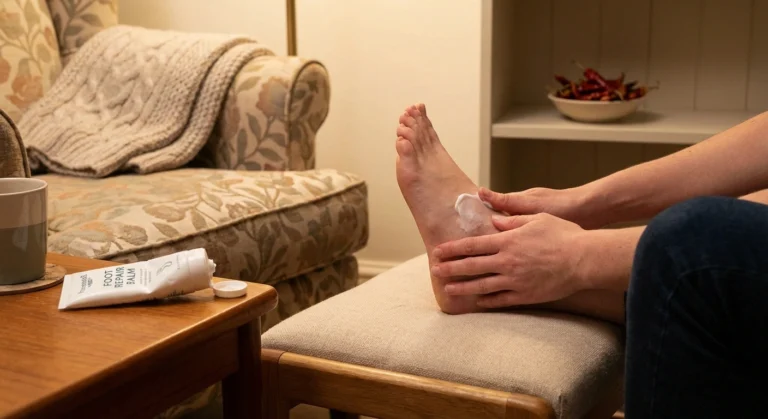
The first time someone suggested I try meditation for my neuropathy, I almost laughed at her. We were sitting in a waiting room, both there for the same neurologist, and she was knitting while I was staring at a magazine I wasn't really reading. I had pins-and-needles running up both calves, my feet felt like they'd been packed in cold soup, and a woman with kind eyes was telling me I should sit still and “notice my breath.”
I went home and ignored the advice for almost a year.
What changed my mind wasn't an article or a doctor. It was a bad night. One of those nights where the burning in my feet won't let me sleep, and I'd already cycled through every distraction I owned. I remembered that woman in the waiting room. I pulled up a free guided body scan on my phone at 2:43 a.m., put in my earbuds, and pressed play because I had nothing left to lose.
I didn't fall asleep. The pain didn't disappear. But something shifted that I didn't have a name for yet. I learned later that the something had a name. It's called Mindfulness-Based Stress Reduction, or MBSR, and there's an entire 8-week program built around it. This article is the one I wish someone had handed me that night.
What MBSR Actually Is (and What It Isn't)
MBSR was created in 1979 by a molecular biologist named Jon Kabat-Zinn at the University of Massachusetts Medical School. He'd been a long-time meditator and noticed something: the patients his colleagues couldn't help — the ones with chronic pain, autoimmune flares, anxiety that wouldn't quit — were the same patients who, in his early experiments, responded to a structured 8-week course in mindfulness and gentle movement.
Key Takeaway
MBSR is a structured 8-week course in mindfulness, gentle yoga, and body awareness. It is not religious, not a cure, and not a replacement for medical care. It is a training program for changing your relationship with sensations in your body — including pain — so that the suffering layered on top of pain starts to come unglued from the pain itself.
That course became MBSR, and it's now taught at hospitals, universities, and community centers in dozens of countries. The program is the same wherever you take it: eight weekly classes, a full-day silent retreat, and a daily home practice you do on your own. About 24 hours of formal instruction, plus whatever you put in at home.
Here's what MBSR is not:
- It is not a religious or spiritual practice. There's no faith requirement. Skeptics are welcome and, frankly, do well in it.
- It is not a cure. No one in MBSR will tell you your nerves are going to regrow because you breathed into them.
- It is not a replacement for medical care. It works alongside whatever your doctor has you doing.
- It is not relaxation. Sometimes you'll feel calmer; sometimes you'll feel more aware of how uncomfortable you actually are. That awareness, oddly, is the point.
What it is, as best as I can describe it: a structured way to change your relationship with sensations in your body — including the bad ones — so that the suffering layered on top of pain starts to come unglued from the pain itself. There's a difference between the actual signal coming from your nerves and the avalanche of fear, anger, and exhaustion that piles on top of it. MBSR works on the avalanche.
