Browse all our understanding neuropathy guides for more articles like this one.
What Does Neuropathy Feel Like? Real Descriptions of Nerve Pain
When I first started experiencing neuropathy symptoms, I found myself struggling to explain what was happening to my husband, my friends, even my diagnostic testing like EMG. “It hurts” didn't capture it. “My feet tingle” sounded trivial. The truth is, neuropathy creates sensations that most people have never experienced—and describing them to someone who hasn't felt them can feel impossible.
Over the years of leading a neuropathy support group, I've heard hundreds of descriptions from people living with this condition. What strikes me most is how similar our experiences are, even though we all struggle to put them into words. This article is my attempt to bridge that gap—both for people who suspect they might have neuropathy and for the family members, friends, and caregivers trying to understand what their loved one is going through.
The Invisible Nature of Neuropathy Pain
One of the most frustrating aspects of neuropathy is that it's invisible. There's no cast, no bruise, no swelling that people can point to and say, “Oh, that must hurt.” Your feet look completely normal from the outside. But inside, your nervous system is sending distorted, amplified, or completely absent signals—and the result is a daily experience that can range from mildly annoying to genuinely debilitating.

Understanding what neuropathy feels like matters for two important reasons. First, recognizing these sensations early can lead to faster diagnosis and treatment before nerve damage progresses through more advanced stages. Second, being able to describe your symptoms accurately to your doctor helps them determine the type and severity of your neuropathy, which directly affects your treatment plan.
Sensory Neuropathy: When Feeling Goes Wrong
Sensory neuropathy—damage to the nerves that carry information about touch, temperature, pain, and position—produces the symptoms most people associate with the word “neuropathy.” These are the sensations that tend to start in the toes and feet and gradually work their way upward. Here's how people commonly describe them:

neuropathic itch is another nerve symptom and Pins-and-Needles
This is often the earliest symptom, and nearly everyone with neuropathy experiences it at some point. People describe it as:
- “Like my foot fell asleep and won't wake up”
- “Constant static—like TV snow in my feet”
- “Tiny ants crawling under my skin”
- “Fizzing, like someone poured soda water inside my feet”
Most people have experienced the temporary pins-and-needles sensation from sitting in an awkward position. The difference with neuropathy is that this feeling doesn't go away when you shift position. It's there when you wake up, there when you go to bed, and present in varying degrees throughout the day. For many people, this tingling is the first sign that something isn't right.
Numbness and Loss of Sensation
As neuropathy progresses, tingling can give way to numbness—a partial or complete loss of feeling. This is perhaps the most unsettling symptom because it means your body's alarm system is going silent in the affected areas. People describe it as:
Americans live with peripheral neuropathy — and many struggle to describe what it feels like
- “Like wearing invisible socks—I know my feet are there, but they feel muffled”
- “Walking on wooden blocks instead of feet”
- “Like my feet are wrapped in thick cotton wool”
- “I can't feel the floor beneath me. It's like walking on clouds, but not in a good way”
- “Someone turned down the volume on my feet”
The “gloves and socks” sensation is one of the hallmark descriptions doctors listen for. It refers to a pattern where numbness affects the hands and feet in a distribution that looks like you're wearing invisible gloves and socks—because that's exactly how the nerve damage tends to progress, starting at the extremities and working inward.
Numbness creates practical dangers beyond just discomfort. People with significant numbness may not notice a pebble in their shoe, a cut on the foot, or scalding water. This is why daily foot care becomes so important—your eyes need to do the job your nerves can no longer do.
Burning Pain
Burning is one of the most commonly reported neuropathy sensations—and one of the most distressing. It's the hallmark symptom of burning feet syndrome and tends to be particularly intense at night. People describe it as:
- “Like standing on hot coals”
- “Someone held a lighter to the bottom of my feet”
- “A sunburn that never heals—deep, constant heat”
- “Like walking barefoot on scorching pavement in August”
- “My feet feel like they're on fire, but touching them they're ice cold”
That last description captures something particularly baffling about neuropathy: the disconnect between what you feel and what's actually happening. Your feet may feel like they're burning, but when you or someone else touches them, they're cold to the touch. This is because the burning sensation isn't caused by actual heat—it's caused by damaged nerves sending distorted signals to your brain.
