Neuropathy Prognosis: What to Expect Long-Term
When people ask about neuropathy prognosis, what they usually mean is not “what is the formal outlook?” They mean: Is this going to keep spreading? Will I still be walking the same way in five years? Can nerves actually heal? Am I heading toward disability?
The honest answer is that neuropathy has no single prognosis. It behaves more like a family of conditions than one disease. Some forms improve when you remove the cause early. Some mostly stabilize. Some progress slowly. And some become a major quality-of-life problem not because they are fatal, but because pain, balance loss, weakness, or foot injury gradually erode function. This guide breaks down what actually drives long-term outlook so you can judge your trajectory more realistically.
The Biggest Factor in Prognosis Is the Cause
This is the first principle: neuropathy prognosis follows the mechanism. If the underlying cause is still active, the nerve injury usually keeps getting fed. If the cause is removed or controlled, the outlook improves. That is why the best prognosis article has to point back to cause-finding, not just symptom management. See neuropathy diagnosis if your workup is still thin.
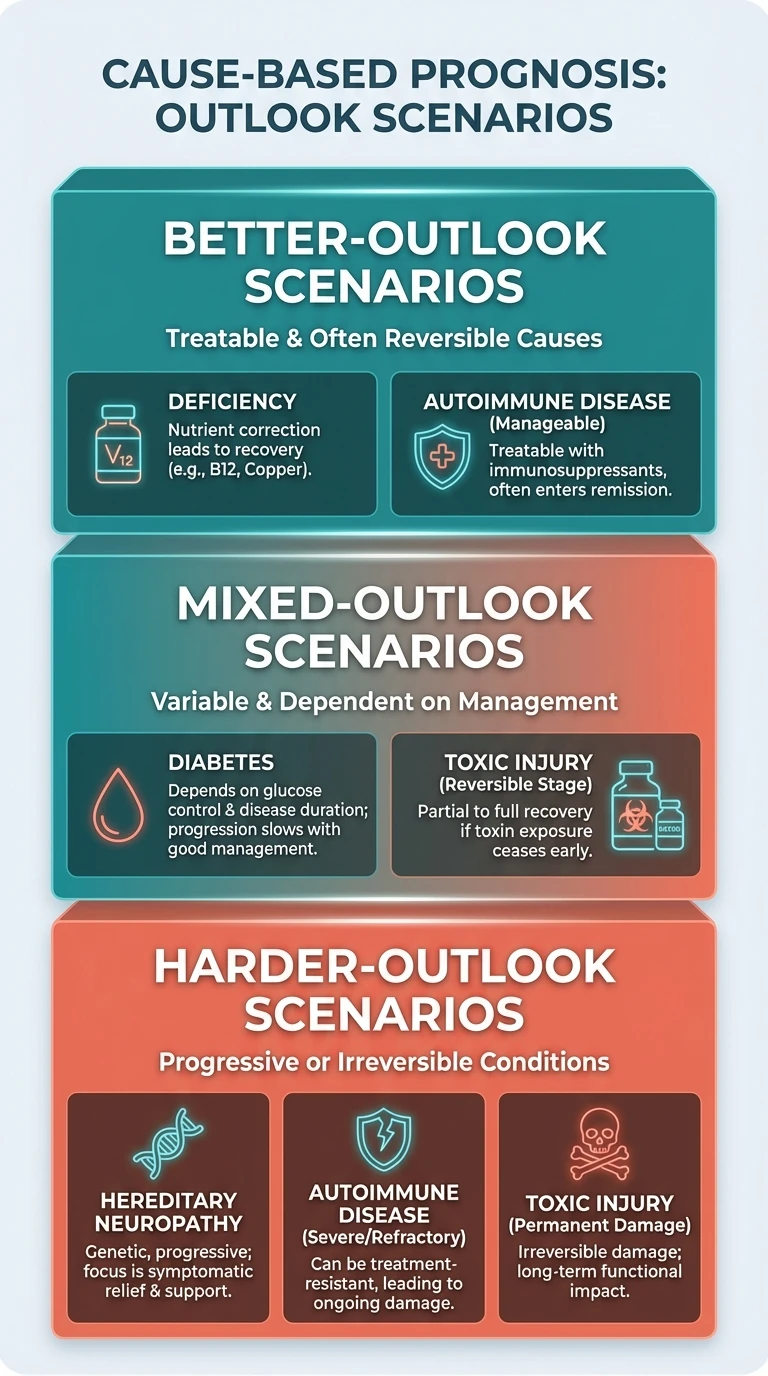
Neuropathy prognosis is driven more by the underlying mechanism than by the word “neuropathy” itself.
