
Neuropathy and Aging: What Changes After 60 and How to Protect Your Nerves
I still remember the day I realized my feet didn't feel quite the same as they used to. I was 58, walking barefoot across my kitchen floor, and it hit me — the cool tile that once felt refreshing now felt muffled, like my feet were wrapped in thin cotton. At the time, I didn't think much of it. “That's just getting older,” I told myself.
But over the next few years, as the numbness crept from occasional to constant, I learned something important: while some nerve changes are a normal part of aging, neuropathy is not something you have to simply accept. Understanding the difference between age-related nerve changes and actual neuropathy can mean the difference between managing symptoms early and dealing with advanced nerve damage later.
If you're over 60 and wondering whether those tingling toes or clumsy fingers are “just aging” — this article is for you.
How Aging Naturally Affects Your Nerves
Your nervous system isn't immune to the passage of time. Just as your hair grays and your joints stiffen, your nerves undergo changes that are considered a normal part of aging. Understanding these changes helps you recognize when something has crossed the line from “normal” to “needs attention.”
Research published in the journal Revue Neurologique found that age-related peripheral nervous system changes include decreased sensory and motor nerve conduction velocities, reduced amplitude of sensory potentials, and loss of ankle jerk reflexes in nearly two-thirds of individuals over 65. These changes tend to increase beyond age 80.
Here's what's happening inside your nervous system as the decades pass:
Nerve Fibers Thin and Decline
With aging, both myelinated and unmyelinated nerve fibers naturally decrease in number and density. The myelin sheath — that protective coating around your nerves that helps signals travel quickly — gradually thins. Think of it like the insulation on old electrical wiring: as it wears down, signals travel slower and less efficiently.
of adults over 65 show measurable changes in peripheral nerve function — but most don't affect quality of life
Nerve Signals Slow Down
Motor nerve conduction velocity decreases by approximately 0.4 meters per second per decade after age 40. Sensory nerve conduction slows even more. This means your brain takes slightly longer to receive messages from your hands and feet — and slightly longer to send commands back.
Reflexes Weaken
The ankle jerk reflex (Achilles reflex) is one of the first to decline with age. Studies show it's absent in about 30-50% of healthy adults over 60, and even more in those over 80. While this is considered a normal finding, it also means your body's automatic protective responses become less reliable.
Blood Flow to Nerves Decreases
Small blood vessels that nourish your nerves (the vasa nervorum) become less efficient with age. Reduced blood flow means your nerves receive less oxygen and fewer nutrients, making them more vulnerable to damage from other conditions like diabetes or vitamin deficiencies.
Nerve Regeneration Slows
When you're young, damaged nerves can regenerate at roughly 1 inch per month. In older adults, this regeneration rate drops significantly. A nerve injury that might resolve in weeks for a 30-year-old could take months — or never fully recover — in someone over 70.
Normal Aging vs. Neuropathy: How to Tell the Difference
