
Grief and Loss When Living with Neuropathy: Understanding What Nobody Talks About
The first time I realized what was happening, I wasn't in pain. I was standing in my kitchen, trying to button my coat to walk to the mailbox — something I'd done ten thousand times — and my fingers wouldn't cooperate. That wasn't the grief. The grief hit later that night, lying in bed, when it finally sank in that the life I'd built, the things I'd taken for granted, were slowly being rewritten without my permission.
If you're reading this, you probably know exactly what I'm describing. Not the clinical definition of neuropathy progression, but the emotional free-fall that comes with it. The sadness that doesn't have an obvious event behind it. The anger that surprises you. The strange, heavy feeling of missing a version of yourself that still exists — just can't do what it used to.
What you're experiencing has a name: ambiguous loss. And it's one of the most psychologically complex forms of grief there is — because you're mourning something that hasn't fully left, but will never fully return.
Why Neuropathy Grief Is Different From Other Chronic Illness Grief
Grief and chronic illness have a well-documented relationship. A 2017 review in Pain Research and Management confirmed that neuropathic pain is associated with worse quality of life, greater psychological distress, and significantly more lost workdays than other chronic pain conditions. But neuropathy grieving the retirement you planned operates differently from grief in other chronic illnesses, and understanding why matters for knowing how to navigate it.
neuropathy patients meet clinical thresholds for anxiety or depression — yet many have never been screened
Journal of the Neurological Sciences, 2023
With many chronic conditions, there's a diagnosis, a treatment plan, and a reasonably clear trajectory. Neuropathy doesn't work that way. The progression is unpredictable. One week you can walk to the corner store. The next, you can't feel the sidewalk beneath your feet. This unpredictability means you're grieving relationship grief when neuropathy changes your partnershipes that haven't happened yet while simultaneously processing the ones that already have.
Psychologist Pauline Boss coined the term “ambiguous loss” to describe grief without closure — when someone or something is physically present but psychologically absent, or vice versa. Neuropathy fits this perfectly. Your body is still here. But the body you knew — the one that could garden all afternoon, or hold pruning shears without thinking about it, or sleep through the night without burning feet waking you at 3am — that body is gone, and it left without a goodbye.
The Invisible Nature of Your Loss
When someone loses a spouse or a parent, the world makes room. People bring food. They send cards. They give you time. But when you lose the ability to feel your feet, or the confidence to drive at night, or the freedom to take a long walk with your partner — nobody brings casseroles for that.

This invisibility compounds the grief. A 2023 study published in the Journal of the Neurological Sciences found that over one-third of patients with small fiber neuropathy met clinical thresholds for anxiety or depression, yet many had never been screened for either. The emotional burden goes unrecognized — by doctors, by family members, sometimes even by you.
The Five Faces of Neuropathy Grief
Grief doesn't follow a predictable script. Elisabeth Kübler-Ross's famous five stages were never meant to be a checklist — they were an observation that grief has recognizable patterns. For neuropathy, I've seen five distinct patterns emerge repeatedly in the support groups I've led over the years.
