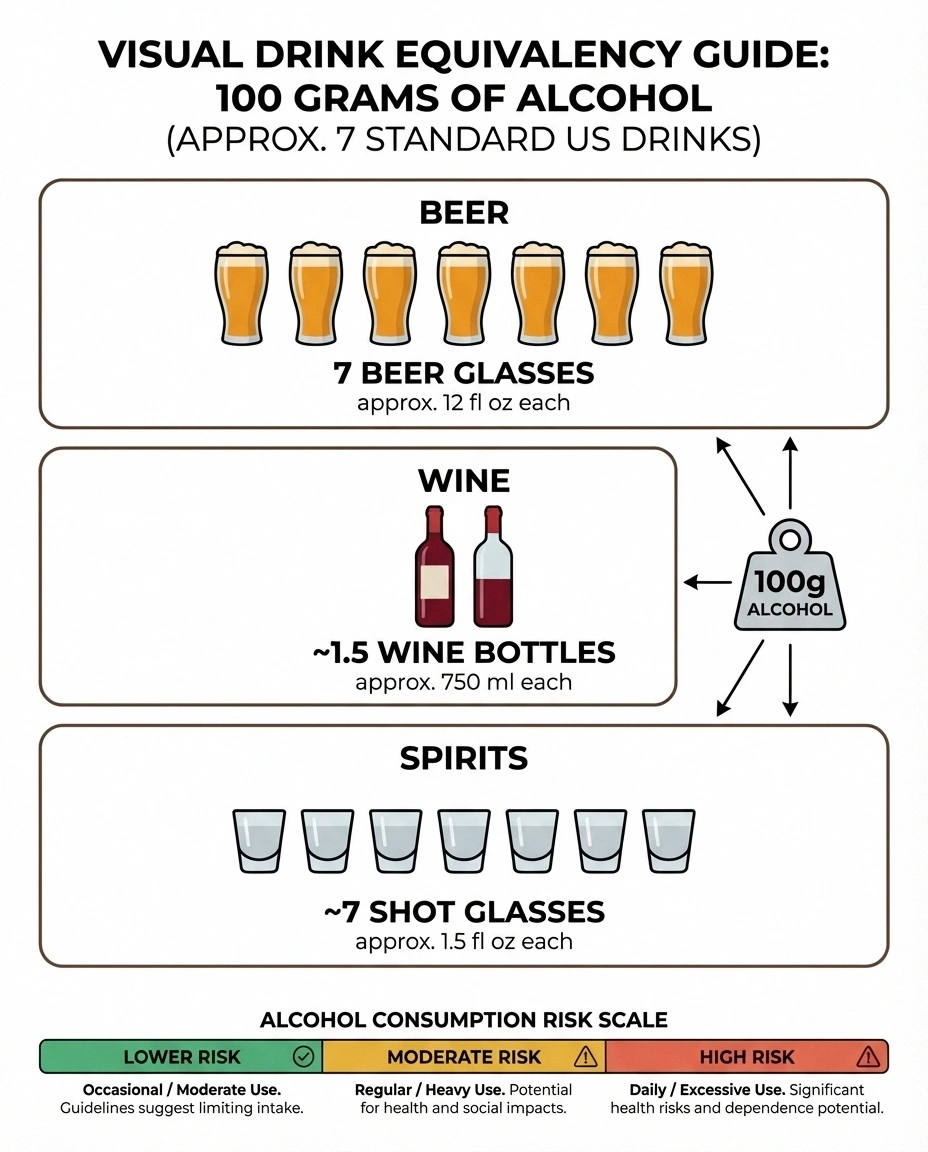
Clinical neuropathy is most commonly associated with consuming more than 100 grams of alcohol per day (about 7 standard US drinks) over many years. But lower amounts can still affect already-damaged nerves, and duration of drinking matters as much as daily quantity.
The clinical threshold. Studies of alcoholic neuropathy have consistently found that significant nerve damage is most commonly associated with consuming more than 100 grams of alcohol per day over a period of years. To put that in perspective, 100 grams of alcohol is roughly equivalent to:
- Seven standard drinks (in the US, where one standard drink = ~14 grams)
- About a bottle and a half of wine
- About six pints of regular beer
That's well beyond what most people would consider casual drinking — and if your consumption is nowhere near this level, that's genuinely reassuring.