- Deficiency-related neuropathy can improve if caught and corrected early.
- Diabetic neuropathy often stabilizes more than it fully reverses, but better glucose control changes the slope.
- Toxic or medication-related neuropathy may improve when exposure stops, though recovery can be slow and incomplete.
- Autoimmune or inflammatory neuropathies may improve dramatically if treated quickly.
- Idiopathic neuropathy is harder to predict because the driver is still unclear.
Neuropathy Types With Better vs. Harder Long-Term Outlooks
The best prognosis usually belongs to cases where the driver is identifiable and reversible: vitamin deficiency, medication toxicity, alcohol-related depletion, entrapment, or a metabolic issue that has not been smoldering for too long. That does not guarantee full recovery, but it gives you a real lever.
The harder prognosis stories tend to involve long-standing diabetes, hereditary neuropathies, severe axonal loss, untreated autoimmune disease, or cases where symptoms were ignored until weakness and balance loss were already established. That does not mean “hopeless.” It means the goal often shifts from reversal to slowing progression, preserving function, and reducing secondary damage. Articles like Can Neuropathy Be Reversed? and toxic neuropathy help separate those tracks.
What Recovery Usually Looks Like in Real Life
Recovery is rarely linear. Pain may calm down before numbness changes. Tingling may come and go. Some people feel better functionally even while a few sensory symptoms hang around. That is normal. Nerves do not repair on the timetable people want.
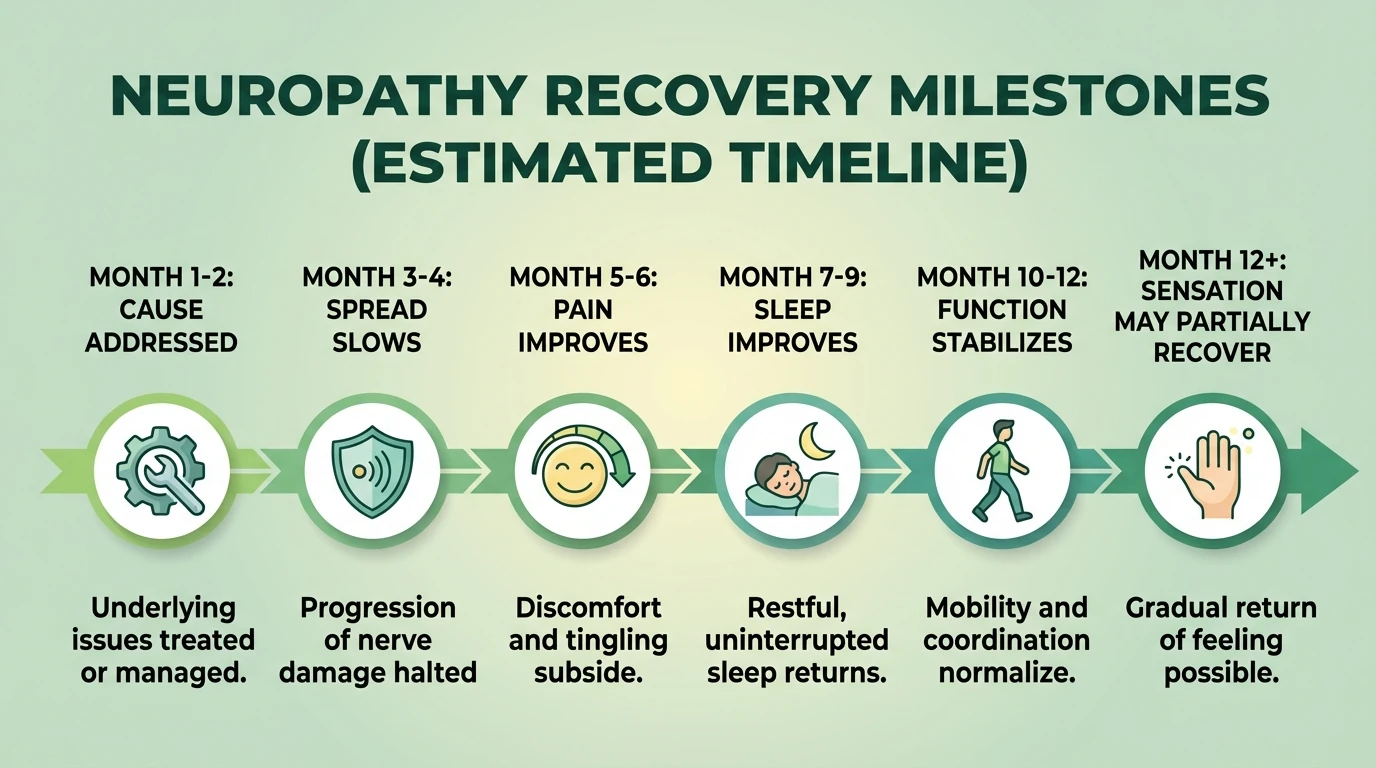
A more realistic sequence is: the cause gets controlled, the spread slows, pain becomes less constant, sleep improves, balance gets a little more reliable, and only then do you start judging whether sensation is returning. That is one reason the stages of neuropathy framework matters — it helps you see whether the condition is actually advancing or whether you are dealing with slow stabilization.
