
Browse all our types and causes of neuropathy guides for more articles like this one.
When my doctor first put me on a statin years ago, I didn't think twice about it. Millions of people take these cholesterol-lowering drugs every day, and the heart benefits are well-documented. But about a year in, I started noticing a persistent tingling in my feet — something I couldn't quite explain. It took several doctor visits before anyone even considered that my medication might be playing a role.
If you're taking a statin and experiencing new or worsening nerve symptoms, you're not alone. The relationship between statins and peripheral neuropathy has been a topic of medical debate for over two decades, and understanding the facts can help you have a more productive conversation with your healthcare provider.
What Are Statins and Why Are They So Widely Prescribed?
Statins — also known as HMG-CoA reductase inhibitors — are a class of drugs that lower cholesterol by blocking an enzyme your liver uses to produce it. Common statins include atorvastatin (Lipitor), rosuvastatin (Crestor), simvastatin (Zocor), and pravastatin (Pravachol). They're among the most widely prescribed medications in the world, with tens of millions of Americans taking them to reduce their risk of heart attack and stroke.
The cardiovascular benefits of statins are well-established and significant. For many people, particularly those with a history of heart disease or high cardiovascular risk, statins are genuinely life-saving medications. But like all drugs, they come with potential side effects — and peripheral neuropathy is one that doesn't always get the attention it deserves.
higher risk of neuropathy in long-term statin users vs. non-users (Danish population study)
The Evidence: Can Statins Actually Cause Neuropathy?
The connection between statins and peripheral neuropathy has been studied extensively, and the evidence is nuanced. One of the most cited studies came from a Danish research team, published in the journal Neurology in 2002. The American Academy of Neurology reported that people taking statins were up to 14 times more likely to develop peripheral neuropathy with no other known cause compared to non-users. The smoking compounds medication-related nerve risks increased with longer duration of use and higher doses.
However, more recent research has complicated this picture. A 2019 study published in Neurology found that statins did not significantly increase the risk of polyneuropathy when accounting for confounding factors like diabetes. And a 2022 narrative review in Clinical Therapeutics highlighted the paradox that while LDL cholesterol itself may impair nerve transmission, the drugs that lower it have also been associated with neuropathy reports.
What we can say with reasonable confidence is this: statin-associated neuropathy appears to be a real but relatively uncommon phenomenon. It likely affects a small percentage of statin users, but for those individuals, the impact on quality of life can be significant.
How Statins May Damage Peripheral Nerves
Several biological mechanisms have been proposed to explain how statins might contribute to nerve damage. Understanding these pathways may help you and your doctor evaluate whether your symptoms could be medication-related.
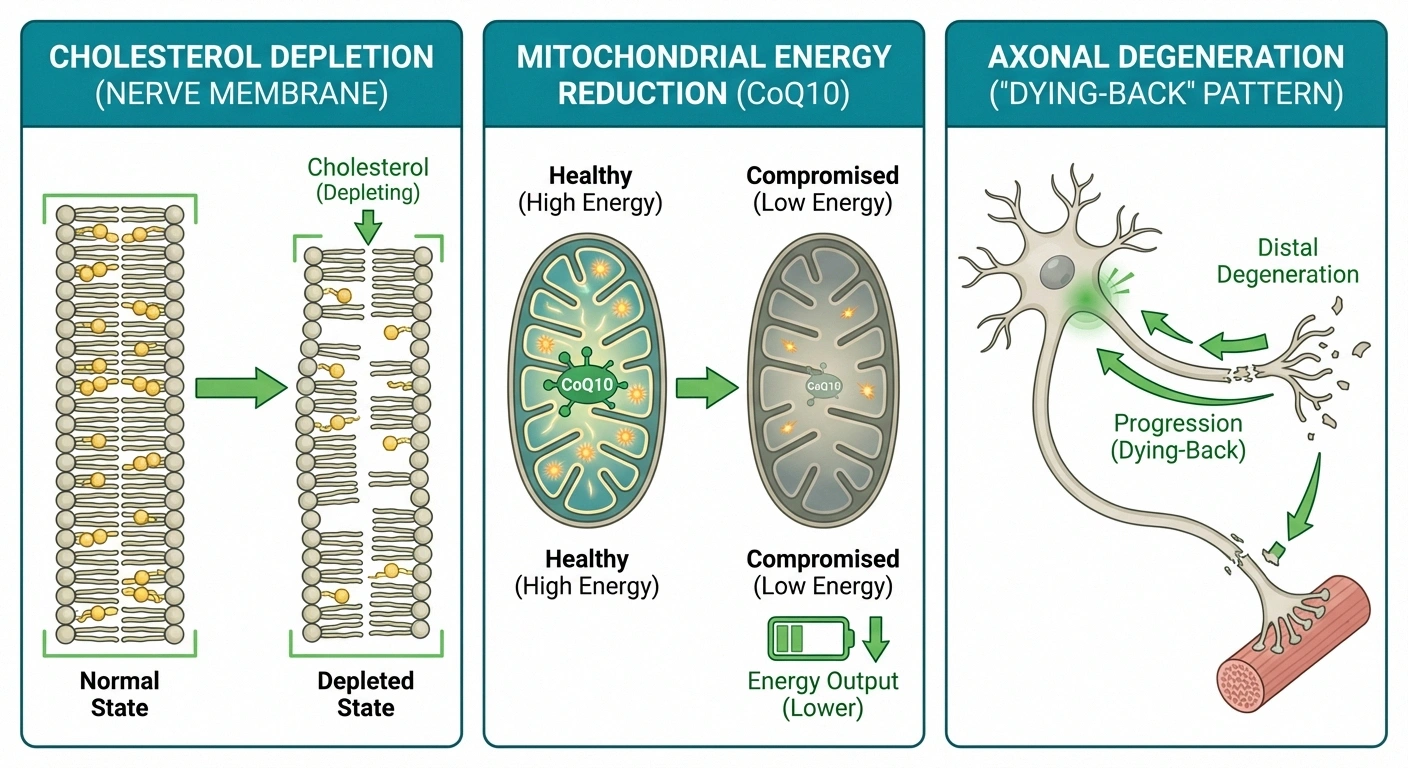