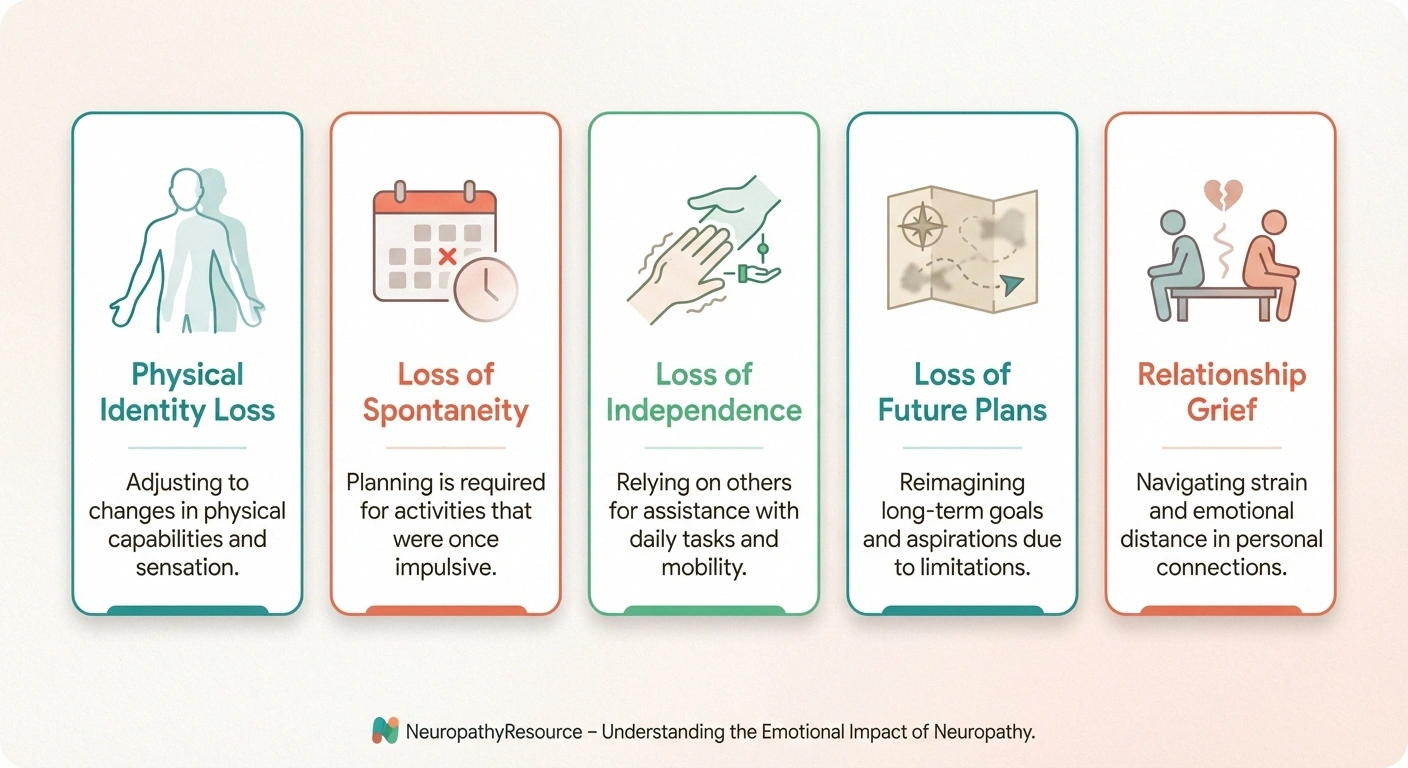

Do You Recognize These Losses?
Activities or hobbies you can no longer do the way you used to
Spontaneous outings you now have to carefully plan around symptoms
Tasks you once handled independently that now require help
Future plans — travel, retirement activities, hobbies — that feel uncertain
Changes in relationships — with your spouse, children, or friends
Loss of Physical Identity
You were the person who hiked every weekend. Or the grandparent who got on the floor with the kids. Or the cook who stood at the stove for hours preparing holiday meals. When neuropathy takes those abilities — or even just changes them — it doesn't just take an activity. It takes a piece of who you understood yourself to be.
This is identity grief, and it runs deep. Research on chronic pain and self-concept shows that people often describe feeling like “a stranger in their own body” after prolonged nerve damage. The disconnect between who you are mentally and what your body can execute creates a constant low-grade mourning.
Loss of Spontaneity
One loss that rarely gets discussed is the death of spontaneity. When every outing requires calculation — Will there be seating? Can I manage the walking? What if my pain flares? — the joy of doing things “just because” erodes. You start declining invitations not because you can't go, but because the mental effort of planning around your symptoms outweighs the pleasure of going.
Loss of Independence
For many people with neuropathy, especially those over 55, independence isn't just a convenience — it's a core value. Having to ask for help with tasks you've done independently for decades can feel humiliating, even when the people helping you are glad to do it. The shift from contributor to someone who needs assistance triggers a grief response that's often misidentified as depression.
