When someone in my support group mentions biofeedback, I usually see one of two reactions. Either “That sounds like pseudoscience” or “Oh — you mean those brain wave things?” Both reactions miss what biofeedback actually is and what it can do for neuropathic pain.
Biofeedback isn't a cure for neuropathy. It's not going to regrow your damaged nerve fibers. But it does something genuinely valuable: it teaches you to change your body's response to pain — your muscle tension, your stress hormones, your circulation, even your brain wave patterns — by showing you those responses in real time and training you to control them.
That might sound abstract, so let me put it concretely. When your feet are burning and you're lying in bed at 2 AM thinking “this is never going to get better,” your nervous system is doing several things that make the pain worse: tensing muscles, restricting blood flow to your extremities, flooding your body with stress chemicals. Biofeedback teaches you to reverse those responses. And unlike medication, once you learn the skill, you own it — no refills, no side effects, no prescriptions.
Let me walk you through how it works, what the research says, and whether it's worth trying.
What Is Biofeedback, Exactly?
Biofeedback is a technique that uses electronic sensors to measure your body's involuntary processes — heart rate, muscle tension, skin temperature, brain wave activity — and display them on a screen in real time. A trained therapist then guides you through relaxation and mental exercises while you watch how your body responds.
Biofeedback in 30 Seconds
1. Measure
Sensors detect your body's signals — muscle tension, temperature, heart rate, brain waves
2. Display
Those signals appear on a screen in real time — making the invisible visible
3. Learn
With practice, you learn to control these signals — reducing pain, tension, and stress response
Think of it as a mirror for your nervous system. Once you learn the skill, you own it — no equipment needed.
Think of it like a mirror for your nervous system. You can't normally see your muscle tension levels or your skin temperature. But when those measurements appear on a screen as numbers, graphs, or even a simple animation that changes color, you can start to learn what it feels like when those numbers change — and eventually, how to change them deliberately.