This is the question I hear most often from people in my support group: “How do I know if this is just aging or actual neuropathy?” It's a fair question, because the early symptoms can look remarkably similar.
🔵 Normal Aging
• Mild, symmetrical changes
• Slightly reduced sensitivity
• Slower reflexes
• Doesn't impact daily life
• Gradual, stable progression
🔴 Neuropathy
• More pronounced symptoms
• Persistent numbness or pain
• Burning, tingling, weakness
• Interferes with daily activities
• Progressive without treatment
The key differences come down to severity, pattern, and progression:
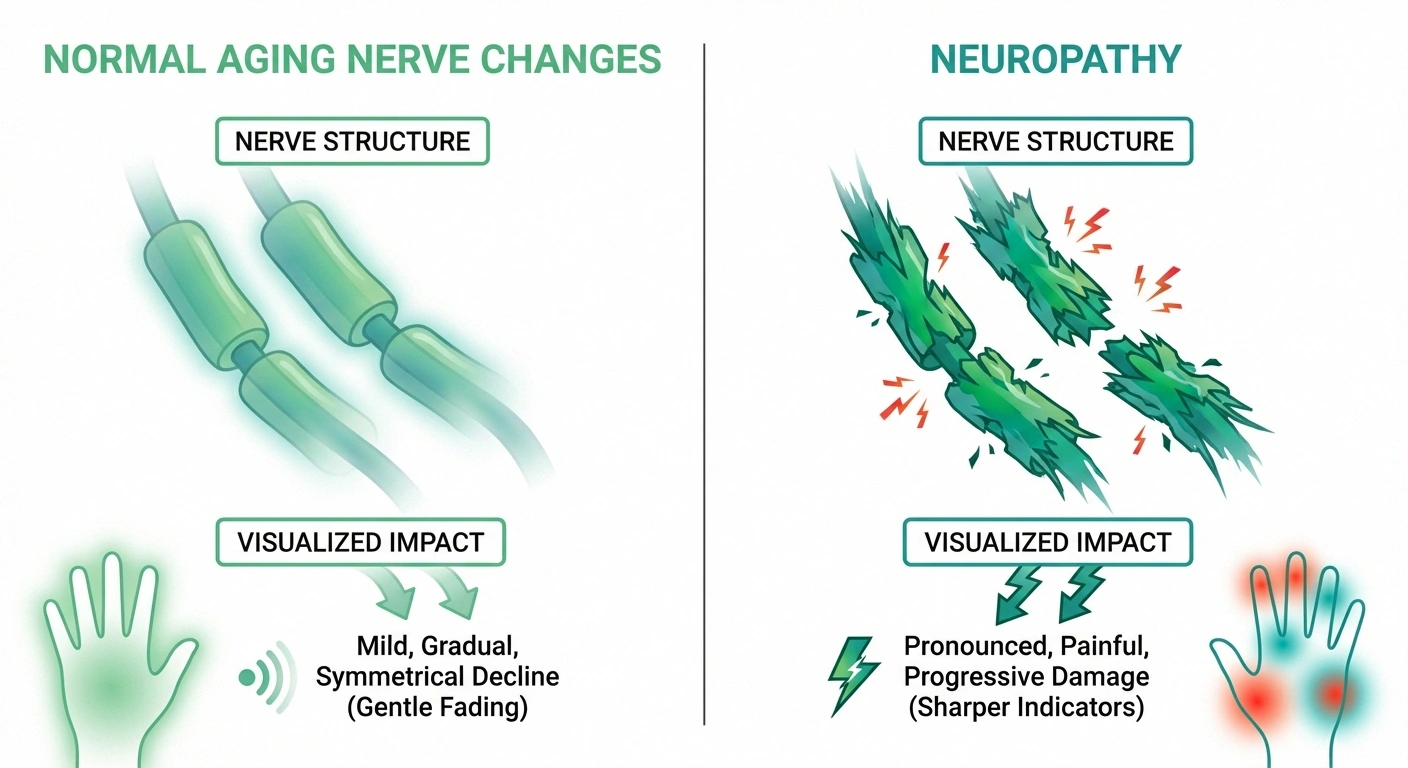
Normal aging changes are typically mild, symmetrical (affecting both sides equally), and don't significantly impact your daily activities. You might notice slightly reduced sensitivity in your feet or slower reflexes, but you can still walk confidently and perform daily tasks without difficulty.
Neuropathy, on the other hand, tends to be more pronounced. The numbness is deeper. The tingling is persistent. You may experience burning pain, especially at night — a phenomenon you can learn more about in our article on why neuropathy gets worse at night. You might start dropping things, tripping over your own feet, or finding it hard to button a shirt.
A retrospective study of 785 elderly patients with neuropathy found that 93.7% had axonal neuropathies, with diabetes being the leading cause (18.8%), followed by immune disorders (7.9%) and toxic causes (7.4%). Notably, 35.4% of cases were classified as idiopathic — meaning no identifiable cause was found.
Why Neuropathy Becomes More Common After 60
It's not just that nerves naturally decline with age — it's that the conditions most likely to cause neuropathy also become more common as we get older. Think of it as a double hit: your nerves become more fragile at the same time they're being exposed to more potential sources of damage.



Diabetes and Pre-Diabetes
More than 25% of Americans over 65 have diabetes, and many more have pre-diabetes without knowing it. High blood sugar levels damage the small blood vessels that supply nerves, which is why diabetic neuropathy is the single most common cause of peripheral neuropathy in the elderly.
Vitamin Deficiencies
As we age, our ability to absorb certain vitamins decreases. Vitamin B12 absorption drops significantly after 60, partly because the stomach produces less acid needed for B12 absorption. Medications like metformin (for diabetes) and proton pump inhibitors (for acid reflux) — both commonly used by older adults — further reduce B12 levels. B12 deficiency damages the myelin sheath protecting your nerves, leading to progressive neuropathy if untreated.
Medication Side Effects
Older adults typically take more medications, and several common ones can contribute to neuropathy. Statins, certain antibiotics, chemotherapy drugs, and some heart medications have all been linked to nerve damage. The more medications you take, the higher the risk — a problem doctors call polypharmacy.
Reduced Immune Function
Your immune system changes with age, becoming both less effective and sometimes more likely to attack your own body. Autoimmune neuropathies, including chronic inflammatory demyelinating polyneuropathy (CIDP), can appear for the first time in older adults. Post-herpetic neuralgia — nerve pain following shingles — is particularly common in older adults whose immune systems can no longer keep the dormant varicella-zoster virus in check.
