
Neuropathic Itch: When Nerve Damage Makes You Scratch
Most people think of neuropathy as numbness, tingling, or burning pain. But there's a symptom that doesn't get nearly enough attention—one that can be just as maddening, if not more so: the itch that comes from nowhere, responds to nothing, and drives you absolutely crazy.
I first heard about neuropathic itch from a reader who described it perfectly: “It's like something is crawling under my skin, but there's nothing there. I scratch until I bleed and it doesn't help.” That description stuck with me because it captures exactly what makes this symptom so different from ordinary itching—and so frustrating to manage.
Neuropathic itch affects approximately eight percent of all people with chronic itch, and about one-third of people experiencing neuropathic pain also report neuropathic itching. If this sounds like you, you're not imagining it, you're not alone, and there are things that can help. Let's talk about what's really going on and what you can do about it.
What Is Neuropathic Itch?
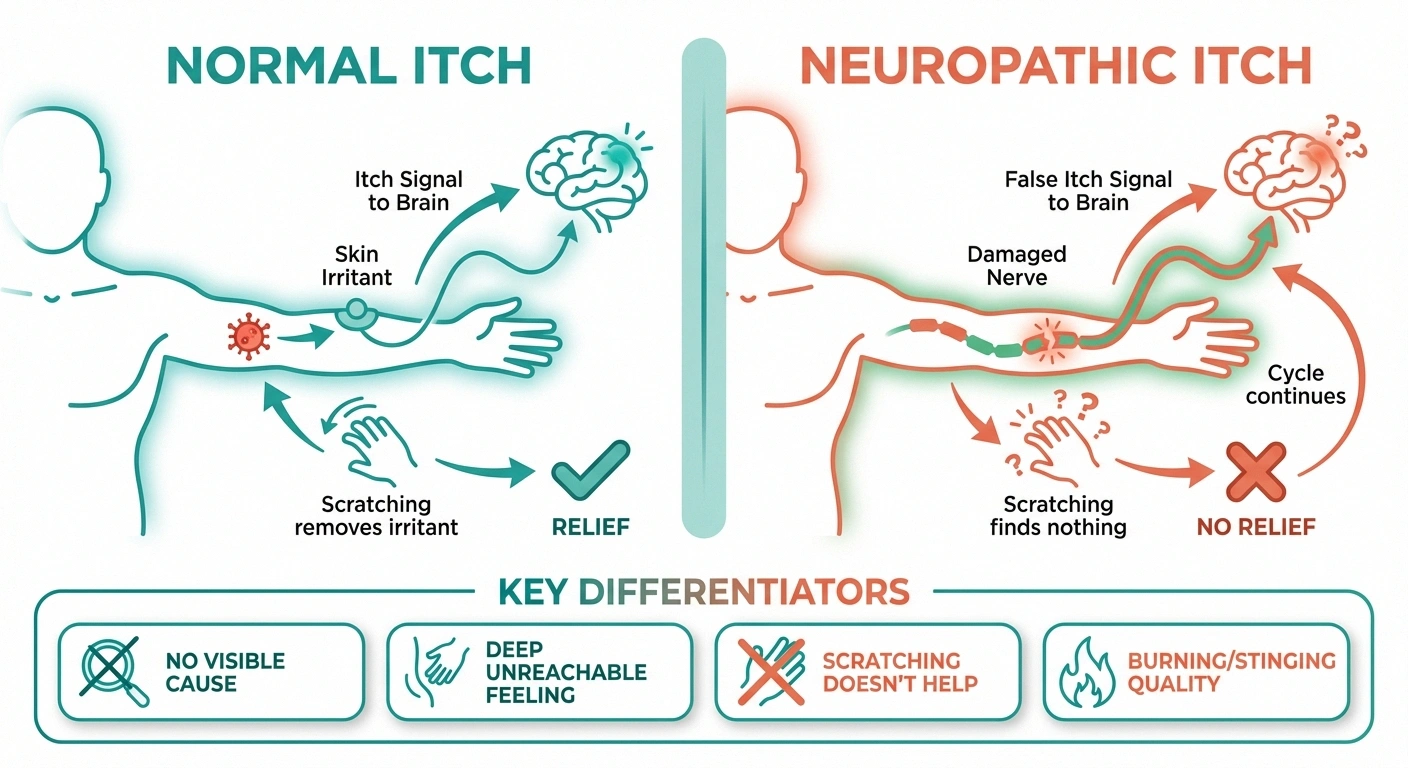
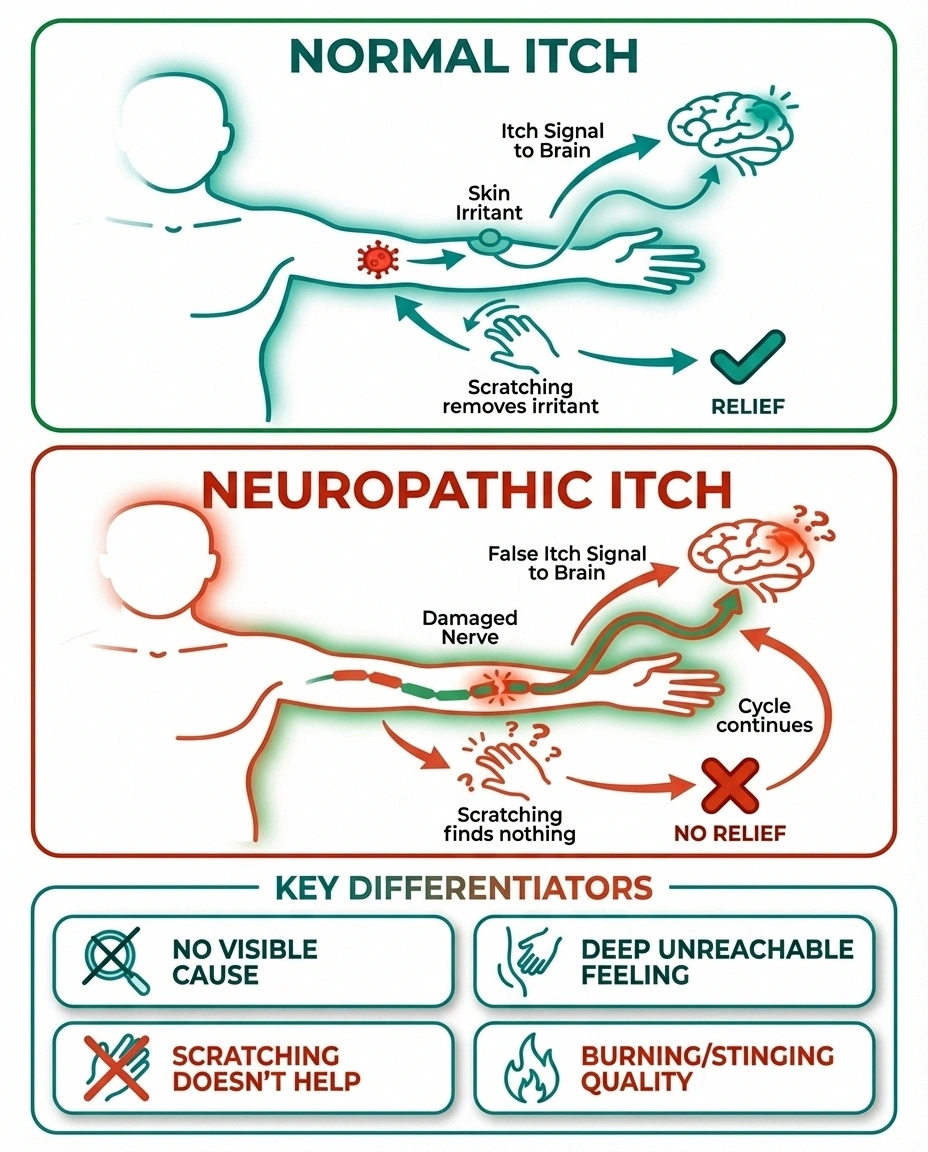
A neuropathic itch is fundamentally different from the kind of itch you get from a mosquito bite, dry skin, or an allergic reaction. Those ordinary itches start at the skin—something irritates it, and nerve endings send an itch signal to your brain. Scratching removes the irritant, and the itch goes away.
of all chronic itch cases are neuropathic — caused by nerve damage, not skin problems
Neuropathic itch starts inside the nervous system itself. Damaged or misfiring nerve fibers send “itch” signals to the brain even when there's absolutely nothing wrong with the skin. Your brain genuinely believes there's something to itch—but there isn't. According to a comprehensive review published in PAIN, neuropathic scalp neuropathy and neuropathic itch is a pathological condition caused by damage within the nervous system that can be severe and unrelenting.
This is why neuropathic itch doesn't respond to the usual treatments. Anti-itch creams, hydrocortisone, and antihistamines target skin-level inflammation and histamine responses—mechanisms that simply aren't involved when the problem originates in the nerves themselves.
