
The first time I missed a step coming down my own staircase, I was carrying a small basket of clean towels. I caught myself on the rail at the last second. My heart pounded for the next ten minutes. That was the night I rearranged my entire stair routine. I'm going to share what I learned, and what's worked for the readers and support group members I've talked to since, so you can avoid the close call I almost didn't avoid.
Stairs are the single most dangerous architectural feature in the home of someone with neuropathy. Not because they're inherently unsafe — millions of people use them every day — but because almost everything stairs require, neuropathy makes harder. Knowing where your foot is. Trusting that it landed where you thought it did. Catching yourself with a quick correction when something doesn't feel right.
If you live in a house with stairs, you probably can't (and shouldn't have to) avoid them entirely. But you can change the way you use them. Here's how.
Why Stairs Are So Hard With Neuropathy
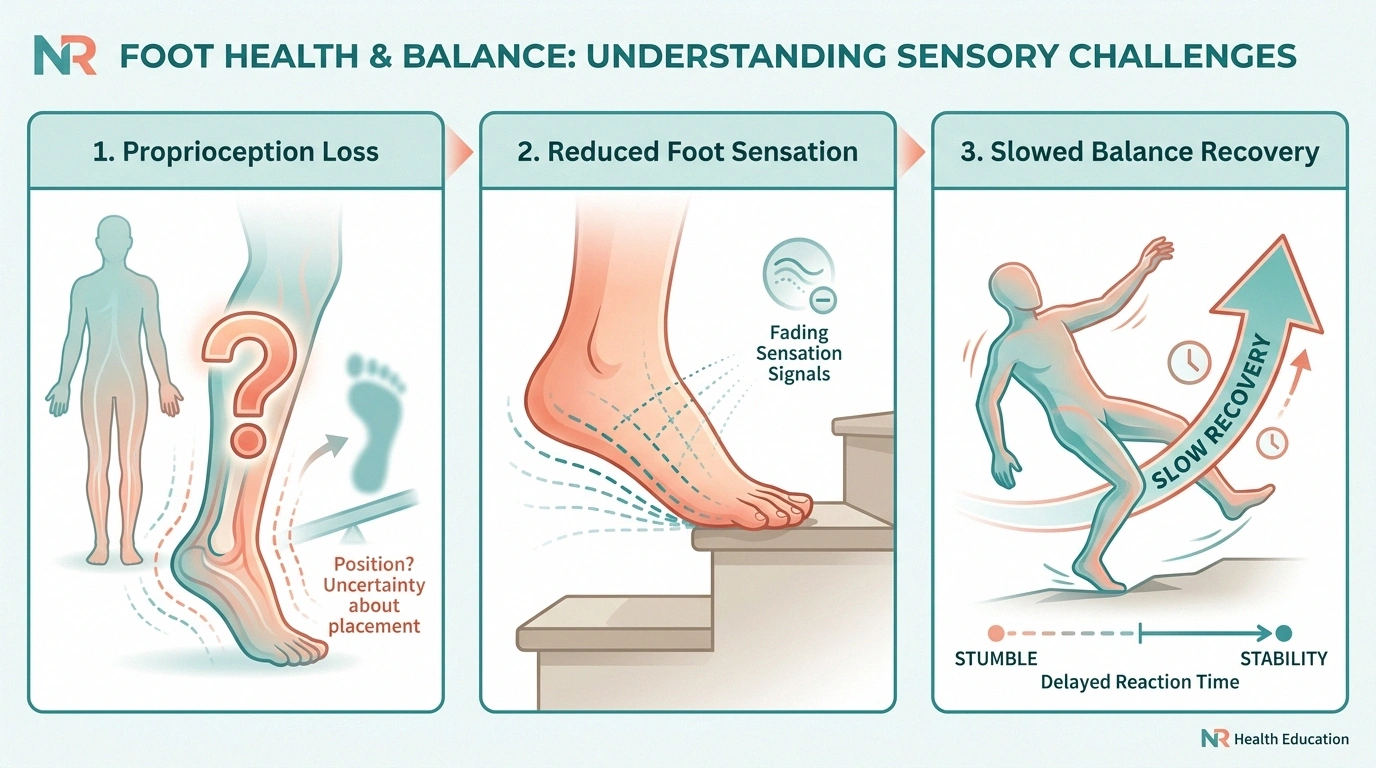
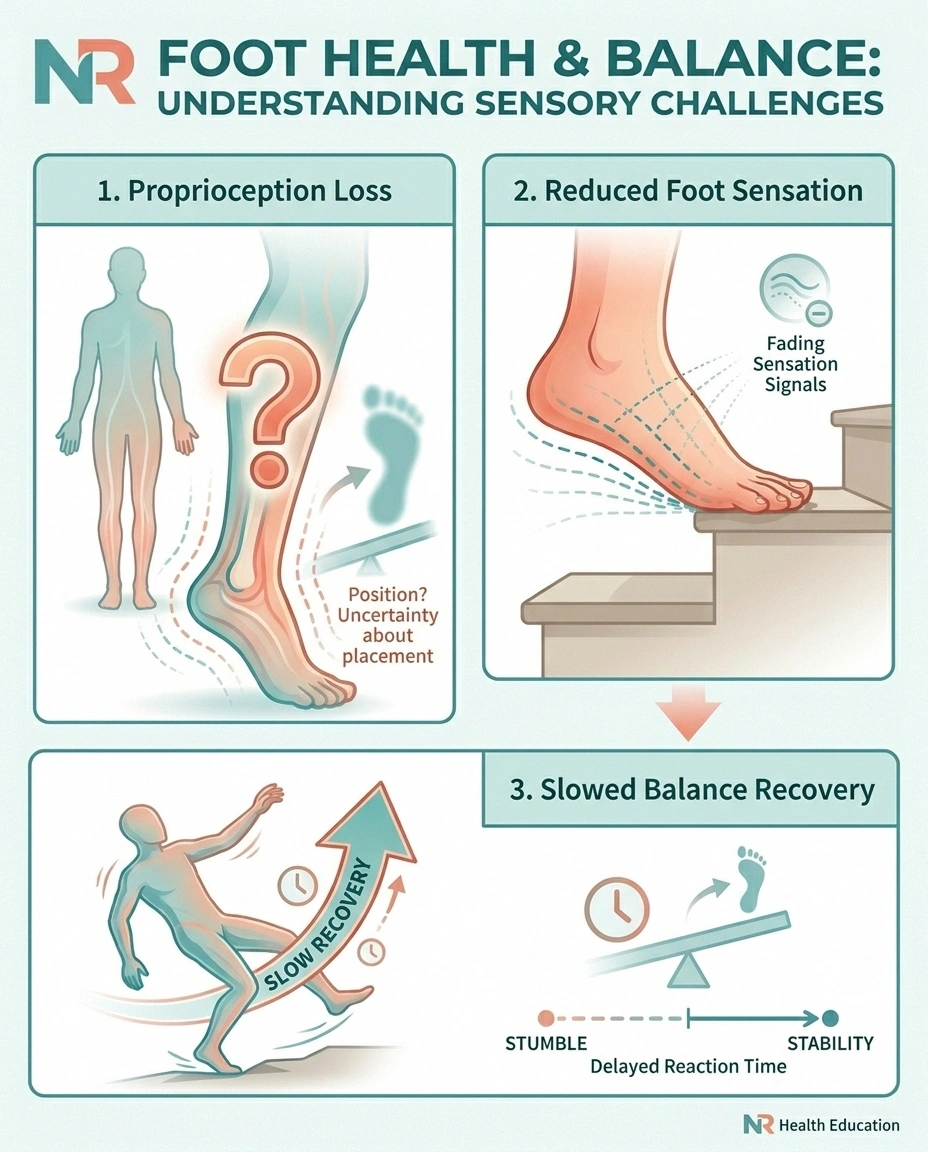
Three things go wrong on stairs when nerves aren't working right.
First, proprioception — your body's internal sense of where your limbs are in space — gets unreliable. Healthy people don't realize how much they depend on it because it works invisibly. With neuropathy, you can't always feel exactly where your foot has landed on a step. You think it's planted. It might not be. (We have a full article on this in proprioception loss in neuropathy if you want the deeper explanation.)