Cholesterol and Nerve Cell Membranes
Cholesterol is a critical component of cell membranes, including the membranes of nerve cells. The myelin sheath — the protective coating around nerves that allows electrical signals to travel quickly — is particularly rich in cholesterol. By aggressively lowering cholesterol production, statins may inadvertently compromise the integrity of nerve cell membranes and myelin, potentially leading to nerve dysfunction over time.
Coenzyme Q10 Depletion
Statins block the same biochemical pathway that produces coenzyme Q10 (CoQ10), also known as ubiquinone. CoQ10 plays a vital role in mitochondrial energy production — the process that powers every cell in your body, including nerve cells. When CoQ10 levels drop, neurons may not have the energy they need to function properly, potentially contributing to neuropathic symptoms.
Axonal Degeneration
Research suggests that statin-associated neuropathy typically involves axonal degeneration — damage to the long, thread-like extensions of nerve cells that carry signals. This pattern, sometimes called “dying-back” neuropathy, means the longest nerves are affected first, which is why symptoms usually begin in the feet before potentially progressing to the hands. Both large and small nerve fibers may be affected.
Symptoms of Statin-Induced Neuropathy
The symptoms of statin-related neuropathy are similar to those of peripheral neuropathy from other causes, which is part of what makes it challenging to diagnose. Common symptoms include:
- Numbness or tingling in the feet, legs, hands, or arms — often starting in the toes
- Burning or prickling sensations, particularly at night
- Increased sensitivity to touch (even bedsheets may feel painful)
- Muscle weakness, especially in the lower legs
- Loss of balance or coordination
- Sharp, stabbing, or electric-shock-like pains
One distinguishing feature of statin-induced neuropathy is the timeline. Symptoms typically develop gradually, often after months or even years of statin use. The average time to symptom onset in the Danish study was approximately 2.8 years. This delayed onset is one reason the connection between statins and neuropathy is sometimes missed — by the time symptoms appear, you and your doctor may not immediately think to question a medication you've been taking without problems for years.
Risk Factors: Who Is More Vulnerable?
Not everyone who takes a statin will develop neuropathy — in fact, most won't. But certain factors may increase your susceptibility:

- Duration of use: Longer statin use is associated with higher risk
- Higher doses: The risk appears to increase with dose
- Pre-existing diabetes: People with diabetic neuropathy may be more vulnerable to additional nerve insults from statins
- Age: Older adults may be more susceptible to medication side effects
- Other neuropathy risk factors: Vitamin deficiencies (especially B12), alcohol use, kidney disease, or other neurotoxic medications
- Genetic factors: Some people may have genetic variations that affect how they metabolize statins
A 2025 study published in Diabetes, Obesity and Metabolism specifically examined statin therapy and neuropathy in people with type 1 diabetes, highlighting the complex interplay between dyslipidemia, statin use, and nerve health in this population.
