
Neuropathy and Diabetes Prevention: Protecting Your Nerves Early
Here's a number that should get your attention: up to 50% of people with diabetes will develop neuropathy during their lifetime. That's according to both the American Diabetes Association and extensive clinical research spanning decades. But here's what often gets lost in that statistic — a significant amount of that nerve damage is preventable, or at least delayable, with the right actions taken early enough.
If you have diabetes or prediabetes, this guide is for you. Not as a scare tactic, but as a practical roadmap for protecting the peripheral nerves that control sensation in your feet and hands, keep your balance steady, and allow you to feel the world around you. Because once nerve damage progresses past a certain point, reversing it becomes far more difficult than preventing it was.
How Diabetes Damages Your Nerves
Understanding the “why” behind diabetic neuropathy helps explain why certain prevention strategies work. It's not just that high blood sugar is “bad for nerves” — the damage follows specific pathways that science has mapped in detail.
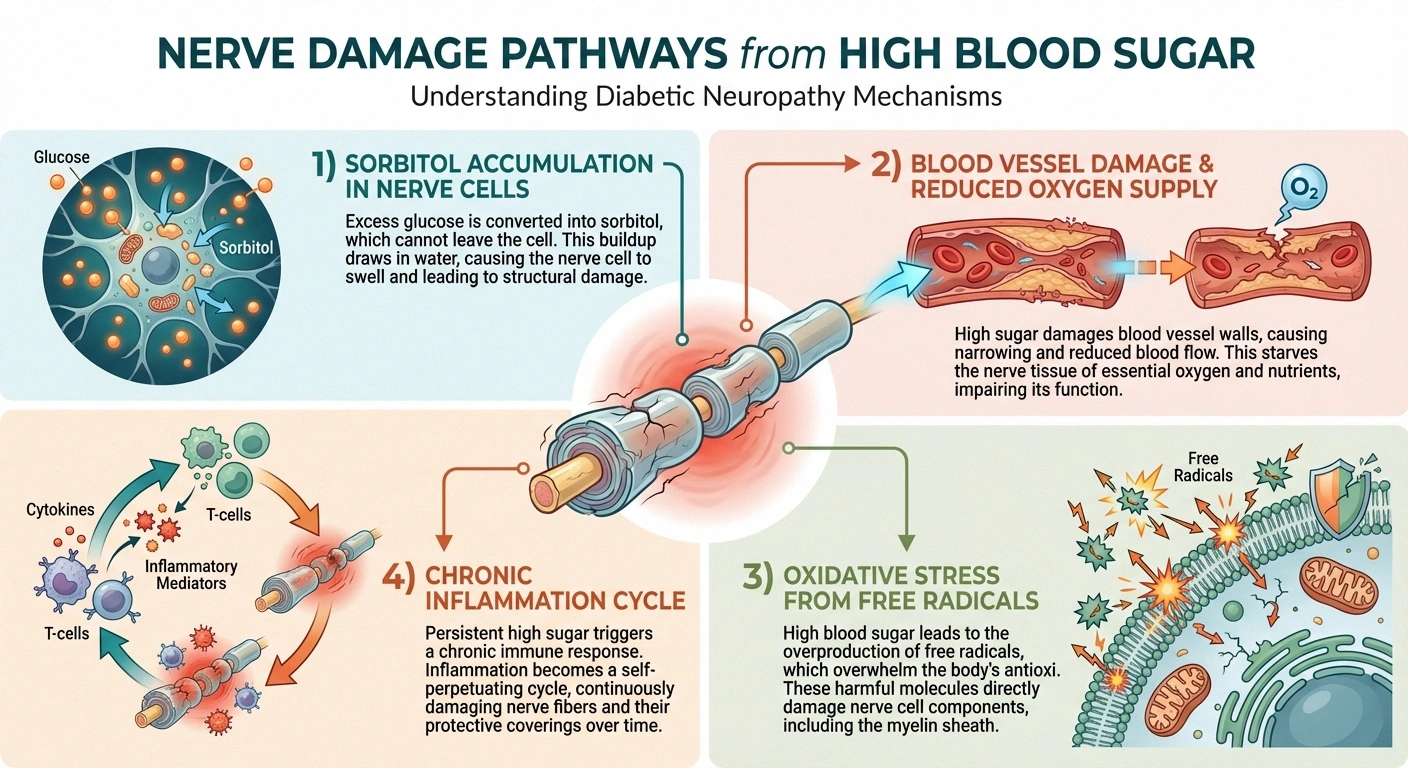
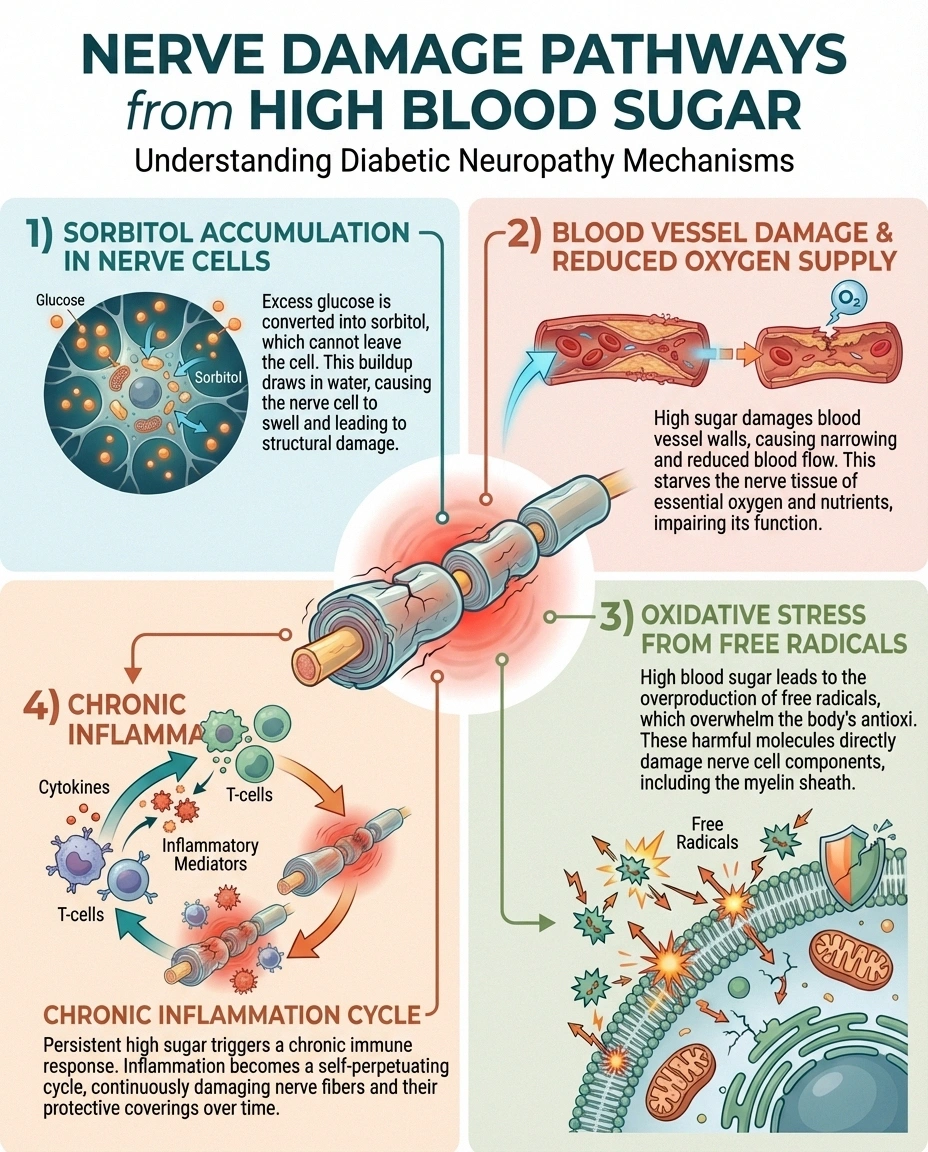
When blood glucose levels remain elevated over months or years, several destructive processes begin:
Direct nerve fiber damage. Excess glucose enters nerve cells and gets converted through a process called the polyol pathway, producing sorbitol. Sorbitol accumulates inside nerve cells, causing them to swell and disrupting their normal function. Over time, this leads to the breakdown of the myelin sheath — the protective coating around nerve fibers — and eventual nerve fiber death.
