Neuropathy and Alcohol: What Happens If You Keep Drinking
I hear from readers all the time who've been diagnosed with peripheral neuropathy and are still wrestling with the same question: “Do I really have to stop drinking completely?” It's an honest question, and I'm not going to judge anyone for asking it. But after years of reading the research and hearing from thousands of people living with nerve damage, I need to be straight with you about what the science says — and what continued drinking actually does to already-damaged nerves.
This isn't another article about what causes alcoholic neuropathy. We've already covered that in our complete guide to alcoholic neuropathy. This article is specifically about what happens next — the progression, the timeline, and the real consequences of continuing to drink when your nerves are already sending you warning signals.
How Alcohol Damages Nerves: The Mechanism You Need to Understand
Before we talk about progression, you need to understand how alcohol damages your peripheral nerves. There are two separate mechanisms working simultaneously, and both get worse the longer you drink.
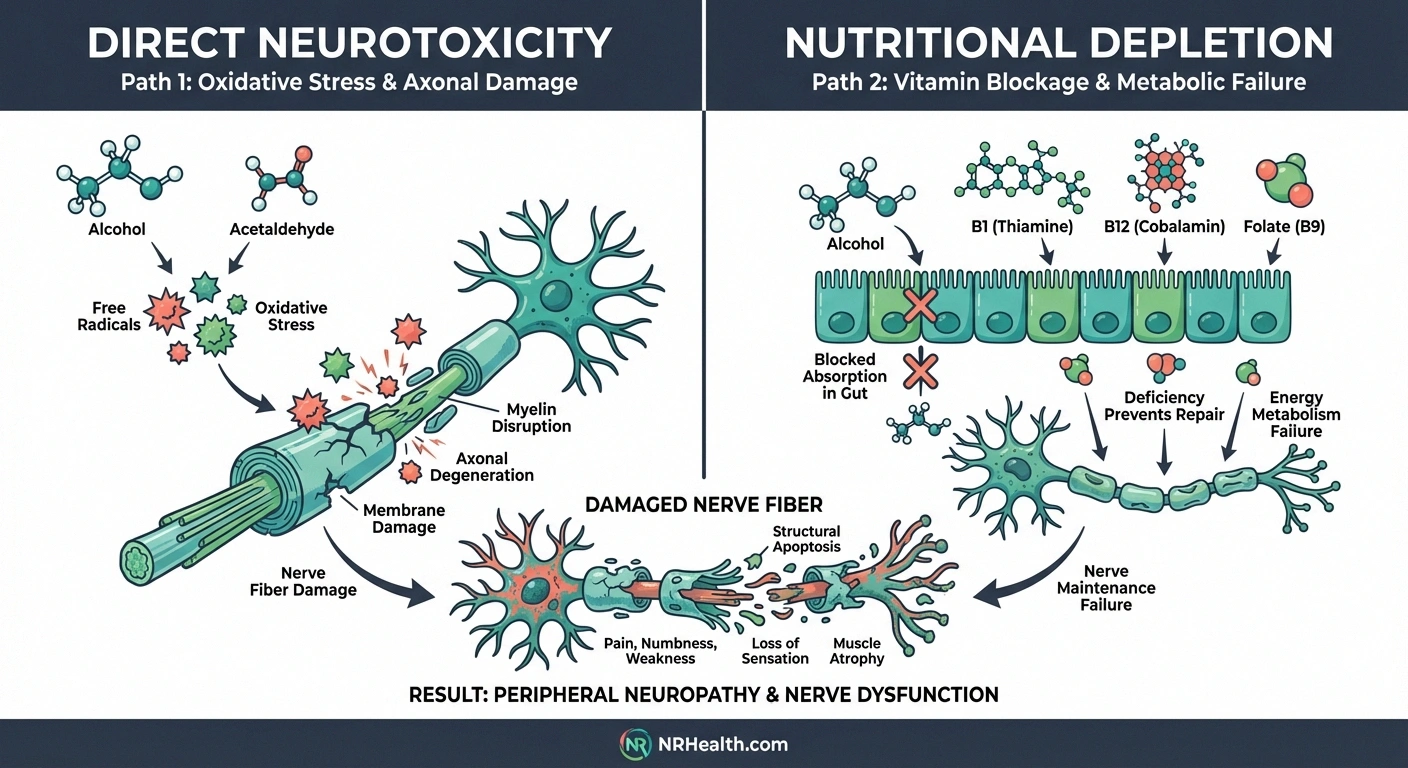
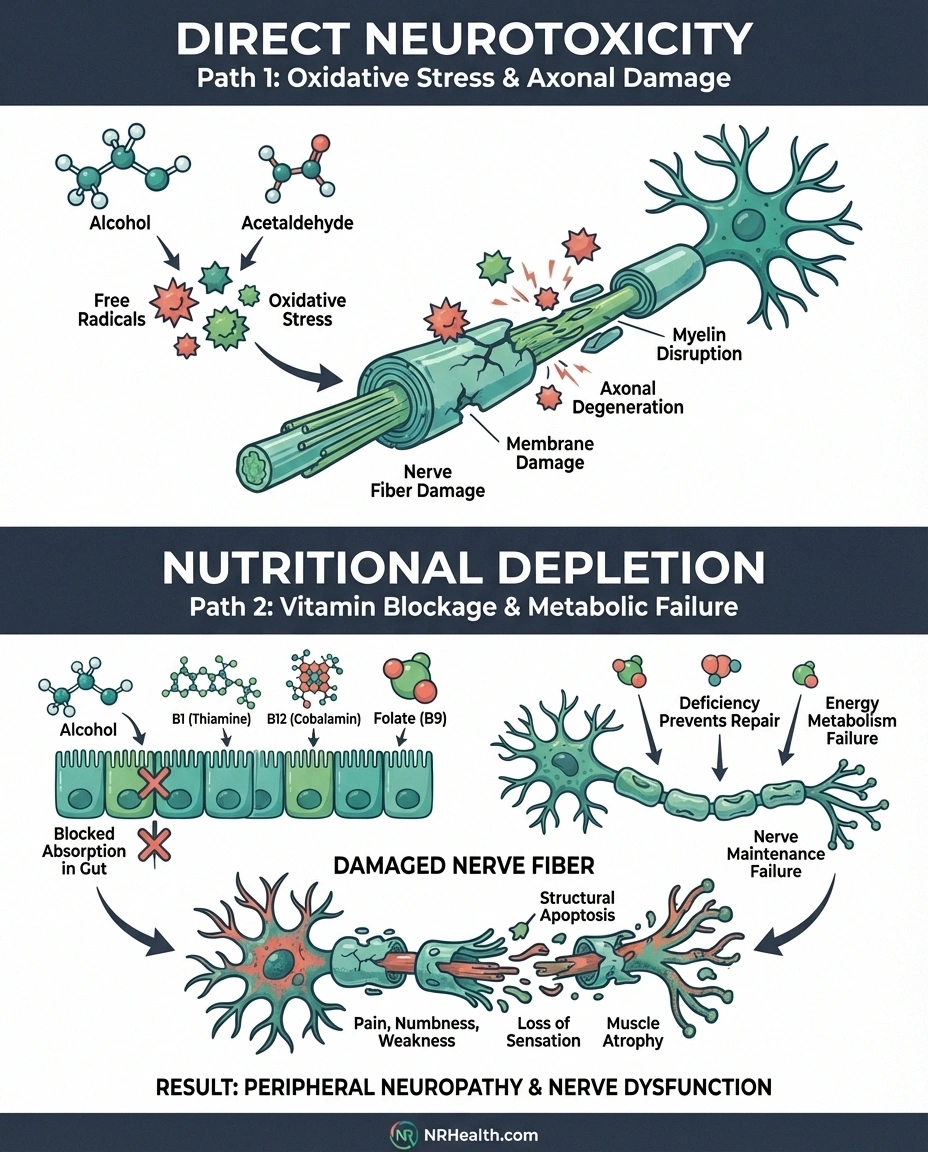
The first is direct neurotoxicity. Alcohol and its metabolite acetaldehyde are toxic to nerve tissue. They damage the axons — the long fibers that carry electrical signals from your spinal cord to your feet and hands. This is called axonal degeneration, and it's the primary pathology researchers find in alcoholic neuropathy. A 2012 review in the Journal of the Peripheral Nervous System confirmed that alcohol-induced oxidative stress generates free radicals that directly damage nerve cell membranes and the proteins nerves need to function.
The second mechanism is nutritional deficiency. Chronic alcohol use impairs your body's ability to absorb thiamine (vitamin B1), folate, vitamin B12, and vitamin E — all nutrients your nerves depend on for maintenance and repair. According to the National Library of Medicine's StatPearls review, up to 80% of people with alcohol use disorder are thiamine-deficient. Without thiamine, your nerves can't maintain their myelin coating — the insulation that keeps electrical signals moving efficiently.
Here's the critical point: these two mechanisms compound each other. Alcohol damages the nerve directly while simultaneously stripping away the nutrients your body needs to repair that damage. It's like punching a hole in a boat while also throwing the repair kit overboard.
The Stages of Alcohol-Related Nerve Damage Progression
Alcoholic neuropathy doesn't happen overnight, and it doesn't progress in a straight line. But researchers have identified a general pattern of how nerve damage unfolds when drinking continues. Understanding these stages of neuropathy may help you recognize where you are — and what's likely coming next.