Stabbing and Electric Shock Pain
Some neuropathy pain comes in sudden, sharp bursts rather than a constant sensation. These episodes can be startling and unpredictable:
Do You Recognize These Sensations?
Tingling or “pins and needles” that won't go away
Numbness — like wearing invisible socks or gloves
Burning pain, especially in the feet
Random electric shocks or stabbing pain
Extreme sensitivity — bedsheets or socks cause pain
Muscle weakness or cramping
Balance problems or unexplained falls
If you checked 2 or more, talk to your doctor about neuropathy testing.
- “Random electric shocks—like touching a live wire”
- “Sharp jabbing, like someone's pushing needles into my toes”
- “Sudden lightning bolts shooting up from my feet”
- “Like being stung by bees at random moments”
- “A knife being twisted in my foot—comes out of nowhere”
These facial nerve pain like trigeminal neuralgias can be triggered by movement, temperature changes, or nothing at all. They can make you gasp, flinch, or stop in your tracks. And because they're unpredictable, they create an underlying anxiety—you're never quite sure when the next jolt will come.
Hypersensitivity (Allodynia)
One of the most confusing neuropathy symptoms is allodynia—when things that shouldn't hurt become painful. This happens when damaged nerves amplify normal signals, interpreting gentle touch as intense pain:
- “A bedsheet on my feet feels like sandpaper”
- “I can't wear socks—the seam against my toes is excruciating”
- “Even a light breeze across my feet causes sharp pain”
- “My husband touched my foot gently and I nearly jumped out of bed”
- “Wearing shoes feels like walking in a box of broken glass”
Allodynia is particularly challenging because it affects basic daily activities. Finding shoes that don't cause pain becomes a serious challenge. Sleep can be disrupted because the weight of blankets on your feet becomes unbearable at night. Even the texture of socks or the pressure of walking can become sources of pain.
Motor Neuropathy: When Movement Is Affected
While sensory symptoms get most of the attention, motor neuropathy—damage to the nerves that control your muscles—creates its own set of challenges:

- Muscle weakness: “My legs feel heavy, like I'm wading through thick mud.” People may notice difficulty climbing stairs, getting up from chairs, or walking long distances.
- Muscle cramps and twitching: “My calf muscles cramp without warning—painful, tight contractions that wake me up at night.”
- Foot drop: “I can't lift the front of my foot properly. I trip on nothing—carpet edges, small bumps in the sidewalk.” This is a specific form of motor neuropathy where the muscles that lift the front of the foot weaken, causing the foot to drag or slap against the ground when walking.
- Loss of muscle bulk: Over time, the muscles in the affected areas may visibly shrink as the nerve signals that maintain muscle tone diminish.
- Coordination problems: “I used to be so sure-footed. Now I wobble like I've been drinking, and I haven't touched a drop.” The combination of reduced sensation and muscle weakness can make balance feel unreliable.