Blood vessel damage. High blood sugar also damages the tiny blood vessels (vasa nervorum) that supply oxygen and nutrients to your nerves. According to a comprehensive 2022 review in the journal Life, the severity of this microvascular damage has been directly linked to the severity of neuropathy in multiple studies. When nerves can't get enough blood, they starve — and starving nerves send abnormal signals (pain, burning, tingling) or stop sending signals altogether (numbness).
Oxidative stress. Elevated glucose triggers a cascade of biochemical pathways that produce excessive free radicals — unstable molecules that damage cells. This oxidative stress is particularly destructive to nerve tissue. It's one reason why antioxidants like alpha-lipoic acid have shown promise in some neuropathy studies.
Inflammation. Chronic hyperglycemia promotes systemic inflammation, which further damages both nerve fibers and the blood vessels supplying them. This creates a vicious cycle: inflammation damages nerves, damaged nerves trigger more inflammation.
The damage typically follows a “length-dependent” pattern — affecting the longest nerves first. That's why symptoms almost always start in the toes and feet and gradually work their way upward. The same process can eventually affect the fingers and hands in what doctors describe as a “stocking-and-glove” distribution.
The Window of Opportunity: Why Timing Matters
One of the most important things to understand about diabetic neuropathy prevention is that timing is everything. The landmark Diabetes Control and Complications Trial (DCCT) and its follow-up Epidemiology of Diabetes Interventions and Complications (EDIC) study tracked over 1,400 people with type 1 diabetes for more than 14 years. The findings were striking:
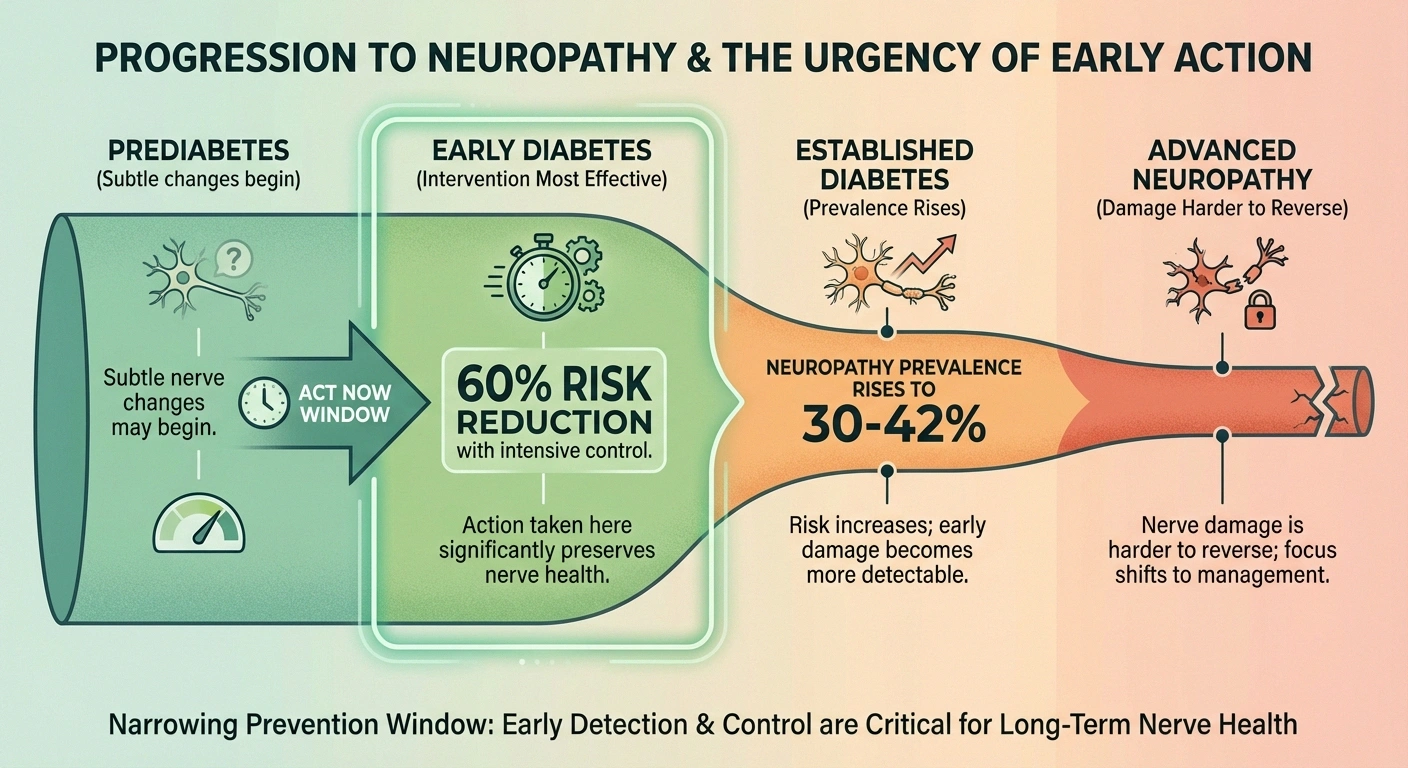
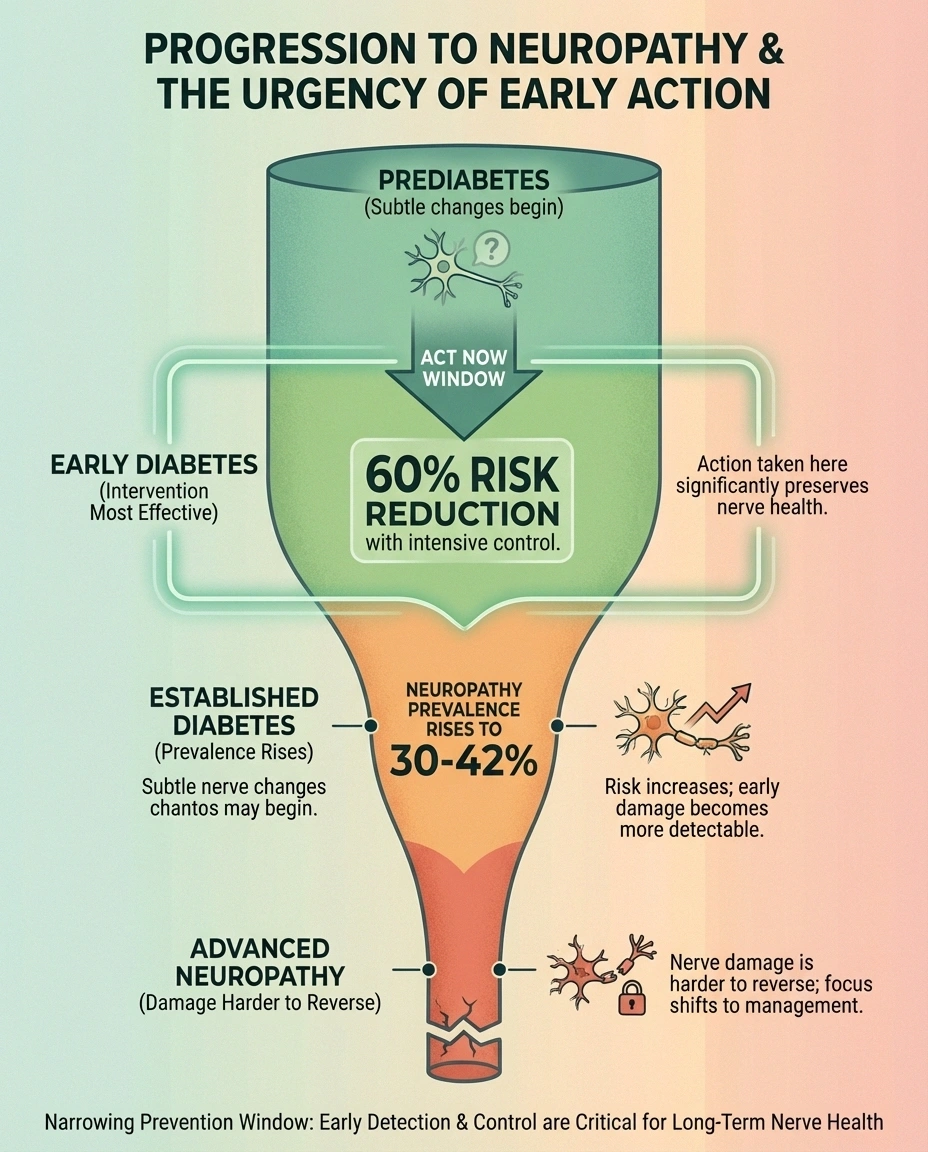
- At baseline, only 6% of participants had neuropathy
- After 14 years, that number had risen to 30%
- Intensive glycemic control reduced the risk of developing neuropathy by up to 60% in people with type 1 diabetes
For type 2 diabetes, the picture is more complex. The ACCORD trial found that 42% of its 10,201 participants with type 2 diabetes already had neuropathy at the start of the study. While intensive glycemic control showed more modest benefits for type 2 diabetes, as the American Academy of Family Physicians noted in a 2024 review, early glucose optimization still provides the greatest benefit.
The message is clear: the earlier you take action, the more nerve damage you may prevent. Waiting until numbness sets in means the window for prevention has already partially closed.
Blood Sugar Control: The Foundation of Prevention
Every clinical guideline on diabetic neuropathy prevention starts with the same recommendation: keep your blood glucose levels within your target range. This isn't a suggestion — it's the single most evidence-backed strategy for protecting your nerves.