Why MBSR Matters for Neuropathy Specifically
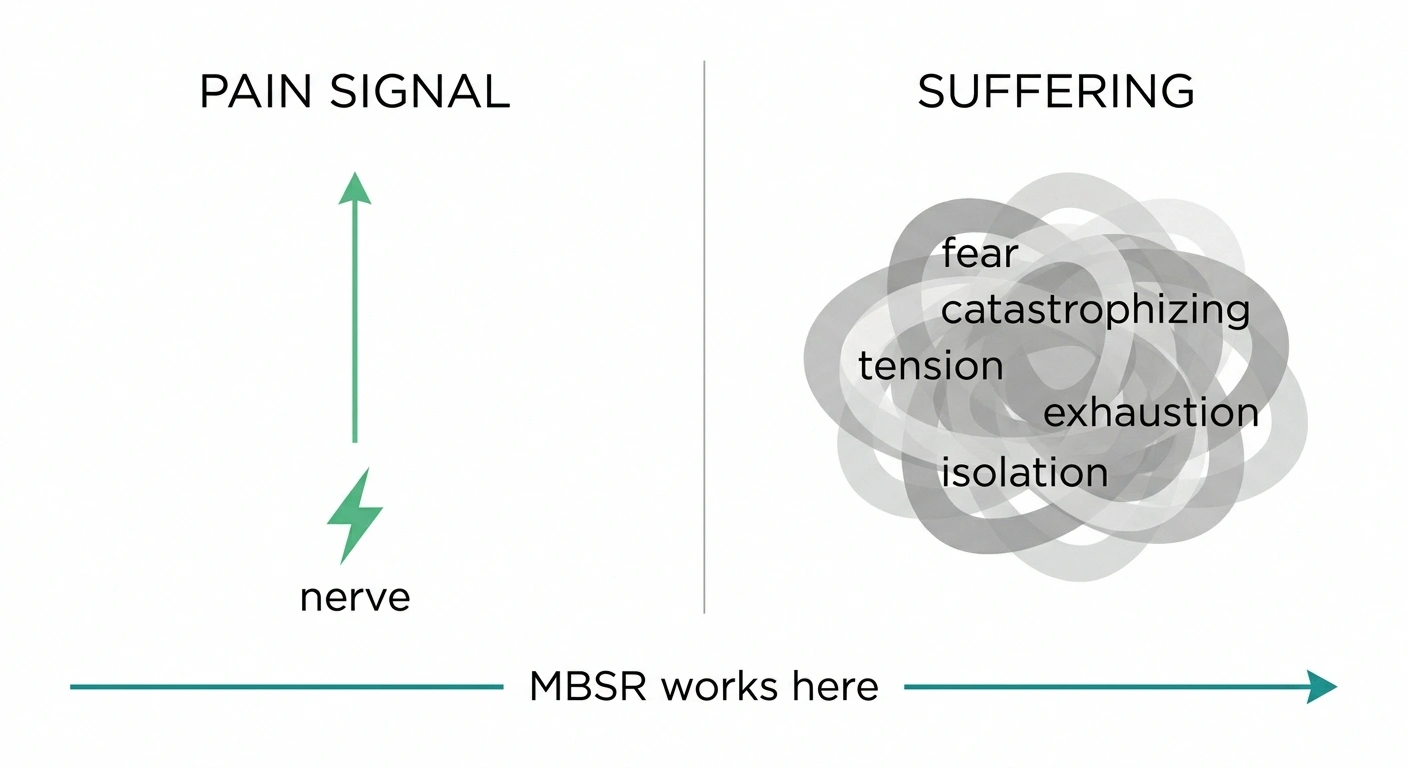
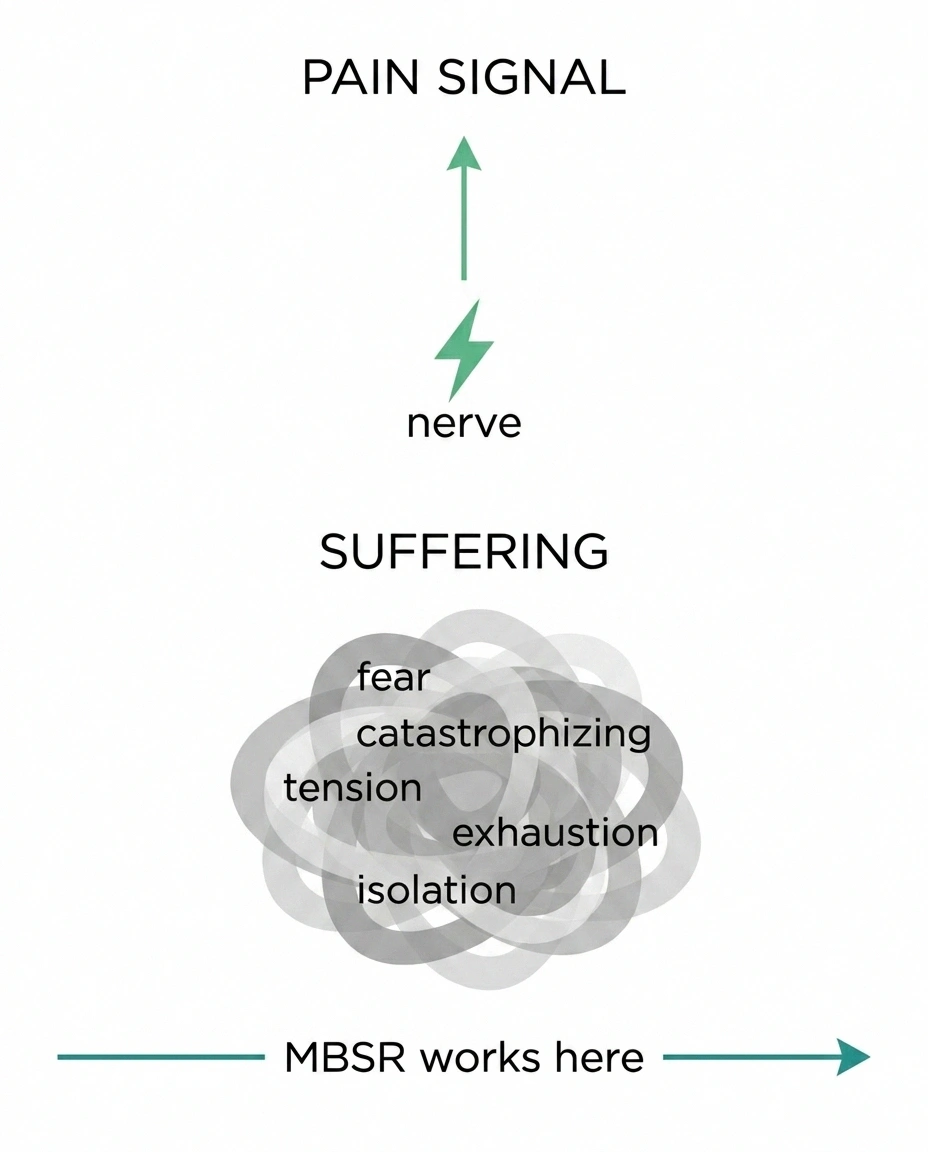
For most of us with peripheral neuropathy, pain isn't the only problem. It's the emotional weather around the pain. The 3 a.m. catastrophizing. The dread of putting on shoes. The way a small flare can hijack a whole afternoon. The withdrawal from people because you don't want to explain again. I've written separately about how heavy the emotional load can get — see Neuropathy and Mental Health and how anger and frustration creep in — and there's a reason MBSR shows up in so many of those conversations.
Outcomes from community-based MBSR studies in painful diabetic peripheral neuropathy and from a 2024 scoping review of mindfulness interventions for neuropathic pain.
Research on MBSR for chronic pain has been building since the 1980s. A few things stand out:
- A 2017 systematic review in the Annals of Behavioral Medicine found that mindfulness meditation produced small but meaningful improvements in pain intensity, depression, and quality of life across chronic pain populations.
- In studies of painful diabetic peripheral neuropathy specifically — patients already optimized on medication — community MBSR participants reported roughly a 30% reduction in pain severity and a 46% drop in pain catastrophizing scores at 12 weeks.
- A scoping review of 12 mindfulness-intervention studies for neuropathic pain found significant improvements in pain intensity in 7 of them and improvements in disability in 10. The quality of evidence is moderate, not slam-dunk, but the direction of the evidence is consistent.
The most interesting piece, to me, is what MBSR doesn't claim to change. It doesn't claim to fix your nerves. It works on a process called central sensitization — the way the central nervous system can amplify pain signals over time, especially in chronic conditions. (We have a full breakdown in our article on central sensitization in neuropathy if you want the deep dive.) MBSR appears to gently turn down the volume on that amplifier without touching the source signal. For people whose neuropathy isn't going away, that distinction matters.
The 8-Week Structure: What You Actually Do

Every authorized MBSR program follows the same skeleton, set out in the curriculum guide originally developed at UMass. The exact wording shifts teacher to teacher, but the bones are consistent. Here's what each week tends to look like.
The 8-Week MBSR Arc at a Glance
Week 1: There Is More Right With You Than Wrong With You
The first class is mostly orientation and the famous raisin exercise — yes, you'll spend several minutes eating a single raisin with full attention. It sounds silly. It's also the cleanest demonstration I've ever seen of how rarely we're actually in our bodies. You'll be introduced to the body scan meditation and asked to do it daily this week.
Week 2: Perception and Creative Responding
The theme is how perception shapes experience. You begin sitting meditation in addition to the body scan. The home practice is roughly 45 minutes a day, six days a week — and yes, that's a lot. We'll talk about the home practice in a minute.