Early Stage: The Warning Signs (Often Ignored)
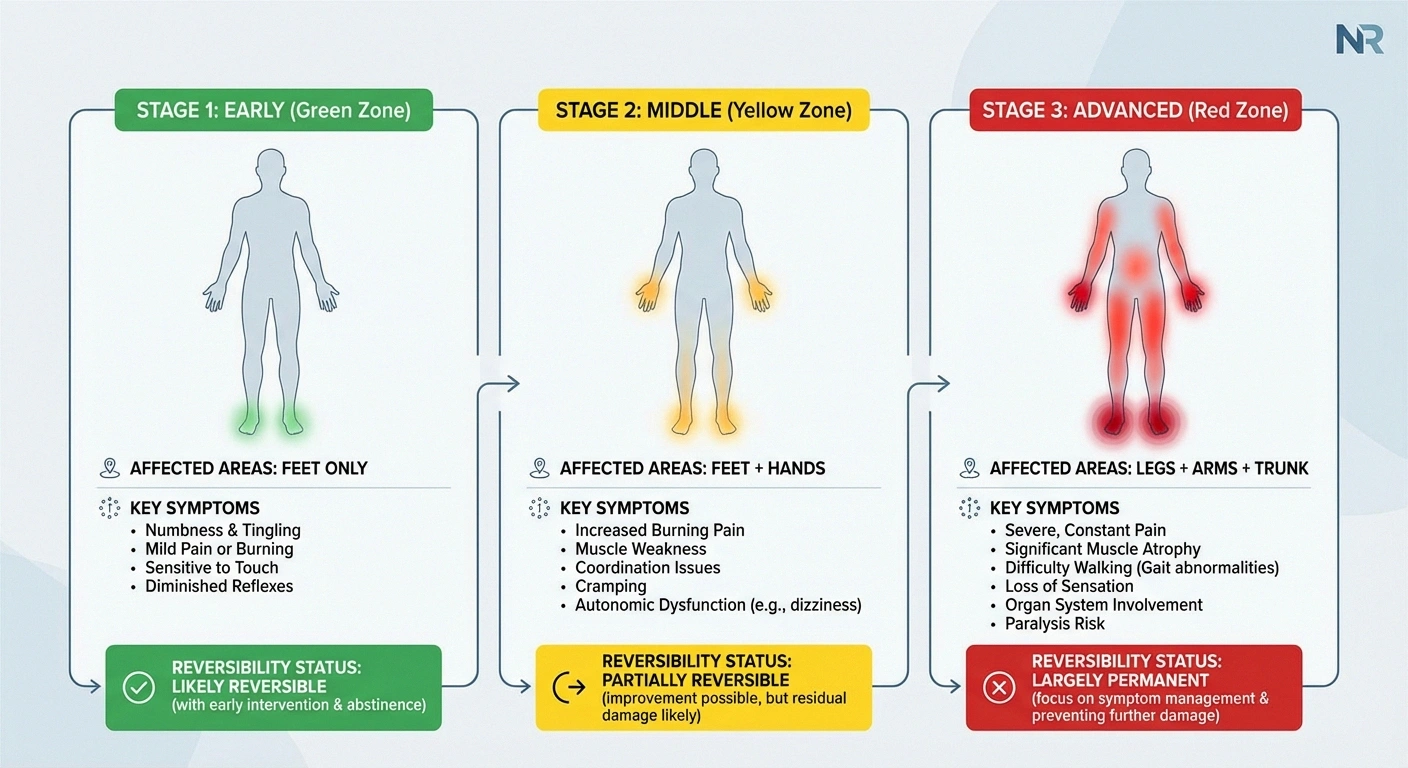
The earliest signs are easy to dismiss. Intermittent tingling or numbness in the toes. A burning sensation on the soles of your feet that comes and goes. Maybe your feet feel oddly cold even when they're not. These symptoms typically appear in the feet first because the longest nerves in your body — the ones running from your spinal cord to your toes — are the most vulnerable to damage.
At this stage, nerve conduction studies may show only subtle changes. Many people chalk these symptoms up to “getting older” or “being on my feet too much.” But if you're drinking heavily and experiencing these sensations, your nerves are sending you a clear message.
Middle Stage: The Damage Becomes Obvious
As drinking continues, symptoms become persistent rather than intermittent. The tingling and burning don't come and go anymore — they're constant companions. Pain often intensifies, described by patients as sharp, stabbing, or like walking on broken glass. Symptoms typically worsen at night, disrupting sleep and creating a cascade of fatigue, depression, and worsening pain.
The sensory changes start creeping upward. What started in the toes moves to the entire foot, then the ankles, then the lower legs. This upward progression — called the “stocking pattern” — is a hallmark of length-dependent neuropathy. Eventually, the fingers and hands join in, creating a “stocking-and-glove” distribution.
Motor symptoms begin to emerge: muscle cramps, weakness in the feet and ankles, and difficulty with balance. You might notice you're tripping more often or that your gait has changed.