Know Your Numbers
Two key measurements tell you how well your blood sugar is controlled:
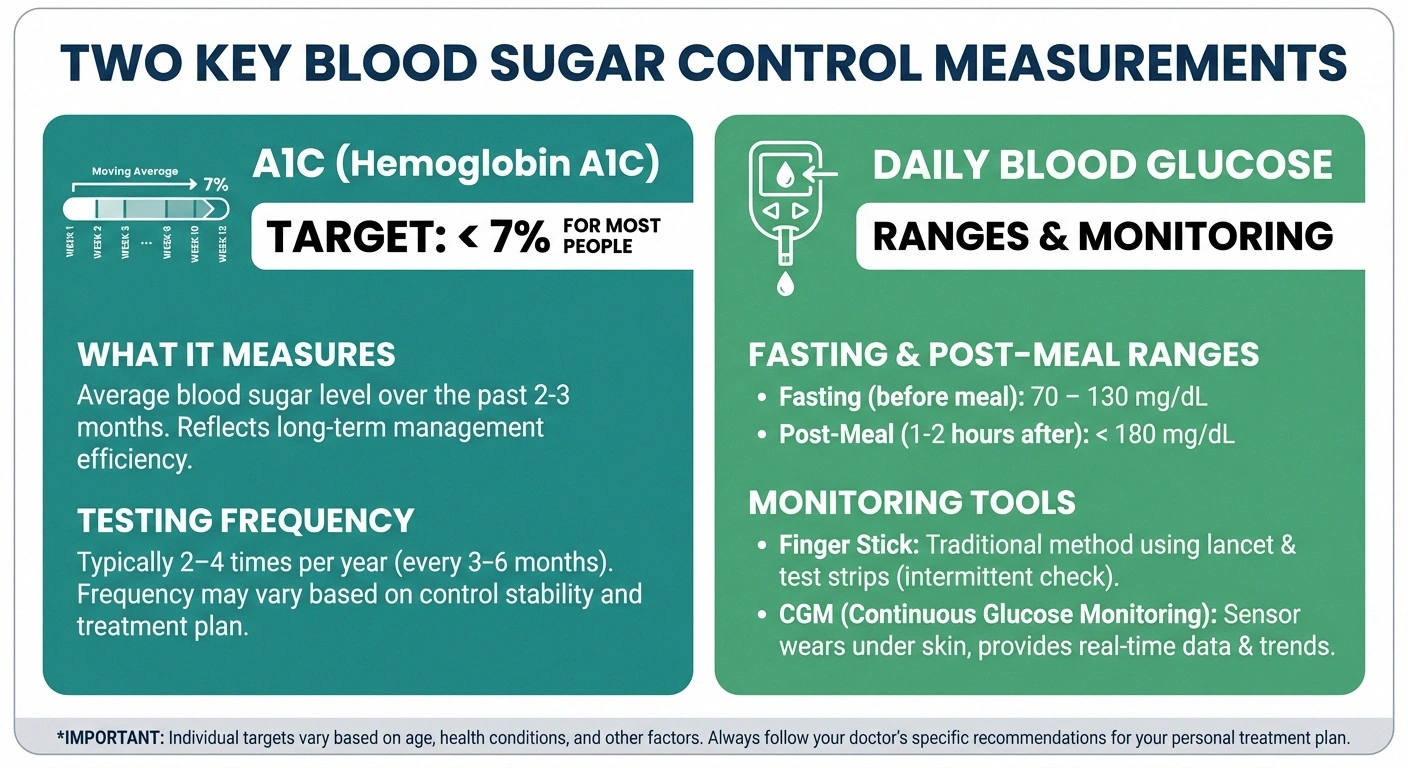


- A1C (hemoglobin A1C) — measures your average blood glucose over the past 2-3 months. For most people with diabetes, the target is below 7%, though your doctor may recommend a different goal based on your individual situation.
- Daily blood glucose monitoring — whether through finger sticks or a continuous glucose monitor (CGM), daily readings help you make real-time adjustments to diet, activity, and medication.
The American Diabetes Association recommends getting your A1C tested at least twice per year. If your treatment has changed or you're not meeting your targets, your doctor may test more frequently.
Beyond Blood Sugar: The Metabolic Package
While blood glucose gets the most attention, research increasingly shows that neuropathy risk is influenced by a broader set of metabolic factors. The 2024 AAFP review specifically called out several additional risk factors that physicians should address:
- Blood pressure — maintaining systolic blood pressure at 140 mmHg or lower has been shown to decrease the development of diabetic peripheral neuropathy
- Cholesterol and lipids — dyslipidemia is an independent risk factor for nerve damage
- Obesity — central obesity contributes to inflammation and metabolic dysfunction that worsen neuropathy risk
- Vitamin B12 levels — particularly important because metformin, one of the most common diabetes medications, can cause B12 deficiency over time. A B12 deficiency can either cause neuropathy or make diabetic neuropathy worse
Addressing all of these factors together — rather than focusing on blood sugar alone — provides the strongest protection for your nerves.
Lifestyle Changes That Protect Your Nerves
Medication plays a crucial role in diabetes management, but lifestyle modifications can be equally powerful for neuropathy prevention. These are changes you can start making today.
Exercise: Your Nerves' Best Friend
Regular physical activity benefits your nerves through multiple pathways simultaneously. Exercise improves insulin sensitivity (lowering blood sugar), enhances blood flow to peripheral nerves, reduces inflammation, and helps manage weight. Some research even suggests that exercise may promote nerve regeneration.

What type of exercise works best? The evidence supports a combination approach:
- Aerobic exercise — walking, swimming, cycling, or other moderate-intensity activities for at least 150 minutes per week. This is the most-studied form of exercise for neuropathy prevention.
- Resistance training — strength exercises 2-3 times per week help with blood sugar control and improve the muscle strength that neuropathy can undermine.
- Balance training — particularly important because neuropathy increases fall risk. Activities like tai chi or specific balance exercises can help maintain stability.
One important caveat: if you already have neuropathy or loss of sensation in your feet, certain exercises may need to be modified to avoid injury. Low-impact options like swimming and cycling are often safer than running or high-impact aerobics. Talk to your healthcare provider or a diabetes-certified exercise specialist about the safest approach for your specific situation.