Loss of Future Plans
You had retirement plans. Travel dreams. A garden you were going to expand. Neuropathy forces a revision of the future, and mourning the future you won't have is every bit as real as mourning the past you've lost. This is particularly painful because it's forward-looking grief — you're not just processing what happened, you're processing what won't happen.
Relationship Grief
Neuropathy changes relationships. It changes intimacy. It changes the dynamic between spouses when one becomes a caregiver. It changes friendships when you can't keep up anymore. The grief here is doubled — you're mourning the change in yourself AND the change in your connections with people you love.
The Biology Behind Why Chronic Pain Amplifies Grief
This isn't just psychology. There's a biological reason why neuropathy grief hits harder than you'd expect, and understanding the science can help you stop blaming yourself for how intensely you feel things.
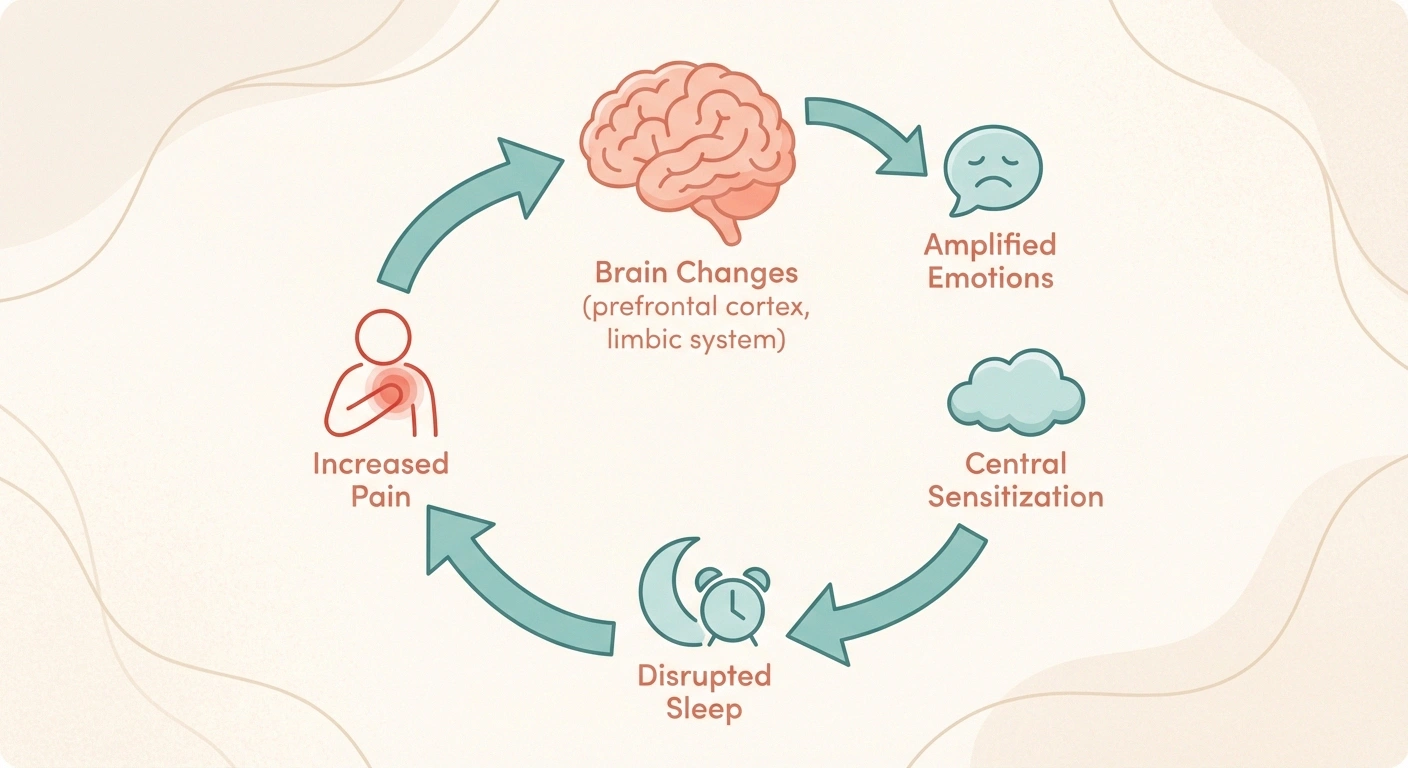
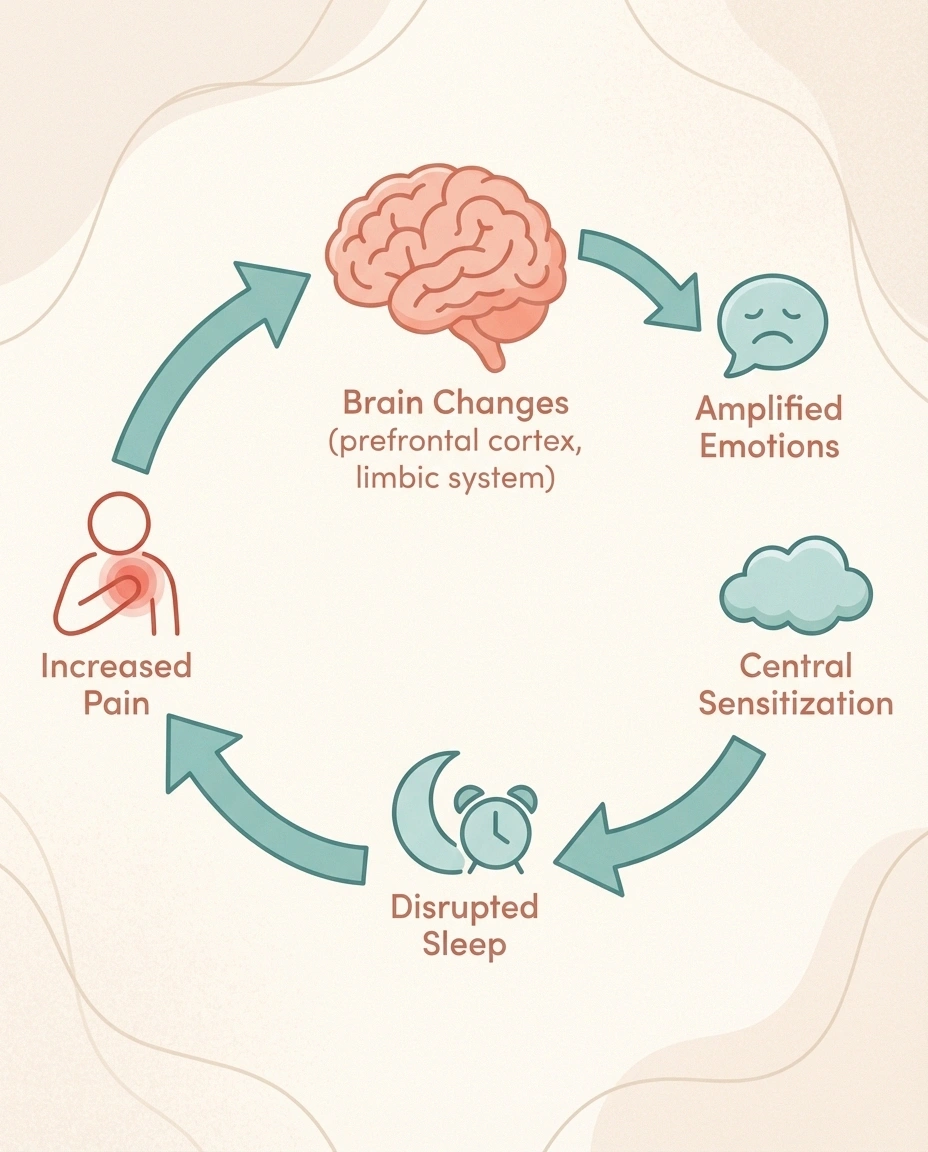
Chronic neuropathic pain physically changes your brain. Research published in the Journal of Pain found that persistent pain alters the prefrontal cortex and limbic system — the same regions responsible for mood regulation and emotional processing. Your brain is literally being rewired to experience emotions more intensely.
