Diabetic Neuropathy Treatment: Complete Guide
If you have diabetic neuropathy, you've probably already heard the frustrating truth: there's no cure. But “no cure” doesn't mean “no options.” The reality is that diabetic neuropathy treatment has advanced significantly, and most people can achieve meaningful symptom relief, slow or stop progression, and maintain their quality of life — if they know what's available and pursue a comprehensive approach.
This guide covers every evidence-based treatment option for diabetic neuropathy, from the foundation (blood sugar management) through prescription medications, natural therapies, and advanced interventions. Whether you were just diagnosed or you've been managing this for years and looking for new options, this is your complete resource. For a broader look at how diabetes affects nerves, see our complete guide to diabetic neuropathy.
The Foundation: Blood Sugar Control
Every treatment discussion for diabetic neuropathy must start here because blood sugar control is the single most important factor in determining whether your neuropathy stabilizes, improves, or gets worse.
Perpetually high blood sugar damages the small blood vessels that supply oxygen and nutrients to your nerves. According to research cited by Cleveland Clinic, maintaining an A1C above 7% for three or more years significantly increases neuropathy risk, and the higher and longer the elevation, the greater the damage.
For people with Type 1 diabetes, tight glycemic control has been conclusively proven to reduce neuropathy risk. The landmark Diabetes Control and Complications Trial (DCCT) demonstrated a 60-70% reduction in neuropathy development with intensive insulin therapy.
For Type 2 diabetes, the picture is more nuanced. Blood sugar control clearly helps prevent neuropathy, but once neuropathy is established, the benefit of aggressive lowering is less dramatic. Still, bringing A1C closer to target slows progression and may allow some nerve recovery. The emerging emphasis on “time in range” — keeping blood sugar within target levels for a greater percentage of the day — appears to matter as much as the A1C number itself.
For a dietary approach to blood sugar management, our guide to sugar and neuropathy explains how blood sugar spikes damage nerves and practical strategies to flatten the curve.
First-Line Prescription Medications for Pain
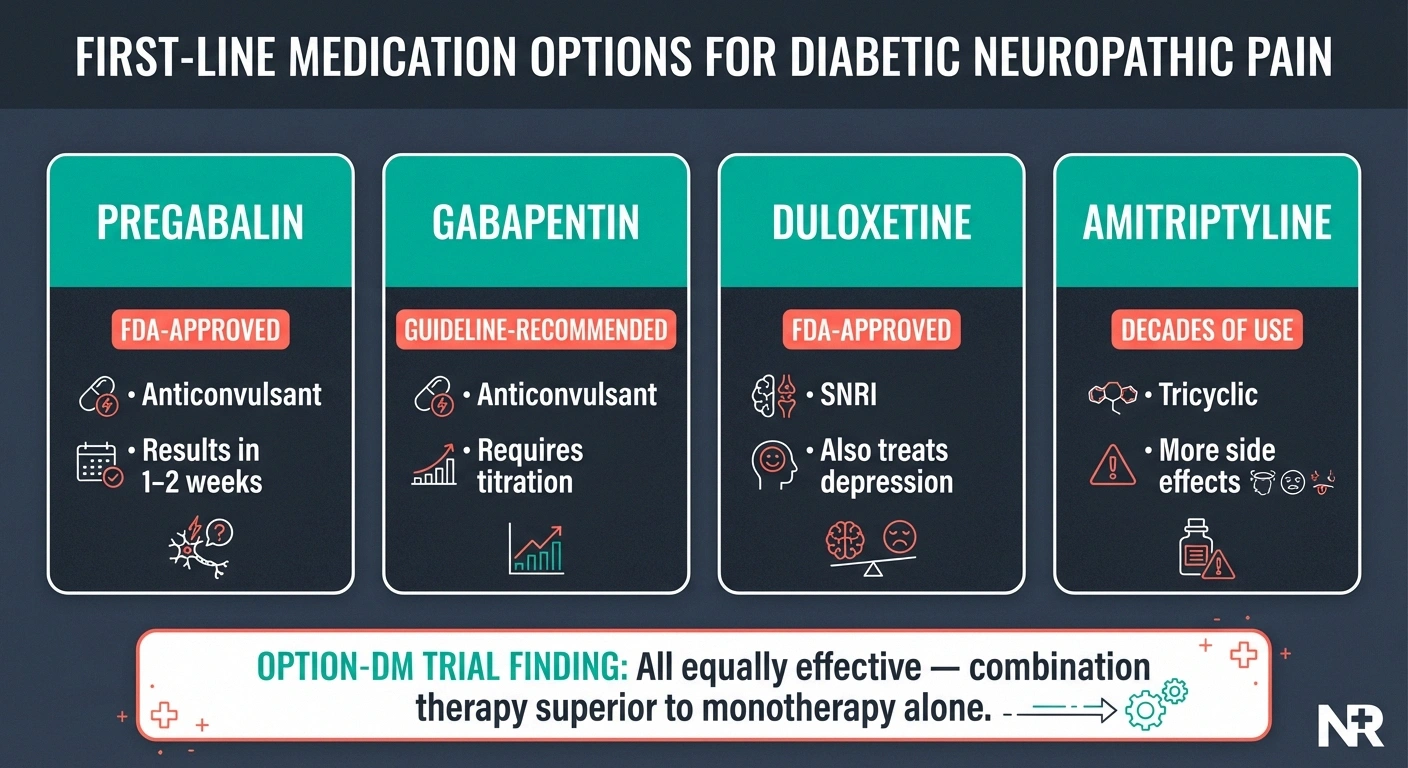
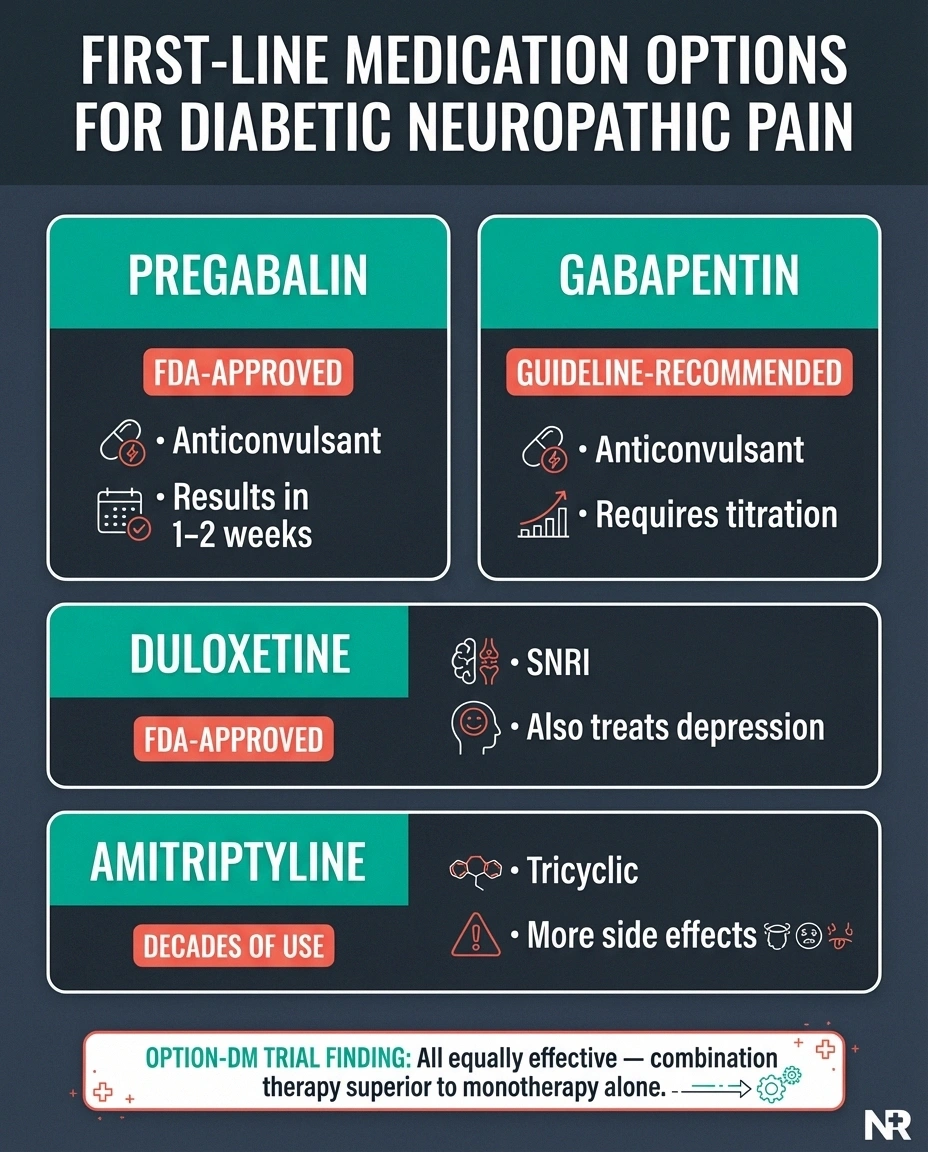
The two FDA-approved medications for diabetic neuropathic pain are pregabalin (Lyrica) and duloxetine (Cymbalta). But several other medications are widely used and supported by clinical evidence. Our complete medication guide covers all options — here's the overview specific to diabetic neuropathy.