Nutrition: Fuel for Nerve Health
What you eat affects your nerves both directly (through the nutrients you provide) and indirectly (through blood sugar control). A nerve-friendly diet focuses on:
- Consistent carbohydrate management — not eliminating carbs, but choosing complex carbohydrates and distributing them evenly throughout the day to avoid blood sugar spikes
- Anti-inflammatory foods — fruits, vegetables, fatty fish (salmon, mackerel, sardines), nuts, and olive oil. The Mediterranean dietary pattern has been associated with reduced inflammation and may support nerve health.
- Adequate B vitamins — particularly B12, B1 (thiamine), and B6. These are essential for nerve function and myelin maintenance. If you take metformin, ask your doctor about monitoring your B12 levels.
- Antioxidant-rich foods — berries, leafy greens, and colorful vegetables help combat the oxidative stress that damages nerve tissue
- Limiting alcohol — alcohol is directly toxic to peripheral nerves and also impairs blood sugar control. If you drink, keep it minimal.
Smoking Cessation
Smoking damages blood vessels throughout your body, including the tiny ones that supply your peripheral nerves. For someone with diabetes, smoking essentially doubles down on the vascular damage that leads to neuropathy. Quitting smoking is one of the most impactful single changes you can make for your nerve health — and your overall cardiovascular health.
Early Detection: Catching Neuropathy Before It Progresses
Prevention isn't just about stopping neuropathy from starting — it's also about catching early signs before significant damage accumulates. Early-stage neuropathy is far more responsive to intervention than advanced neuropathy.
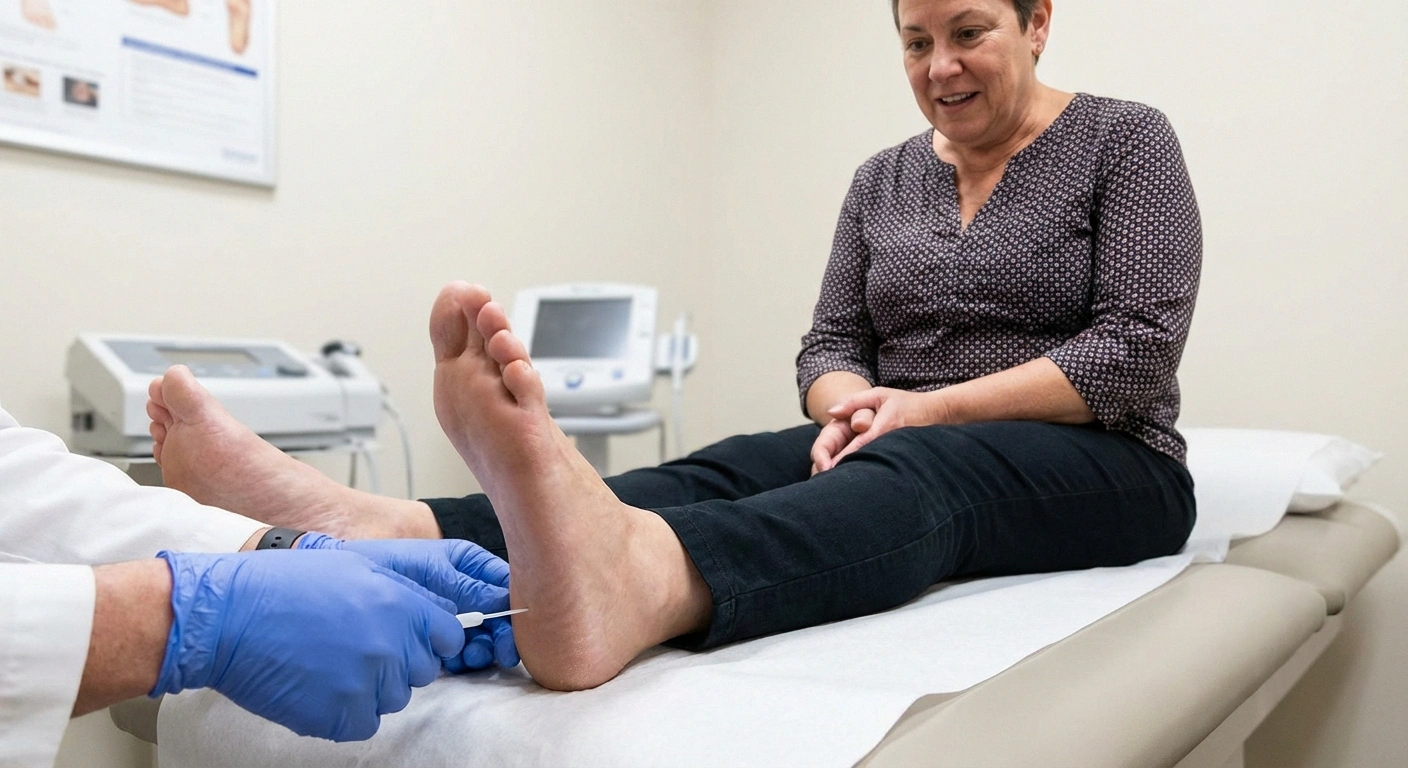
Annual Screening
The American Diabetes Association recommends that all people with diabetes be screened for peripheral neuropathy regularly:
- Type 1 diabetes — start screening 5 years after diagnosis, then annually
- Type 2 diabetes — start screening at diagnosis (since neuropathy may already be present), then annually
Screening typically involves a monofilament test (pressing a thin nylon fiber against the sole of your foot to check sensation), vibration testing, and an ankle reflex check. While monofilament testing has limitations in sensitivity, it's a practical starting point.
Know the Early Warning Signs
Don't wait for your annual screening to notice changes. Report any of the following symptoms to your doctor as soon as they appear:
☐ Numbness starting in toes that doesn't resolve
☐ Burning sensations in feet, especially at night
☐ Unusual sensitivity — pain from socks or sheets
☐ Loss of balance or coordination
☐ Muscle weakness in feet or ankles
☐ Cuts or sores you didn't feel happening
- Tingling or “pins and needles” in your feet or hands
- Numbness that starts in your toes and doesn't go away
- Burning sensations in your feet, especially at night
- Unusual sensitivity — your feet hurt when touched by socks or sheets
- Loss of balance or coordination
- Muscle weakness in your feet or ankles
- Cuts or sores on your feet that you didn't feel happen
These symptoms may seem minor at first, but they represent the beginning of a process that, left unchecked, can lead to serious complications including foot ulcers, infections, and in severe cases, amputation.