There's also central sensitization — a process where your nervous system gets stuck in a state of heightened reactivity. This doesn't just amplify physical pain. It amplifies emotional pain too. The tearfulness that catches you off guard, the irritability over small things, the feeling of being overwhelmed by situations you used to handle easily — all of this can trace back to a nervous system that's been pushed past its capacity.
Add sleep disruption to the equation, and the picture gets worse. Neuropathy pain intensifies at night, fragmenting the deep sleep your brain needs to process emotions and regulate mood. Without adequate sleep, your brain's ability to handle grief — which requires significant emotional processing — is fundamentally compromised.
Disenfranchised Grief: When the World Doesn't Validate Your Loss
Psychologist Kenneth Doka identified a category called “disenfranchised grief” — grief that isn't socially acknowledged, publicly mourned, or recognized by others as legitimate. Neuropathy grief fits squarely in this category.
Understanding Ambiguous Loss
Psychologist Pauline Boss identified “ambiguous loss” as grief without closure — when something is physically present but psychologically changed. Neuropathy fits this exactly: your body is still here, but the body you knew is gone. This type of grief is uniquely disorienting because it lacks the social rituals and recognition that help people process more visible losses.
The people around you may genuinely care about you, but they don't see what you've lost. They see that you're alive, that you can still walk (maybe), that you can still talk and think and breathe. From the outside, the losses are invisible — and invisible losses don't generate the social support that visible ones do.
Common invalidating responses you might recognize:
- “At least it's not cancer.”
- “You look fine to me.”
- “Have you tried just staying positive?”
- “My aunt has neuropathy and she does great.”
- “You just need to push through it.”
These comments come from care, not cruelty. But they communicate the same message: your grief isn't big enough to warrant attention. Over time, this social minimization teaches you to suppress what you're feeling — which doesn't eliminate the grief, it just drives it underground where it manifests as anxiety, withdrawal, irritability, or deepening depression.
Grieving While the Loss Is Still Happening
Here's what makes neuropathy grief uniquely disorienting: the loss isn't over. With a death, the loss is finite and complete. With neuropathy, new losses can arrive at any time. You process the grief of losing feeling in your toes, and then six months later you lose feeling in your fingers. You grieve the inability to exercise the way you used to, and then the balance problems start.
Chronic Sorrow
Grief that comes in waves, triggered by specific losses. You can still feel joy in good moments. The sadness is clearly connected to what neuropathy has taken. A normal response to an ongoing situation.
Clinical Depression
A persistent, global hopelessness affecting all areas of life. Loss of ability to feel pleasure even in good moments. May include appetite/weight changes and thoughts of self-harm. Requires professional treatment.
This ongoing nature creates what researchers call “chronic sorrow” — a grief that never fully resolves because the losses keep accumulating. It's different from depression, though it can coexist with it. Chronic sorrow is a rational emotional response to an ongoing situation. Depression is a clinical condition that requires treatment. Understanding which you're experiencing — or whether it's both — matters for how you approach it.
Signs you may be experiencing chronic sorrow rather than (or in addition to) clinical depression:
- You can still feel joy in some moments, but sadness keeps returning
- The grief intensifies after specific triggers (a new symptom, a milestone you can't participate in)
- You function relatively well most days but have periodic waves of deep sadness
- The sadness is clearly connected to specific losses rather than a general hopelessness
How to Grieve What Neuropathy Has Taken
I'm not going to tell you to “accept” your losses and move on. That's the advice of people who don't understand what you're living with. What I will tell you is that there are ways to hold your grief without letting it consume everything else — and that processing it, rather than suppressing it, is the path to less suffering.
Name What You've Lost — Specifically
Vague grief is heavier than specific grief. “Everything is different now” feels crushing. “I can't walk to the park with my grandchildren anymore” is painful but manageable. Writing down your specific losses — making them concrete and visible — takes them out of the fog and into a form you can actually process.