Advanced Stage: Severe and Potentially Irreversible
In advanced alcoholic neuropathy, the damage extends well beyond sensory discomfort. Significant muscle wasting can occur in the legs and feet. Walking without assistance becomes difficult or impossible. Complete loss of sensation means you can injure your feet without realizing it — leading to ulcers, infections, and in severe cases, complications similar to those seen in diabetic foot disease.
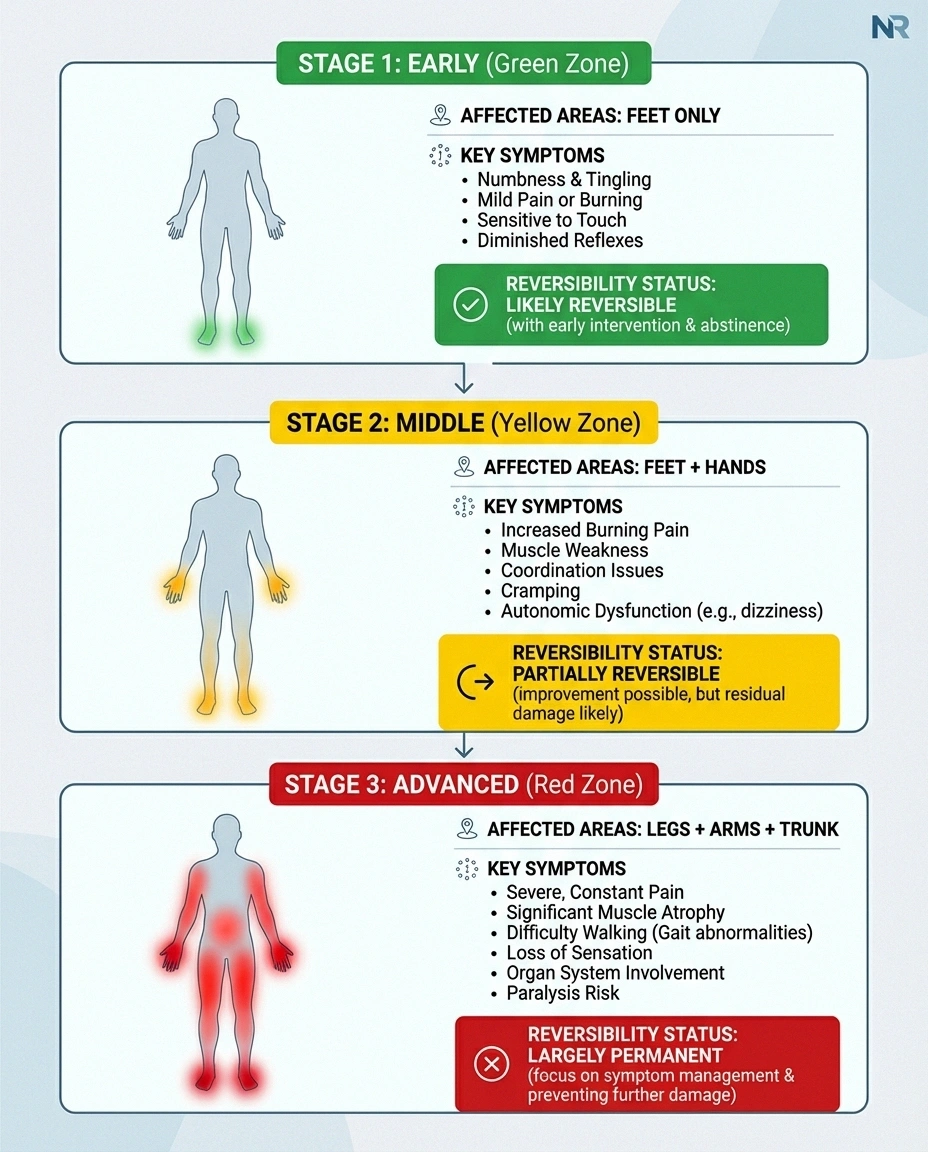
Autonomic nerve involvement may develop, affecting digestion, blood pressure regulation, bladder function, and sexual function. The MedlinePlus medical encyclopedia notes that damage at this stage is “usually permanent” and “likely to get worse if the person continues to use alcohol.”
What the Research Says About Continued Drinking
The research is unambiguous on this point: continuing to drink accelerates nerve damage. There's no “safe amount” of alcohol for someone who already has alcohol-related neuropathy.
A comprehensive review published in the Journal of the Peripheral Nervous System documented that the severity of alcoholic neuropathy correlates with lifetime alcohol consumption. The more you've drunk over your lifetime, the worse the neuropathy tends to be. And every additional drink adds to that lifetime total.