Anticonvulsants
Pregabalin is the most studied medication for diabetic neuropathic pain. It works by calming overactive nerve signals and typically shows results within 1-2 weeks. Common side effects include dizziness, drowsiness, and weight gain. Starting at a low dose and gradually increasing helps minimize side effects.
Gabapentin works through a similar mechanism and is often tried first because it's available as a generic and is generally less expensive. While not FDA-approved specifically for diabetic neuropathy, it's recommended by multiple clinical guidelines including the American Academy of Neurology (AAN). It requires titration over several weeks to reach an effective dose.
Antidepressants (SNRIs and Tricyclics)
Duloxetine is an SNRI (serotonin-norepinephrine reuptake inhibitor) that's FDA-approved for diabetic neuropathic pain. It modulates pain processing pathways in the spinal cord and brain. The most common side effects are nausea (usually temporary), dry mouth, and constipation. Duloxetine has the added benefit of treating depression, which frequently coexists with chronic neuropathic pain.
Amitriptyline is a tricyclic antidepressant that has been used for neuropathic pain for decades. While effective, it carries more side effects than newer medications (dry mouth, constipation, drowsiness, weight gain) and requires careful use in older adults and those with heart conditions.
The landmark OPTION-DM trial compared these medication classes head-to-head and found that no single class was significantly superior. This means finding the right medication is about individual response and tolerability — not about one drug being objectively “the best.” Importantly, the trial found that combination therapy (using medications from two different classes together) provided significantly better pain relief for patients who didn't respond adequately to a single drug.
Topical Pain Treatments
Topical treatments offer pain relief at the site of application without the systemic side effects of oral medications. They're particularly useful for people who can't tolerate or prefer to avoid oral medications.

Capsaicin cream works by depleting substance P, a neurotransmitter involved in pain signaling. Over-the-counter capsaicin (0.075%) requires multiple daily applications over several weeks to take effect. Prescription-strength capsaicin patches (8%) are applied by a healthcare provider and can provide pain relief lasting up to 3 months per application. A 2024 review in JAMA highlighted high-concentration capsaicin as a recommended treatment for refractory diabetic neuropathic pain.
Lidocaine patches (5%) provide numbing relief directly over painful areas. They're applied for up to 12 hours and work by blocking sodium channels in local nerve fibers. They're particularly helpful for focal pain areas and have virtually no systemic side effects.
Over-the-counter neuropathy creams containing menthol, camphor, or botanical ingredients may provide temporary comfort. While evidence for these is less robust than for capsaicin and lidocaine, many patients find them useful as part of a broader pain management strategy.
Evidence-Based Natural and Supplement Therapies
Several natural approaches have meaningful clinical evidence for diabetic neuropathy specifically. Our supplement hub covers the full range — here are the ones with the strongest evidence for diabetes-related nerve damage.


