
Browse all our neuropathy supplements and nutrition guides for more articles like this one.
If you live with neuropathy, you know the cruel irony: the same nerve pain that exhausts you during the day often gets worse at night, right when you desperately need rest. You're caught in a vicious cycle where pain ruins sleep and poor sleep makes pain worse. So when people ask me about melatonin — a supplement sitting on nearly every pharmacy shelf — I understand why they're hopeful. Could something this simple and accessible actually help with nerve pain and sleep?
The answer is more interesting than a simple yes or no. Emerging research suggests that melatonin may do more than just help you fall asleep — it appears to have genuine pain-modulating properties that could be particularly relevant for people with neuropathic pain. Let's dig into what the science actually says, what melatonin can and can't do, and how to use it wisely.
What Is Melatonin, Exactly?
Melatonin is a hormone produced naturally by your pineal gland — a pea-sized structure deep in your brain. As daylight fades, your brain ramps up melatonin production, signaling to your body that it's time to prepare for sleep. When the sun rises, production drops, and you feel more alert.
But melatonin is far more than a sleep switch. Your body also produces it in your gut, bone marrow, and other tissues, where it plays roles in immune function, antioxidant defense, and inflammation regulation. This wider biological role is what makes melatonin relevant to neuropathy — not just as a sleep aid, but as a molecule that may influence pain processing itself.
Melatonin supplements — synthetic versions of this natural hormone — are widely available over the counter in the United States, though they require a prescription in some other countries. They come in standard tablets, extended-release formulas, gummies, liquids, and sublingual dissolving tablets.
The Pain-Sleep Connection in Neuropathy
Before we talk about how melatonin might help, it's important to understand why the relationship between neuropathy and sleep matters so much.
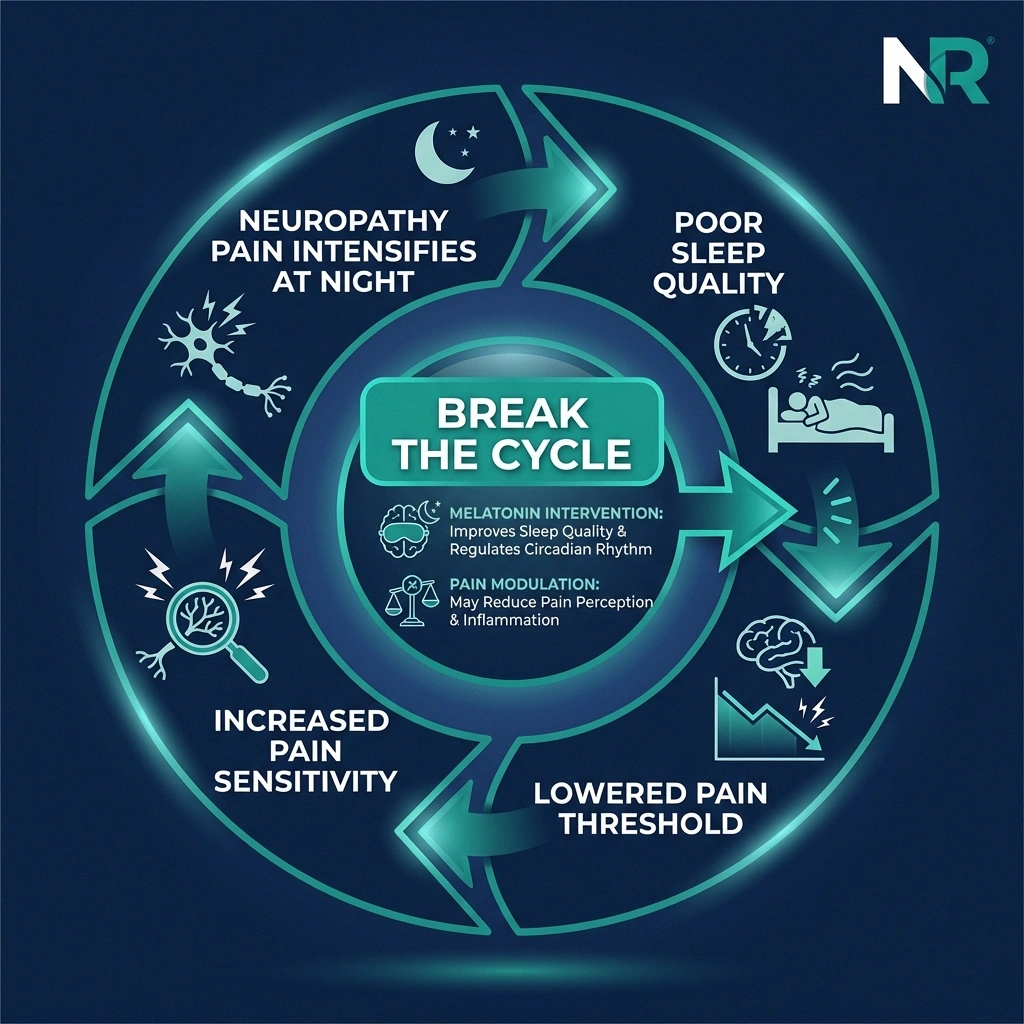
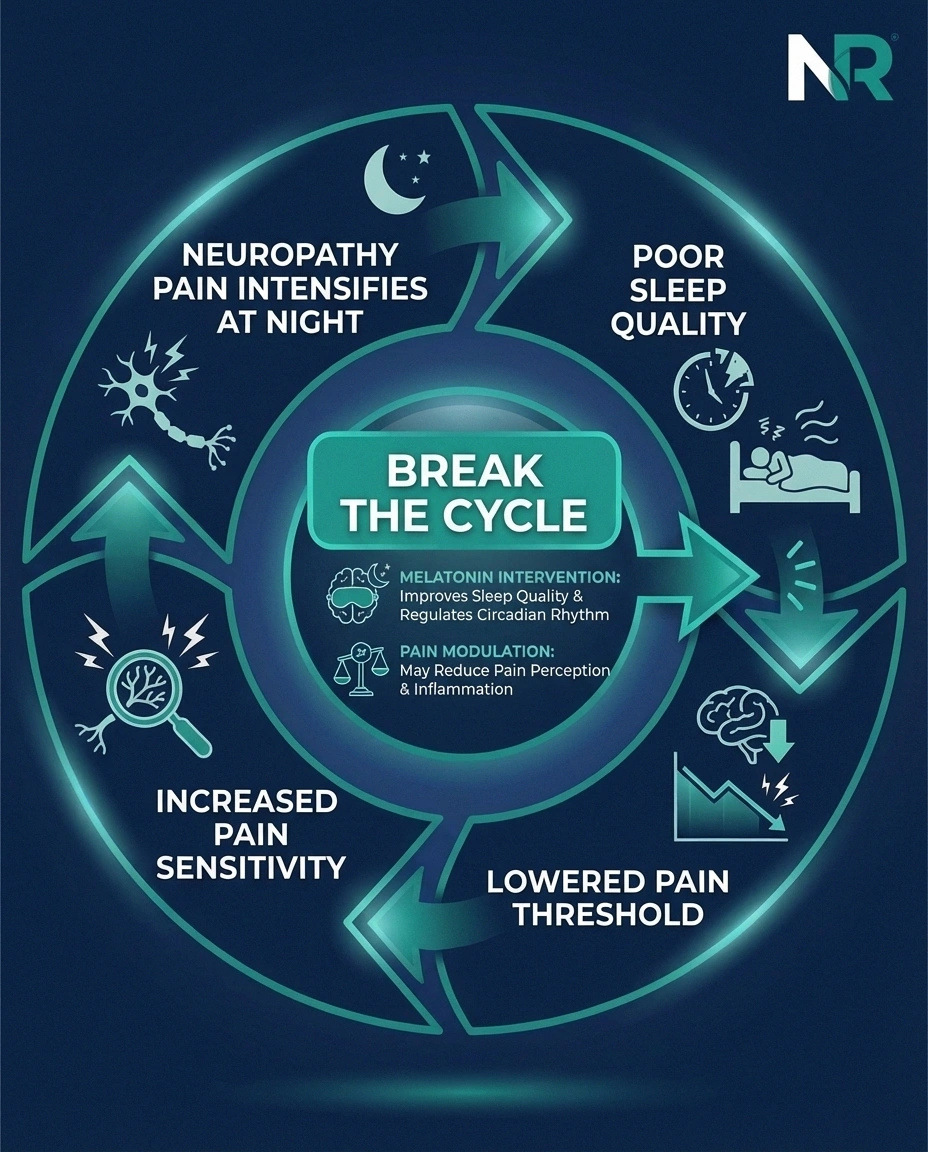
Research has established a clear bidirectional relationship between pain and sleep:
