
Neuropathy and Heat Sensitivity: Managing Symptoms in Summer
The first summer after my neuropathy diagnosis, I made the mistake of spending an entire afternoon at a family barbecue. By the time we packed up, my feet felt like they were on fire — not the usual tingling I'd learned to live with, but a deep, throbbing burn that kept me up most of the night. It was the moment I realized that heat and neuropathy don't play well together, and that summer would require a whole new set of strategies.
If you've noticed your neuropathy symptoms getting worse when temperatures climb, you're far from alone. Research published in the Journal of Pain Medicine has found that many neuropathy patients can actually predict weather changes twelve to twenty-four hours in advance based on increased pain levels. Understanding why heat affects your nerves — and what you can do about it — can make the difference between dreading summer and actually enjoying it.
Browse all our living with neuropathy guides for more articles like this one.
Why Does Heat Make Neuropathy Worse?
To understand why your symptoms flare in warm weather, it helps to know what's happening inside your body when temperatures rise. When it's hot outside, your body triggers a series of cooling mechanisms — and for people with damaged nerves, each one can create problems.
of neuropathy patients report worse symptoms during temperature extremes
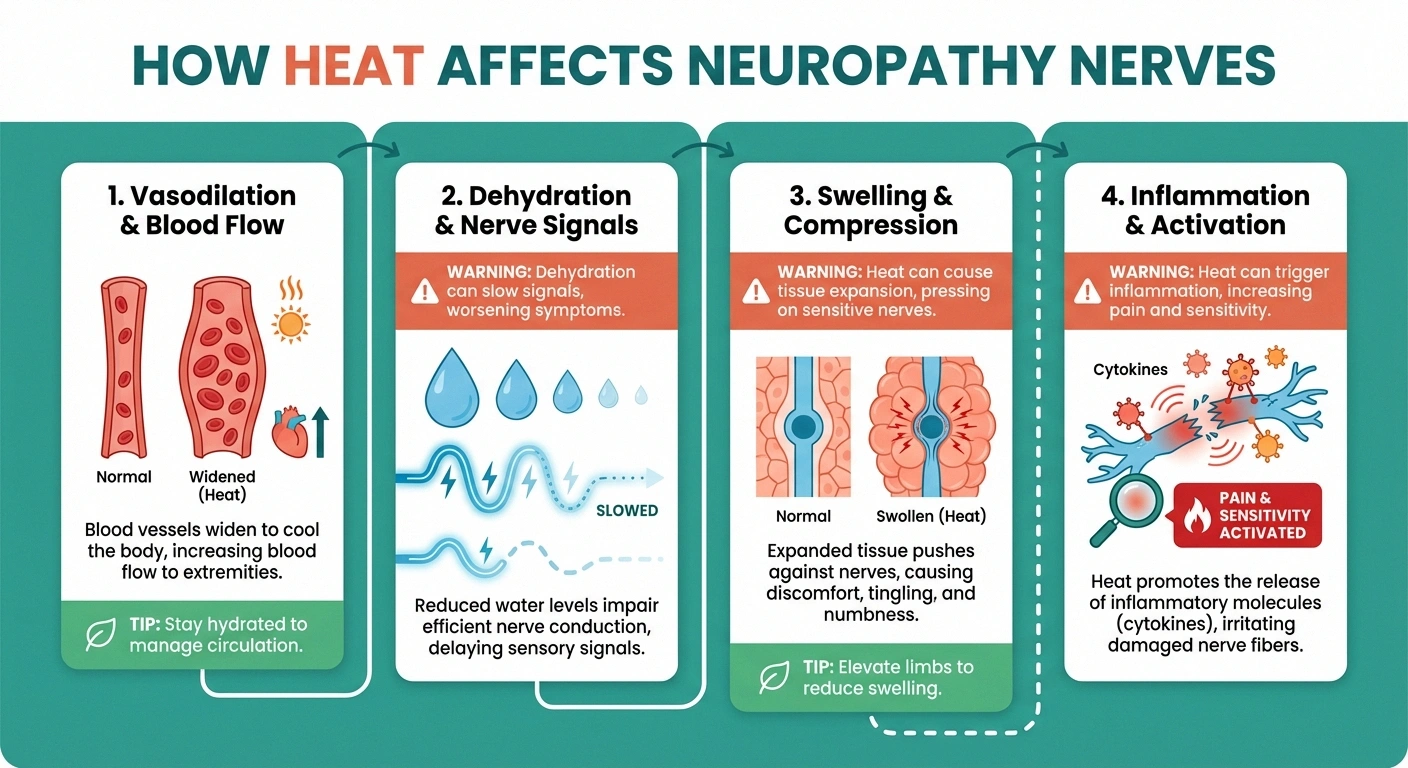
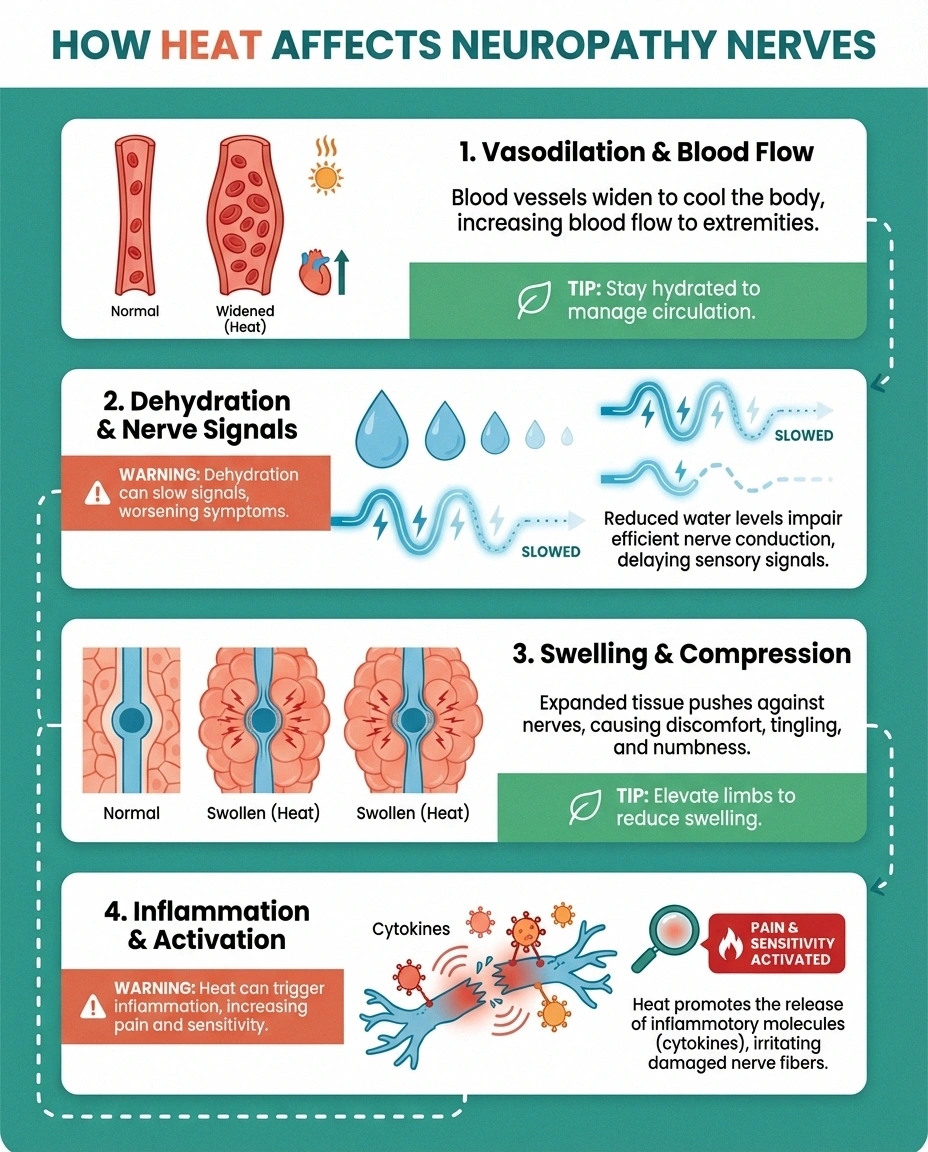
Vasodilation and blood flow changes. Your blood vessels widen (a process called vasodilation) to release heat through the skin. While this sounds beneficial, the increased blood flow can create uncomfortable throbbing and pulsing sensations in nerves that are already damaged. For people with small fiber neuropathy, this effect can be particularly intense because the small nerve fibers responsible for temperature regulation are the very ones that are compromised.