The goal is to eventually be able to reproduce these beneficial states without the equipment — to carry the skill with you into daily life. The monitor is the training tool; the real therapy is what you learn to do on your own.
Types of Biofeedback Used for Neuropathy
Several different biofeedback approaches can help with neuropathic pain, each targeting a different aspect of your body's pain response. Here's what's available and how each one works:
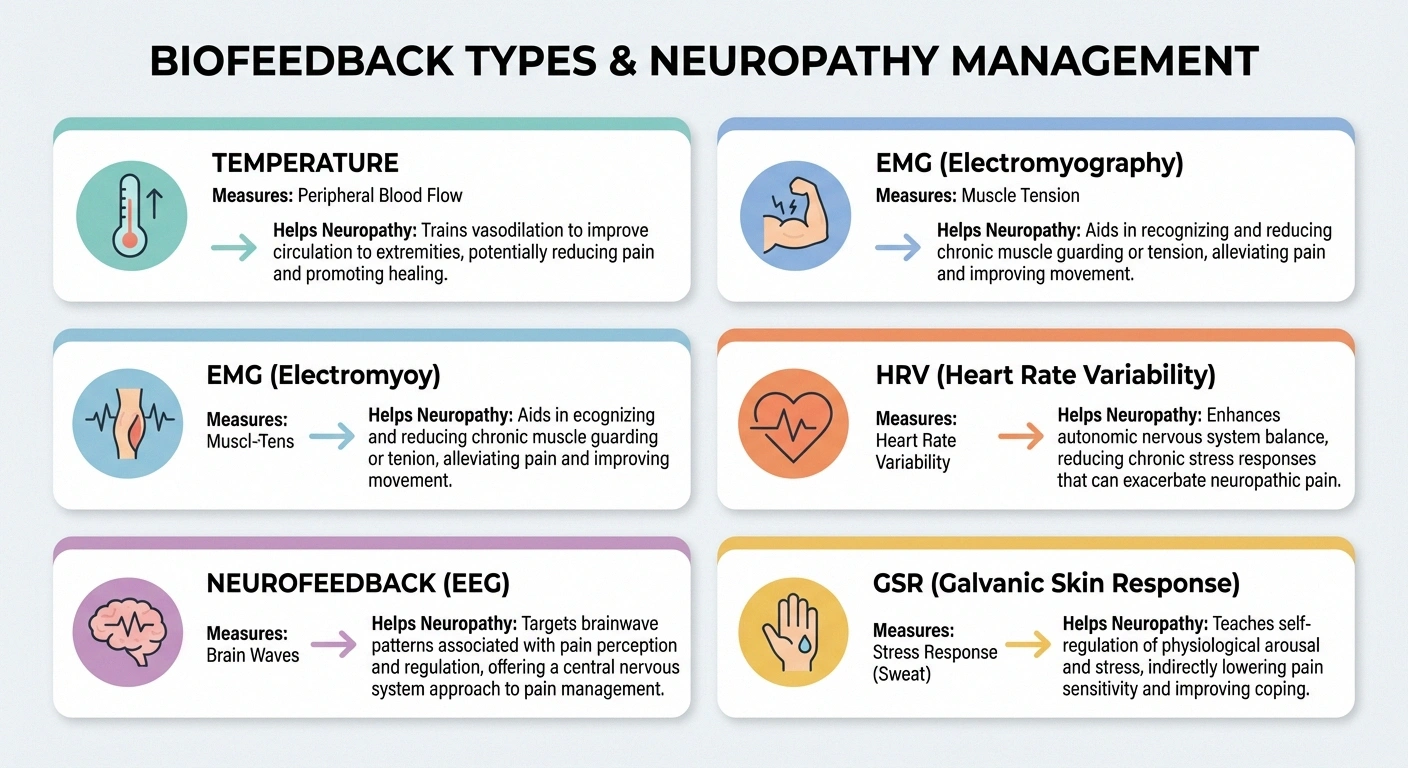
Temperature Biofeedback (Thermal Biofeedback)
Sensors on your fingertips or feet measure skin temperature. When you're stressed or in pain, your body pulls blood away from your extremities (part of the fight-or-flight response), which lowers skin temperature. This is particularly relevant for neuropathy patients because restricted blood flow to your hands and feet means less oxygen and fewer nutrients reaching already-damaged nerves.
Temperature biofeedback teaches you to increase blood flow to your extremities through guided relaxation and visualization techniques. One practitioner, Cindy Perlin of the Alternative Pain Treatment Directory, has reported that clients with peripheral neuropathy experienced significant pain relief after learning to warm their extremities using this technique — effectively increasing circulation to areas where damaged nerves need it most.
This approach is especially relevant if your neuropathy symptoms worsen with cold weather or if you have circulation-related symptoms.
EMG Biofeedback (Electromyographic Biofeedback)
Sensors placed on your skin measure the electrical activity in your muscles — essentially how tense or relaxed they are. Many neuropathy patients unconsciously tense muscles in response to pain, which creates a vicious cycle: pain leads to tension, tension reduces circulation and increases pain, which leads to more tension.
EMG biofeedback makes this invisible tension visible. You learn to recognize subtle muscle guarding patterns you weren't aware of and systematically release them. This can be particularly helpful for people whose neuropathy causes muscle spasms, cramping, or gait changes that lead to compensatory tension elsewhere in the body.
Heart Rate Variability (HRV) Biofeedback
This approach measures the variation in time between heartbeats — a key indicator of your autonomic nervous system's flexibility. Higher HRV generally reflects a healthier, more adaptable stress response. Lower HRV is associated with chronic pain, anxiety, and poor stress resilience.