- Pain disrupts sleep. Neuropathic pain — the burning, tingling, shooting sensations — tends to intensify in the evening and nighttime hours. A 2021 study examining patients with diabetic neuropathy found that as neuropathy symptoms worsened, sleep quality declined proportionally across every measured dimension: time to fall asleep, total sleep time, and sleep efficiency.
- Poor sleep amplifies pain. Sleep deprivation lowers your pain threshold. “The structures in the brain that are associated with sleep are also associated with pain,” explains Gabriella Gobbi, MD, a neuroscientist at McGill University. “If you don't sleep, the threshold of pain decreases.” This means the same nerve signals that might be tolerable when you're well-rested become significantly more painful when you're sleep-deprived.
- The cycle feeds itself. Pain causes poor sleep, which increases pain sensitivity, which further disrupts sleep. Without intervention, this spiral can significantly worsen quality of life — affecting mood, function, and even nerve healing.
This is where melatonin becomes interesting. If it can improve sleep quality and independently reduce pain sensitivity, it could potentially break this cycle at two points simultaneously.
What Research Says About Melatonin and Nerve Pain
The research on melatonin and neuropathic pain is still evolving, but what we have so far is genuinely encouraging. Here's what the evidence shows:
Animal Studies: Strong Signals
A comprehensive review published in the Journal of Pain Research analyzed a large body of preclinical evidence and found that melatonin administration consistently reduced pain in animal models of neuropathy. Specifically, melatonin:
- Alleviated thermal hyperalgesia (excessive sensitivity to heat) in sciatic nerve injury models
- Reduced cold allodynia (pain from cold that shouldn't be painful)
- Reversed mechanical pain thresholds in spinal nerve ligation models
- Showed dose-dependent effects — meaning higher doses produced greater pain relief
A particularly revealing study from 2014 found that sleep-deprived animals were significantly more vulnerable to nerve injury-induced pain, and this vulnerability was directly linked to lower melatonin levels. When melatonin was administered to these sleep-deprived animals, it restored pain thresholds and reduced inflammatory markers.