Second, foot sensation drops. The skin on the bottoms of your feet normally tells you “the front edge of my foot is hanging off the step” or “my heel is on a slick spot.” When that signal weakens, your brain stops getting the warnings it would normally use to make a tiny correction.
Third, balance recovery slows. When something does go wrong — and on stairs, even healthy people sometimes wobble — neuropathic legs respond more slowly to the correction. The window between “I'm starting to fall” and “I'm actually falling” gets shorter.
Researchers studying gait in diabetic peripheral neuropathy have documented all three of these patterns specifically on stairs. Going down is consistently more dangerous than going up, because eccentric quad control (controlling your weight as you descend) requires more precise feedback from the nerves than concentric control (pushing yourself up).
The Single Most Important Habit: Slow Down

If you take only one thing from this article, take this. Most stair falls happen because the person was moving at the speed they used to move — not the speed their body now needs.
~30 seconds
Extra Per Flight
That's the cost of “one step at a time, both feet on each step.” The benefit: dramatically reduced chance of mis-placing a foot or catching a heel.
The fix is unglamorous and free: one step at a time, both feet on each step before moving. You climb (or descend) one stair, your second foot joins the first on that same stair, then you move to the next stair. It looks slow. It is slow. It also dramatically reduces the chance that you'll mis-place a foot, miss the edge, or catch a heel on the way down.
An entire flight using this method takes about 30 extra seconds. I'd rather spend 30 extra seconds than spend 6 weeks recovering from a hip fracture, and so would every patient I've ever met who has actually fallen on their stairs.
Twelve Practical Habits for Stairs

1. Always use the handrail.
I don't care if your stairs are short, your hand is full, or you've been climbing them for 40 years. Use the rail. Even a light fingertip touch keeps your balance system grounded with an external reference point. If your stairs only have one rail, request quotes for adding a second rail on the other side — both-side rails reduce fall risk significantly more than a single rail.
Six Habits That Cost Nothing
2. Keep one hand free at all times.
The single most preventable cause of stair falls in older adults is carrying things with both hands. If you must move something heavy, set up a stair caddy at the bottom and another at the top, or have someone else carry it. A laundry basket can ride down on its own if you slide it carefully step by step. A grocery bag can wait at the foot of the stairs while you go up.
3. Lead with the same foot consistently.
Going down, lead with the leg that feels stronger or has better sensation. Going up, lead with the same leg. Your body learns the pattern, and it removes one decision point from each step. If both legs are equally affected, lead with whichever leg has more reliable proprioception (often the dominant side).
4. Look at the steps, not the destination.
This sounds obvious, but it's the habit I see broken most often. We look up at the door we're heading toward instead of at the next step. Bring your eyes back to the steps for the entire flight. You can look up when you arrive.
5. Pause at landings before turning.
Direction changes are when balance gets confused. Set both feet on the landing, take a breath, then start the next flight. This single habit prevents the half-step / half-turn moment that's responsible for a surprising number of mid-staircase falls.
6. Wear actual shoes — even indoors.
Backless slippers, flip-flops, slick socks, and bare feet are all stair hazards with neuropathy. Wear shoes with a low heel, a snug heel cup, and full-sole contact. (Our article on best shoes for neuropathy covers what to look for.) Many readers keep a dedicated pair of indoor shoes by the stairs and never go up or down without putting them on.
7. Light every step.
Stairs need to be lit at every step, not just at the landings. Aim for at least one fixture per flight, ideally two — one at the top and one at the bottom — plus motion-activated nightlights along the wall if you ever take the stairs in low light. The cheap stick-on motion lights from a hardware store are fine; you don't need anything fancy.
8. Mark step edges with high-contrast tape.
This is the single biggest renovation-free improvement you can make. Bright contrasting tape (yellow, white, or fluorescent on dark stairs; black on light stairs) along the front edge of each step gives your eyes the depth perception cue your nerves can no longer provide. It's also genuinely useful for visitors who don't expect a sudden step.
9. Carry only what you can carry safely.
If you can't hold the rail with one hand and what you're carrying with the other, what you're carrying needs to wait. A small backpack lets you keep both hands free and is the right tool for moving things up and down stairs.