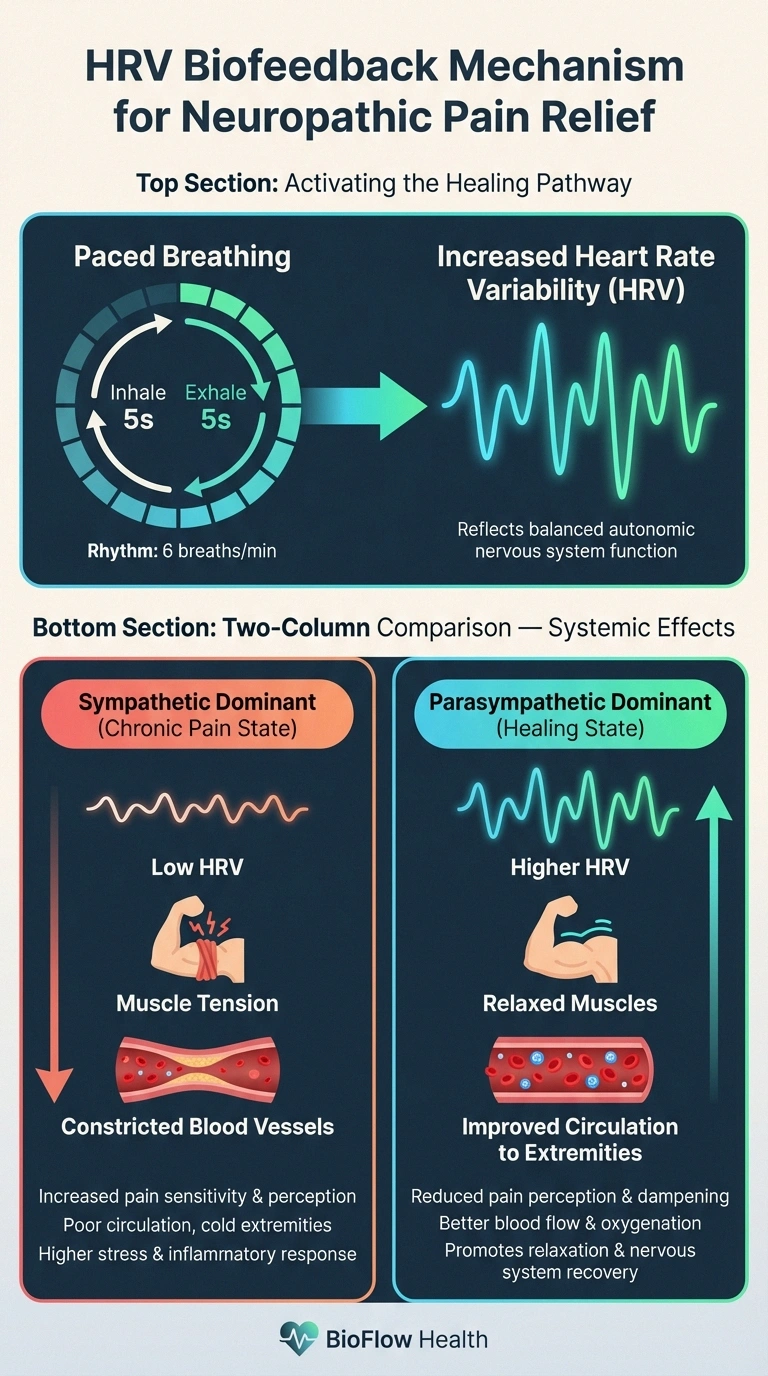
HRV biofeedback trains you to breathe in patterns that optimize your heart rate variability, essentially shifting your autonomic nervous system from a stress-dominant (sympathetic) state to a rest-and-repair (parasympathetic) state. A randomized controlled trial in veterans found that HRV biofeedback significantly reduced both pain and stress levels. For neuropathy patients who also deal with autonomic neuropathy, this approach may offer particular benefit because it directly targets the autonomic system.
Neurofeedback (EEG Biofeedback)
This is the most sophisticated form, using electrodes on the scalp to measure brain wave patterns. Research has identified specific brain wave signatures associated with chronic pain — particularly changes in theta (4 to 8 Hz) and alpha (8 to 12 Hz) wave activity. Neurofeedback trains you to modify these patterns, essentially teaching your brain to turn down its pain processing.
The Foundation for Peripheral Neuropathy highlights neurofeedback as a promising alternative treatment, noting that it uses real-time displays of brain activity to teach self-regulation of brain function. The concept is that if you can see your brain's pain-processing activity on a screen, you can learn to change it — similar to how a thermostat display lets you adjust the temperature in your house.