Week 3: The Pleasure and Power of Being Present
This week introduces mindful movement (gentle yoga done lying down or seated) and a short pleasant-events log. You write down one pleasant moment a day — what you noticed in your body, your thoughts, your emotions. For people in chronic pain, this exercise can feel revelatory. We've often stopped looking for the pleasant.
Week 4: The Shadow of Stress
Here you start the unpleasant-events log alongside the pleasant one. The teacher introduces the concept of stress reactivity — what happens in your body and mind when something hard shows up. For neuropathy, this is the week things tend to click. You start to notice the cascade: pain spike → catastrophic thought → tense muscles → more pain. Awareness of the cascade is what eventually lets you interrupt it.
Week 5: Finding the Space for Responding Rather than Reacting
Sitting meditation gets longer. You learn techniques for working with difficult sensations and emotions rather than fighting them. This is also where, in many programs, you'll have your first real experience of allowing pain to be present in awareness without the usual mental tug-of-war.
Week 6: Mindful Communication
The theme shifts a little outward — how mindfulness shows up in conversations and conflict. People often resist this week (I did) because it doesn't feel as relevant to a body problem. It is relevant. So much of how we handle a chronic condition happens in conversation: with doctors, with partners, with ourselves at 3 a.m. (See our piece on neuropathy and isolation for more on the relational side of this.)
Between Week 6 and 7: The All-Day Retreat
Most programs include a 7-hour silent retreat on a Saturday. You sit, walk, eat, and move — all in silence, all with attention. It is much harder than it sounds and much more useful than it sounds. This is the day people stop being polite about their meditation practice and start actually meeting their experience.
Week 7: Lifestyle and Self-Compassion
You're given more freedom in your home practice — you choose the practices that have helped most. The teacher introduces self-compassion practices, which can be the most quietly transformative element of MBSR for people with chronic conditions. Many of us are kinder to strangers than we are to our own bodies.
Week 8: The Rest of Your Life
The final class is review and integration. What worked? What will you keep? How will you build this into your life when the structure of the class is gone? You don't graduate from MBSR — you start it. The 8 weeks are the on-ramp.
What the Daily Home Practice Really Looks Like

I want to be honest about the home practice because almost no article tells you the truth: about 45 minutes a day, six days a week. That's a lot. It is the single biggest reason people drop out.
Be Honest About the Time Commitment
The single biggest reason people drop out of MBSR is the home practice. ~45 minutes a day, six days a week, for eight weeks, is a real commitment. If you cannot honestly carve that out, build up first with shorter daily practices for 2-3 weeks before signing up for the full program — or start with a self-paced option like Palouse Mindfulness, which lets you set your own pace.
MBSR can also surface difficult emotions. If you are in active mental-health crisis or untreated severe depression, talk with a clinician about whether to start now or stabilize first.
That number breaks down roughly as one formal practice (body scan, sitting meditation, or yoga) — usually 30-45 minutes — plus shorter informal practices through the day (mindful eating, mindful walking, the three-minute breathing space). Some weeks you'll be assigned two formal practices.
Here's what I'd tell a friend with neuropathy starting tomorrow:
- The body scan is non-negotiable in the early weeks. It's also the practice that probably has the most direct relevance to nerve pain. You're learning to drop your attention into different parts of your body — including the parts that feel terrible — without flinching away or fixing.
- Sitting meditation is the hardest if your feet burn. You're allowed to sit in a chair, allowed to recline, allowed to shift. The instruction isn't to be still — it's to be aware of whatever is happening, including the urge to move.
- The yoga is genuinely gentle. Most of it is done lying down or in a chair. If you've struggled with balance — see our balance and falls article for context — there are versions that don't require standing. Or pair MBSR with a more neuropathy-friendly yoga practice that respects what your feet can and can't tell you.
- Skipping a day isn't failure. The instruction is “begin again.” That phrase is the whole program in two words.
Where to Find a Program


You have more options than you probably realize, and they range from completely free to a few hundred dollars.