Foot Care: Your First Line of Defense
Daily foot care may sound mundane, but it's one of the most critical prevention strategies for anyone with diabetes. Here's why: as neuropathy develops, you gradually lose the ability to feel injuries on your feet. A small cut, blister, or pressure sore that a healthy person would immediately notice and treat can go undetected for days — long enough for a serious infection to develop.
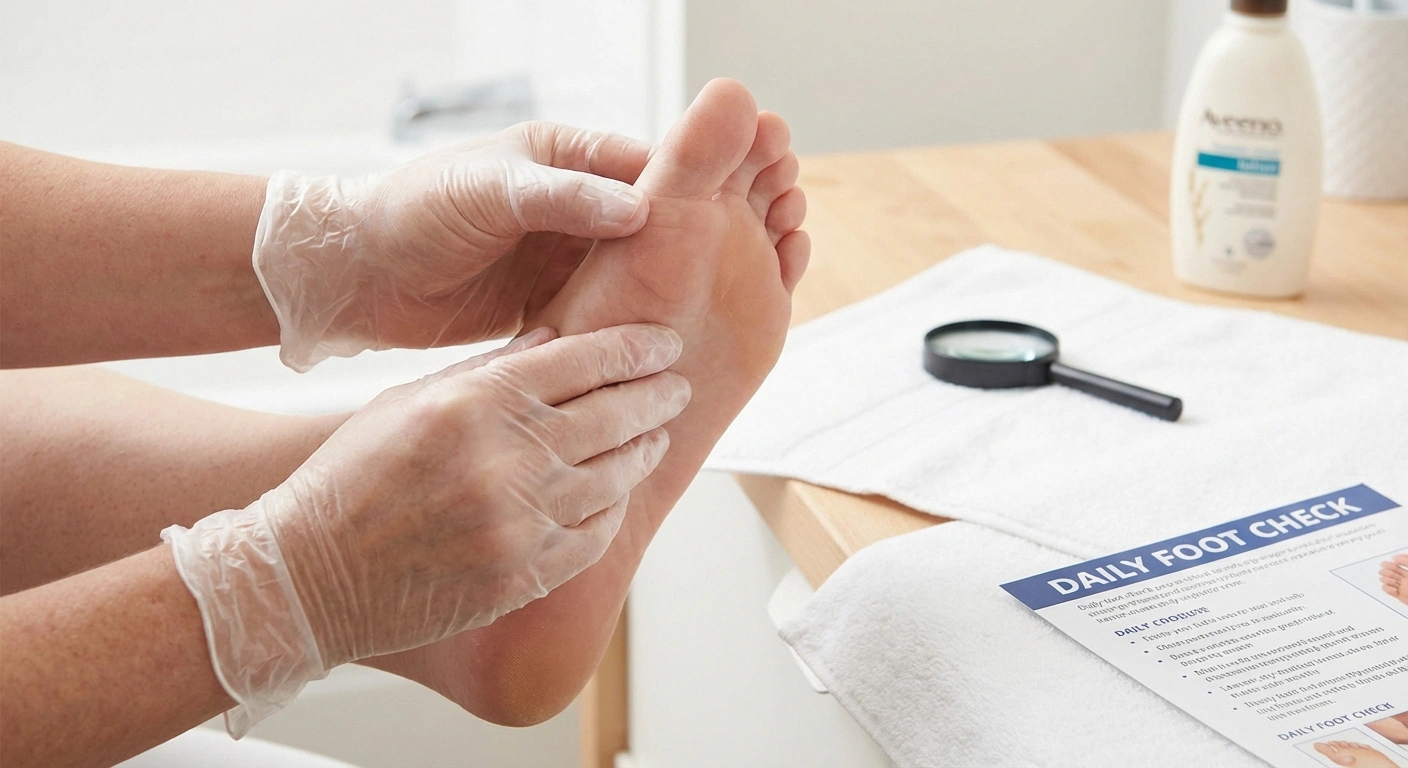
☑️ Wash: Warm water daily, dry thoroughly between toes
☑️ Moisturize: Lotion on tops and bottoms, NOT between toes
☑️ Trim: Cut nails straight across, file edges smooth
☑️ Protect: Wear shoes always — even indoors
☑️ Check shoes: Feel inside for objects before wearing
The ADA recommends these daily practices:
- Inspect your feet every day — use your eyes to check for cuts, blisters, red areas, swelling, or skin changes. Use a mirror to see the bottoms of your feet, or ask someone to help.
- Wash your feet daily in warm (not hot) water. Dry them thoroughly, especially between the toes.
- Moisturize to prevent cracking — apply lotion to the tops and bottoms of your feet, but not between the toes (moisture there can promote fungal infections).
- Trim toenails carefully — cut straight across and file the edges. If you can't see well or reach your feet, have a podiatrist do it.
- Wear proper footwear — never go barefoot, even indoors. Choose shoes that fit well and provide protection. Medicare may cover therapeutic shoes for people with diabetes-related foot problems.
- Check shoes before wearing — feel inside for small stones, rough seams, or other objects that could cause injury you won't feel.
Supplements and Emerging Therapies
Beyond the foundational strategies of blood sugar control, lifestyle modification, and foot care, some supplemental approaches show promise for neuropathy prevention — though the evidence varies:
Alpha-lipoic acid (ALA): This antioxidant has been the most-studied supplement for diabetic neuropathy. Several clinical trials have shown that ALA may reduce neuropathy symptoms, particularly at doses of 600mg daily. Some European guidelines include it as a treatment option. While the evidence is stronger for symptom management than prevention, its antioxidant properties may help protect nerves from oxidative damage.
B Vitamins and Other Emerging Options
B vitamin supplementation: If you have confirmed deficiencies — especially B12 — supplementation may protect nerves. However, supplementing without a deficiency has not been shown to prevent neuropathy, and the American Association of Neuromuscular and Electrodiagnostic Medicine specifically recommends against routine B vitamin supplementation for neuropathy when no deficiency exists.