Some people find it helpful to write a letter to what they've lost. Not a journal entry about how they feel, but a direct acknowledgment: “I lost the ability to drive long distances. That meant freedom to me, and I miss it.” The specificity matters. It validates the loss without letting it swallow everything.
Find Witnesses to Your Grief
Grief that isn't witnessed tends to fester. A neuropathy support group — online or in-person — gives you space with people who understand without needing an explanation. When someone in the group says “I had to give up painting” or “I can't feel my grandchild's hand when they hold mine,” the room doesn't respond with “at least it's not cancer.” They respond with a nod, because they know.

If support groups aren't your style, a therapist who specializes in chronic illness or grief counseling can serve as that witness. Look for someone familiar with ambiguous loss — not every therapist understands the particular shape of grief that comes without a funeral.
Rebuild Identity Around What Remains
This is the hardest part, and it's not a one-time event. It's an ongoing process of finding new anchors for your sense of self when the old ones have shifted. If you were the hiker, maybe you become the person who knows every accessible trail in your area. If you were the cook who stood for hours, maybe you become the person who teaches others to cook from a seated position.
This isn't about replacing what you've lost — nothing replaces it. It's about expanding your definition of who you are so that neuropathy doesn't get to be the whole story. The activities may change, but the qualities that made you who you are — curiosity, generosity, creativity, determination — those haven't gone anywhere.
Allow Good Days and Bad Days
One of the cruelest aspects of neuropathy grief is the guilt that comes with good days. When you're having a low-pain day and genuinely enjoying something, a voice in the back of your mind whispers: “But it won't last.” And on the bad days, there's the opposite guilt — feeling like you should be handling things better because you had a good day yesterday.
Both of these are grief talking. Give yourself permission to feel good without guilt and feel bad without shame. The inconsistency isn't weakness — it's the natural rhythm of grief that doesn't have a finish line.
When Grief Becomes Something More: Recognizing Depression
Grief and depression share symptoms — sadness, withdrawal, difficulty sleeping, loss of interest. But they're not the same thing, and sometimes grief crosses into clinical territory that benefits from professional treatment.
If You Need Help Now
If you're having thoughts of self-harm or feeling like a burden to others, please reach out. Call or text the 988 Suicide and Crisis Lifeline (dial 988) for free, confidential support 24/7. You deserve help — for both the grief and the depression.
The NIDDK notes that chronic pain from peripheral neuropathy can lead to grief, anxiety, and depression — and that these emotional responses deserve medical attention just as much as the physical symptoms do. If you're experiencing any of these persistently for more than two weeks, it's worth talking to your doctor:
- Feeling hopeless about everything, not just neuropathy-related losses
- Loss of interest in things that still bring others joy
- Significant changes in appetite or weight
- Difficulty getting out of bed unrelated to physical pain
- Thoughts of self-harm or feeling like a burden to others
- Inability to feel pleasure or positive emotions even in good moments
If any of these describe your experience, please talk to your doctor. Depression in chronic pain conditions is highly treatable, and treatment doesn't mean your grief isn't real — it means you deserve support for both the grief AND the depression. Some of the medications commonly used for neuropathic pain, like duloxetine, can also help with depression.
Grief and Relationships: Navigating the Distance
Neuropathy grief doesn't happen in isolation. It ripples through every relationship you have, and often the people closest to you are grieving too — they're just grieving different things.

Your spouse may be grieving the partnership dynamic you once had. Your children may be grieving the parent who used to be active and adventurous. Your friends may be grieving the ease of a friendship that didn't require planning around symptoms. None of these losses cancel yours out, and yours doesn't cancel theirs. They exist in parallel.
What helps is honest communication — telling the people you love what you need (and what you don't). “I don't need you to fix this. I need you to hear that I'm struggling with it” is a sentence that can transform a frustrating conversation into a connecting one.