Dehydration and electrolyte loss. Sweating is your body's primary cooling mechanism, but it comes with a cost. As you lose fluids through sweat, your blood becomes more concentrated and circulation to your extremities may decrease. Even mild dehydration can impair nerve signaling, and electrolyte imbalances — particularly drops in sodium, potassium, and magnesium — can directly affect how your nerves transmit signals. A study in the Journal of Clinical Neurophysiology confirmed that proper hydration is essential for maintaining nerve conduction velocity.
Swelling and nerve compression. Heat causes tissues to expand and fluids to accumulate, especially in the feet, ankles, and hands. This swelling can put additional pressure on nerves that are already struggling, particularly in confined spaces like the carpal tunnel or tarsal tunnel. If your shoes feel tighter on hot days, this swelling may be contributing to increased pain and tingling.
Increased inflammatory response. Temperature changes can trigger the release of inflammatory chemicals called cytokines, which sensitize already damaged nerves. According to research from the National Institute of Neurological Disorders and Stroke, this inflammatory cascade can lower your pain threshold — meaning sensations that would normally feel mild become significantly more painful.
Autonomic dysfunction. Many people with neuropathy also have some degree of autonomic nerve damage, which affects the body's ability to regulate temperature through sweating. If your autonomic nerves aren't functioning properly, your body may struggle to cool itself efficiently, leading to a dangerous cycle where rising body temperature further aggravates nerve symptoms.
Symptoms That Get Worse in Summer Heat
Not everyone with neuropathy experiences the same summer symptoms. How heat affects you depends on which type of nerve fibers are damaged and how severely. Here are the most common heat-related complaints I hear from readers:
🌡️ Common Summer Neuropathy Symptoms
Intensified burning — especially in feet after walking on warm surfaces
Amplified tingling — hands and feet feel “electrified”
Swollen feet and ankles — gets worse throughout the day
Dizziness — from blood pressure drops when standing
Disrupted sleep — hot nights make nighttime nerve pain worse
Intensified burning sensations. This is by far the most reported summer symptom. The burning feet that many neuropathy patients already experience can become nearly unbearable on hot days, particularly after walking on warm pavement or standing for extended periods.
Increased tingling and “pins and needles.” Heat-related vasodilation can amplify the abnormal electrical signals from damaged nerves, making the familiar tingling sensations noticeably stronger. Some people describe it as their feet or hands feeling “electrified.”
Greater numbness and reduced sensation. Paradoxically, some people experience more numbness in the heat — not less. This can be particularly dangerous because reduced sensation in your feet means you may not notice burns from hot pavement, sand, or pool decks.
Swollen feet and ankles. Heat-related edema (swelling) puts additional pressure on compromised nerves and can make shoes uncomfortable or even unwearable. This swelling often gets worse as the day progresses.
Dizziness and lightheadedness. If autonomic neuropathy affects your blood pressure regulation, heat can cause orthostatic hypotension — a sudden drop in blood pressure when you stand up — leading to dizziness and an increased risk of falls.
Sleep disruption. Hot nights can make neuropathy-related sleep problems significantly worse. When your body can't cool down effectively, nerve pain tends to intensify right when you're trying to rest.
Small Fiber Neuropathy and Heat: A Particularly Difficult Combination
If you have small fiber neuropathy, you may find summer especially challenging. Small nerve fibers (called C-fibers and A-delta fibers) are specifically responsible for detecting temperature and pain. When these fibers are damaged, your temperature perception becomes unreliable — you might feel burning heat when the actual temperature is only moderately warm, or you might not feel dangerous heat at all.
Research Says
About 40% of people with small fiber neuropathy report significant worsening of symptoms in warm weather — compared to roughly 25% of those with large fiber neuropathy alone. The small C-fibers and A-delta fibers responsible for temperature detection are the very ones damaged in SFN.
Small fiber neuropathy also commonly affects the autonomic nerves that control sweating. Some people with this condition experience reduced sweating (hypohidrosis) in their affected areas, making it harder for those body parts to cool down naturally. Others experience excessive sweating (hyperhidrosis) in unaffected areas as the body compensates. Either way, temperature regulation becomes unpredictable and often inadequate.
Research suggests that approximately forty percent of people with small fiber neuropathy report significant worsening of symptoms during warm weather, compared to about twenty-five percent of those with large fiber neuropathy alone.
Practical Strategies for Managing Heat-Related Neuropathy Symptoms
The good news is that with some planning, you don't have to spend every summer hiding indoors. Here are the strategies that have worked best for me and for the thousands of readers who've shared their experiences:
Key Takeaway
Hydration is the single most important summer strategy. Your nerves need proper fluid and electrolyte balance to function — even mild dehydration can increase tingling, burning, and pain. Aim for 8–10 glasses of water daily, plus electrolytes containing magnesium, potassium, and sodium.