10. Don't talk on the phone going up or down.
Cognitive distraction is now well-documented as a fall risk factor. The slight cognitive load of holding a conversation reduces the attention you can devote to foot placement. Take the phone call, then do the stairs.
11. Avoid stairs when you're tired, in pain, or freshly medicated.
Late-evening stairs after a long day of pain, or shortly after taking a new medication that affects balance, are the highest-risk versions of an already risky activity. If you can shift activities to keep heavy stair use earlier in the day, do it.
12. Practice on the bottom three steps.
If you're new to neuropathy or your symptoms are progressing, spend a week practicing your stair routine — both feet on each step, lead foot, hand on rail — using just the bottom three steps. Build the pattern at low height. Then graduate to the full flight.
Renovations and Equipment Worth Considering

Some changes go beyond habit. Here are the ones I see make the biggest difference for readers who can swing them.
Equipment Upgrades — Cost vs Impact
High-contrast step-edge tape — $10–$30
Highest-impact, no-renovation improvement. Fixes the depth-perception gap.
A second handrail. If you have one rail, adding a second on the opposite side roughly doubles your safety margin. You can grip with both hands during the highest-risk moments. Cost: typically $200–$500 installed, depending on length and finish.
Stair tread covers or runners with secure backing. Cushioned non-slip treads reduce slipping and soften the surface if you do stumble. Make sure any runner is firmly attached on every step — a loose runner is more dangerous than no runner at all. Avoid plush carpets where the edge of each step blends visually into the next.
Stair lighting upgrades. Hardwired step lights along the side walls, or LED strips under the nosing of each step, are increasingly affordable and dramatically improve safety in low-light conditions.
A stair lift or chair lift. If stairs have become genuinely dangerous despite all other modifications — or if you've already had a fall — a stair lift is worth seriously considering. They're quiet, modern ones look unobtrusive, and the new chair fold-down models don't take up much space when not in use. Cost ranges from about $3,000 for a straight-flight model to $10,000+ for curved or custom installs. Some long-term care insurance policies cover them.
A “halfway” landing seat. If your stairs have a landing midway up, a small built-in or freestanding seat lets you rest before continuing. For some people this is the difference between making the climb safely and rushing through fatigue.
Grab bars at top and bottom. The first and last step of a flight are the highest-risk locations because you're transitioning between flat ground and stairs. A short grab bar at each end gives you something to anchor to during that transition.
The Conversation to Have With Your Family
One of the hardest parts of progressive neuropathy is asking for help around the house. Many of my readers have lived in their home for decades and pride themselves on independence. Asking your kids or your spouse to bring something up the stairs feels like a small surrender.
Try reframing it: “I'd rather ask you to bring the laundry up than have you find me at the bottom of the stairs in two weeks.” That sentence usually ends the argument. The people who love you would much rather take five minutes to help than visit you in the hospital after a hip fracture.
If you live alone, set up a “stair-free zone” on whichever floor you spend most of your time. Keep the essentials there — bathroom, bedroom, comfortable chair, kitchen access. Use the stairs for the things that genuinely require the other floor. Many readers have moved their bedroom to the main floor of a two-story house and report it as one of the highest-impact decisions they've made.
When to Talk to Your Doctor

Talk to your doctor or physical therapist about stairs if any of these apply to you:
🔎 Research Says
Gait studies in patients with diabetic peripheral neuropathy show delayed weight transfer, increased medio-lateral sway, and poor edge detection on the lead foot during stair descent. These specific deficits are why “going down” is consistently more dangerous than “going up” — and why slowing down and adding visual edge cues (high-contrast tape) directly address the documented problem.
- You've had a near-miss or an actual fall on stairs in the last 6 months.
- You feel like you have to “pull yourself up” with both arms rather than stepping.
- You've started avoiding the stairs in your own home because of fear.
- Your breathing or heart rate is dramatically out of proportion to the flight you climbed (this is a sign that deconditioning is compounding the safety problem).
- One leg consistently feels weaker or “less reliable” than the other on stairs.
- You've had a recent change in medication and the stairs feel different than they did before.