Alpha-lipoic acid (ALA) is the most-studied supplement for diabetic neuropathy. Multiple randomized controlled trials — including the SYDNEY and NATHAN trials — demonstrate that 600mg daily reduces pain, burning, and numbness. ALA is approved for diabetic neuropathy treatment in Germany and is recommended in European clinical guidelines. It works as a potent antioxidant that reduces oxidative stress in nerve tissue and may improve nerve blood flow.
B vitamins play a critical role, especially when deficiency is contributing. Metformin — taken by millions with Type 2 diabetes — depletes B12. If you take metformin, get your B12 levels checked regularly. Benfotiamine (a fat-soluble form of B1) has specific evidence for diabetic neuropathy and may be more effective than standard thiamine.
Acetyl-L-carnitine has shown promise in clinical trials for diabetic neuropathy, with evidence of both symptom improvement and nerve fiber regeneration. A dose of 1,000mg twice daily was used in the positive trials.
Omega-3 fatty acids may support nerve health through anti-inflammatory mechanisms. While evidence is still emerging, some clinical trials have shown improvement in nerve conduction velocity and subjective symptoms with omega-3 supplementation.
Physical Therapy and Exercise
Exercise may be the most powerful and underutilized treatment for diabetic neuropathy — and it comes with virtually no negative side effects (when done appropriately).

A growing body of research shows that regular exercise can improve nerve function, reduce neuropathic pain, improve balance, and — most remarkably — may actually promote nerve regeneration. A 2017 study published in Annals of Neurology found that a supervised exercise program increased skin nerve fiber density (a direct measure of nerve health) in people with diabetic neuropathy. This is one of the few interventions shown to actually regrow nerves.
Walking is the simplest starting point. Even 20-30 minutes of daily walking has shown benefits for neuropathy symptoms and blood sugar control. Swimming and water therapy provide the benefits of exercise without the fall risk and impact stress of land-based activity. Yoga combines gentle movement with balance training and stress reduction. Working with a physical therapist who understands neuropathy ensures your exercise program is safe and targeted.
Exercise also directly addresses the underlying diabetes: regular physical activity improves insulin sensitivity, lowers blood sugar, and reduces A1C — attacking the root cause of the neuropathy while simultaneously treating its symptoms.
Advanced Interventions for Severe Cases
When standard medications and therapies don't provide adequate relief, several advanced options are available.
Spinal cord stimulation (SCS) uses a small device implanted near the spinal cord to deliver mild electrical pulses that interrupt pain signals. High-frequency SCS (10kHz) received FDA approval specifically for painful diabetic neuropathy in 2021 after clinical trials showed superior pain relief compared to conventional medical management alone. Candidates typically trial the device temporarily before permanent implantation.
Scrambler therapy is a non-invasive option that uses surface electrodes to send “non-pain” signals along the same nerve pathways that carry pain signals. While still considered emerging, several studies have shown meaningful pain reduction in diabetic neuropathy patients. It requires a series of treatments (typically 10-12 sessions).
TENS units (transcutaneous electrical nerve stimulation) provide a more accessible form of electrical therapy. While evidence is modest compared to SCS, TENS units are safe, affordable, and can be used at home. The 2024 JAMA review described peripheral TENS as “well tolerated and inexpensive” for diabetic neuropathic pain.
Acupuncture has moderate evidence for neuropathic pain relief. A 2017 Cochrane review was cautiously positive, and several subsequent trials have shown benefit. It's generally safe when performed by a licensed practitioner and may be worth trying when other approaches haven't provided sufficient relief.
Foot Care: The Treatment Nobody Thinks About
Foot care isn't glamorous, but it may be the most important “treatment” in diabetic neuropathy — because it prevents the most devastating complications. When you can't feel your feet, small injuries become medical emergencies. Diabetic foot ulcers are a leading cause of non-traumatic amputation, and neuropathy is the primary risk factor.

Daily foot inspection is non-negotiable. Check the tops, bottoms, and between all toes every single day for cuts, blisters, redness, swelling, or temperature changes. Use a mirror for the soles if you can't see them. Our complete foot care guide covers the full protocol, but the essential practices are: never walk barefoot, wear properly fitted shoes, keep feet clean and moisturized, trim nails carefully (or have a podiatrist do it), and see a podiatrist at least annually.