But lower amounts aren't necessarily safe. The 100-gram figure comes from studies looking at when clinically diagnosable neuropathy develops. That doesn't mean lower amounts can't affect your nerves at all, especially if:
- You already have neuropathy from another cause (diabetes, chemotherapy, etc.)
- You have nutritional deficiencies
- You're taking medications that also affect the nervous system
- You have genetic factors that make your nerves more vulnerable
Duration matters as much as quantity. Alcoholic neuropathy is strongly correlated with the length of drinking history, not just the daily amount. A 2024 study in Clinical Neurophysiology Practice found that subjects with neuropathy had significantly longer durations of alcohol abuse than those without — even when daily amounts were similar.
Continuous drinking is worse than episodic. Research has found that people who drink every day are more likely to develop neuropathy than those who drink the same total amount but with breaks in between. The constant exposure gives nerves no time to recover.
Women may be more vulnerable. Studies suggest that women develop alcohol-related neuropathy with shorter durations of abuse and at lower consumption levels than men. The neuropathy also tends to be more severe. This may be related to differences in body composition, liver metabolism, and hormonal factors.
If You Already Have Neuropathy: What Alcohol Does to Existing Nerve Damage
This section is for the large number of people who have neuropathy from another cause — diabetes, chemotherapy, idiopathic causes, autoimmune conditions — and are wondering whether alcohol makes their existing condition worse.

Medication Warning
Many neuropathy medications — including gabapentin, pregabalin, duloxetine, and amitriptyline — interact with alcohol, causing increased drowsiness, impairment, and fall risk. Check every medication label for alcohol warnings, and ask your pharmacist for a comprehensive interaction check.
The honest answer is: probably yes, to some degree, even at moderate levels.
When your nerves are already damaged, they have less reserve capacity. The nutritional depletion and oxidative stress caused by even moderate alcohol consumption hits harder because the nerves are already compromised. Think of it like a fraying rope — it takes less additional strain to break it.
More specifically, alcohol can:
- Worsen blood sugar control — particularly problematic if your neuropathy is diabetes-related. Alcohol can cause blood sugar spikes and crashes, and poor glucose control is the primary driver of diabetic nerve damage.
- Interfere with neuropathy medications — many neuropathy drugs come with specific warnings about alcohol. gabapentin for nerve pain, pregabalin, and duloxetine all interact with alcohol, primarily through increased drowsiness and impairment, but also potentially reducing the medication's effectiveness.
- Increase fall risk — if you have balance problems from neuropathy, even one or two drinks can significantly increase your risk of falling. Alcohol impairs coordination in everyone; when your proprioception is already compromised by nerve damage, the combination can be dangerous.
- Disrupt sleep quality — alcohol may help you fall asleep initially but disrupts deep sleep cycles later in the night. Since neuropathy symptoms often worsen at night, anything that reduces sleep quality can create a cascade of increased pain and fatigue.
- Add nutritional stress — even moderate drinking depletes B vitamins and increases inflammation. If your nerves are already struggling, this additional nutritional burden can slow any recovery process.
This doesn't necessarily mean you can never have a drink. But it does mean the decision should be made with eyes open about the real trade-offs involved.
Signs That Alcohol May Be Affecting Your Nerves
How do you know if alcohol is contributing to your neuropathy symptoms? Here are warning signs to watch for:

Is Alcohol Affecting Your Nerves?
Neuropathy symptoms worsen within 24-48 hours after drinking
Pain is symmetrical — both feet affected equally
More burning and shooting pain than numbness alone
Balance and coordination problems seem worse than neuropathy alone would explain
Symptoms improve when you stop drinking for a few weeks
If you checked 2 or more, consider discussing alcohol's role in your neuropathy with your doctor and tracking your consumption alongside symptoms.
Symptoms that worsen after drinking. If you notice increased burning, tingling, or pain in the 24 to 48 hours after having drinks, that's a meaningful signal. Some people track this and discover a clear pattern they'd never noticed before.
Symptoms concentrated in feet and lower legs. Alcohol-related neuropathy is almost always a symmetrical, length-dependent polyneuropathy — meaning it affects both sides equally and starts in the feet, gradually moving upward. If your symptoms match this pattern and you drink regularly, alcohol may be a factor.
More pain than numbness. A distinctive feature of alcohol-related neuropathy is that it tends to be painfully sensitive rather than simply numb. Burning feet, sharp shooting pains, and hypersensitivity to touch are common presentations.