Free MBSR vs Paid MBSR — Decision Guide
| What You Get | Free (Palouse) | Paid Live Program |
|---|---|---|
| Cost | $0 | $300-$650 typical |
| Curriculum | Full 8-week MBSR | Full 8-week MBSR |
| Live group | No | Yes (in-person or video) |
| Teacher feedback | No | Yes |
| All-day retreat | Self-guided | Held with cohort |
| Schedule | Self-paced | Fixed weekly cohort |
| HSA-eligible | N/A (free) | Possibly, with LMN |
| Best for | Self-directed learners, tight budgets | Group accountability, hands-on guidance |
Paid In-Person and Live-Online Programs
The most authoritative option is a course taught by a teacher certified through the original UMass program (now run by the Brown University School of Public Health, which acquired the certifying body in 2017). Many large hospitals run them — Mayo Clinic, Cleveland Clinic, Mass General, Stanford, UC San Diego, Penn Medicine, and others. UMass Memorial itself offers live-online MBSR cohorts from the program's birthplace.
Typical cost in the US: $300-650 for the full 8-week program. Some hospital systems offer sliding-scale or scholarship spots. Always ask. Most teachers I've met would rather have you in the room at a reduced rate than not at all.
Free Online MBSR — Palouse Mindfulness
This is the one I always send people to first, especially if money or scheduling is the barrier. Palouse Mindfulness is a free, full 8-week MBSR course built by Dave Potter, a certified MBSR instructor and retired psychotherapist. It's a 501(c)(3) non-profit. No fees, no email signup, no cookies, no upsell. The same body scan, sitting meditation, and yoga practices used in paid programs are there, plus video teachings from leading mindfulness teachers.
What you give up going the Palouse route: the live group, the teacher feedback, the accountability of a Tuesday-night class. Some people thrive in self-paced formats. Others need the structure. Know yourself.
Free Apps and Supplements
- UCLA Mindful — free guided meditations from the UCLA Mindful Awareness Research Center. Strong body scan and breath practices.
- Insight Timer — free tier includes hours of MBSR-style guided meditations, including Dave Potter's recordings.
- Jon Kabat-Zinn's recordings — the original guided body scans and sitting meditations are widely available; some are free on YouTube and Insight Timer.
Cost, Insurance, and HSA: What You Need to Know

This is where I have to put on my “patient who learned the hard way” hat. MBSR is not routinely covered by US health insurance. The Veterans Health Administration is the standout exception — it includes mindfulness-based interventions in its standard benefits package for veterans receiving VA care.
What the Research Actually Says
Strong evidence at short-term follow-up. A 2017 systematic review in Annals of Behavioral Medicine found mindfulness meditation produces small but meaningful improvements in pain intensity, depression, and quality of life across chronic-pain populations. Effects are strongest at 8 weeks and 6 months, with moderate persistence at 1-2 years.
Specific neuropathy evidence is moderate, not definitive. A scoping review of 12 mindfulness studies in neuropathic pain showed pain-intensity improvement in 7 and disability improvement in 10. Quality of evidence: moderate. Findings consistent in direction; effect sizes vary by individual.
Mechanism: appraisal, not signal. MBSR doesn't change the nerve damage. It appears to reduce pain catastrophizing and the central-sensitization amplification process — turning down the volume on the pain alarm without touching the source.
For HSA or FSA reimbursement, the path is narrower than people assume. A generic stress-reduction class is not automatically eligible. What can make it eligible is a Letter of Medical Necessity from your physician — a short letter that names a diagnosed condition (peripheral neuropathy, chronic pain, generalized anxiety disorder, depression) and recommends MBSR specifically as part of treatment. With that letter, many HSA/FSA administrators will reimburse the program fee. Without it, you're rolling the dice.
Practical steps if you want to pursue HSA reimbursement:
- Ask your prescribing doctor or neurologist if they'd be willing to write an LMN.
- Confirm in writing with your HSA/FSA administrator that an LMN-supported MBSR program qualifies under their rules. Get the email response — don't take a phone agent's word for it.
- Pay for the program with your HSA card or pay out of pocket and submit for reimbursement, depending on what your administrator prefers.
- Keep a copy of the LMN, the receipt, and the program description for at least three years. The IRS rules are clear that you, not the administrator, are responsible for substantiating eligibility.
If you can't get the LMN or the reimbursement is too much hassle, Palouse Mindfulness exists. The free version of MBSR is, by every honest report I've read and lived, a real program. The cost-free path is not the lesser path.
What MBSR Has Done — and Hasn't Done — for My Neuropathy

I want to be careful here, because I've read enough articles by patients evangelizing for some intervention to know how easy it is to overpromise.
What MBSR has done for me, after about three years of on-and-off practice:
- The 3 a.m. spiral is shorter. Not gone. Shorter. I can usually catch it earlier and not amplify it.