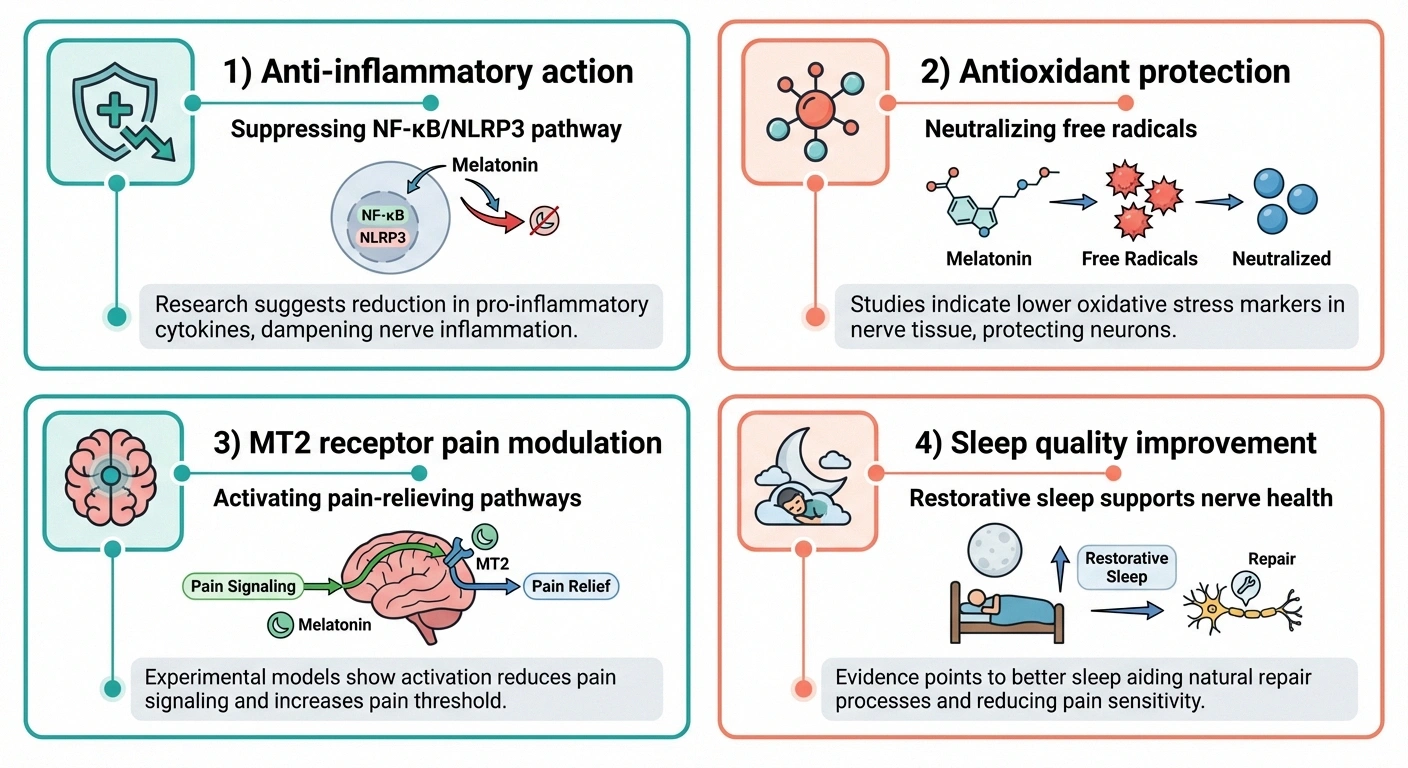
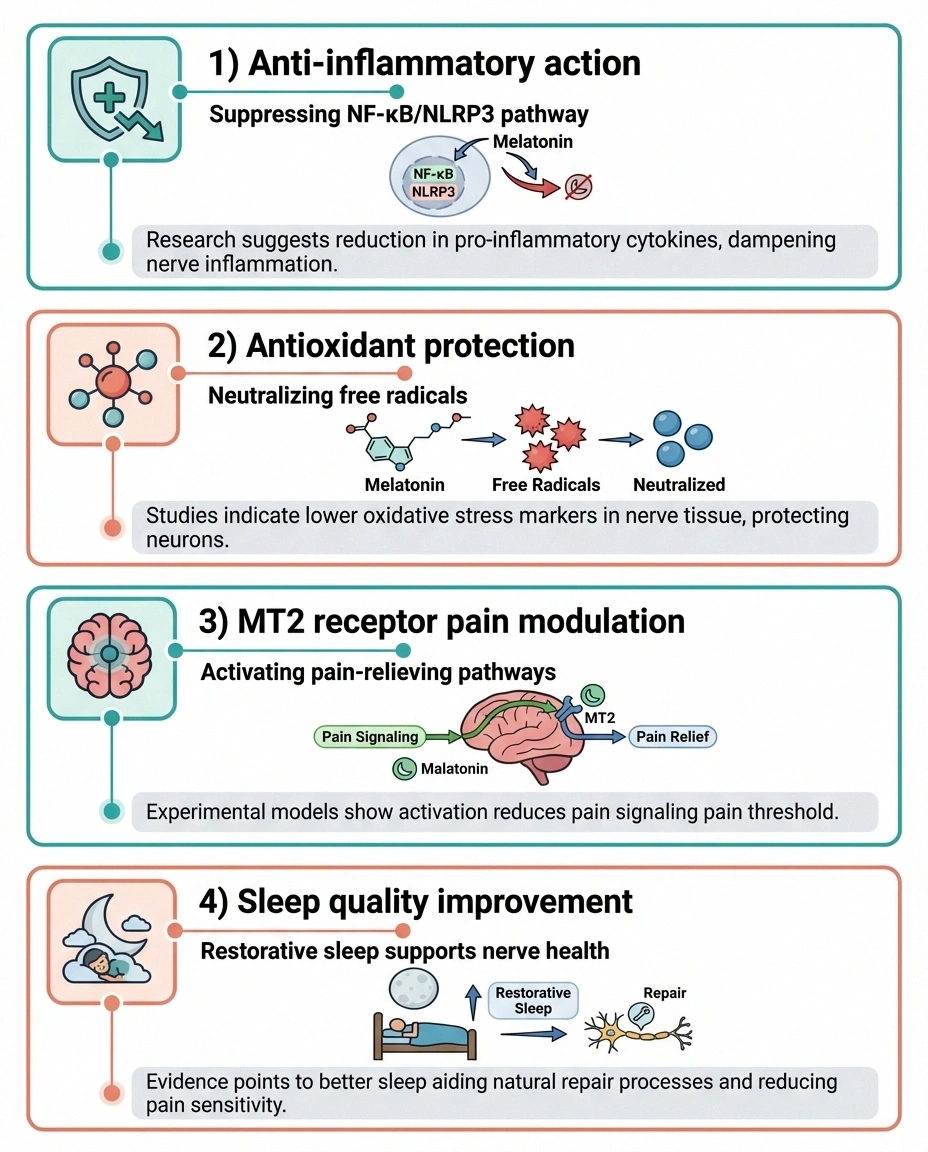
The Anti-Inflammatory Mechanism
One of the most promising findings is melatonin's apparent ability to reduce neuroinflammation — a key driver of neuropathic pain. A 2023 study published in Scientific Reports demonstrated that exogenous melatonin alleviated neuropathic pain-induced emotional disturbances by suppressing the NF-κB/NLRP3 inflammatory pathway. This pathway is a critical mediator of the inflammation that drives chronic nerve pain.
In simpler terms: melatonin didn't just mask the pain — it appeared to address one of the underlying inflammatory processes that generates neuropathic pain in the first place.
Antioxidant Protection for Nerves
Melatonin is one of the most potent natural antioxidants your body produces. Free radicals and oxidative stress play a significant role in nerve damage — they're implicated in diabetic neuropathy, chemotherapy-induced neuropathy, and many other forms of nerve injury. By neutralizing free radicals, melatonin may help protect nerves from further damage and support the regeneration process.