Temperature monitoring is an emerging tool: studies show that areas of elevated foot temperature precede ulceration by about 3 weeks. Some clinicians now recommend daily temperature checks of the feet to catch problems before they become visible.
Managing the Mental Health Impact
Chronic pain from diabetic neuropathy takes a significant toll on mental health. Depression affects up to 30% of people with diabetic neuropathy — roughly double the rate in the general diabetes population. And depression doesn't just make you feel worse emotionally — it amplifies pain perception and reduces treatment adherence.
Cognitive behavioral therapy (CBT) has strong evidence for improving both pain and mood in neuropathy patients. It works by changing the thought patterns that amplify pain perception and teaching practical coping strategies. Mindfulness and meditation practices have also shown benefit in multiple clinical trials.
If you're struggling emotionally, please bring it up with your healthcare team. Treating depression often improves pain levels — and treating pain often improves mood. Breaking into either side of this cycle creates a positive feedback loop. Some neuropathy medications (particularly duloxetine) treat both pain and depression, which is why they're often a good first choice for patients experiencing both.
Building Your Treatment Plan: A Practical Framework
The most effective approach to diabetic neuropathy treatment is layered — combining multiple strategies that address different aspects of the condition. Here's a practical framework for building your plan with your healthcare team.
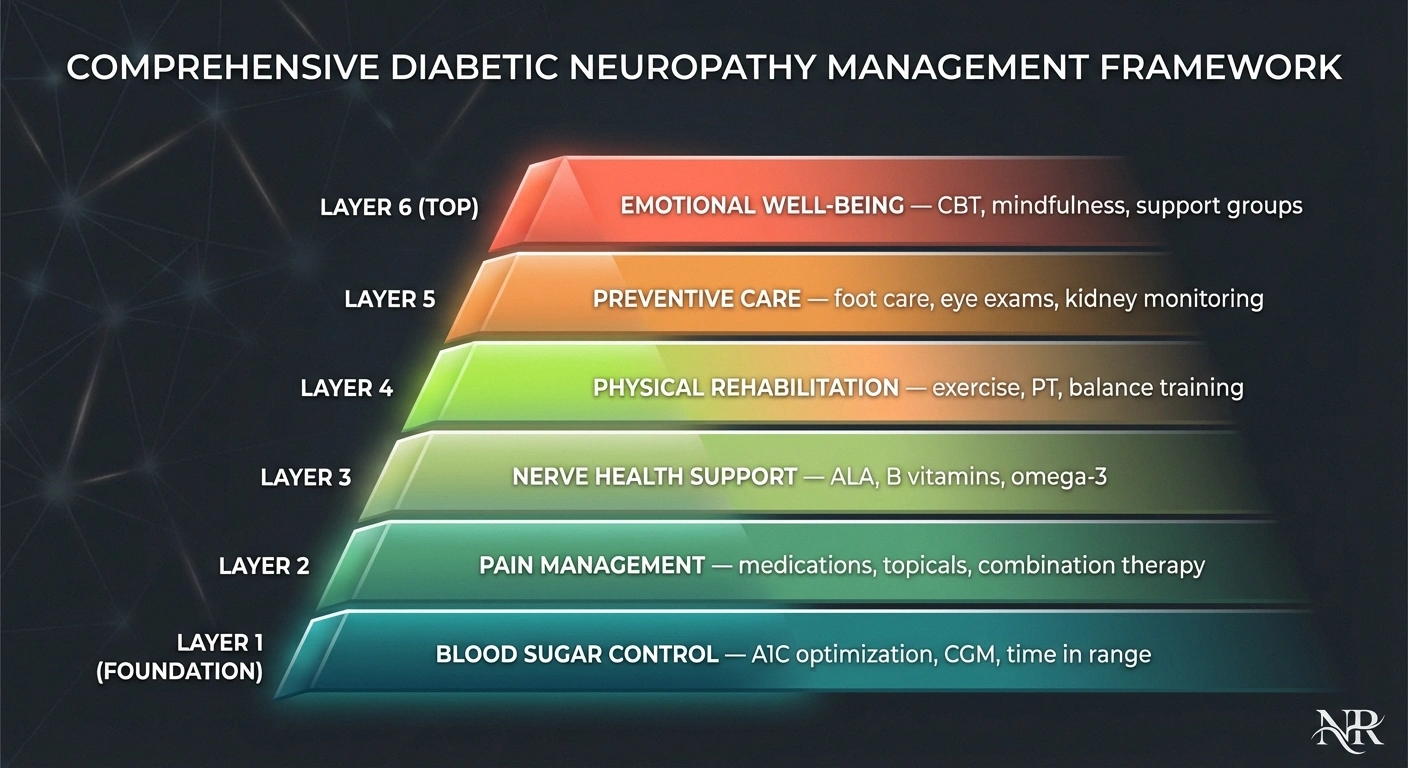
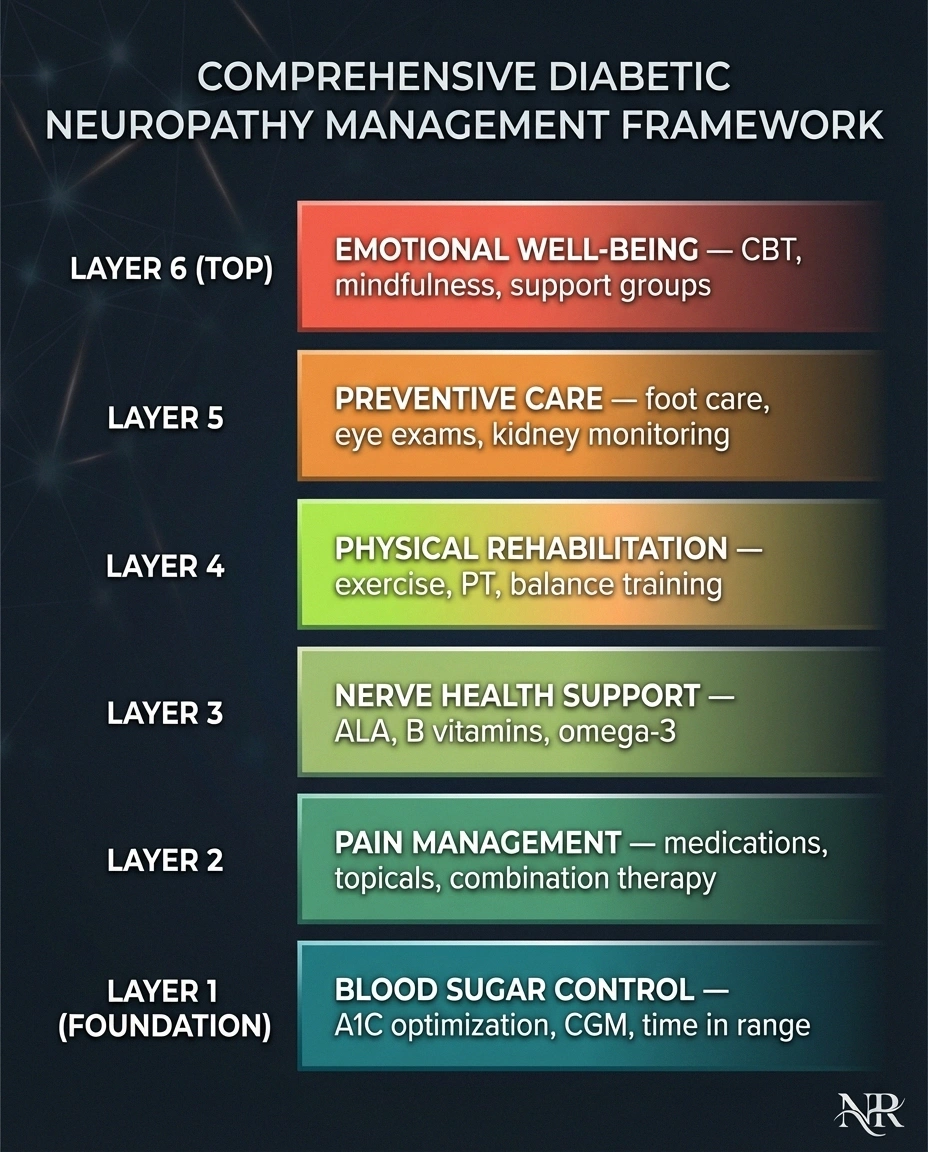
Layer 1: Address the root cause. Blood sugar optimization. Work with your endocrinologist or primary care doctor to bring A1C as close to target as safely possible. Consider continuous glucose monitoring for better time-in-range data.