Stay Hydrated — Beyond Just Drinking Water
Hydration is arguably the single most important thing you can do for your nerves in summer. But “drink more water” is only part of the picture. Your nerves need proper electrolyte balance to function, so:
Aim for at least eight to ten glasses of water daily, and more if you're spending time outdoors or exercising. Consider adding an electrolyte supplement — look for ones containing sodium, potassium, and magnesium, which is particularly important for nerve function. Avoid excessive caffeine and alcohol, both of which contribute to dehydration. Eat water-rich foods like watermelon, cucumbers, and berries. Keep water at room temperature rather than ice-cold — very cold drinks can trigger temperature-sensitive nerve pain in some people.
Plan Around the Heat
The simplest strategy is often the most effective: avoid the worst of the heat whenever possible. Schedule outdoor activities for early morning (before ten AM) or evening (after six PM). If you need to be outside during peak heat, plan for frequent breaks in air conditioning or shade. Check the weather forecast each morning and adjust your plans accordingly — a day with eighty percent humidity is going to be harder on your nerves than a dry ninety-degree day.
Dress Strategically
What you wear makes a bigger difference than you might expect. Choose loose, breathable fabrics like cotton, linen, or moisture-wicking synthetics. Avoid tight clothing that restricts circulation, especially around your ankles and wrists. Light colors reflect heat better than dark ones. And invest in a wide-brimmed hat and UV-protective clothing if you're spending extended time outdoors — sunburn adds another source of inflammation that your nerves don't need.
Protect Your Feet — This Is Critical
Your feet are ground zero for most neuropathy symptoms, and summer adds several specific dangers. Never walk barefoot on hot surfaces — pavement, sand, and pool decks can reach temperatures over one hundred forty degrees Fahrenheit on a sunny day, and if your sensation is reduced, you may not realize you're being burned until the damage is done.

Wear breathable, supportive shoes — your neuropathy-appropriate shoes should have good ventilation for summer. Moisture-wicking socks are essential to prevent sweat from creating blisters or fungal infections. Check the inside of your shoes before putting them on — they can get surprisingly hot if left in a car or direct sunlight. And practice daily foot care, inspecting for any injuries you may not have felt.
Use Cooling Strategies That Won't Backfire
Cooling your body down can bring significant relief, but some approaches work better than others for neuropathy patients:
Ice Pack Safety Warning
Never apply ice packs directly to areas with reduced sensation. Neuropathy can prevent you from feeling when cold reaches dangerous levels. Use cool (not ice-cold) compresses, always wrap cold items in a towel, limit to 15 minutes, and check your skin frequently during use.
Cool (not ice-cold) compresses on the back of your neck, wrists, or forehead can lower your core temperature quickly. A cooling vest or neck wrap is invaluable for outdoor activities. A cool foot soak (around seventy to seventy-five degrees Fahrenheit) can provide relief without the shock of cold water. Air conditioning is your friend — keep your home between sixty-eight and seventy-two degrees when possible. Consider a small portable fan for situations where air conditioning isn't available.
A word of caution: Avoid ice packs directly on areas with reduced sensation. If your nerve damage limits your ability to feel temperature accurately, you may not notice when an ice pack is causing frostbite damage to your skin.
Exercise in Summer With Neuropathy: Finding the Right Balance
Regular exercise is one of the best things you can do for neuropathy — walking, swimming, and yoga have all been shown to improve nerve function and reduce pain. But exercising in the heat requires extra caution.

Swimming is your summer superpower. Pool water (typically eighty-three to eighty-eight degrees Fahrenheit) provides a naturally cool environment while supporting your body weight and reducing joint strain. Water therapy is especially beneficial because it keeps your body temperature regulated while you exercise. If your local pool or gym offers aquatic therapy classes, summer is the perfect time to try them.
Move your walks indoors or to early morning. If walking is part of your routine, shift to a climate-controlled environment during the hottest months. Mall walking, treadmills, or indoor tracks are all excellent alternatives. If you prefer being outdoors, walk before eight AM or after sunset when temperatures are more manageable.
Listen to your body more carefully than usual. In summer, you may notice your exercise tolerance is lower — that's normal. Reduce intensity by about twenty percent on very hot days. Take more frequent breaks. And if you start feeling dizzy, nauseated, or notice your neuropathy symptoms suddenly increasing during exercise, stop immediately and cool down.