Autonomic Neuropathy: The Hidden Symptoms
Autonomic neuropathy affects the nerves that control involuntary body functions—things your body does automatically without you thinking about it. These symptoms can be harder to recognize because they don't always “feel” like nerve damage:
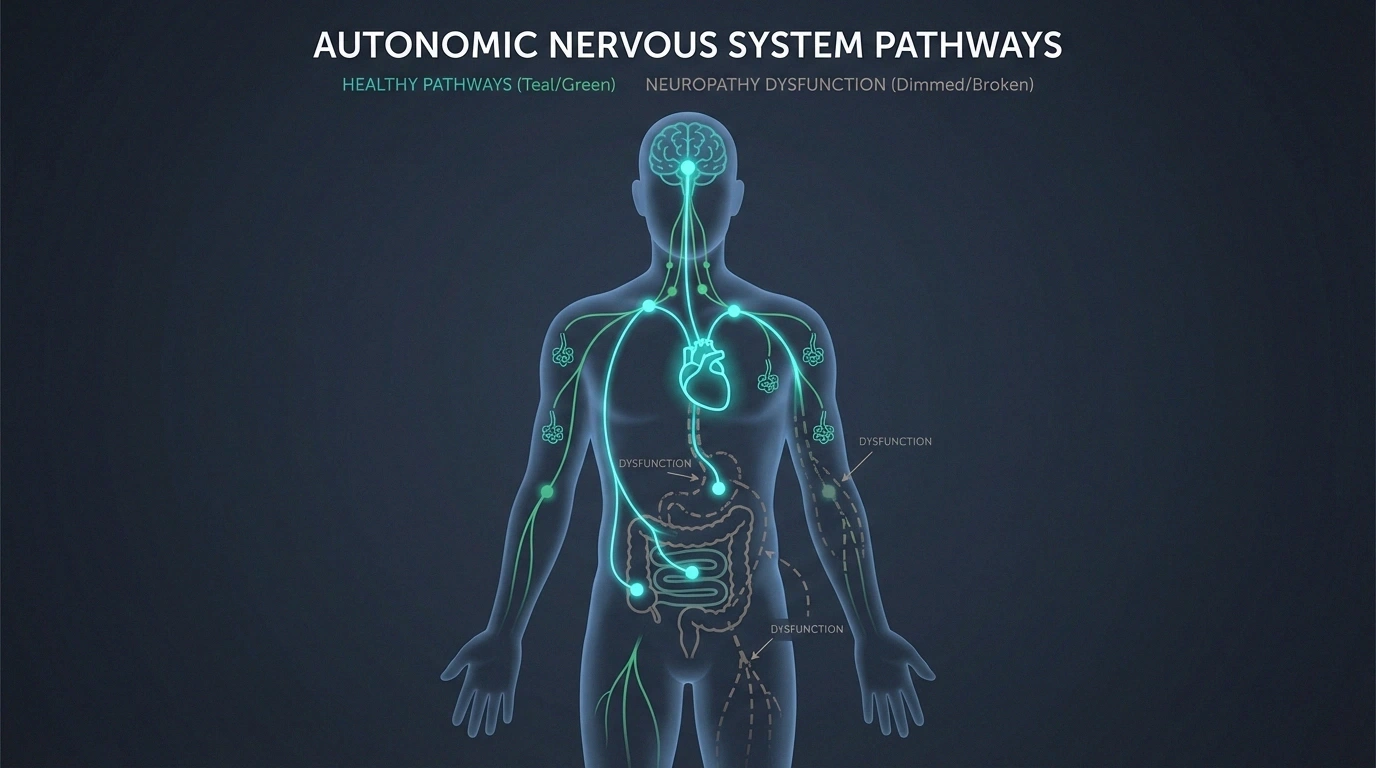
- Digestive problems: Bloating, nausea, constipation, or diarrhea that seems to have no clear dietary cause
- Dizziness when standing: A sudden drop in blood pressure when you stand up, causing lightheadedness or even fainting
- Sweating abnormalities: Excessive sweating in some areas and inability to sweat in others
- Heart rate irregularities: A heart rate that doesn't adjust properly to activity or rest
- Bladder problems: Difficulty sensing when your bladder is full, or incomplete emptying
- Temperature regulation: Feeling too hot or too cold without any external reason
Many people with autonomic neuropathy don't realize these symptoms are connected to their neuropathy. They may see different specialists for each symptom—a gastroenterologist for digestion, a cardiologist for heart rate—without recognizing the common thread of nerve damage.
⚡ Neuropathy Pain
Burning, electric, tingling. Starts in toes/fingers, spreads symmetrically. Worse at night and at rest. Pain without physical trigger.
🦴 Arthritis Pain
Deep, achy. Centered in specific joints. Worse with movement, better with rest. Associated with stiffness and swelling.