A systematic review and meta-analysis of clinical trials found that neurofeedback reduced the severity of pain and pain-associated symptoms including sleep disturbances, mood disturbances, fatigue, and anxiety across multiple chronic pain conditions. The researchers concluded that neurofeedback has potential as an integrative non-pharmacological approach to pain management.
Galvanic Skin Response (GSR) Training
Sensors measure the electrical conductance of your skin, which changes with sweat gland activity — a direct indicator of your stress and anxiety levels. This form of biofeedback is particularly useful for the emotional aspects of living with neuropathy: the fear, frustration, and hypervigilance about symptoms that can amplify pain perception.
How Biofeedback Actually Helps Neuropathic Pain
To understand why biofeedback works for neuropathy, you need to understand the relationship between your nervous system's stress response and your pain experience.
“If you have peripheral neuropathy and you're thinking, ‘My feet are burning; it's going to get worse, and I'm not going to be able to walk' — if that's the way you're focusing, you're reducing your circulation.”
— Cindy Perlin, CEO, Alternative Pain Treatment Directory
The fear-pain cycle isn't just in your head — it has measurable physiological effects. Biofeedback teaches you to reverse them.
When you're in chronic pain, your sympathetic nervous system — the fight-or-flight system — stays activated. This isn't a character flaw or a sign that you're not coping well. It's a physiological response: pain signals activate stress pathways, which cause your body to:
- Tense muscles around painful areas (guarding), which can compress nerves and worsen symptoms
- Constrict blood vessels in the extremities, reducing circulation to your hands and feet — exactly where most neuropathy patients need more blood flow, not less
- Release stress hormones (cortisol, adrenaline) that increase inflammation and lower your pain threshold
- Amplify pain signals in the brain through a process called central sensitization — your brain literally becomes more efficient at processing pain
As practitioner Cindy Perlin explains: “If you have peripheral neuropathy and you're thinking, ‘My feet are burning; it's going to get worse, and I'm not going to be able to walk' — if that's the way you're focusing, you're reducing your circulation.” The fear-pain cycle isn't just psychological. It has measurable, physiological consequences that biofeedback can address.
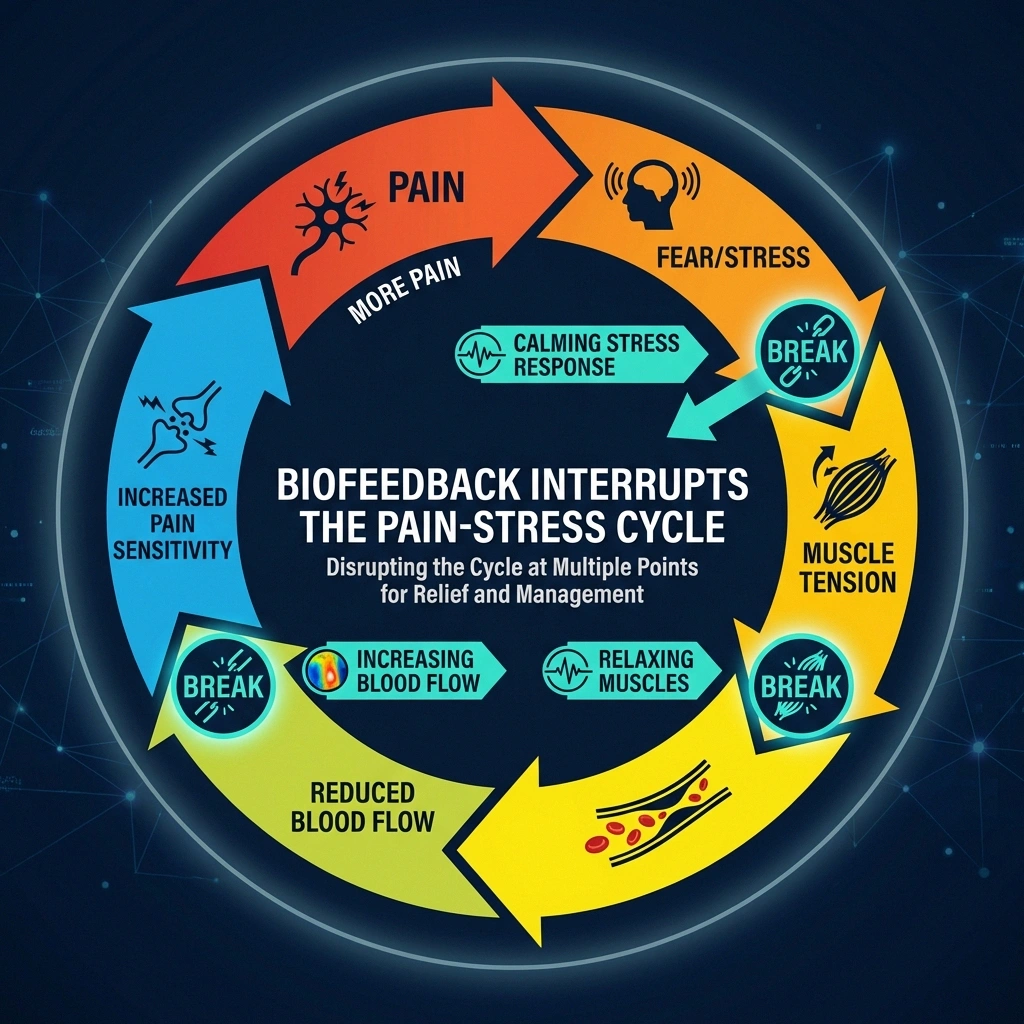
Biofeedback interrupts this cycle at multiple points. It teaches you to:
- Relax specific muscle groups, reducing compression and guarding
- Increase peripheral blood flow, improving oxygen and nutrient delivery to damaged nerves