How Neuropathic Itch Feels Different
People describe neuropathic itch differently from regular itching. If you recognize these descriptions, it may be worth exploring a neuropathic cause with your doctor:
Could Your Itch Be Neuropathic?
The itch feels deep — like it's under the skin, not on the surface
Your skin looks completely normal in the area that itches
Scratching provides no lasting relief (or makes it worse)
The itch has a burning, stinging, or prickling quality
Anti-itch creams and antihistamines haven't helped
You also have tingling, numbness, or burning in the same area
If you checked 3 or more, discuss the possibility of neuropathic itch with your doctor.
- Deep and unreachable. The itch feels like it's coming from under the skin, not on the surface. No amount of scratching reaches it.
- Burning or stinging quality. Unlike the ticklish sensation of a regular itch, neuropathic itch often has a painful, burning, or prickling edge to it.
- No visible cause. There's no rash, no redness, no dry patch—the skin looks completely normal in the area that itches intensely.
- Scratching doesn't help. In fact, scratching often makes it worse by irritating already-sensitive nerves.
- Localized to specific areas. Neuropathic itch often affects particular spots—one arm, one patch on the back, the feet—rather than generalized itchiness all over.
- Comes with other nerve symptoms. You may also notice tingling, numbness, burning, or pins-and-needles sensations in the same area.
- Persistent or cyclical. It may be constant, or it may come in waves—triggered by heat, stress, or fatigue—but it never fully goes away.
What Causes Neuropathic Itch?
Neuropathic itch can result from damage anywhere along the nervous system—from the peripheral nerves in your hands and feet all the way up through the spinal cord to the brain. According to research published in Frontiers in Medicine, metabolic, neurodegenerative, orthopedic, infectious, autoimmune, and even malignant conditions can trigger neuropathic itch.
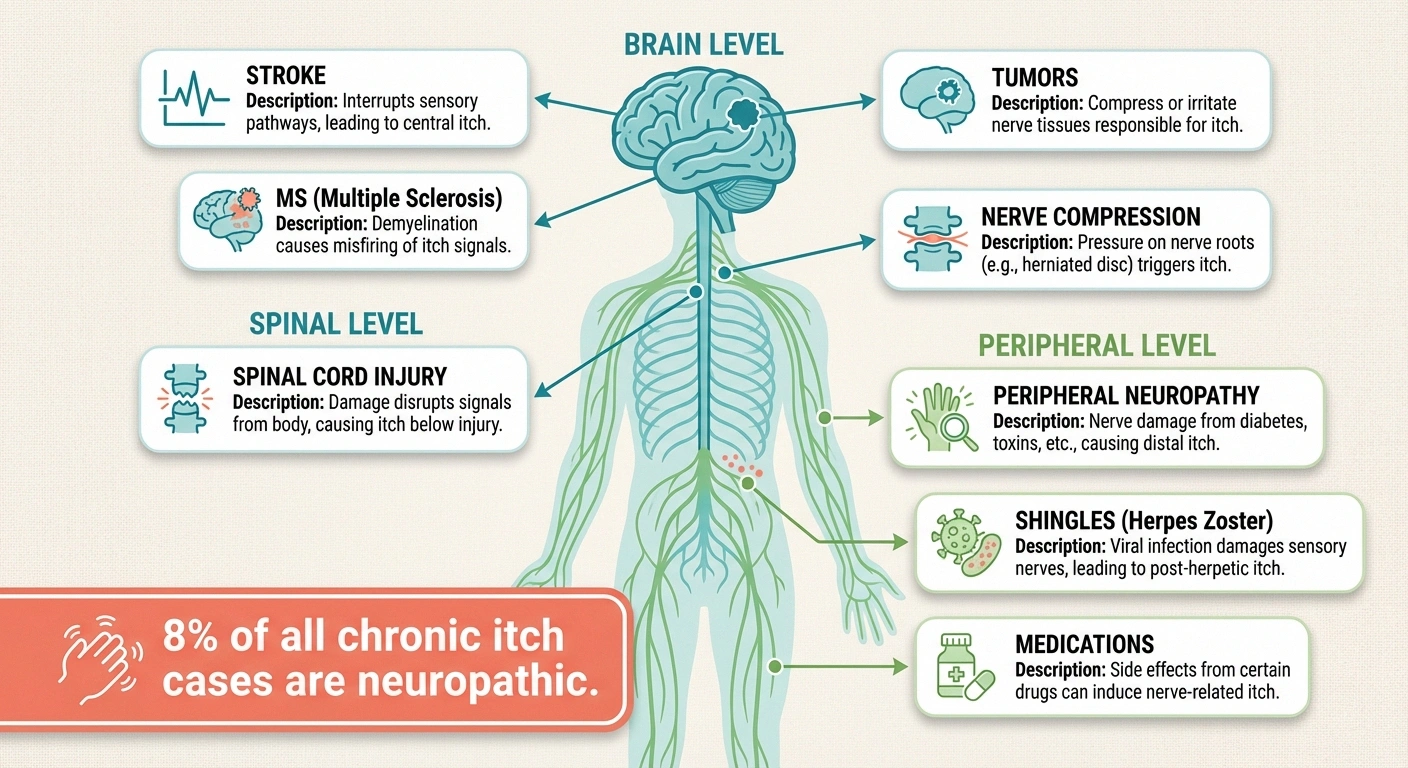
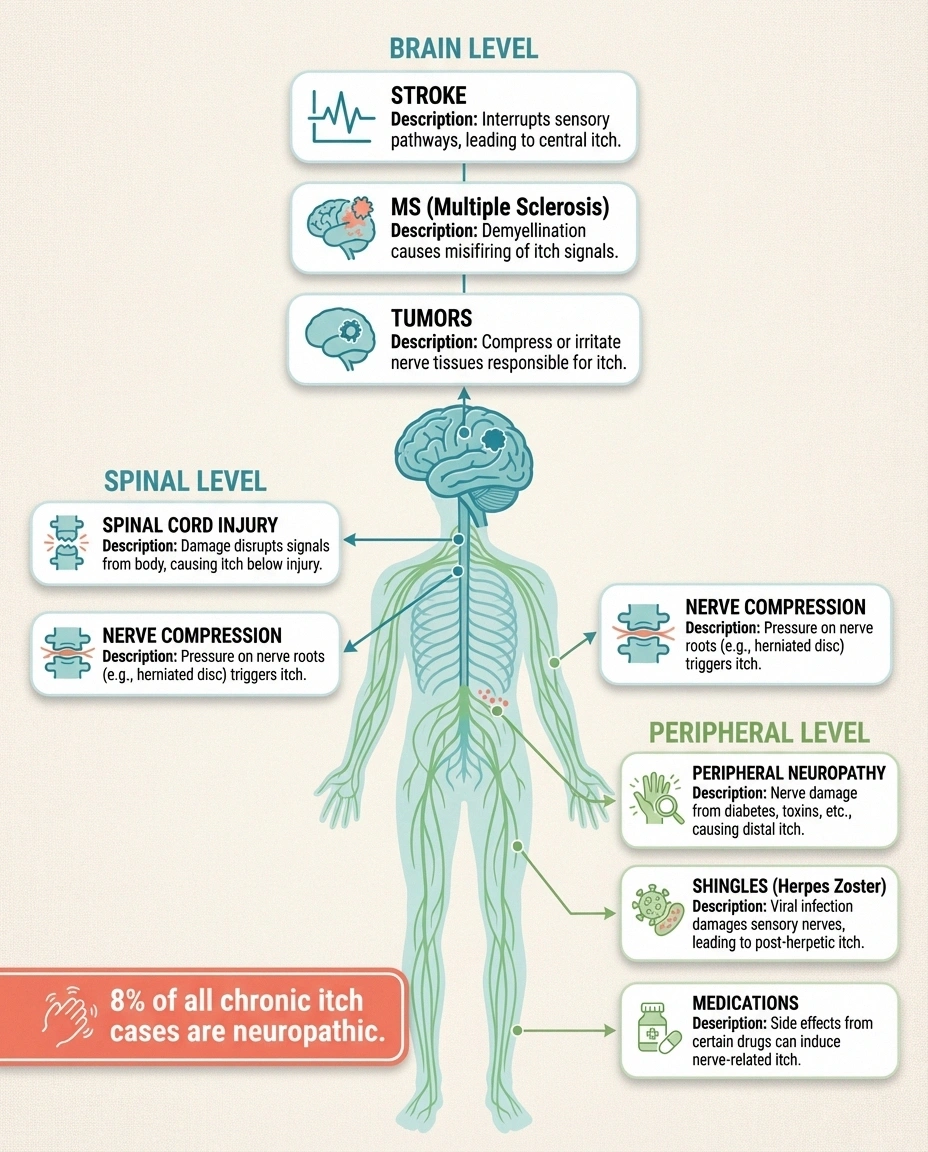
Here are the most common causes:
Peripheral Neuropathy
The same nerve damage that causes burning feet, tingling, and numbness can also produce intense itching—particularly in the hands, feet, and legs. Diabetic neuropathy, chemotherapy-induced neuropathy, and vitamin deficiency neuropathy are all common underlying causes. Many people experience neuropathic itch alongside neuropathic pain, and the itch may actually be worse at night—just like nighttime nerve pain.