Research from the Mayo Clinic Proceedings (2024) further clarified that alcohol-related neuropathy is primarily a small-fiber neuropathy in its early stages — meaning it attacks the pain-sensing and temperature-sensing nerves first. But with continued exposure, it progresses to involve larger nerve fibers responsible for movement and proprioception (your sense of where your body is in space).
The progression isn't always gradual. Some people experience periods of relative stability punctuated by sudden worsening — often linked to binge drinking episodes, illnesses, or periods of particularly poor nutrition.
The Nutritional Spiral: How Alcohol Creates a Deficiency Trap
One of the most insidious aspects of continued drinking with neuropathy is what I call the nutritional spiral. Alcohol doesn't just deplete your B vitamins — it actively blocks your body from absorbing them, even if you're taking supplements.
Chronic alcohol use damages the lining of your small intestine, reducing absorption of thiamine, folate, B12, and other critical nutrients. It impairs your liver's ability to store and activate these vitamins. And it increases urinary excretion of nutrients your body desperately needs. Even if you eat well and take B vitamin supplements, heavy drinking undermines your body's ability to use them.
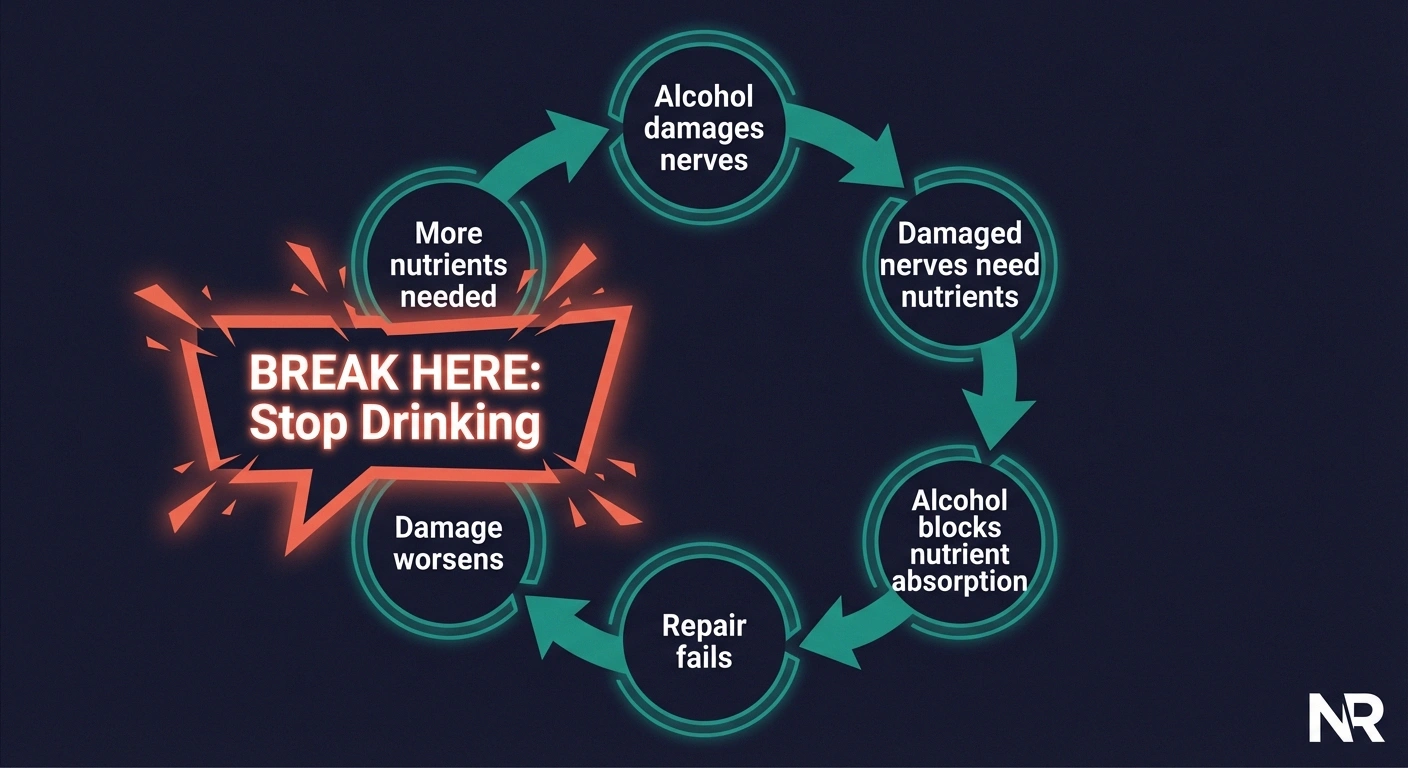
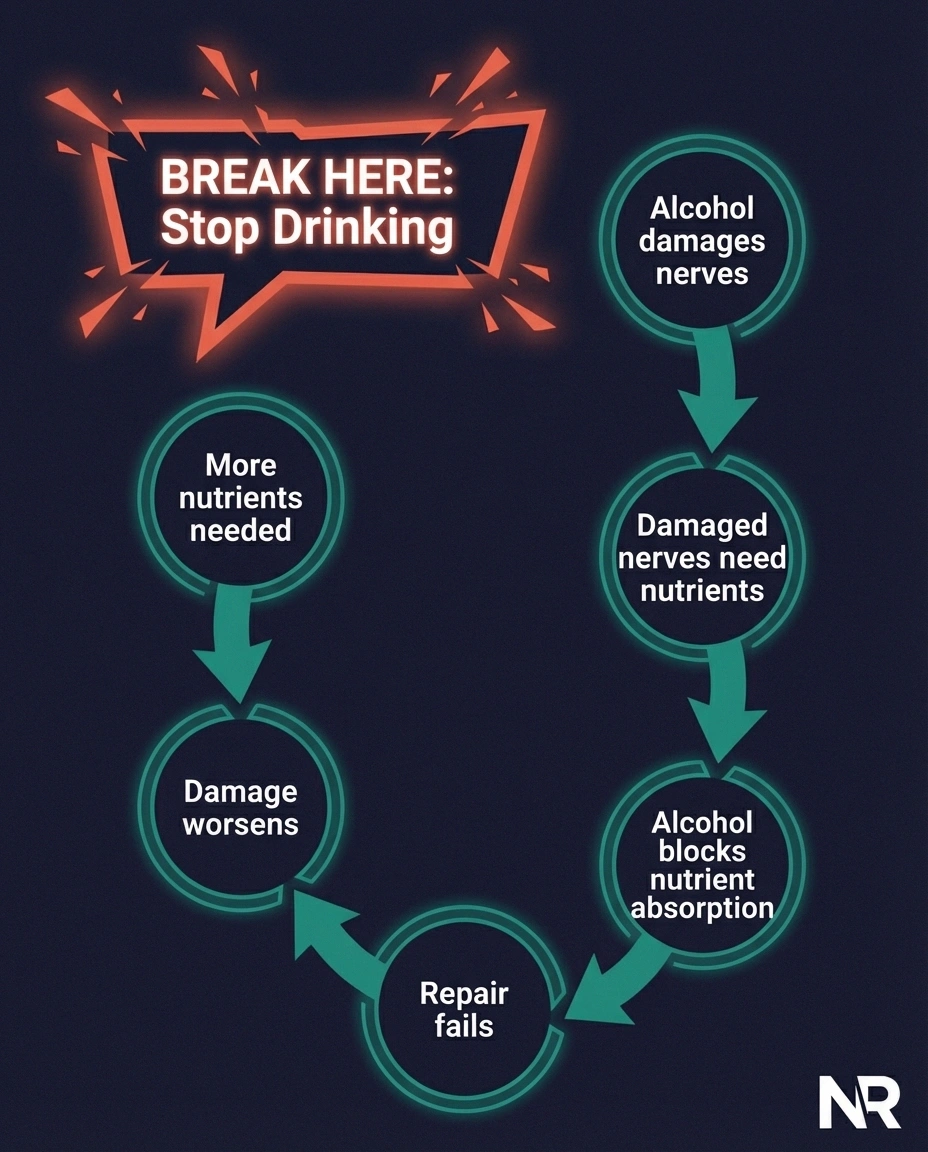
This creates a vicious cycle: alcohol damages nerves → damaged nerves need nutrients to repair → alcohol prevents nutrient absorption → nerve damage worsens → more nutrients needed → alcohol continues blocking absorption. The only way to break this cycle is to stop drinking.
Vitamin deficiency neuropathy compounds the direct toxic effects of alcohol, making the combined damage significantly worse than either factor alone. Research in StatPearls confirms that patients with both direct alcohol toxicity and nutritional deficiency have more severe neuropathy than those with either factor in isolation.
Can You Reverse Alcohol-Related Neuropathy?
This is the question everyone wants answered, and the honest answer depends on timing and severity.

If you stop drinking early — when symptoms are still intermittent and limited to the toes and feet — there's a reasonable chance of significant recovery. The Foundation for Peripheral Neuropathy notes that people who stop drinking “may alleviate their current symptoms and prevent further nerve damage.” Nerves can regenerate at a rate of about 1-2 millimeters per day, but only if the toxic exposure stops and nutritional deficiencies are corrected.
If you stop in the middle stages, some recovery is possible, but it's likely to be incomplete. You may see improvement in pain levels and some return of sensation, but the nerve damage that has already occurred may not fully reverse. Studies suggest recovery can take 6-12 months or longer after complete cessation.