🩸 Vascular Pain
Cramping during activity, relieved by rest. Described as aching or cramping. No tingling or electric sensations. Skin changes may be visible.
How Neuropathy Symptoms Change Over Time
Neuropathy isn't static—it changes as the condition progresses or (hopefully) improves with treatment. Here's a general pattern many people experience, though everyone's journey is different:
Early stages: Intermittent tingling or numbness in the toes. You might notice it only at certain times—after a long day on your feet, or when you're trying to fall asleep. Many people dismiss these early signs as “my foot fell asleep” or “I must have been sitting wrong.”
Middle stages: Symptoms become more persistent and spread. The tingling may extend to the balls of the feet, then the whole foot, then the ankle. Pain elements—burning, stabbing, electric shocks—may appear. You start modifying behavior: choosing different shoes, avoiding long walks, checking the water temperature with your hand before stepping in the shower.
Advanced stages: Numbness may dominate, with significant loss of protective sensation. Balance problems become more pronounced. Motor recording your specific symptom patterns like muscle how leg weakness from neuropathy actually feels or foot drop may develop. Daily activities require more conscious effort and planning.
The important thing to understand is that progression is not inevitable—especially if the underlying cause is identified and treated. Correcting a vitamin deficiency, managing blood sugar levels, or discontinuing a nerve-toxic medication can halt progression and sometimes reverse symptoms, particularly in the earlier stages.
Why It Feels Hot but Is Cold
Neuropathy burning isn't caused by actual heat — it's caused by damaged nerve fibers sending distorted pain signals to your brain. This is why your feet can feel like they're on fire while actually being cold to the touch. Understanding this disconnect helps explain neuropathy to family members who may not understand why you're kicking off the blankets.
Neuropathy Pain vs. Other Types of Pain
If you're trying to figure out whether what you're experiencing might be neuropathy, it helps to understand how neuropathic pain differs from other common pain types:
Neuropathy pain typically starts in the toes or fingers and spreads symmetrically. It's often described using words like “burning,” “electric,” “stabbing,” or “tingling.” It tends to be worse at night and may include numbness alongside neuropathy vs fibromyalgia differences. It can occur without any physical trigger—you don't need to touch or move the affected area for it to hurt.
Arthritis pain is centered in specific joints, worsens with movement, and improves with rest. It's associated with stiffness and swelling. It burning feet comparison guides more “achy” and “deep” rather than burning or electric.
Vascular pain (from poor blood circulation) typically causes cramping during activity (like walking) that improves with rest—the opposite pattern from neuropathy pain, which often worsens at rest. Vascular pain is usually described as “cramping” or “aching” rather than burning or tingling.
Musculoskeletal pain is usually related to a specific area of injury or strain, gets worse with certain movements, and improves with rest and treatment. It doesn't typically produce tingling, numbness, or the electric-shock sensations characteristic of neuropathy.
The Emotional Side of Living With Neuropathy
No honest discussion of what neuropathy feels like is complete without addressing the emotional dimension. Chronic nerve pain doesn't just affect your body—it profoundly affects your mental health and quality of life:
Don't Wait — See Your Doctor
If tingling, numbness, or pain in your hands or feet lasts more than a few days or is spreading, see your doctor promptly. Early diagnosis gives you the best chance of slowing nerve damage and finding effective treatment. Don't dismiss early symptoms as “just getting older.”
- Frustration at not being believed or understood: “People look at me and think I'm fine. They can't see the fire in my feet.”
- Grief for activities you can no longer enjoy: “I used to love hiking. Now a trip to the grocery store is a challenge.”
- Sleep deprivation from nighttime symptom flare-ups: “I haven't had a full night's sleep in two years.”
- Anxiety about progression: “Every time I feel a new tingle, I wonder—is it spreading?”
- Isolation from reduced mobility and social withdrawal: “I stopped accepting dinner invitations because I can't sit comfortably for that long.”
If any of this resonates with you, please know that these feelings are normal and shared by millions of people living with neuropathy. You're not exaggerating. You're not being dramatic. What you're experiencing is real, and it deserves to be acknowledged and addressed.