Managing Summer Sleep When Neuropathy Keeps You Awake
Hot nights are a double challenge for neuropathy patients. Your symptoms tend to be worse at night to begin with, and added heat can make sleep feel impossible. Here's what helps:


Keep your bedroom cool — sixty-five to sixty-eight degrees Fahrenheit is ideal for sleep, and even more important when neuropathy is a factor. Use moisture-wicking sheets and breathable bedding materials. A ceiling fan or oscillating fan can improve air circulation without the noise of a window AC unit. Cooling mattress toppers or pads that circulate cool water can make a significant difference. Take a cool shower about an hour before bed — this lowers your core body temperature, which helps signal your body that it's time to sleep.
If your feet are the main problem, try placing a cool (not cold) damp towel over them as you fall asleep. Some readers have found that elevating their feet slightly with a pillow helps reduce heat-related swelling that contributes to nighttime pain.
Summer Travel and Outdoor Activities With Neuropathy
Summer vacations and outdoor activities don't have to be off-limits, but they do require more planning when you have neuropathy. Here's a quick survival guide:
Beach trips. Bring water shoes for hot sand. Stay under an umbrella or tent for shade. Keep your feet elevated when sitting. Apply sunscreen carefully — sunburn adds inflammatory stress. Keep water and electrolyte drinks in a cooler within easy reach.
Hiking and nature walks. Choose shaded trails. Start early. Bring twice as much water as you think you'll need. Wear breathable, supportive hiking shoes with moisture-wicking socks. Plan your route so you know where rest stops are.
Traveling. If you're traveling with neuropathy, pack extra cooling supplies (neck wraps, portable fans, extra water). Request ground-floor hotel rooms to reduce walking. Choose accommodations with reliable air conditioning. And don't forget to bring any medications or supplements you take for nerve pain — heat can sometimes require dosage timing adjustments, so check with your doctor before your trip.
When Heat Symptoms Signal Something More Serious
While heat-related neuropathy flare-ups are usually temporary and manageable, certain symptoms warrant medical attention:
Seek Medical Attention
Call your doctor or seek emergency care if you experience: sudden new numbness or weakness that doesn't resolve when you cool down, severe dizziness or fainting, burns or wounds on your feet you didn't feel, or any signs of heat stroke (hot dry skin, rapid pulse, confusion).
Sudden new numbness or weakness that doesn't improve when you cool down. Severe dizziness, confusion, or fainting in the heat — this could indicate heat exhaustion or problems with autonomic regulation. Burns or wounds on your feet that you didn't feel happening. Rapidly worsening symptoms that are significantly beyond your normal pattern. Any signs of heat stroke — hot dry skin, rapid pulse, confusion, or loss of consciousness — which is a medical emergency.
If you have diabetes along with neuropathy, be especially vigilant. Heat can affect blood sugar levels and insulin absorption, which in turn can worsen nerve damage from diabetes. Check your blood sugar more frequently during heat waves and hot weather activities.
The Connection Between Heat, Neuropathy, and Your Other Health Conditions
Neuropathy rarely exists in isolation. Many of the conditions that cause or accompany neuropathy are also affected by heat:
Diabetes. Heat can change how your body absorbs insulin and may cause blood sugar fluctuations. Poor blood sugar control directly worsens neuropathy symptoms. Stay on top of your glucose monitoring in summer.
Medications. Some neuropathy medications can increase your sensitivity to heat or reduce sweating. Gabapentin, pregabalin, and duloxetine can all affect heat tolerance to varying degrees. Talk to your prescribing doctor about whether your medications may make summer harder.
Circulation problems. Conditions like peripheral artery disease, which commonly coexists with neuropathy, can be worsened by heat-related dehydration and blood pressure changes.
Obesity. Carrying extra weight makes heat regulation harder and puts additional stress on nerves, particularly in the feet and legs. If weight is contributing to your neuropathy, summer can compound both issues.
Building Your Personal Summer Management Plan
The strategies that work best are different for everyone, which is why I recommend creating a personalized summer plan. Here's a framework you can adapt:

Your 5-Step Summer Action Plan
Track Your Triggers
Keep a 2-week diary noting temperature, humidity, activities, and symptom levels to find your personal thresholds.
Identify Worst Symptoms
Burning feet? Swelling? Balance issues? Knowing your primary problem lets you target the right solutions.
Set Up Your Environment
Check AC, stock cooling supplies, prepare a summer go-bag with water, cooling towels, sunscreen, and medications.