Research has shown that melatonin can protect myelin sheaths (the protective coating around nerve fibers) from oxidative damage and may even support nerve regeneration after injury. While this doesn't mean melatonin can reverse existing neuropathy, it suggests a potential neuroprotective role — especially when combined with other treatments.
The MT2 Receptor Discovery
One of the most exciting developments in melatonin research involves the discovery that the MT2 melatonin receptor in the brain appears to be specifically involved in pain modulation — in addition to its role in sleep. Dr. Gobbi's lab at McGill University is developing melatonin analogs (synthetic molecules that target these receptors more precisely) that could potentially deliver stronger analgesic effects than over-the-counter melatonin.
This research is still in its early stages, but it suggests that the pain-relieving effects of melatonin are not merely a side effect of better sleep — they appear to operate through a distinct neurological pathway.
Human Clinical Evidence
While animal data is strong, human evidence is still limited but growing. A double-blind randomized controlled trial protocol published in 2022 was designed specifically to test melatonin for neuropathic pain in humans, recognizing the gap between preclinical promise and clinical proof. This study aims to evaluate whether melatonin can reduce pain intensity and improve sleep in patients with chronic neuropathic pain.
Several smaller human studies have shown:
- Melatonin supplementation improved sleep quality in chronic pain patients
- Some patients reported reduced pain intensity alongside improved sleep
- Melatonin was well-tolerated with minimal side effects compared to prescription sleep medications
- The effects appeared most pronounced in patients whose pain was worst at night
The honest assessment: we have strong biological rationale and encouraging preliminary evidence, but we don't yet have the large-scale clinical trials that would make melatonin a proven treatment for neuropathic pain. What we do have is enough evidence to consider it a reasonable complement to existing treatments — especially given its excellent safety profile.
How Melatonin May Help Your Neuropathy
Based on the available evidence, melatonin may benefit people with neuropathy through multiple mechanisms:
- Improving sleep quality. This is melatonin's most well-established benefit and, for neuropathy patients, potentially the most impactful. Better sleep raises pain thresholds, improves mood, and supports the body's natural healing processes — including nerve repair.
- Reducing neuroinflammation. By suppressing inflammatory pathways like NF-κB/NLRP3, melatonin may directly reduce the inflammatory component of neuropathic pain.
- Providing antioxidant protection. Melatonin's powerful antioxidant properties may help protect nerves from ongoing oxidative damage and support regeneration.
- Modulating pain signals. Through MT2 receptors and interactions with the body's opioid system, melatonin appears to influence how pain signals are processed in the brain.
- Breaking the pain-sleep cycle. By working on both sides of the pain-sleep connection simultaneously, melatonin may be uniquely positioned to interrupt the vicious cycle that makes neuropathy worse over time.
Dosage: How Much Melatonin Should You Take?
Here's something important that most people get wrong about melatonin: more is not necessarily better. In fact, too much melatonin can actually disrupt your sleep architecture and leave you feeling groggy.

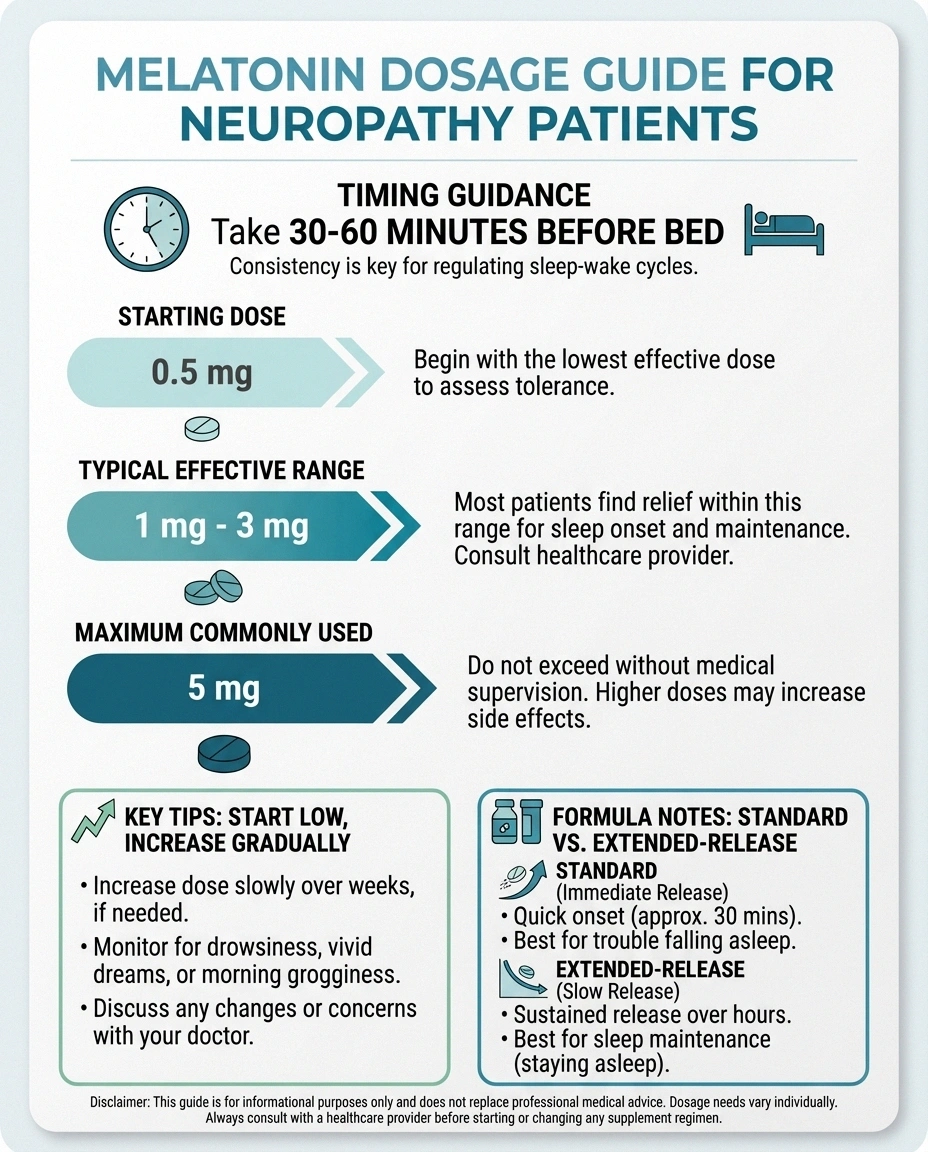
For sleep improvement:
- Starting dose: 0.5 to 1 milligram, taken thirty to sixty minutes before bedtime
- Typical effective dose: 1 to 3 milligrams for most people
- Maximum commonly used: 5 milligrams (higher doses have not shown additional sleep benefits in most studies)
For pain modulation: The pain-related research has used doses ranging from 3 to 10 milligrams, though there's no established clinical dosing for neuropathic pain specifically. Dr. Gobbi notes that “only a minimal part goes into the brain” with oral dosing, which means “you need a very high dose to have an effect” on pain pathways. However, higher doses also increase the likelihood of next-day grogginess.