Accumulated Wear and Inflammation
Research from UC San Francisco found that even “normal” levels of inflammation and glucose metabolism are associated with accelerated nerve decline in aging adults. Decades of low-grade inflammation take a cumulative toll on nerve health, contributing to what researchers call “inflammaging.”
The Hidden Danger: How Neuropathy Increases Fall Risk in Older Adults
If there's one consequence of neuropathy that keeps me up at night — both as someone living with it and as a support group leader — it's the fall risk. Peripheral neuropathy is a significant factor in disability among older adults, and falls are the primary mechanism.
Here's the cascade: neuropathy reduces sensation in your feet, which means your brain receives less information about the ground beneath you. Your proprioception — the body's ability to sense its position in space — deteriorates. At the same time, reflexes slow, muscle strength decreases, and balance becomes increasingly compromised.
A study published in the Journal of Gerontology found that older adults with peripheral neuropathy are 15 times more likely to report an injurious fall compared to those without it. For someone over 65, a fall can mean a hip fracture, head injury, or the beginning of a spiral toward loss of independence.
This is why neuropathy management in older adults isn't just about comfort — it's about safety and independence.
Getting the Right Diagnosis After 60
One of the biggest challenges in diagnosing neuropathy in older adults is separating it from normal aging. Many older adults — and even some doctors — dismiss early neuropathy symptoms as “just getting old.” This can delay diagnosis by months or years, allowing preventable damage to progress.

Fall Risk Alert
Older adults with peripheral neuropathy are up to 15 times more likely to experience an injurious fall. If you have neuropathy, talk to your doctor about a fall risk assessment and home safety evaluation.
If you're experiencing persistent numbness, tingling, burning, or weakness, ask your doctor about a proper neuropathy evaluation. This typically includes:
- Blood tests — checking for diabetes, vitamin deficiencies (especially B12 and folate), thyroid function, kidney function, and inflammatory markers
- Nerve conduction studies and EMG — measuring how quickly and effectively your nerves transmit signals
- Physical and neurological exam — testing reflexes, sensation, muscle strength, and balance
- Skin biopsy — may be recommended if small fiber neuropathy is suspected (standard nerve conduction studies can miss this type)
Important: Don't let anyone tell you that your symptoms are “just aging” without proper testing. Many causes of neuropathy in older adults — vitamin deficiencies, medication side effects, thyroid problems, even diabetes — are treatable or reversible when caught early.
Treatment Considerations Specific to Older Adults
Treating neuropathy in older adults requires a different approach than in younger patients. As the Mayo Clinic Proceedings noted in a comprehensive review, aging affects both pharmacokinetics (how your body processes medications) and pharmacodynamics (how medications affect your body), meaning standard dosing can be too aggressive for older patients.
Medication Adjustments
If your doctor prescribes neuropathy medications like gabapentin or pregabalin, expect to start at a lower dose with slower increases. Older adults are more sensitive to central nervous system side effects like dizziness, drowsiness, and confusion — which can increase fall risk. Duloxetine may also be considered, but requires careful monitoring for blood pressure changes and drug interactions.
Key principle: “start low, go slow.” Any new medication should be introduced at the lowest effective dose and increased gradually while monitoring for side effects.
Topical Treatments
For older adults concerned about systemic medication side effects, topical options can be particularly appealing. Capsaicin cream and lidocaine patches work locally without significant systemic absorption, making them safer for people taking multiple medications. Topical neuropathy creams are often a good first-line option.
Key Takeaway
Don't dismiss persistent numbness, pain, or weakness as “just getting old.” Many causes of neuropathy in older adults — vitamin deficiencies, medication side effects, thyroid problems, diabetes — are treatable or even reversible when caught early. Ask your doctor for a proper neuropathy evaluation.
Supplement Support
Given the high prevalence of vitamin deficiencies in older adults, supplementation may play a particularly important role. Key supplements to discuss with your doctor include:
- Vitamin B12 — especially important if you take metformin or proton pump inhibitors; injections may be more effective than oral supplements for those with absorption issues
- Alpha-lipoic acid — research suggests 600mg daily may help reduce neuropathy symptoms, with particular evidence in diabetic neuropathy
- Magnesium — supports nerve function and is commonly deficient in older adults
- Acetyl-L-carnitine — may support nerve fiber regeneration, though evidence is still emerging
Lifestyle Strategies That Make a Real Difference
Medications and supplements are only part of the equation. Some of the most effective strategies for managing neuropathy in older adults are lifestyle-based — and many of them help with overall healthy aging at the same time.