Gait and balance problems. If you're noticing increasing difficulty with walking, coordination, or balance — particularly unsteadiness that seems worse than your neuropathy alone would explain — alcohol's effects on the cerebellum (balance center) may be compounding the neuropathy.
Symptoms improving during abstinent periods. If your neuropathy symptoms genuinely improve when you stop drinking for a few weeks and worsen when you resume, that's strong evidence that alcohol is a contributing factor.
Making Informed Choices: A Practical Guide
If you have neuropathy and choose to drink, here's a practical framework for minimizing the impact on your nerves:
Keep it occasional, not daily. The research consistently shows that continuous daily drinking is more damaging than the same amount spread over fewer occasions with breaks. If you currently drink every day, even cutting to weekends only may reduce the toll on your nerves.
Stay well within moderate limits. For people with existing neuropathy, the general moderate drinking guidelines (up to one drink per day for women, up to two for men) represent an upper boundary, not a target. Many neurologists would recommend staying below even these levels.
Protect your nutrition aggressively. If you do drink, supporting your body's nutritional reserves becomes even more important. A B-complex supplement, adequate folate intake, and a nerve-healthy diet can help offset some (but not all) of alcohol's nutritional effects. Talk to your doctor about whether a targeted supplement regimen makes sense for you.
Avoid drinking on empty stomachs. Food slows alcohol absorption, reducing peak blood alcohol levels and the intensity of the toxic spike your nerves experience. If you do have a drink, have it with a meal.
Check your medication interactions. Review every medication you take for alcohol warnings. This is especially important with neuropathy medications, pain medications, sleep aids, and any psychiatric medications. Your pharmacist can provide a comprehensive interaction check.
Hydrate deliberately. Alcohol is a diuretic that dehydrates your body, and dehydration can worsen neuropathy symptoms. Alternate alcoholic drinks with water, and drink extra water before bed.
Track the connection. Keep a simple log noting when you drink, how much, and how your neuropathy symptoms are the following day. After a month, patterns often become clear that you wouldn't have noticed otherwise.
When It's Time to Stop Completely
For some people, the right answer is complete abstinence. This isn't about moral judgment — it's about medical reality. Consider stopping entirely if:
🛑 Consider Stopping If:
- Neuropathy is alcohol-related
- Symptoms are progressing
- You can't control how much you drink
- Strong medication warnings
- Existing liver damage
✓ If You Choose to Drink:
- Keep it occasional, not daily
- Stay well below moderate limits
- Supplement B vitamins
- Always eat before drinking
- Track symptoms afterward
- Your neuropathy is diagnosed as alcohol-related — Stopping is the single most important treatment step. Research shows that many people experience stabilization or even partial reversal of symptoms after sustained abstinence.
- Your symptoms are progressing — If your neuropathy is getting worse despite treatment, removing every possible contributing factor — including alcohol — becomes more important.
- You have difficulty controlling how much you drink — If one glass reliably turns into three or four, moderate drinking isn't a realistic option. The CAGE questionnaire (Have you ever felt you should Cut down? Have people Annoyed you by criticizing your drinking? Have you felt Guilty? Have you needed an Eye-opener?) is a useful self-assessment.
- You're taking medications with strong alcohol warnings — The risk of dangerous interactions may outweigh any enjoyment from drinking.
- You have liver damage or other alcohol-related health conditions — Your body's ability to metabolize alcohol safely is already compromised.
If you do decide to stop and you've been drinking heavily for a long time, talk to your doctor first. Alcohol withdrawal can be medically dangerous in heavy drinkers and may require supervised detoxification. This is not a situation for cold turkey without medical guidance.
Recovery: Can Nerve Damage from Alcohol Be Reversed?
The encouraging news is that alcohol-related neuropathy has a better prognosis than many other forms of nerve damage — if you stop or significantly reduce drinking early enough.

Key Takeaway
Alcohol-related nerve damage has a better prognosis than many other forms of neuropathy — especially when caught early. Stopping alcohol, replacing depleted vitamins (particularly thiamine), and maintaining good nutrition can lead to meaningful improvement over months. Even partial recovery is a worthwhile outcome.
When the damage is primarily nutritional (thiamine and other vitamin deficiencies), replacing those nutrients while stopping alcohol can lead to meaningful improvement. Some people notice changes within weeks of supplementation and abstinence, though full recovery — if it occurs — typically takes months to years.