Practical approach: Start low (0.5–1 mg) and increase gradually if needed. If 3 milligrams helps you sleep better without grogginess, that's likely your sweet spot. Going higher specifically for pain relief is reasonable to try, but do so in conversation with your doctor.
Timing matters: Take melatonin thirty to sixty minutes before your intended bedtime. Taking it too early or too late can shift your circadian rhythm in unintended ways. Extended-release formulas may be better if you tend to wake up in the middle of the night, while standard-release forms are better if your main problem is falling asleep.
Choosing the Right Melatonin Supplement
Not all melatonin supplements are created equal. Because they're classified as dietary supplements in the United States, they're not subject to the same quality controls as prescription medications. Studies have found that actual melatonin content in supplements can vary significantly from what's listed on the label — sometimes containing much more or less than stated.
Here's what to look for:
- Third-party testing. Look for supplements verified by USP (United States Pharmacopeia), NSF International, or ConsumerLab. These organizations independently verify that the product contains what it claims.
- Pharmaceutical-grade melatonin. Some brands specifically label their melatonin as pharmaceutical grade, indicating higher purity standards.
- Avoid unnecessary additives. Some melatonin products include added ingredients like valerian root, L-theanine, or herbal blends. While these aren't necessarily harmful, they make it harder to assess what's actually helping you.
- Form matters. Sublingual (under the tongue) melatonin may absorb more quickly than swallowed tablets. Extended-release formulas provide a steadier level throughout the night.
Safety, Side Effects, and Interactions
Melatonin has an excellent safety profile compared to most sleep and pain medications. However, it's not without considerations:
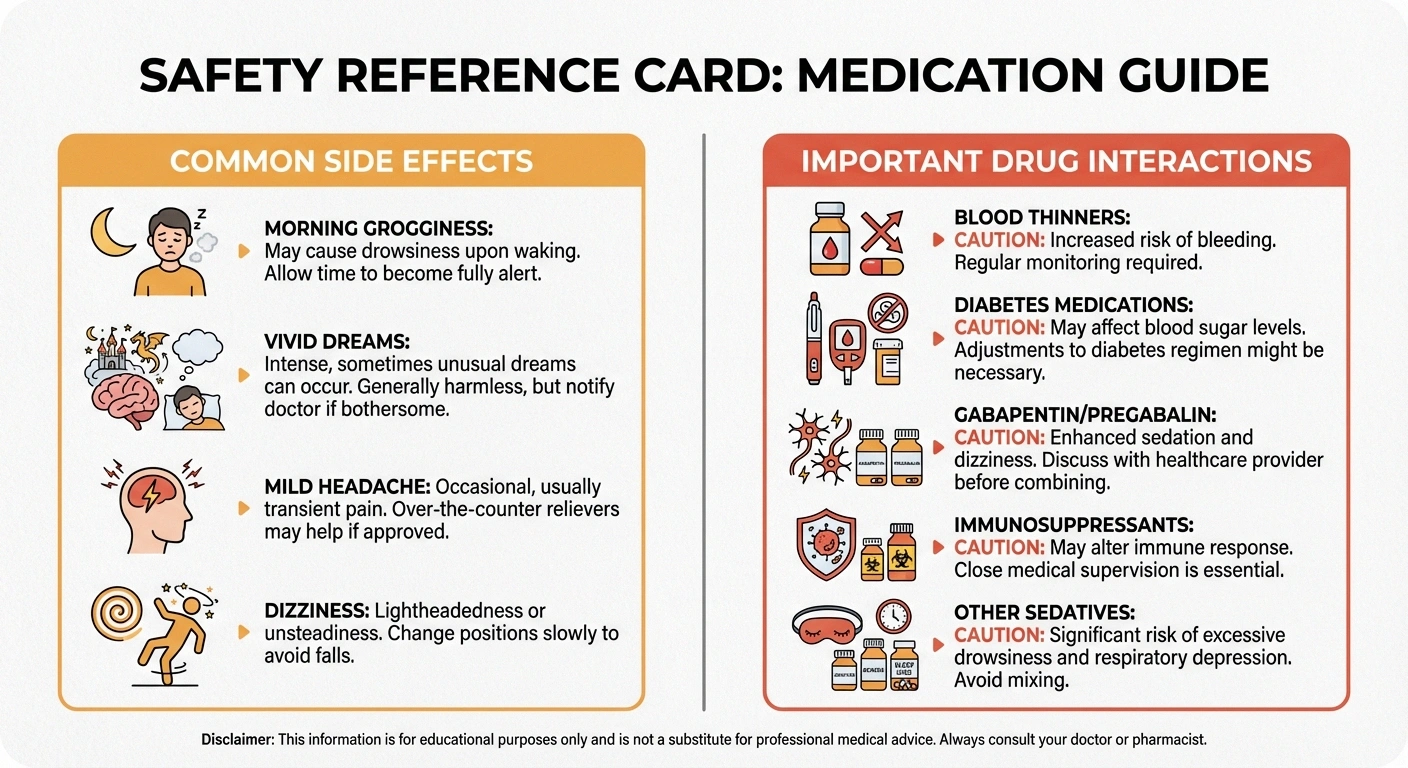
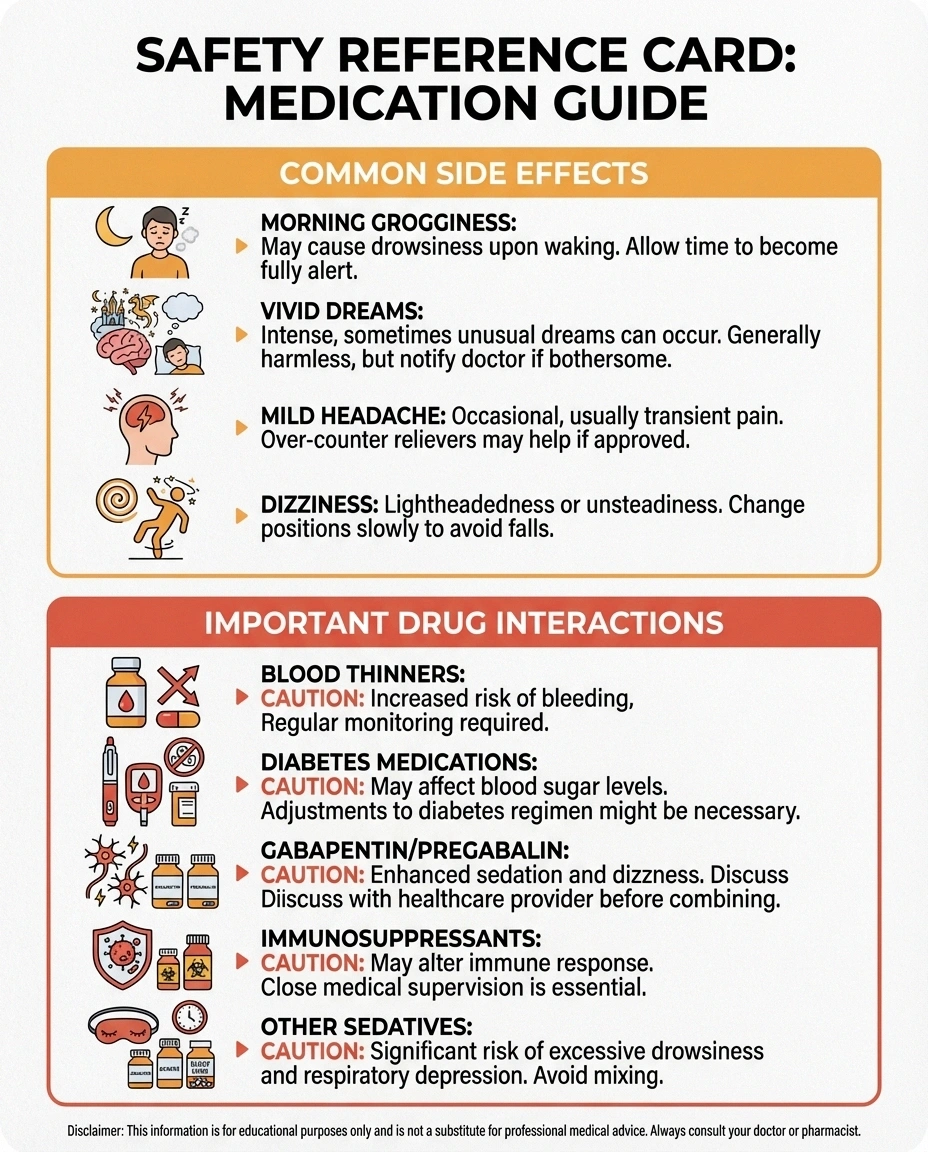
Common side effects (usually mild):
- Morning grogginess or drowsiness (especially at higher doses)
- Vivid dreams or nightmares
- Mild headache
- Dizziness
- Nausea (uncommon)
Important interactions to know about:
- Blood thinners (warfarin, aspirin) — Melatonin may enhance anticoagulant effects. If you take blood thinners, talk to your doctor before starting melatonin.
- Diabetes medications — Melatonin may affect blood sugar levels. People with diabetic neuropathy should monitor their blood sugar carefully when starting melatonin.
- Gabapentin and pregabalin — Melatonin may enhance sedative effects. This can be beneficial (better sleep) or problematic (excessive drowsiness). Start with a lower dose of melatonin if you're already taking these medications.
- Immunosuppressant medications — Melatonin has immune-modulating properties and may interfere with immunosuppressive therapy.