It also helps to be direct about practical changes. Rather than silently resenting that your spouse doesn't understand your limitations, have the conversation about what you need. “I can't stand for more than twenty minutes at the stove anymore — can we figure this out together?” is more productive than suffering through pain to avoid admitting the change.
Finding Meaning After Loss
This isn't a silver-lining section. I'm not going to tell you that neuropathy happened for a reason or that suffering builds character. What I will say — because I've seen it happen hundreds of times in support groups — is that many people eventually find meaning not because of their neuropathy, but through how they respond to it.

Remember This
Your grief is legitimate. The qualities that made you who you are — curiosity, generosity, creativity, determination — haven't gone anywhere. The activities may change, but you haven't. Grief and gratitude, loss and purpose, can all coexist. They're not contradictions. They're the full human experience of living with something difficult.
Some people become advocates for others going through similar experiences. Some discover creative outlets they never would have explored without being pushed out of their previous routines. Some find that neuropathy clarified which relationships truly mattered and which were built on shared activities rather than genuine connection.
None of this erases the grief. The grief stays. But it doesn't have to be the only thing. Post-traumatic growth research consistently shows that people can simultaneously hold deep grief and genuine gratitude, real loss and new purpose. They're not contradictions. They're the full human experience of living with something difficult.
The most important thing I can tell you is this: your grief is legitimate. Not because neuropathy is the worst thing that can happen — it's not — but because any loss that changes the shape of your life deserves to be acknowledged, felt, and honored. You're not weak for grieving. You're human. And the fact that you're looking for ways to understand and process what you're going through tells me you're already doing the hardest part.
Frequently Asked Questions
Is it normal to grieve when you have neuropathy?
Completely normal. Research shows that over one-third of people with peripheral neuropathy experience anxiety or depression, and grief is a documented response to chronic pain conditions. You are mourning real losses — abilities, independence, future plans, and aspects of your identity. The fact that these losses are invisible to others doesn't make them any less real or your grief any less valid.
How do I know if my grief has become depression?
Grief typically comes in waves and is connected to specific losses. Depression tends to feel more constant and global — affecting your interest in everything, not just neuropathy-related activities. If you feel hopeless about all aspects of life, have lost the ability to experience pleasure, have changes in appetite or sleep beyond what neuropathy itself causes, or have thoughts of self-harm, talk to your doctor. These are signs that grief may have crossed into clinical depression, which is treatable.
Why doesn't my family understand what I'm going through emotionally?
Neuropathy grief is a form of ambiguous loss — a grief without a clear event others can point to. Your family may see you as the same person, because the losses are invisible. They may also struggle with their own grief about your changes, which can make them minimizing or avoidant. Direct communication about what you need emotionally, and potentially inviting a family member to a support group or therapy session, can help bridge the gap.
Can grief actually make neuropathy pain worse?
Yes. Chronic pain and emotional distress share overlapping brain pathways. Grief triggers stress hormones like cortisol, which increase inflammation and can worsen nerve damage. The emotional burden also disrupts sleep, which further amplifies pain sensitivity. This creates a cycle where pain causes grief and grief worsens pain. Addressing both the emotional and physical aspects of neuropathy is important for managing the condition effectively.
What type of therapist should I look for?
Look for a therapist who specializes in chronic illness, chronic pain psychology, or grief counseling — ideally someone familiar with the concept of ambiguous loss. Cognitive behavioral therapy has strong evidence for helping chronic pain patients manage both pain and emotional distress. Some therapists specialize in acceptance and commitment therapy, which focuses on living a valued life alongside pain rather than waiting for pain to stop before living. Ask potential therapists if they have experience with patients who have chronic pain conditions.
Will the grief ever go away completely?
Honestly, probably not entirely — and that's okay. Because neuropathy is ongoing, the grief tends to be ongoing too. What changes is your relationship with it. Over time, with support and intentional processing, the grief becomes something you carry rather than something that carries you. The waves come less frequently and feel less overwhelming. Many people in support groups describe reaching a place where grief coexists with purpose, connection, and even joy — not replacing them, but living alongside them.