- Shift your autonomic nervous system from sympathetic (fight-or-flight) to parasympathetic (rest-and-repair) dominance
- Modify brain wave patterns associated with pain amplification
- Replace fear-based thought patterns with intentional, healing-focused responses
None of these changes fix the underlying nerve damage. But they address the layers of amplification that sit on top of that damage and make the pain worse than the physical injury alone would warrant.
What the Research Says
Let me be straightforward about the evidence: biofeedback for neuropathic pain specifically has a smaller research base than for conditions like migraines, chronic back pain, or fibromyalgia, where it's well-established. But the studies that exist are encouraging.
A 2025 systematic review in Heliyon examining biofeedback for chronic pain rehabilitation found significant results across multiple modalities. Among the findings relevant to neuropathy patients:
- A study of 20 neuropathic pain patients found that biofeedback electrostimulation resulted in significant pain relief and positive hormonal responses
- A trial of over 2,000 adults using electrodermal biofeedback showed decreased pain and inflammation in the treatment group, with improved quality of life
- Veterans receiving HRV biofeedback experienced significant reductions in both pain and stress
A 2024 narrative review in Frontiers in Psychology specifically evaluating neurofeedback for chronic pain found a positive correlation between neurofeedback interventions and improved pain management. Several studies reported significant reductions in pain intensity, improved quality of life, and decreased reliance on medication following neurofeedback therapy.
A pilot study in BMC Neurology investigating neurofeedback for central neuropathic pain in spinal cord injury patients found that training patients to modify specific brain wave patterns was associated with changes in pain perception. While this focused on central rather than peripheral neuropathy, the underlying mechanism — modifying brain processing of pain signals — is relevant to both.
The honest assessment: the evidence is promising but not definitive. We need larger, well-designed randomized controlled trials specifically examining biofeedback for peripheral neuropathic pain. The existing literature supports biofeedback as a reasonable complementary approach — not a replacement for other treatments, but a potentially valuable addition.
What a Biofeedback Session Looks Like
If you've never experienced biofeedback, here's what to expect so you walk in prepared rather than anxious:

📅 Your Biofeedback Journey: What to Expect
Sessions 1-3: Learning the Basics
Baseline assessment, sensor familiarization, introduction to relaxation techniques while watching your body's response in real time.