- Other sedatives and sleep medications — Combining melatonin with prescription sleep aids, benzodiazepines, or antihistamines used for sleep can cause excessive sedation.
Long-term safety: Melatonin does not appear to cause dependence, tolerance, or withdrawal — a significant advantage over many prescription sleep medications. Your body continues to produce its own melatonin even when you supplement, and you can stop taking it without rebound insomnia in most cases. However, long-term studies beyond a few years are limited.
Melatonin vs. Prescription Sleep Medications for Neuropathy
Many neuropathy patients are prescribed medications that serve double duty as both pain relievers and sleep aids — particularly gabapentin and pregabalin, which reduce nerve pain and have sedating effects. How does melatonin compare?
Melatonin is not a replacement for prescription neuropathy medications. If you have significant nerve pain that's being managed with gabapentin, pregabalin, or other prescribed medications, melatonin should be considered a complement — not a substitute. Don't stop or reduce your prescribed medications to try melatonin instead.
Where melatonin may add value:
- If your prescription medications help with pain but don't fully resolve your sleep problems
- If you want to improve sleep quality without increasing the dose of sedating medications
- If you're looking for a low-risk addition to your existing treatment plan
- If you're concerned about the long-term effects of prescription sleep aids
- As a first-line approach for mild neuropathy where prescription medications haven't been started
The ideal approach for many neuropathy patients may be a combination: prescription medications targeting nerve pain specifically, plus melatonin to optimize sleep quality and provide additional anti-inflammatory and antioxidant support.
Practical Tips for Better Sleep With Neuropathy
Melatonin works best when combined with good sleep hygiene practices. These strategies can amplify melatonin's effectiveness:

Create a sleep-friendly environment. Keep your bedroom cool (studies suggest sixty-five to sixty-eight degrees Fahrenheit is optimal), dark, and quiet. Consider blackout curtains and a white noise machine if needed.
Manage nighttime pain proactively. Rather than waiting for pain to wake you up, time your evening medications to provide coverage through the night. Some people find that topical creams applied before bed can provide localized relief. A warm foot soak before bedtime may also help reduce evening pain levels.
Mind your light exposure. Bright light (especially blue light from screens) suppresses natural melatonin production. Dim the lights and avoid screens for sixty to ninety minutes before bed. If you must use devices, enable night mode or use blue-light-blocking glasses.