Acetyl-L-carnitine: Some small studies suggest potential benefits for nerve regeneration, but larger studies are needed. The 2024 AAFP review listed it among treatments requiring further study.
Always discuss any supplements with your healthcare provider before starting them, as they can interact with diabetes medications and other treatments.
The Prediabetes Advantage
If you've been told you have prediabetes, you have an extraordinary opportunity. Nerve damage can actually begin during the prediabetes stage — before a formal diabetes diagnosis. But prediabetes is also the stage where lifestyle interventions are most powerful.
The landmark Diabetes Prevention Program study showed that intensive lifestyle changes (modest weight loss of 5-7% of body weight combined with 150 minutes of weekly exercise) reduced the progression from prediabetes to type 2 diabetes by 58% — more effective than metformin alone (31% reduction). Every year you prevent or delay diabetes is a year you protect your nerves from the damage that high blood sugar causes.
If you have prediabetes, this is your moment to act. The same lifestyle changes that may prevent diabetes also directly protect your nerves.
Building Your Prevention Plan
Preventing diabetic neuropathy isn't about any single heroic action — it's about consistent, sustained effort across multiple fronts. Here's a practical summary of what an effective prevention plan looks like:
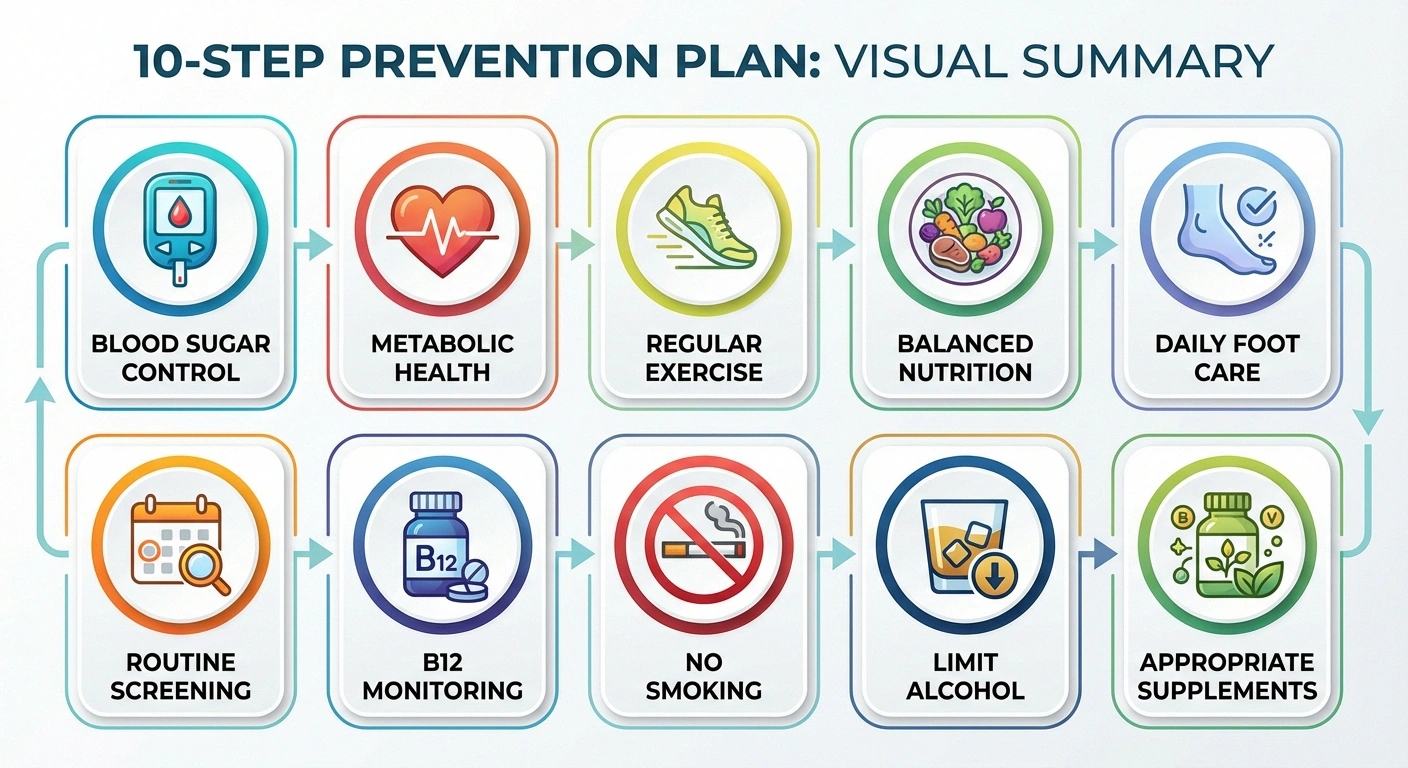
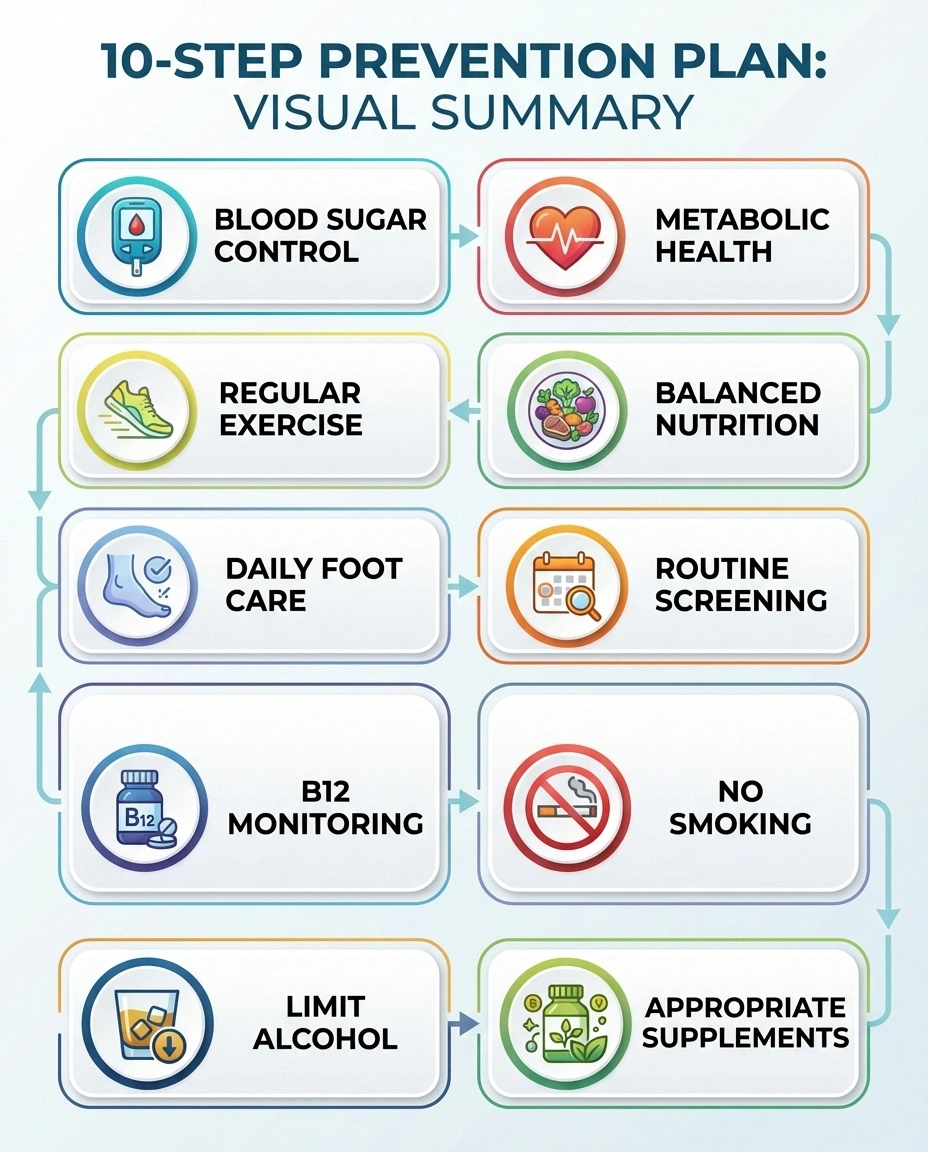
- Work with your healthcare team to establish and meet your blood sugar targets. Get your A1C tested regularly and use daily monitoring to make real-time adjustments.
- Address the full metabolic picture — blood pressure, cholesterol, and weight alongside blood sugar.
- Move your body regularly — aim for at least 150 minutes of moderate aerobic activity per week, plus resistance and balance training.
- Eat to support your nerves — focus on complex carbohydrates, anti-inflammatory foods, and adequate B vitamins.
- Inspect your feet daily and maintain proper foot hygiene and protection.
- Get screened annually for neuropathy, and report new symptoms immediately.
- If you take metformin, ask about regular B12 monitoring.
- Don't smoke. If you do, make quitting a priority.
- Limit alcohol consumption.
- Discuss supplement options like alpha-lipoic acid with your doctor, especially if you have early signs of neuropathy.
Frequently Asked Questions
Can diabetic neuropathy be reversed?
In some cases, early-stage diabetic neuropathy may improve or partially reverse with tight blood sugar control and lifestyle changes. However, advanced neuropathy with significant nerve fiber loss is generally not reversible. This is why prevention and early detection are so critical. The earlier you intervene, the better your chances of preserving nerve function.

At what blood sugar level does nerve damage start?