Diagnosis: Connecting the Dots
Diagnosing statin-induced neuropathy can be tricky because there's no single test that definitively proves a medication caused nerve damage. Instead, the diagnosis is typically made through a process of elimination. Your doctor may:
- Review your medication timeline — correlating when you started statins with when symptoms began
- Order nerve conduction studies and EMG — to confirm the presence and pattern of nerve damage ()
- Test for other causes — blood glucose, B12 levels, thyroid function, kidney function, and other common neuropathy culprits
- Consider a medication trial — temporarily stopping or switching the statin to see if symptoms improve
If your symptoms improve after discontinuing the statin and no other cause is found, statin-induced neuropathy becomes the most likely diagnosis. Research suggests that symptoms often begin to resolve within weeks to months of stopping the medication, though recovery isn't always complete, particularly if the drug was continued for a long time after symptoms began.
Important Warning
Never stop taking a statin on your own. Statins provide genuine cardiovascular protection, and suddenly discontinuing them could increase your risk of a heart event. Always talk to your doctor before making any changes to your medication.
What to Do If You Suspect Statin-Related Neuropathy
If you're taking a statin and experiencing symptoms of neuropathy, the most important step is to talk to your doctor — but please don't stop your medication on your own. Statins provide genuine cardiovascular protection, and suddenly discontinuing them could put you at risk for a heart event.
Here's a practical approach to the conversation with your healthcare provider:
- Document your symptoms: Keep a log of what you're experiencing, when it started, and how it has progressed
- Bring your full medication list: Include all prescription drugs, over-the-counter medications, and supplements
- Ask about alternatives: If statin-induced neuropathy is suspected, your doctor may try switching to a different statin (some may be better tolerated than others) or to a non-statin cholesterol-lowering medication
- Discuss a supervised trial: Your doctor may suggest a temporary discontinuation to see if symptoms improve, with careful monitoring of your cholesterol and cardiovascular risk
- Request appropriate testing: Nerve conduction studies, blood work to rule out other causes, and possibly a referral to a neurologist
Treatment and Recovery
The primary treatment for statin-induced neuropathy is discontinuing or changing the offending medication, under your doctor's guidance. Beyond that, several strategies may help manage symptoms and support nerve recovery:
CoQ10 Supplementation
Since statins deplete CoQ10, some healthcare providers recommend supplementing with CoQ10 (typically 100-200 mg daily). While the evidence specifically for neuropathy improvement is limited, CoQ10 supplementation is generally well-tolerated and may help address one of the underlying mechanisms of statin side effects. Talk to your doctor about whether this makes sense for you.
Symptom Management
While waiting for nerve recovery, your doctor may recommend medications like gabapentin or pregabalin to manage neuropathic pain. Topical creams containing capsaicin or lidocaine may also provide localized relief.
Nutritional Support
Ensuring adequate levels of B vitamins (especially B12), magnesium, and ALA and neuropathy research may support nerve health during recovery. A nerve-friendly diet rich in antioxidants and anti-inflammatory foods can also be beneficial.
Physical Activity
Gentle, regular exercise improves circulation to the extremities and may support nerve regeneration. Exercises designed for neuropathy patients can help maintain mobility and strength while you recover.
The Bigger Picture: Balancing Heart Health and Nerve Health
This is where things get complicated, and it's worth being honest about it. Statins save lives — they significantly reduce the risk of heart attacks and strokes in people with cardiovascular risk factors. The decision to take or stop a statin should never be made lightly.
At the same time, the quality-of-life impact of neuropathy is real. Living with constant pain, numbness, or balance problems takes a genuine toll. The goal isn't to demonize statins — it's to ensure that you and your doctor are making fully informed decisions about your care.
For some people, the answer may be trying a different statin, adjusting the dose, or switching to a non-statin cholesterol medication. For others, the cardiovascular benefits may still outweigh the neuropathy risk, and the focus shifts to managing nerve symptoms alongside continued statin therapy. There's no one-size-fits-all answer — it depends on your individual health profile, risk factors, and values.