Position for comfort. Nerve pain often worsens with pressure. Use pillows to support affected limbs and prevent compression. If your feet are affected, try keeping sheets and blankets off them with a bed frame tent or blanket lifter.
Maintain a consistent schedule. Go to bed and wake up at roughly the same time every day — even on weekends. This consistency reinforces your circadian rhythm and helps melatonin (both natural and supplemental) work more effectively.
Limit stimulants. Caffeine can interfere with sleep for eight or more hours after consumption. If you have neuropathy and sleep problems, try cutting off caffeine by early afternoon.
What Melatonin Won't Do
In the interest of setting realistic expectations, let me be clear about melatonin's limitations:
- It won't cure neuropathy. Melatonin may support nerve health and reduce symptoms, but it's not going to reverse existing nerve damage.
- It's not a strong painkiller. If your neuropathic pain is moderate to severe, melatonin alone is unlikely to provide adequate relief. It may take the edge off, especially at night, but it's not comparable to prescription pain management.
- It doesn't work instantly. Unlike prescription sleep aids, melatonin often takes several days to a week of consistent use before you notice significant improvements in sleep quality.
- It may not help everyone. Some people respond well to melatonin supplementation; others notice little difference. Your response may depend on your baseline melatonin levels, the severity of your pain, and individual biological factors.
Other Supplements Worth Considering Alongside Melatonin
If you're exploring supplements for neuropathy management, melatonin can be part of a broader strategy. Other supplements with evidence supporting nerve health include:
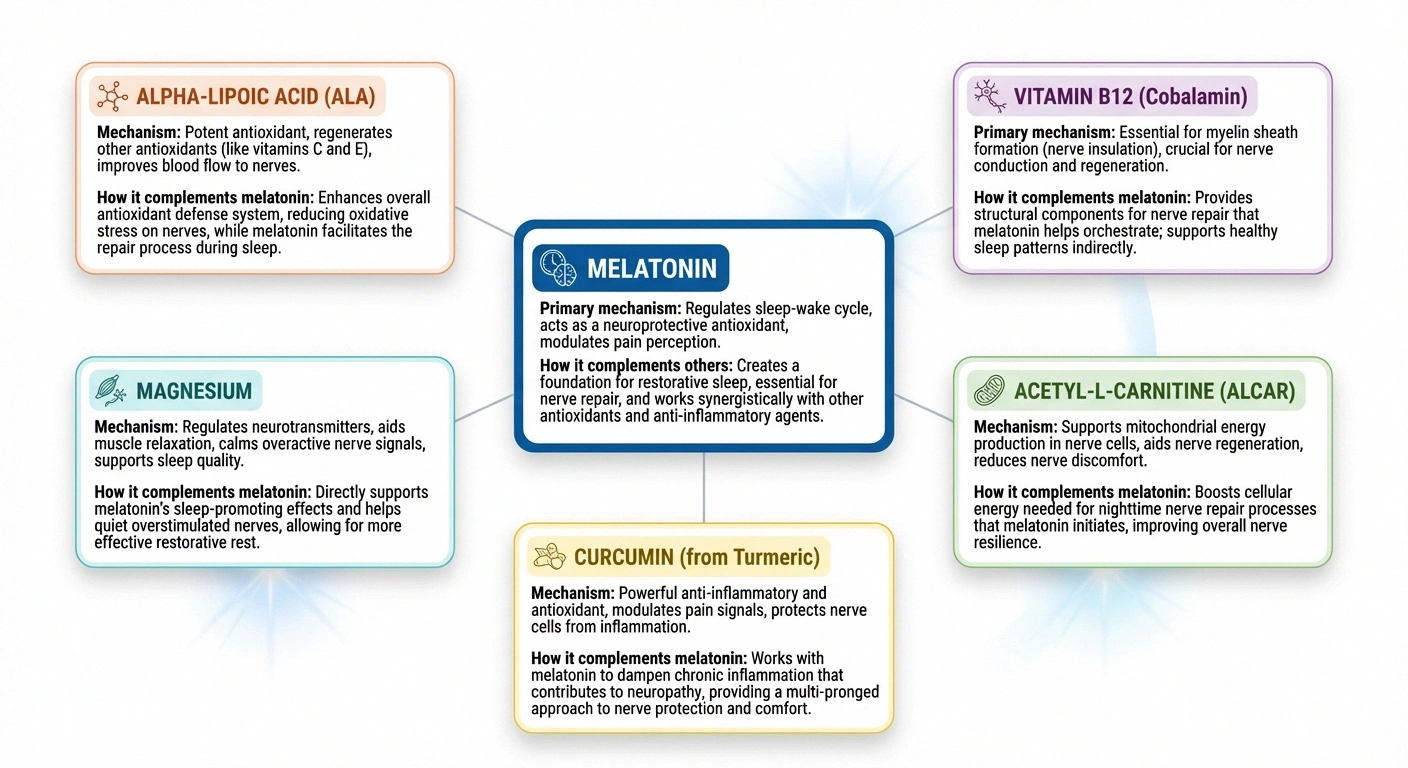
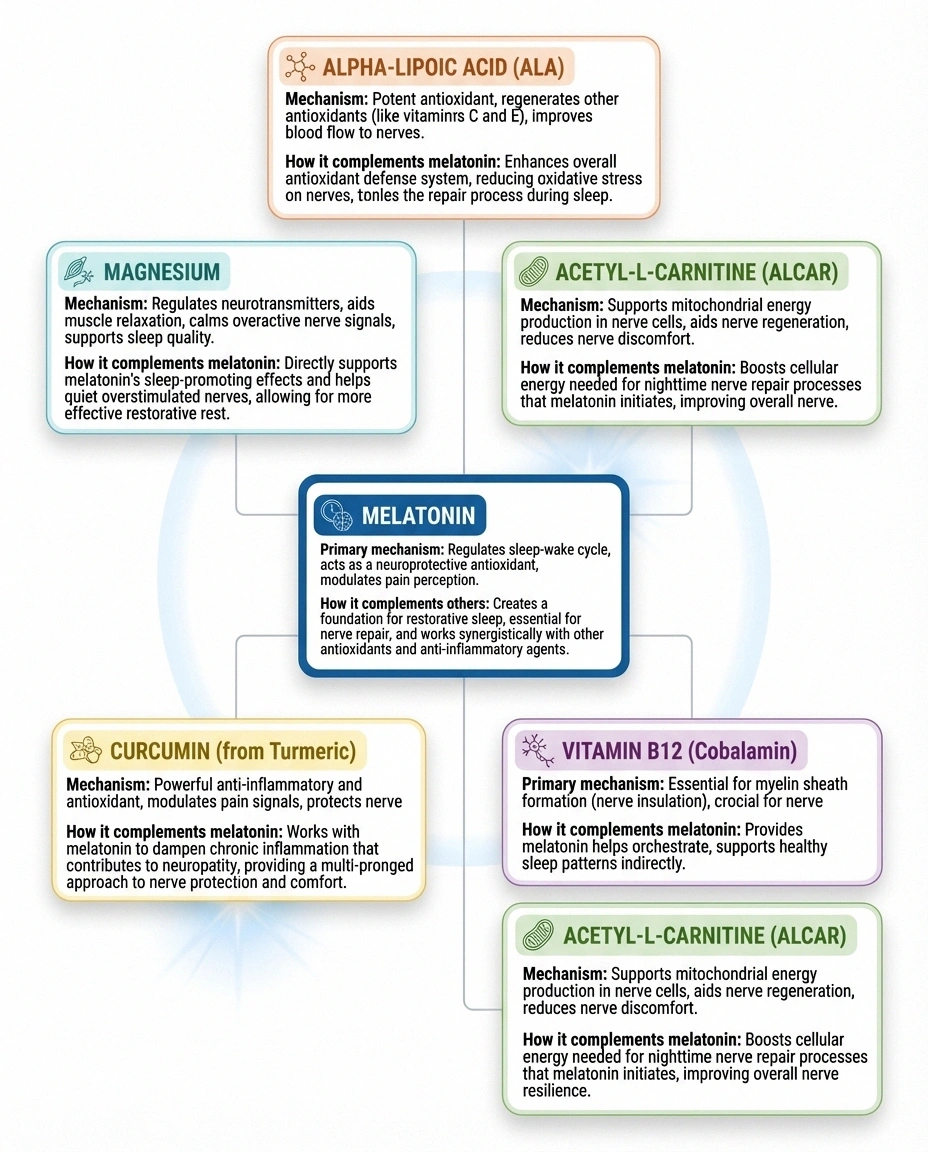
- alpha-lipoic acid supplements — The most studied supplement for diabetic neuropathy, with antioxidant properties that complement melatonin's effects.
- Vitamin B12 — Essential for nerve function and myelin production. Deficiency is a treatable cause of neuropathy.
- Acetyl-L-carnitine — May support nerve regeneration and reduce neuropathic pain, particularly in diabetic and chemotherapy-induced neuropathy.
- Magnesium — Plays a role in nerve signaling and may help with muscle cramps and sleep quality.
- Curcumin (turmeric) — Anti-inflammatory properties that may complement melatonin's inflammation-reducing effects.
As always, discuss any supplement additions with your doctor — especially if you're taking prescription medications for neuropathy. For a comprehensive overview, see our guide to the best supplements for nerve health.
Frequently Asked Questions
Can melatonin help with diabetic neuropathy specifically?
There's particular relevance for diabetic neuropathy because oxidative stress and inflammation are major drivers of diabetic nerve damage — and these are exactly the pathways melatonin targets. Melatonin's antioxidant properties may help protect nerves from ongoing glucose-related damage. However, people with diabetes should monitor blood sugar carefully when starting melatonin, as it may affect glucose metabolism.
Is melatonin safe to take with gabapentin or Lyrica?