Talk to Your Doctor
Discuss seasonal medication adjustments and plan for any summer travel or activities.
Build in Recovery Time
After heat exposure: cool shower, elevate feet, rehydrate, and rest in AC to prevent minor flares from becoming multi-day episodes.
Step one: Track your triggers. For two weeks at the start of summer, keep a simple diary noting the temperature, humidity, your activities, and your symptom levels. This will help you identify your personal thresholds — some people flare up at eighty degrees, others don't have trouble until it hits ninety-five.
Step two: Identify your worst symptoms. Is it burning feet? Swelling? Balance problems? Knowing what bothers you most lets you prioritize the right interventions.
Step three: Set up your environment. Make sure your home, car, and workspace are ready for summer. Check your air conditioning. Stock up on cooling supplies. Put together a summer “go bag” with water, cooling towels, sunscreen, and any medications.
Step four: Talk to your doctor. Discuss your summer symptoms and ask whether any medication adjustments make sense for the warmer months. Mention any specific activities or trips you're planning so your doctor can help you prepare.
Step five: Build in recovery time. After any significant heat exposure, give your body time to recover. A cool shower, elevated feet, a rehydration break, and some time in air conditioning can prevent a minor flare from becoming a multi-day episode.
Frequently Asked Questions
Does heat actually damage nerves, or just make symptoms worse?
Heat typically makes existing nerve damage symptoms more noticeable rather than causing new nerve damage. The increased blood flow, swelling, and dehydration that come with heat exposure can temporarily amplify pain signals from already damaged nerves. However, prolonged exposure to extreme heat without proper precautions — particularly for people with diabetic neuropathy — could contribute to conditions that worsen nerve damage over time.
Why do my feet burn more in summer even when I'm indoors?
Indoor temperatures and humidity still fluctuate with the seasons. Even in air conditioning, summer indoor environments tend to be warmer than winter ones. Your body also responds to overall seasonal changes in barometric pressure and humidity. Additionally, if you've been outdoors earlier in the day, the inflammatory response triggered by heat exposure can persist for hours even after you've cooled down.
Is it safe to use ice packs on numb feet during summer?
You should use caution with ice packs if you have reduced sensation. Because neuropathy can impair your ability to feel temperature accurately, you may not realize when an ice pack is causing frostbite or skin damage. Use cool compresses rather than ice, wrap any cold items in a towel, limit application to fifteen minutes at a time, and check your skin frequently during use.
Can swimming in a cold pool help with heat-related neuropathy symptoms?
Swimming in moderately warm water (eighty-three to eighty-eight degrees Fahrenheit) is generally the best option. Very cold pool water can actually trigger nerve pain in some people, particularly those with cold-sensitive neuropathy. The ideal approach is a pool that feels comfortable — not shockingly cold — and allows you to exercise while keeping your body temperature regulated.
Should I change my neuropathy supplements or medications in summer?
Never change medication dosages without consulting your doctor. However, it is worth discussing with your healthcare provider whether seasonal adjustments make sense. Some people benefit from increasing their magnesium or electrolyte intake during summer months. Certain medications can also affect your heat tolerance or sweating ability, so your doctor may want to adjust timing or dosages during the hottest months.
Does humidity or dry heat affect neuropathy differently?
Yes, they can affect you differently. High humidity tends to cause more swelling and fluid retention, which puts pressure on nerves. It also makes it harder for sweat to evaporate, reducing your body's natural cooling ability. Dry heat, while still challenging, typically causes less swelling but more dehydration risk. Many neuropathy patients report that humid heat is harder to tolerate than dry heat.
Living Well in Summer Despite Neuropathy
Summer doesn't have to be a season of suffering when you have neuropathy. Yes, heat can make your symptoms worse — sometimes significantly. But with the right strategies, preparation, and mindset, you can still enjoy cookouts, beach trips, garden time, and long summer evenings.

The key is shifting from reactive to proactive. Instead of waiting for a flare-up and then trying to deal with it, build heat management into your daily routine the same way you've learned to manage other aspects of living with neuropathy. Keep your body hydrated, your environment cool, and your feet protected. Know your limits, but don't be afraid to push them gently when conditions are right.
And remember — you've already proven you can adapt to life with neuropathy. Summer is just one more adaptation. Talk to your doctor about your specific situation, lean on the strategies that work best for you, and give yourself permission to take it a little easier on the hottest days. Your nerves will thank you.