There is no single threshold. Nerve damage from diabetes is caused by prolonged exposure to elevated blood sugar rather than a specific number. However, research shows that the risk increases significantly with A1C levels above 7 percent. Even people with prediabetes and impaired glucose tolerance may begin experiencing subtle nerve changes before a formal diabetes diagnosis.
Does metformin cause neuropathy?
Metformin itself does not directly damage nerves, but long-term use can deplete vitamin B12 levels. B12 deficiency can cause a neuropathy that looks and feels identical to diabetic neuropathy. This means some people on metformin may develop worsening neuropathy symptoms not from their diabetes but from medication-induced B12 deficiency. Regular B12 monitoring and supplementation when needed can prevent this complication.
How quickly does diabetic neuropathy develop?
Diabetic neuropathy typically develops gradually over years, not weeks or months. In type 1 diabetes, it rarely appears before 5 years of disease duration. In type 2 diabetes, neuropathy may already be present at the time of diagnosis because blood sugar may have been elevated for years before diabetes was formally identified. The rate of progression varies widely depending on how well blood sugar and other metabolic factors are controlled.
Is walking good for diabetic neuropathy prevention?
Yes. Walking is one of the most accessible and evidence-supported forms of exercise for diabetes management and neuropathy prevention. Regular walking improves blood sugar control, enhances circulation to peripheral nerves, and helps manage weight. Aim for at least 30 minutes most days of the week. If you already have neuropathy in your feet, wear properly fitted shoes and inspect your feet after walking for any signs of injury you may not have felt.
What is the best vitamin for preventing diabetic neuropathy?
Vitamin B12 is the most clinically relevant vitamin for diabetic neuropathy prevention, particularly if you take metformin. Beyond B12, vitamins B1 (thiamine) and B6 also play roles in nerve health. However, medical guidelines recommend supplementing only when a deficiency is documented. Taking high doses of B vitamins without a deficiency has not been shown to prevent neuropathy and can actually cause nerve problems in some cases, particularly with excessive B6.
Take Action Today
Diabetic neuropathy may be common, but it is not inevitable. The research consistently shows that people who take active, early, and comprehensive steps to manage their diabetes and overall metabolic health significantly reduce their risk of developing nerve damage.
You don't need to overhaul your entire life overnight. Start with the one area where you know you're falling short — whether that's blood sugar monitoring, exercise, foot care, or that long-overdue conversation with your doctor about your B12 levels. Each step forward is a step toward protecting the nerves that let you feel the ground under your feet, the warmth of a loved one's hand, and the thousands of small sensations that make up a fully lived day.
Your nerves are counting on you. Start today.