Sessions 4-6: Building Skills
You can reliably shift your physiological state with the monitor's help. Deeper techniques. Home practice begins making a difference.
Sessions 7-10: Measurable Improvement
Most people notice meaningful pain changes. Techniques become more natural. Some sessions may focus without the monitor.
Sessions 10+: Independence
Reproducing relaxation responses without equipment. The skill is yours. Occasional tune-up sessions may help maintain gains.
First visit (assessment): The therapist will discuss your neuropathy symptoms, pain patterns, sleep quality, stress levels, and what you've already tried. They'll attach sensors to measure your baseline — muscle tension, skin temperature, heart rate, or brain waves, depending on the type of biofeedback being used. This baseline tells them where you're starting and which approach is most likely to help.
Typical session (30 to 60 minutes): Sensors are attached — these are non-invasive and painless. They simply measure; they don't send anything into your body. You'll watch a monitor while the therapist guides you through various techniques:
- Deep breathing exercises — you'll watch how your breathing rate and depth affect your heart rate variability and muscle tension in real time
- Progressive muscle relaxation — systematically tensing and releasing muscle groups while watching the EMG readings respond
- Guided visualization — imagining warmth flowing to your hands or feet while watching temperature readings climb (or not — which tells you when you need to adjust your technique)
- Mindfulness exercises — learning to observe pain without reacting to it, while watching how your physiological responses change when you shift from reactive to observational awareness
Progress over time: Most people begin to see meaningful improvements within 8 to 10 sessions, though some conditions take 20 sessions or more. The first few sessions are about learning the basics. By sessions 4 to 6, most people can reliably shift their physiological state with the monitor's help. The final sessions focus on reproducing these changes without the equipment.
Home practice: Between sessions, you'll practice the techniques you've learned — typically 10 to 20 minutes daily. Some therapists provide simple home biofeedback devices (temperature dots, portable HRV monitors, or smartphone apps) to reinforce your training.
Biofeedback Combined With Other Treatments
Biofeedback works best as part of a comprehensive pain management approach, not as a standalone treatment. Here's how it fits with other common neuropathy therapies:
With medications: Biofeedback doesn't interfere with gabapentin, pregabalin, duloxetine, or other neuropathy medications. In fact, one of the documented benefits is that patients who learn biofeedback techniques sometimes find they can reduce their medication doses — under medical supervision — because the biofeedback provides an additional layer of pain management. Some of the medications used for neuropathy cause significant side effects, so any strategy that allows dose reduction is welcome.
With physical therapy: The skills learned in biofeedback — particularly muscle relaxation and stress management — directly complement physical therapy for neuropathy. If you tend to tense up during exercises because you're anticipating pain, biofeedback training can help you relax into your PT routine, which makes it more effective and less uncomfortable.
With other mind-body approaches: Biofeedback pairs naturally with yoga, acupuncture, and meditation. These practices all work on overlapping pathways — calming the stress response, improving body awareness, and changing your relationship with pain. Biofeedback adds the element of objective measurement, which helps you know whether your meditation or relaxation practice is actually producing the physiological changes you're aiming for.
With mental health support: Chronic neuropathy pain takes a real toll on mental health. The anxiety-pain cycle is well-documented. Biofeedback provides concrete, measurable tools for breaking that cycle — which can be more convincing for people who are skeptical of purely talk-based therapy. When you can see your stress response on a screen and watch yourself change it, it makes the mind-body connection tangible rather than theoretical.
Finding a Biofeedback Practitioner
Not all biofeedback providers are equal. Here's what to look for:

Certification: Look for practitioners certified by the Biofeedback Certification International Alliance (BCIA). This is the gold standard credential and ensures the provider has completed accredited training, supervised practice hours, and passed a certification exam.
Experience with pain conditions: Biofeedback is used for many conditions, from ADHD to urinary incontinence. You want someone experienced specifically with chronic pain — ideally with neuropathic pain. Ask how many pain patients they've treated and what outcomes they typically see.
Professional background: Biofeedback practitioners come from various backgrounds — psychology, physical therapy, nursing, counseling. Any of these can be effective, but someone with a background in pain management or neurology may have a better understanding of neuropathic pain specifically.