Layer 2: Treat pain and symptoms. Start with a first-line medication (gabapentin, pregabalin, or duloxetine). Add topical treatments for localized pain. Consider combination therapy if monotherapy isn't sufficient.
Layer 3: Support nerve health. Alpha-lipoic acid (600mg daily), B vitamin optimization (check and supplement if deficient), and omega-3 fatty acids. Correct any nutritional deficiencies identified by blood work.
Layer 4: Physical rehabilitation. Regular exercise program (start with walking, add swimming/yoga as tolerated). Physical therapy for balance and strength. Targeted exercises for affected areas.
Layer 5: Preventive care. Daily foot care routine. Annual comprehensive foot exam. Annual eye exam (retinopathy screening). Regular kidney function monitoring.
Layer 6: Emotional well-being. Address depression and anxiety. Consider CBT or mindfulness training. Connect with support groups.
Bring a list of questions to ask your doctor about each layer. Not every patient needs every layer, but understanding the full toolkit empowers you to advocate for comprehensive care.
Frequently Asked Questions
What is the best medication for diabetic neuropathy?
There is no single best medication. The OPTION-DM trial showed that pregabalin, duloxetine, amitriptyline, and gabapentin have equivalent overall efficacy. The best medication for you depends on your individual response, other health conditions, other medications, and tolerability. Many patients need to try two or three options before finding the right fit. Combination therapy (using two different drug classes together) often works when a single medication alone is insufficient.
Can diabetic neuropathy be reversed?
In some cases, yes — particularly when caught early and blood sugar is brought under tight control. Research has shown that improving glycemic control can allow some nerve regeneration, and exercise may promote nerve fiber regrowth. However, long-standing severe neuropathy is less likely to reverse fully. The earlier you intervene, the better the outcome. Focus on stopping progression and allowing whatever recovery is possible.
Does metformin cause neuropathy?
Metformin doesn't directly damage nerves, but it can deplete vitamin B12 over time, and B12 deficiency causes neuropathy. Studies suggest 10-30% of people on long-term metformin develop B12 deficiency. If you take metformin, get your B12 level checked at least annually and supplement if levels are low. This is one of the most common and easily preventable causes of worsening neuropathy in diabetic patients.
How long does it take for diabetic neuropathy treatment to work?
It depends on the treatment. Pain medications like pregabalin may show effects within 1-2 weeks, while gabapentin requires gradual dose increases over several weeks. Supplements like alpha-lipoic acid typically need 3-5 weeks to show benefit. Nutritional correction (B12, thiamine) may take months to produce noticeable nerve recovery. Exercise benefits accumulate over weeks to months. Blood sugar optimization is an ongoing process. Give each new treatment a fair trial of at least 4-8 weeks before deciding it isn't working.
Is there a diet that helps diabetic neuropathy?
A diet that controls blood sugar is the most important dietary intervention. The anti-inflammatory diet and Mediterranean diet both show promise for neuropathy by reducing inflammation and providing nerve-supporting nutrients. Our neuropathy diet guide covers specific foods that help and hurt nerve health. Key principles: minimize processed sugar and refined carbohydrates, emphasize vegetables, healthy fats, lean protein, and whole grains, and ensure adequate B vitamins through food and supplementation if needed.
Should I see a neurologist or can my endocrinologist manage my neuropathy?
Your endocrinologist manages the diabetes; a neurologist manages the neuropathy. Ideally, you want both working together. A neurologist can provide accurate diagnosis (distinguishing diabetic neuropathy from other types), perform nerve conduction studies, prescribe specialized pain medications, and offer advanced treatment options like spinal cord stimulation referrals. If your pain is not well controlled, if you have rapid progression, or if there's uncertainty about the diagnosis, a neurologist referral is warranted.