Can the Damage Be Reversed?
The encouraging news is that statin-induced neuropathy is often at least partially reversible. Research indicates that symptoms frequently improve within weeks to months after discontinuing the statin. However, several factors influence recovery:

- How long you took the statin after symptoms began: Earlier recognition generally means better outcomes
- Severity of nerve damage: Mild cases tend to recover more fully than severe ones
- Other contributing factors: If you also have diabetes or other neuropathy risk factors, recovery may be more complex
- Age: Younger patients tend to recover nerve function more readily
This is why recognizing the potential connection early matters. If you're experiencing neuropathy symptoms and taking a statin, bringing this up with your doctor sooner rather than later gives you the best chance of a meaningful recovery. Learn more about the potential for neuropathy reversal in our dedicated guide.
Other Medications That Can Cause Neuropathy
Statins aren't the only class of medication linked to peripheral neuropathy. If you're experiencing nerve symptoms and take multiple medications, it's worth reviewing all of them with your doctor. Medications that can cause neuropathy include certain chemotherapy drugs, antibiotics (like metronidazole and fluoroquinolones), heart medications (amiodarone), and even some anti-seizure drugs.
Frequently Asked Questions
How common is neuropathy from statins?
Statin-induced neuropathy is considered relatively uncommon. While one Danish study found that statin users were 4-14 times more likely to develop neuropathy than non-users, the absolute risk remains low. Most people take statins without developing nerve problems. However, given that millions of people take these drugs, even a small percentage translates to a significant number of affected individuals.
How long does it take for statin neuropathy to develop?
Statin-associated neuropathy typically develops gradually over months to years of use. In the major Danish study, the average duration of statin use before neuropathy diagnosis was approximately 2.8 years. Symptoms tend to progress slowly, which can make the connection to the medication difficult to recognize.
Will my neuropathy go away if I stop taking statins?
Many people experience improvement in neuropathy symptoms within weeks to months of discontinuing statin therapy. However, recovery varies from person to person. Some individuals experience complete resolution, while others may have residual symptoms, particularly if the drug was continued for an extended period after symptoms first appeared. Never stop a statin without consulting your doctor first.
Are some statins more likely to cause neuropathy than others?
The research hasn't definitively identified one statin as more neurotoxic than others, though case reports exist for all commonly prescribed statins. Higher potency statins and higher doses may carry a somewhat greater risk. If you develop neuropathy symptoms on one statin, your doctor may try switching to a different one at a lower dose to see if your symptoms improve.
Should I stop taking my statin if I have neuropathy?
Do not stop taking your statin without talking to your doctor. Statins provide important cardiovascular protection, and stopping them abruptly can increase your risk of heart events. Instead, discuss your symptoms with your healthcare provider so they can weigh the benefits and risks and potentially adjust your treatment plan.
Can CoQ10 supplements prevent statin-induced neuropathy?
There is some theoretical basis for CoQ10 supplementation since statins deplete this important compound. Some doctors recommend CoQ10 supplementation for statin users, particularly those experiencing side effects. However, there is limited clinical evidence specifically proving that CoQ10 prevents statin-induced neuropathy. It may help with overall mitochondrial function and energy production in nerve cells.
❌ If Unrecognized
Continuing the medication while neuropathy progresses can lead to more extensive nerve damage that may be harder to reverse. Symptoms gradually worsen over months and years.
✓ If Caught Early
When identified and addressed promptly — by switching medications, adjusting doses, or supplementing with CoQ10 — many people see meaningful improvement within weeks to months.
Key Takeaways
Statin-induced neuropathy is a real but relatively uncommon side effect that deserves more awareness among both patients and healthcare providers. The key points to remember:
- Statins may cause neuropathy through cholesterol depletion in nerve membranes, CoQ10 reduction, and other mechanisms
- Symptoms typically develop gradually over months to years
- Risk increases with higher doses and longer duration of use
- The condition is often at least partially reversible when caught early
- Never stop statins on your own — always work with your doctor
- The benefits of statins for cardiovascular health are significant and well-proven
If you're living with both neuropathy and the need for cholesterol management, you're navigating a genuinely complex situation. Be your own advocate, keep track of your symptoms, and work closely with your healthcare team to find the approach that protects both your heart and your nerves. You deserve a treatment plan that considers all of you — not just your cholesterol numbers.