Stay Moving (Safely)
Regular physical activity improves circulation, supports nerve health, and helps maintain the muscle strength needed for balance. The key is choosing activities appropriate for your abilities:
- Chair exercises and gentle strength training — build muscle without fall risk
- Water therapy — the buoyancy supports your body while reducing joint stress
- Gentle yoga — improves balance, flexibility, and proprioception
- Walking — even 15-20 minutes daily can improve circulation and nerve function
Prioritize Foot Care
When you can't fully feel your feet, daily inspection becomes essential. Check for cuts, blisters, or sores you might not feel. Wear properly fitted shoes with good support. Keep toenails trimmed. A comprehensive foot care routine is one of the most important things you can do to prevent serious complications.
Eat for Nerve Health
A neuropathy-supportive diet rich in B vitamins, antioxidants, and omega-3 fatty acids supports nerve health from the inside out. Focus on leafy greens, fatty fish, eggs, nuts, and whole grains. Limit sugar and processed foods, which contribute to inflammation and blood sugar spikes.
Fall-Proof Your Home
Since neuropathy increases fall risk, making your home safer is a proactive investment in your independence:
- Remove loose rugs and clutter from walkways
- Install grab bars in bathrooms
- Improve lighting, especially in hallways and stairways
- Use non-slip mats in the bathroom and kitchen
- Consider a shower chair if balance is an issue
- Keep frequently used items within easy reach
When to Sound the Alarm: Red Flags That Need Immediate Attention
While neuropathy often progresses slowly, certain symptoms in older adults warrant prompt medical attention:
- Sudden onset of severe numbness or weakness — could indicate stroke or acute nerve compression
- Rapidly worsening symptoms over days to weeks — may suggest Guillain-Barré syndrome or another acute inflammatory process
- Symptoms that are markedly worse on one side — asymmetric neuropathy has a different set of causes that need investigation
- New difficulty with bladder or bowel control — may indicate autonomic neuropathy progression
- Foot wounds that won't heal — a medical emergency for anyone with neuropathy and reduced circulation
Frequently Asked Questions
Is neuropathy a normal part of aging?
Some decline in nerve function is a normal part of aging, including slightly reduced sensation and slower reflexes. However, actual neuropathy — with persistent numbness, pain, or weakness that affects daily life — is not normal and should be evaluated by a healthcare provider. Many causes of neuropathy in older adults are treatable when caught early.
🚨 See Your Doctor Promptly If You Experience:
Sudden onset of severe numbness or weakness (could indicate stroke)
Rapidly worsening symptoms over days to weeks
Symptoms markedly worse on one side of your body
New difficulty with bladder or bowel control
Foot wounds that won't heal — a medical emergency
What percentage of older adults have peripheral neuropathy?
Studies suggest that peripheral neuropathy affects approximately 5-7% of adults over 45, but the rate rises significantly with age. Some research estimates that up to 8% of adults over 55 and up to 20% of adults over 80 have some form of peripheral neuropathy, though many cases go undiagnosed.
Can age-related neuropathy be reversed?
It depends on the cause. Neuropathy caused by vitamin deficiencies, medication side effects, or poorly controlled blood sugar may improve significantly or even resolve when the underlying cause is addressed. However, nerve regeneration is slower in older adults, so recovery typically takes longer. Early intervention gives the best chance of improvement.
Should I stop taking a medication if I think it's causing neuropathy?
Never stop a prescribed medication without talking to your doctor first. Some medications that can cause neuropathy are also treating serious conditions. Your doctor can evaluate whether the medication is likely causing your symptoms and may be able to adjust the dose, switch to an alternative, or help you weigh the risks and benefits.
What type of doctor should I see for neuropathy?
Your primary care doctor is a good starting point. They can order initial blood tests and may refer you to a neurologist for nerve conduction studies and more specialized evaluation. Some older adults also benefit from seeing a geriatrician — a doctor who specializes in the health needs of older adults — especially if multiple health conditions are involved.
Does neuropathy always get worse with age?
Not necessarily. While untreated neuropathy often progresses, many people are able to slow or stabilize their symptoms through proper management — addressing underlying causes, medication management, lifestyle changes, and consistent self-care. The key is not ignoring symptoms and working with your healthcare team to create a management plan.
Moving Forward: You're Not “Just Getting Old”
If there's one message I want every person over 60 to hear, it's this: don't dismiss your symptoms as “just aging.” Yes, your nerves change as you get older. But persistent numbness, pain, and weakness deserve investigation — not resignation.
I've watched people in my support group transform their quality of life simply by getting a proper diagnosis and addressing a vitamin deficiency or medication issue they didn't know about. I've seen 75-year-olds improve their balance and reduce their pain through consistent exercise and dietary changes.
Aging doesn't have to mean suffering. It means paying more attention, being more proactive, and giving your nerves the support they need to carry you through the decades ahead. Talk to your doctor, get tested, and take those first steps toward protecting your nerve health.
Have questions about neuropathy and aging? Explore our guide to the stages of neuropathy for a deeper understanding of how this condition progresses, or check out our supplement guide for evidence-informed options that may support nerve health.