When the damage is from direct alcohol toxicity to the nerve fibers, recovery is slower and less complete. Peripheral nerves can regenerate, but they do so at roughly one millimeter per day — which means nerves reaching from your spine to your feet may need 12 to 18 months to regrow, even under ideal conditions.
Factors that affect recovery include:
- How early you stop — The earlier you address the problem, the more reversible the damage tends to be. Advanced neuropathy with significant axonal loss may not fully recover.
- Nutritional support — Aggressive vitamin supplementation (under medical supervision) can accelerate recovery. Thiamine is the priority, but B12, folate, and other B vitamins matter too.
- Overall health — Good blood sugar control, regular exercise, and adequate sleep all support nerve regeneration.
- Abstinence sustainability — Periods of recovery followed by resumed heavy drinking are worse than continuous moderate consumption. Consistency matters.
Even if full recovery isn't possible, most people who stop drinking experience at least stabilization — the neuropathy stops getting worse, which is a significant outcome in itself. And the improvements in sleep, energy, mental clarity, and overall health that come with reducing alcohol often improve quality of life even before the nerves themselves begin to heal.
Frequently Asked Questions
Is one glass of wine per day safe if I have neuropathy?
For most people with non-alcohol-related neuropathy, an occasional glass of wine is unlikely to cause significant additional nerve damage. However, even moderate alcohol consumption can worsen symptoms in the short term, interfere with neuropathy medications, increase fall risk, and deplete nerve-supporting vitamins. There's no amount that's been proven safe for nerves — only amounts that haven't been proven harmful in research.
How quickly does alcohol-related nerve damage develop?
Alcoholic neuropathy typically develops over years of heavy drinking, not weeks or months. Studies indicate that duration of alcohol use is as important as the daily amount. However, people who already have nerve damage from other causes may notice alcohol worsening their symptoms much more quickly.
Can I reverse alcoholic neuropathy if I stop drinking?
Partial or full recovery is possible, particularly if the damage is caught early and is primarily nutritional in nature. Stopping alcohol, replacing depleted vitamins (especially thiamine), and maintaining good nutrition can lead to meaningful improvement over months. Advanced neuropathy with significant nerve fiber loss may stabilize but not fully reverse.
Does beer cause more or less neuropathy than liquor?
The type of alcoholic beverage matters less than the total amount of alcohol consumed. Beer, wine, and spirits all contain ethanol, which is the substance that damages nerves. A standard drink of beer, wine, or liquor contains roughly the same amount of alcohol (about 14 grams in the US). However, beer's higher volume may contribute to greater B vitamin depletion through increased urination.
I drink moderately and just got diagnosed with neuropathy. Is alcohol the cause?
Moderate drinking alone is unlikely to be the sole cause of neuropathy. Your doctor will evaluate other potential causes — diabetes, vitamin deficiencies, medications, autoimmune conditions, and more. However, even moderate alcohol use can be a contributing factor alongside other causes, and reducing intake is generally recommended as part of comprehensive neuropathy management.
Should I take B vitamins if I drink and have neuropathy?
It's a reasonable precaution, but talk to your doctor about appropriate doses and formulations. A B-complex supplement that includes thiamine (B1), B6, B12, and folate can help offset some of alcohol's nutritional effects. Keep in mind that supplements can reduce but not eliminate alcohol's direct toxic effects on nerves — they're not a free pass to drink more.
The Bottom Line: Making This Decision for Yourself
Alcohol and neuropathy exist on a spectrum, not a binary. For people who drink heavily, the path is clear — reducing or stopping alcohol consumption is one of the most important things you can do for your nerves. For people who drink moderately and have neuropathy from other causes, the decision is more nuanced and personal.

What I encourage people in my support groups to do is approach this as a data-driven decision rather than an emotional one. Track your drinking and your symptoms. Notice the patterns. Have an honest conversation with your doctor about your specific situation — your type of neuropathy, your medications, your nutritional status, your other risk factors.
If you find that alcohol is genuinely worsening your symptoms, that information is a gift — it means you have a modifiable factor that you can actually control. In a condition where so much feels out of your hands, that's valuable.
And if you're struggling with alcohol use, know that you're not alone and help is available. Your doctor can connect you with resources, and the 24-hour SAMHSA helpline (1-800-662-4357) provides free referrals and support.
For a comprehensive overview of how alcohol damages nerves, read our complete guide to alcoholic neuropathy. To learn about protecting your nerves through nutrition, see our guide to the best neuropathy diet and vitamin deficiency neuropathy.