If you've reached advanced stages, the damage is typically permanent. Muscle wasting, significant sensory loss, and autonomic dysfunction are unlikely to reverse even with complete abstinence. Treatment at this point focuses on managing symptoms and preventing further deterioration.
The critical takeaway: nerve damage reversibility depends almost entirely on when you stop. Every day of continued drinking narrows the window for recovery.
What “Moderate Drinking” Does to Damaged Nerves
Some people try to compromise — cutting back instead of quitting entirely. While reducing consumption is certainly better than maintaining heavy drinking, the research offers little comfort for this approach when neuropathy is already present.
There are no clinical studies demonstrating that “moderate” drinking is safe for someone with established alcohol-related neuropathy. The current medical consensus, reflected in guidelines from the Foundation for Peripheral Neuropathy, is that complete abstinence gives the best chance for stabilization and recovery.
The reason is biological: even small amounts of alcohol continue the toxic exposure to already-vulnerable nerve tissue. Your damaged nerves are more susceptible to further injury than healthy nerves. What might be a harmless amount for someone with intact nerves can cause disproportionate damage to nerves that are already struggling.
Additionally, even moderate alcohol consumption continues to impair nutrient absorption, keeping your nerves in the deficiency state that prevents healing. If you're serious about giving your nerves the best chance to recover, understanding your alcohol limits means understanding that the safest limit with existing neuropathy is zero.
How to Tell If Your Neuropathy Is Getting Worse
Monitoring your own progression is important because neuropathy can worsen so gradually that you don't notice until significant damage has accumulated. Watch for these red flags:
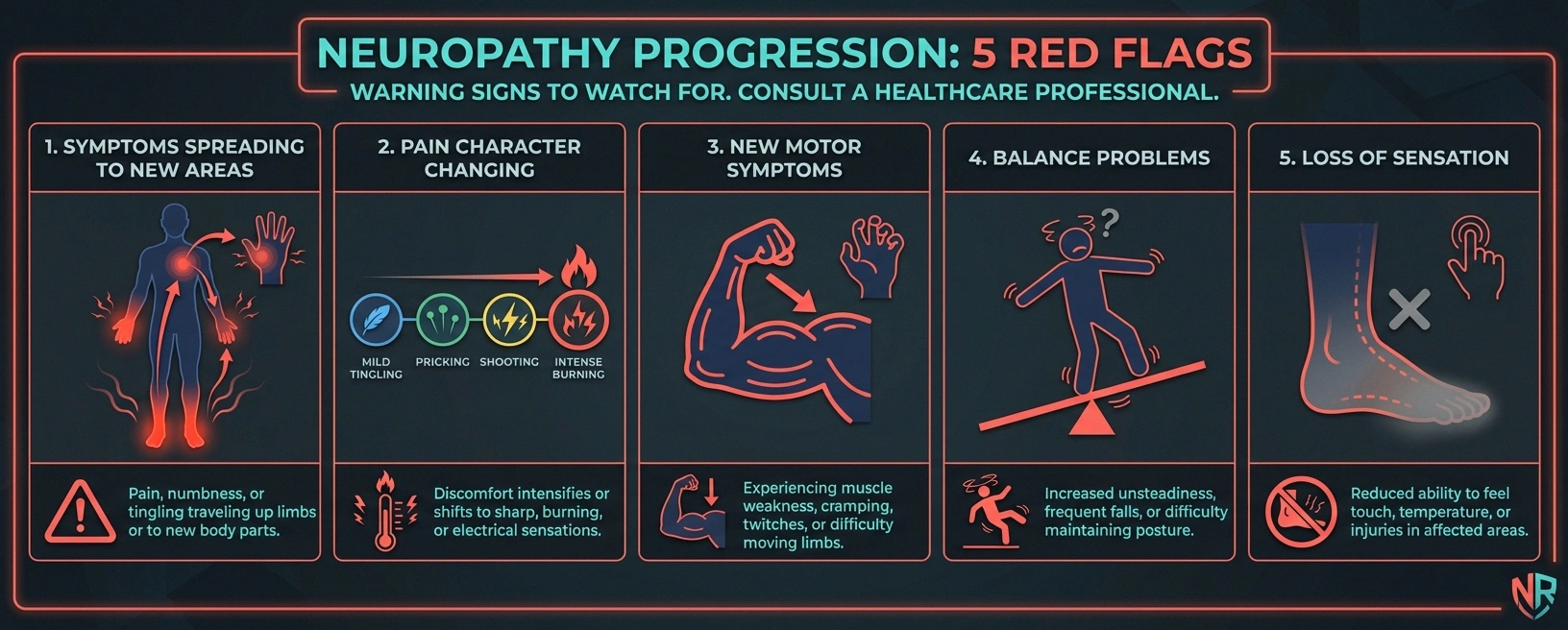

Symptoms spreading to new areas. If numbness or tingling that was only in your toes is now in your whole foot, or if your hands are starting to be affected when previously only your feet were involved, the neuropathy is progressing.