A physical therapist who works with neuropathy patients can do a “stair assessment” — watching you go up and down, identifying specific weak points, and prescribing targeted exercises. This is one of the highest-yield uses of a single PT session that I've seen. (See our article on physical therapy for neuropathy for more on what to expect.)
What This All Adds Up To
I want to leave you with the same thought I leave my support group with on this topic. You are not being overcautious by treating stairs with respect. You are responding intelligently to what your body is now telling you. The people who get hurt are usually the ones still navigating their stairs the way they did 20 years ago, hoping nothing has changed.
Slow down. Use the rail. Light every step. Mark the edges. Wear real shoes. Carry only what fits in one hand. Take 30 extra seconds. These are small things, individually. Together, they're the difference between using your stairs comfortably for another 20 years and not using them at all.
Your stairs aren't your enemy. They just need a different set of rules now. Once you've internalized those rules, they recede into the background of your day — and you go on with your life.
Frequently Asked Questions
What's the safest way to go down stairs with neuropathy?
One step at a time, both feet meeting on each step before moving to the next. Always keep at least one hand on the handrail. Look down at the steps, not ahead at the destination. Lead with the same foot consistently each trip — usually your stronger or more sensitive leg. Going down is consistently more dangerous than going up because controlled descent requires more precise feedback from your nerves.
Should I avoid stairs entirely if I have neuropathy?
For most people, no. Avoiding stairs entirely tends to lead to muscle deconditioning, which makes balance and falls worse. The right approach is to use stairs more carefully — slower pace, handrail, good lighting, real shoes — rather than avoiding them. If your stair use has dropped because of fear, talk to a physical therapist about safe practice. If stairs have become genuinely unsafe even with modifications, a stair lift or moving sleeping arrangements to one floor is reasonable.
Are carpeted or uncarpeted stairs safer for neuropathy?
It depends on the carpet. Low-pile, snug, well-secured carpet with clear visual contrast at each step nosing is fine and may add a slight cushion if you stumble. Plush, deep carpet that obscures step edges is more dangerous, because it removes the depth perception cue your eyes need to compensate for reduced foot sensation. Uncarpeted hardwood or laminate stairs are safer with a low-pile runner securely attached, ideally with high-contrast tape on each nosing.
How do I make my stairs safer without remodeling?
The biggest no-renovation improvements are: high-contrast tape on every step nosing, motion-activated nightlights along the wall, securely-attached non-slip stair treads, and a dedicated pair of indoor shoes you put on before using the stairs. Beyond that, behavior changes — slower pace, hand on rail, one hand always free — make a bigger difference than most people expect.
Should I use a cane on stairs?
Generally no — single-point canes are awkward on stairs and give a false sense of security. The handrail is a much better balance aid for stair use. If you use a cane on level ground, you'll typically place it at the top or bottom of the flight, climb with both hands free (one on the rail), then pick the cane up at the other end. If you genuinely need extra support beyond a single rail, a second rail on the opposite wall is the better solution.
What kind of shoes are best for stairs with neuropathy?
Closed-back shoes with a low heel, secure heel cup, full-sole contact, and a slip-resistant sole. The shoes should hug your foot — not loose, not flopping. Avoid backless slippers, flip-flops, high heels, and bare feet. Many readers keep a dedicated pair of indoor shoes specifically for use inside the home, separate from outdoor shoes.
How do I know if it's time to consider a stair lift?
Time to seriously consider one when: you've had any actual fall on the stairs (even one), you're avoiding the stairs altogether because of fear, your breathing or heart rate is dramatically out of proportion to the climb (deconditioning compounding the safety issue), or you're sleeping on the main floor because the bedroom has become inaccessible. A stair lift restores access to the rest of your home and removes the daily fall risk. Cost is significant but generally far less than the cost of a fall, both medically and emotionally.
Should I do exercises specifically to help with stairs?
Yes. Quad-strengthening exercises (sit-to-stand from a chair, mini-squats holding a counter, step-ups on a low step), heel-to-toe walking for proprioception, and standing balance exercises all directly improve stair safety. Tai chi and gentle yoga are particularly good for the proprioceptive side. A physical therapist can build a specific program; our article on balance and fall prevention covers the basics.