Where to find providers:
- BCIA's practitioner directory at bcia.org
- The Association for Applied Psychophysiology and Biofeedback (AAPB) at aapb.org
- Ask your neurologist, pain specialist, or primary care doctor for referrals
- Some occupational therapy and physical therapy practices offer biofeedback as part of their services
Cost and Insurance Coverage
This is often the deciding factor for people considering biofeedback. Here's the realistic picture:
💰 Biofeedback Cost Overview
Insurance may cover when prescribed by a physician. Ask about CPT codes 90901 and 90875/90876.
Session costs typically range from $75 to $200 per session, depending on the type of biofeedback, the provider's credentials, and your location. Neurofeedback (EEG-based) tends to be at the higher end because it requires more specialized equipment.
Course of treatment usually involves 8 to 20 sessions, meaning total cost can range from roughly $600 to $4,000. Some people see meaningful improvement in 8 to 10 sessions; others need 15 to 20 for sustained benefits.
Insurance coverage varies widely. Some health insurance plans cover biofeedback — particularly when it's delivered by a licensed healthcare professional (psychologist, physical therapist, or nurse) and prescribed for a documented pain condition. Many plans require pre-authorization. Ask your insurance company specifically about CPT codes 90901 (biofeedback training) and 90875/90876 (biofeedback with psychotherapy). If you have disability benefits, your coverage may differ from standard health insurance.
Home devices are an increasingly affordable alternative. Temperature biofeedback dots cost just a few dollars. HRV biofeedback devices and apps (like HeartMath or Elite HRV) range from $50 to $300. These can't replace professional training, but they can extend and reinforce what you learn in sessions, and some people use them as a lower-cost entry point to see if biofeedback is right for them.
Home Biofeedback: What You Can Do on Your Own
Professional biofeedback training is ideal, but not everyone has access or can afford it. Here are evidence-based techniques you can practice at home that use the same principles:

Temperature Awareness Training
Buy a simple digital thermometer (or biofeedback temperature dots) and tape the sensor to your fingertip. Sit comfortably and practice deep, slow breathing while imagining warmth flowing to your hands. Watch the temperature reading. With practice, many people can raise their finger temperature by several degrees — indicating real increases in blood flow. Once you can do this reliably, try it with your feet if foot symptoms are your main concern.
Breathing for Pain Relief
Slow, paced breathing at about 6 breaths per minute (inhale for 5 seconds, exhale for 5 seconds) is one of the most reliable ways to shift your autonomic nervous system toward parasympathetic dominance. This is the core technique behind HRV biofeedback. Practice for 10 to 20 minutes daily, especially during evening hours when neuropathy symptoms typically worsen.
Progressive Muscle Relaxation
Systematically tense each muscle group for 5 seconds, then release for 30 seconds, working from your feet upward. Pay attention to the difference between tension and relaxation in each area. This builds the body awareness that's central to EMG biofeedback — without the equipment. It's especially useful before bed if muscle tension contributes to your nighttime symptoms.
Smartphone Apps
Several apps provide basic biofeedback functionality using your phone's sensors. HRV-focused apps can measure heart rate variability through your phone's camera. While these aren't as precise as clinical equipment, they provide enough feedback to guide practice. Look for apps that specifically guide paced breathing and track your HRV trends over time.
Who Benefits Most From Biofeedback?
Based on the research and clinical experience, biofeedback tends to be most helpful for neuropathy patients who:

- Have significant stress or anxiety related to their neuropathy — the more your pain is amplified by stress, the more biofeedback has to work with
- Notice that symptoms worsen with stress — if you've observed that your flare-ups correlate with stressful events, biofeedback directly targets this connection
- Have not responded fully to medications — biofeedback adds a non-pharmacological approach that works through different mechanisms than drugs
- Want to reduce medication dependence — particularly if side effects from neuropathy medications are a concern
- Are motivated to practice regularly — biofeedback is a skill, not a passive treatment. It requires consistent practice, like learning a musical instrument. People who are willing to practice daily tend to see the best results.