Pain character changing. A shift from intermittent tingling to constant burning, or from surface-level discomfort to deep, stabbing pain, indicates worsening nerve damage.
New motor symptoms. Muscle weakness, foot drop (difficulty lifting the front of your foot), muscle cramps, or visible muscle wasting are signs that motor nerves are now involved — a significant escalation.
Balance problems. Increasing difficulty with balance, more frequent stumbles, or needing to hold onto furniture when walking suggests proprioceptive nerves are being damaged.
Loss of sensation. Paradoxically, when severe pain gives way to numbness, that's not improvement — it's the nerve dying completely. Complete loss of sensation is an emergency sign that requires immediate medical attention.
Keeping a symptom journal is one of the most effective ways to track changes over time. What seems gradual day-to-day becomes starkly visible when you compare notes from three months ago.
Treatment Options If You Stop Drinking Now
If you make the decision to stop, the treatment path forward has several components that work together:
Nutritional rehabilitation is the immediate priority. High-dose thiamine supplementation (often by injection initially, then oral), along with B12, folate, and a comprehensive multivitamin. Your doctor may order blood work to check specific levels. Our guide to B12 injections for neuropathy covers what to expect.
Pain management using medications like gabapentin, pregabalin, or duloxetine can help manage neuropathic pain while your nerves heal. Topical capsaicin and lidocaine patches offer additional relief for localized pain.
Physical therapy helps maintain muscle strength, improve balance, and prevent falls while nerve recovery occurs. Working with a physical therapist who understands neuropathy is especially valuable during recovery.
Regular monitoring with nerve conduction studies and clinical assessments helps track whether your nerves are actually recovering. Ask your neurologist to establish baseline measurements so you can see objective progress (or lack of it) over time.
Getting Help to Stop: You Don't Have to Do This Alone
I want to acknowledge something important: if you have alcohol use disorder, “just stop drinking” is not simple advice. Alcohol dependence is a medical condition that often requires professional treatment, and quitting cold turkey can be medically dangerous.

Talk to your doctor first. Alcohol withdrawal can cause seizures and other serious complications. Your doctor can prescribe medications that make withdrawal safer and more manageable, and connect you with appropriate treatment programs.
SAMHSA's National Helpline (1-800-662-4357) is free, confidential, and available 24/7. They provide treatment referrals and information in English and Spanish.
Many people find that understanding the concrete, progressive nature of nerve damage provides motivation that general health warnings didn't. You're not protecting an abstract concept of “health” — you're protecting your ability to walk, to use your hands, to maintain balance, and to live independently. Those are real, tangible things worth fighting for.
Frequently Asked Questions
How quickly does alcoholic neuropathy progress?
There's no fixed timeline. For some people, noticeable symptoms develop over several years of heavy drinking. For others, the progression is faster, especially when combined with nutritional deficiencies. Binge drinking can cause more rapid progression than the same total amount of alcohol consumed steadily. Once symptoms appear, continued drinking typically leads to worsening over months to years.
Can you drink occasionally if you have neuropathy from other causes?
If your neuropathy is from a non-alcohol cause like diabetes or chemotherapy, moderate alcohol consumption may not directly worsen the neuropathy in the same way. However, alcohol can interfere with neuropathy medications, impair balance further, and reduce your body's ability to absorb nerve-supporting nutrients. Discuss your specific situation with your neurologist.
Does the type of alcohol matter?
No. Beer, wine, and spirits all contain ethanol, and ethanol is what damages nerves. There's no evidence that one type of alcoholic beverage is safer for nerves than another. What matters is the total amount of ethanol consumed over time.
Will taking B vitamins protect my nerves if I keep drinking?
Supplementing B vitamins while continuing to drink is significantly less effective than supplementing after stopping. Alcohol actively impairs absorption of these vitamins, so even high-dose supplements may not reach your nerves in adequate amounts. B vitamins may slow progression somewhat, but they cannot fully protect against the combined effects of direct alcohol toxicity and malabsorption.
Is alcoholic neuropathy the same as diabetic neuropathy?
They're different conditions with different causes but share some similarities. Both cause length-dependent damage starting in the feet, and both involve axonal degeneration. Diabetic neuropathy is caused by blood sugar damage to nerve blood vessels, while alcoholic neuropathy involves direct toxicity plus nutritional deficiency. Having both conditions simultaneously — which is not uncommon — accelerates nerve damage significantly.
How long after quitting drinking will neuropathy improve?
Some people notice pain reduction within weeks of stopping, but meaningful nerve regeneration takes months. Clinical improvement in nerve conduction studies typically appears 6-12 months after complete cessation, with maximum recovery taking 1-2 years. The extent of recovery depends on how severe the damage was before stopping.