- I am better at noticing when my legs hurt and when my mind is hurting about my legs hurting. Those used to be the same thing. Now they're two things, and I can sometimes work with them separately. Our piece on neuropathy and identity goes deeper into this — the practice of letting the diagnosis be one part of you rather than the whole of you.
- I sleep better on nights I've practiced earlier in the day. Not perfect — see our notes on why neuropathy gets worse at night for the broader picture — but better.
- I am less afraid of bad days. I still hate them. I'm just less afraid of them.
What MBSR has not done:
- It has not changed the underlying nerve damage. My EMG looks how it looks.
- It has not stopped flares. I still have weeks where I can barely walk to the mailbox.
- It has not replaced any of the medications or supplements my doctor and I have settled on.
That's the honest version. If a program promises more, run.
Should You Try It?
I am not your doctor. I'm a person with neuropathy who tried MBSR and stayed with it. The questions I'd want a friend to ask before signing up are:
- Can you commit to 45 minutes a day for 8 weeks? Be honest. If the answer is a real no, start with 10-minute guided sittings and build from there before doing the full program.
- Are you in a stable enough place mentally? MBSR can surface difficult emotions. If you're in active crisis or untreated severe depression, talk to a clinician about whether to start now or stabilize first.
- Do you respond better to live group accountability or to self-paced learning? That answer will steer you toward a hospital program or toward Palouse.
- Have you talked to your doctor? You don't need permission to meditate. But it's worth letting them know — both because they may have an opinion on timing, and because they may be willing to write the letter that makes it HSA-eligible.
If you do try it, give it the full 8 weeks before you decide whether it's working. The first three weeks are awkward. The middle is when the real shifts begin. Walking out of week 4 because nothing has changed yet is like leaving the theater 20 minutes into a movie. You don't yet know what you're watching.
Frequently Asked Questions
Is MBSR proven to help peripheral neuropathy?
The evidence is moderate and growing. Studies of MBSR in painful diabetic peripheral neuropathy have shown roughly 30% reductions in pain severity and around 46% reductions in pain catastrophizing at 12 weeks. The quality of evidence is described as moderate, not definitive. MBSR is best understood as a complement to standard medical treatment, not a replacement.
How much does MBSR cost?
A standard paid 8-week MBSR program in the United States typically costs $300 to $650, depending on the hospital, university, or center offering it. Free alternatives exist — Palouse Mindfulness offers the full curriculum at no cost. Many paid programs offer scholarships or sliding-scale spots if cost is a barrier.
Will my insurance cover MBSR?
Most US health insurance plans do not cover MBSR routinely. The Veterans Health Administration is the major exception, including mindfulness in its standard benefits for veterans. HSA or FSA accounts may reimburse MBSR fees if you have a Letter of Medical Necessity from a physician tied to a diagnosed condition. Confirm eligibility with your HSA administrator before paying.
How much time does MBSR really take each day?
The standard expectation is around 45 minutes of formal practice per day, six days a week, for the full 8 weeks. That's the single most common reason people drop out. You can build up to it gradually with shorter practices before starting the full program, which often makes the time commitment feel more sustainable.
Is online MBSR as effective as in-person?
Live-online MBSR cohorts taught by certified instructors appear to produce outcomes broadly similar to in-person programs in research to date. Self-paced free courses like Palouse Mindfulness use the same curriculum and meditation recordings but lack the live group and teacher feedback. Effectiveness in self-paced formats depends heavily on consistency. People who do well with structure may benefit from a live program; self-directed learners can thrive with the free option.
What if I cannot sit still because of nerve pain?
You are not required to sit still. MBSR teachers explicitly tell you that you can recline, sit in a chair, shift positions, or stand. The practice is awareness, not stillness. The body scan is done lying down. Yoga is gentle and frequently done from a chair or on the floor. If your physical situation needs serious modifications, tell your teacher in week one — that conversation is normal and welcomed.
Can MBSR replace my neuropathy medications?
No. MBSR is intended to work alongside whatever your physician has prescribed, not to replace it. Never stop or change a prescribed medication based on starting a meditation program. If you find that consistent practice changes your symptoms substantially, talk to your prescribing doctor about whether and how to adjust your treatment plan.
What is the difference between MBSR and regular meditation apps?
Standard meditation apps offer guided practices but no structured curriculum, no group accountability, no full-day retreat, and no integration arc across weeks. MBSR is a complete 8-week course developed in a clinical setting and taught by certified instructors. The free Palouse Mindfulness course closely mirrors the full MBSR curriculum, while most general-purpose meditation apps do not.