- Have cold extremities alongside neuropathy — temperature biofeedback is particularly relevant when reduced circulation is contributing to symptoms
Biofeedback may be less helpful for people whose neuropathy is purely mechanical (severe nerve compression) without a significant stress component, or for those who aren't able to commit to regular practice sessions.
Frequently Asked Questions
Is biofeedback safe for neuropathy patients?
Yes. Biofeedback is non-invasive and has virtually no side effects. The sensors measure your body's activity but do not send any electrical signals into your body. It is safe to use alongside medications, physical therapy, and other treatments. The only consideration is that if you are prone to seizures, certain types of neurofeedback should be supervised by a practitioner experienced with seizure disorders.
How many sessions will I need before I notice a difference?
Most people begin to see improvements within eight to ten sessions, though some notice changes earlier. Simple temperature and breathing biofeedback may produce noticeable relaxation in just a few sessions. Neurofeedback, which involves training brain wave patterns, typically requires more sessions, sometimes fifteen to twenty, before changes become sustained. Your practitioner should be able to show you measurable progress in your biofeedback readings even before you notice subjective pain changes.
Does insurance cover biofeedback for neuropathy?
Coverage varies significantly by insurance plan and state. Biofeedback is more likely to be covered when it is delivered by a licensed healthcare provider such as a psychologist or physical therapist and when it is prescribed for a specific diagnosed condition like neuropathic pain. Call your insurance company before starting treatment and ask specifically about CPT codes 90901 and 90875. Some plans require pre-authorization or a referral from your primary care physician.

Can I do biofeedback at home without professional training?
Home practice can provide some benefit, particularly for breathing-based and temperature biofeedback techniques. However, professional training gives you the advantage of personalized assessment, expert guidance on which techniques are most appropriate for your specific situation, and access to more precise equipment. A good approach is to start with a few professional sessions to learn the fundamentals, then continue practicing at home with simple tools to maintain and build on your skills.
Is biofeedback the same as meditation or mindfulness?
They share some overlap but are distinct. Meditation and mindfulness involve focusing attention and cultivating non-reactive awareness, but without real-time physiological feedback. Biofeedback adds the measurement component, showing you exactly what is happening in your body as you practice. This makes biofeedback more precise and often faster to learn, because you are not guessing whether your relaxation practice is actually producing the intended physical changes. Many biofeedback practitioners incorporate mindfulness techniques into their sessions.
Can biofeedback help with neuropathy symptoms beyond pain?
Yes. The research suggests biofeedback can improve sleep quality, reduce anxiety and depression associated with chronic pain, decrease muscle tension and spasms, and improve overall quality of life. For neuropathy patients who struggle with insomnia due to nighttime pain, the relaxation skills learned through biofeedback can be particularly valuable as part of a better sleep routine.
The Bottom Line
Biofeedback isn't a miracle cure — and I'm always suspicious of anything that claims to be one. But it's a legitimate, evidence-supported approach that gives neuropathy patients something genuinely valuable: a sense of agency over their pain.
When you live with chronic nerve pain, it's easy to feel like your body is out of your control. The burning, the tingling, the flare-ups that seem to come from nowhere — these experiences can make you feel helpless. Biofeedback offers a counter-narrative: with training and practice, you can measurably change how your body responds to pain. Not eliminate the pain entirely, but turn down the amplifiers that make it worse.
As Cindy Perlin puts it, biofeedback helps people move from a fragile, fearful “Oh-my-God” place to a solution-centered “What can I do?” And in my experience, that shift in orientation — from helpless to active, from victim to problem-solver — makes a real difference in how people experience their neuropathy, even beyond what the physiological changes alone would predict.
If you're interested, start with a conversation with your doctor. Ask for a referral to a BCIA-certified practitioner. Or try the home techniques in this article — paced breathing, progressive muscle relaxation, temperature awareness — and see if they affect your symptoms. The worst that can happen is you learn some relaxation techniques. The best that can happen is you discover a powerful new tool for managing your pain.
Either way, it costs you nothing but a little time and an open mind.