Generally yes, but use caution. Both gabapentin and pregabalin (Lyrica) have sedating effects, and adding melatonin may increase drowsiness. Start with a low dose of melatonin (0.5–1 mg) and see how you respond. Many patients find this combination helpful — the prescription medication handles pain, while melatonin optimizes sleep quality. Discuss with your doctor before combining them.
How long should I try melatonin before deciding if it works?
Give melatonin at least two to four weeks of consistent nightly use before assessing its effectiveness. Unlike prescription sleep aids that work immediately, melatonin's effects on sleep quality and pain may build gradually. Keep a simple sleep and pain diary to track changes objectively.
Can I take melatonin every night long-term?
Current evidence suggests that nightly melatonin use is safe for most adults, even over periods of months to years. Unlike many sleep medications, melatonin doesn't appear to cause tolerance (needing increasing doses) or dependence. However, long-term studies beyond five years are limited. It's reasonable to periodically reassess whether you still need it — try stopping for a few nights to see if your sleep remains improved.
Does melatonin help with the burning sensation of neuropathy?
Some patients report that the burning sensation of neuropathy feels less intense after starting melatonin, particularly at night. This may be because better sleep raises pain thresholds, or because melatonin's anti-inflammatory effects reduce nerve inflammation. However, for significant burning pain, melatonin alone is unlikely to be sufficient — it should be part of a comprehensive treatment approach.
Is melatonin better than CBD oil for neuropathy sleep problems?
These supplements work through different mechanisms. Melatonin specifically targets circadian rhythm and has demonstrated anti-inflammatory and antioxidant effects in nerve tissue. CBD oil interacts with the endocannabinoid system and may affect pain perception. The evidence base for melatonin's safety profile is more established. Some people use both, but always discuss this with your doctor, especially if you take other medications.

The Bottom Line: A Promising Piece of the Puzzle
Melatonin isn't a miracle cure for neuropathy — no honest assessment would claim that. But it's shaping up to be something potentially more valuable: a safe, accessible, well-tolerated supplement that may address multiple aspects of the neuropathy experience simultaneously — sleep, inflammation, oxidative damage, and pain signaling.
For the millions of people lying awake at night with burning feet or tingling hands, even modest improvement in sleep quality can be transformative. Better sleep means better pain tolerance, better mood, and better conditions for your body to heal.
If you're considering trying melatonin for your neuropathy-related sleep problems, here's my suggestion: talk to your doctor, start with a low dose, be consistent for at least two to four weeks, combine it with good sleep hygiene practices, and keep realistic expectations. It may not change everything — but it might change enough to help you get the rest your body desperately needs.
And that rest? It's not just comfort. It's medicine.