When to See a Doctor
If you're experiencing any of the sensations described in this article—especially if they're persistent or getting worse—it's time to talk to your doctor. Specifically, seek medical attention if you notice:
- Tingling, numbness, or burning that lasts more than a few days
- Symptoms that are spreading (from toes to feet, from one area to both sides)
- Weakness in your hands or feet that affects daily activities
- Balance problems or unexplained falls
- Pain that disrupts your sleep most nights
- Cuts or injuries on your feet that you didn't notice happening
Early diagnosis and treatment give you the best chance of slowing or stopping progression. Your doctor can perform diagnostic tests to determine the type and cause of your neuropathy, which is essential for choosing the right treatment approach.
Frequently Asked Questions
Does neuropathy hurt all the time?
Not necessarily. Many people experience fluctuating symptoms—periods of intense pain followed by periods of relative calm. Some people have constant low-level tingling with occasional flare-ups of more intense pain. Others experience mainly numbness with intermittent shooting or burning pain. The pattern varies depending on the type of neuropathy, its cause, and its severity.
Why does neuropathy feel worse at night?
There are several reasons neuropathy symptoms tend to intensify at night. With fewer daytime distractions, your brain focuses more on pain signals. Body temperature changes at night can affect nerve function. The weight of blankets on sensitive feet causes discomfort. And cortisol levels—your body's natural anti-inflammatory—drop at night, potentially lowering your pain threshold. Learn more about why neuropathy gets worse at night and strategies to manage nighttime symptoms.
Can you have neuropathy without pain?
Yes. Some people experience primarily numbness without significant pain, especially in more advanced stages where the nerve damage has progressed beyond the “pain signal” phase. Others have motor neuropathy that mainly causes weakness and coordination problems. Autonomic neuropathy may cause digestive or cardiovascular symptoms without any pain at all. The absence of pain doesn't mean the neuropathy is less serious—in fact, complete numbness can be more dangerous because you lose the ability to feel injuries.
Is neuropathy the same as sciatica?
No. Sciatica is caused by compression or irritation of the sciatic nerve, usually in the lower back. It typically causes pain that radiates down one leg in a specific nerve pathway. Peripheral neuropathy involves damage to many nerves and usually affects both sides of the body symmetrically, starting in the toes and fingers. While both involve nerve pain, the causes, patterns, and treatments are different.
What does early-stage neuropathy feel like?
Early neuropathy typically begins with intermittent tingling or a subtle “pins and needles” sensation in the toes. You might notice it comes and goes—perhaps appearing when you're resting in the evening and disappearing by morning. Some people describe a slight numbness or a feeling that their sock is bunched up when it isn't. These early symptoms are easy to dismiss but warrant attention, especially if you have risk factors like diabetes, vitamin deficiencies, or a history of chemotherapy.
How do you explain neuropathy to someone who doesn't have it?
Try using comparisons to sensations most people have experienced. The tingling is like your foot falling asleep but never waking up. The burning is like a sunburn deep inside your foot. The numbness is like novocaine from the dentist that never fully wears off. The electric shocks are like accidentally touching a live wire. The hypersensitivity is like having a bruise so bad that even a bedsheet touching it causes pain. These analogies help people understand the intensity even if they haven't experienced neuropathy themselves.
You're Not Alone in This
If you recognized your own experience in the descriptions above, I hope knowing that millions of others share these same sensations brings some comfort. Peripheral neuropathy affects an estimated 20 million people in the United States alone, and the real number is likely higher because so many cases go undiagnosed.
Your pain is real. Your frustration is valid. And while neuropathy may change what your daily life looks like, it doesn't have to define it. With proper diagnosis, treatment of the underlying cause, and a management plan that may include nerve-supportive supplements, appropriate medications, topical treatments, and lifestyle adjustments, many people find their how classic neuropathy symptoms compare with Lyme patterns stabilize or improve over time.
The first step is talking to your doctor. The second step is never letting anyone tell you it's “all in your head.”