Months Matter More Than Days
If you are changing treatment every week because you cannot tell whether something is working, you will misread the process. Neuropathy prognosis often plays out over six to eighteen months, sometimes longer. Early improvements usually show up as less spread, less nighttime pain, or steadier walking, not dramatic nerve “regrowth” you can feel instantly.
Signs Your Prognosis May Be Improving
- Symptoms are no longer moving higher up the legs or into the hands
- Burning or electric pain is less constant or less intense
- Sleep is better because the pain is less intrusive
- You are falling less or feel more stable on uneven ground
- Foot wounds, skin problems, or sensory surprises are happening less often
These are not glamorous markers, but they are clinically meaningful. Function is the scoreboard. If you are not sure whether you are improving, a symptom journal is more useful than memory alone.

Better-than-yesterday markers
- Symptoms are no longer spreading
- Pain is less constant at night
- Walking feels steadier
- Fewer falls or near-falls
- Daily function is getting easier
Signs the Outlook Needs Reassessment
There are also patterns that should push you back into evaluation mode rather than passive waiting.
Do not confuse waiting with monitoring
Rapid spread, weakness, falls, or autonomic symptoms mean the prognosis story may need new testing — not more passive hope.
- Numbness is climbing quickly
- Weakness is joining a previously sensory problem
- You are developing foot drop, falls, or hand clumsiness
- The symptoms are asymmetrical, rapidly progressive, or paired with autonomic issues
- Standard treatment has not helped and the cause still is not clear
Those are the moments to stop treating prognosis like a weather report and start treating it like a diagnostic problem. This is where specialist evaluation, EMG testing, or expanded lab work can change the trajectory.
Can Neuropathy Affect Life Expectancy?
Peripheral neuropathy itself is rarely what kills people. The more important question is what it signals and what complications it creates. In older adults, neuropathy tracks with reduced life expectancy in part because it increases fall risk, injury risk, immobility, and the burden of the underlying diseases that cause it. Autonomic involvement can also raise stakes because it may affect blood pressure, heart rhythm, digestion, or bladder function.

In plain English: neuropathy is usually more of a function threat than a direct mortality threat, but ignoring it is still costly. Foot injuries, fractures, and deconditioning add up fast. That is why pages like fall prevention and daily foot care matter so much for long-term outlook.
The Most Useful Way to Think About Prognosis
Ask three questions in this order: What is causing the neuropathy? Has that cause actually been controlled? What objective sign tells me the condition is stabilizing or worsening? That framing is better than chasing a vague yes-or-no answer about recovery.

If the cause is treatable and you are acting early, prognosis is often better than people fear. If the cause is chronic, the right goal may be to bend the curve — fewer flares, fewer falls, slower progression, and more preserved independence. That still counts as winning.
Frequently Asked Questions
Does neuropathy always get worse?
No. Some neuropathies stabilize, some improve, and some continue to progress. The cause matters more than the label. Diabetic neuropathy can stabilize with better glucose control, deficiency-related neuropathy may improve after correction, and untreated progressive causes can worsen.
Can neuropathy prognosis improve after treatment starts?
Yes. Pain may improve before numbness does, and stabilization is often a real win even if symptoms do not fully disappear. The sooner the underlying cause is addressed, the better the odds of preserving function.
How long does nerve healing take?
Usually months, not days. Nerves recover slowly, so timelines often stretch over six to eighteen months, and some damage may remain permanent depending on severity and duration.
Does neuropathy shorten life expectancy?
Peripheral neuropathy itself is rarely the direct cause of death, but it can track with conditions that raise risk, such as diabetes, vascular disease, falls, infections, or autonomic dysfunction.
What is the best sign that prognosis is improving?
Less spread, fewer falls, better sleep, and more stable day-to-day function are often better signals than waiting for numbness to vanish completely.