Shingles and Post-Herpetic Neuralgia
Even after the shingles rash has healed, the damaged nerves can keep sending itch signals for months or even years. Post-herpetic neuralgia is one of the most common causes of neuropathic itch, and the itching typically affects the same area where the original rash appeared. This lingering itch can be especially intense and resistant to treatment.
Nerve Compression Syndromes
Pinched or irritated nerves can produce neuropathic itch in very specific locations. Two well-documented examples include:
- Brachioradial pruritus: Severe itching on the outer arms, often linked to cervical spine nerve compression. It tends to worsen in warm weather and improve with cold application.
- Notalgia paresthetica: Chronic itching on a specific area of the upper back, usually caused by thoracic nerve irritation. It often creates a darkened patch of skin from repeated scratching over time.
Both conditions highlight how even minor nerve compression can create intense, persistent itching in a very localized area.
Multiple Sclerosis
Multiple sclerosis (MS) disrupts how the brain and spinal cord process sensory information. For some people with MS, itching is one of the earliest unusual sensations they notice—often described as a crawling or electric feeling. These episodes may come and go with MS flare-ups and can be particularly worsened by heat.
Stroke
When a stroke damages areas of the brain involved in processing touch and sensation, the brain may misinterpret normal sensory input as itching. This “central” neuropathic itch typically occurs on the side of the body opposite to where the stroke occurred in the brain.
Spinal Cord Injury
Injuries to the spinal cord can scramble sensory signals, creating persistent itch in areas below the injury site. This type of neuropathic itch can be among the most challenging to treat because the damage is in the central nervous system itself.
Medications
Some medications—including certain antidepressants, chemotherapy drugs, and opioid pain medications—can affect how nerves process signals and trigger itching as a side effect. If itching started or worsened after beginning a new medication, discuss this with your prescribing doctor.
Why Scratching Makes It Worse
With regular itching, scratching provides relief because it interrupts the itch signal at the skin level. But with neuropathic itch, the signal isn't coming from the skin—it's coming from malfunctioning nerves. Scratching the area provides only fleeting relief (if any) and then typically intensifies the itch by further irritating the already-sensitive nerve endings.

Protect Your Skin
If you scratch in your sleep, keep fingernails trimmed very short and wear cotton gloves at night. Open wounds from scratching can lead to infections and scarring. If you wake up with unexplained skin damage, talk to your doctor about protective measures.
This creates a vicious cycle: itch → scratch → temporary relief → worse itch → more scratching → skin damage. Over time, aggressive scratching can lead to:
- Open wounds and skin breakdown
- Secondary infections from bacteria entering broken skin
- Scarring and permanent skin changes
- In severe cases, self-injury deep enough to require medical attention
Some people scratch so intensely during sleep that they wake up with bloody skin or scabs without any conscious memory of scratching. If this happens to you, protective measures like wearing gloves at night or covering the affected area become important safety steps.
Getting the Right Diagnosis
One of the biggest challenges with neuropathic itch is that it's frequently misdiagnosed as a skin condition. Many people cycle through dermatologists, try countless anti-itch creams, and undergo allergy testing—all without relief—before someone considers a neurological cause.
According to research published in Frontiers in Medicine, doctors may perform skin biopsies when the cause of persistent itching is unknown. This can help rule out dermatological causes and may reveal reduced nerve fiber density in the affected area—a hallmark of neuropathic itch.
You can help your doctor reach the right diagnosis by documenting:
- When the itch started and whether it coincided with any other health events
- Exactly where it occurs (specific body locations)
- Whether the skin looks normal in the itching area
- What you've already tried and whether it helped
- Whether you have any other nerve-related symptoms (tingling, numbness, burning, pain)
- Your medical history, including diabetes, shingles, spinal conditions, or neurological conditions
If your primary care doctor or dermatologist has ruled out skin causes but the itch persists, ask for a referral to a neurologist. Nerve conduction studies and a thorough neurological exam can help identify the underlying nerve damage responsible for the itch.
Treatment Options That Actually Work
Treating neuropathic itch requires a different approach than treating regular itching. Since the problem starts in the nerves, treatments need to target nerve function rather than skin inflammation. Here's what has shown benefit:
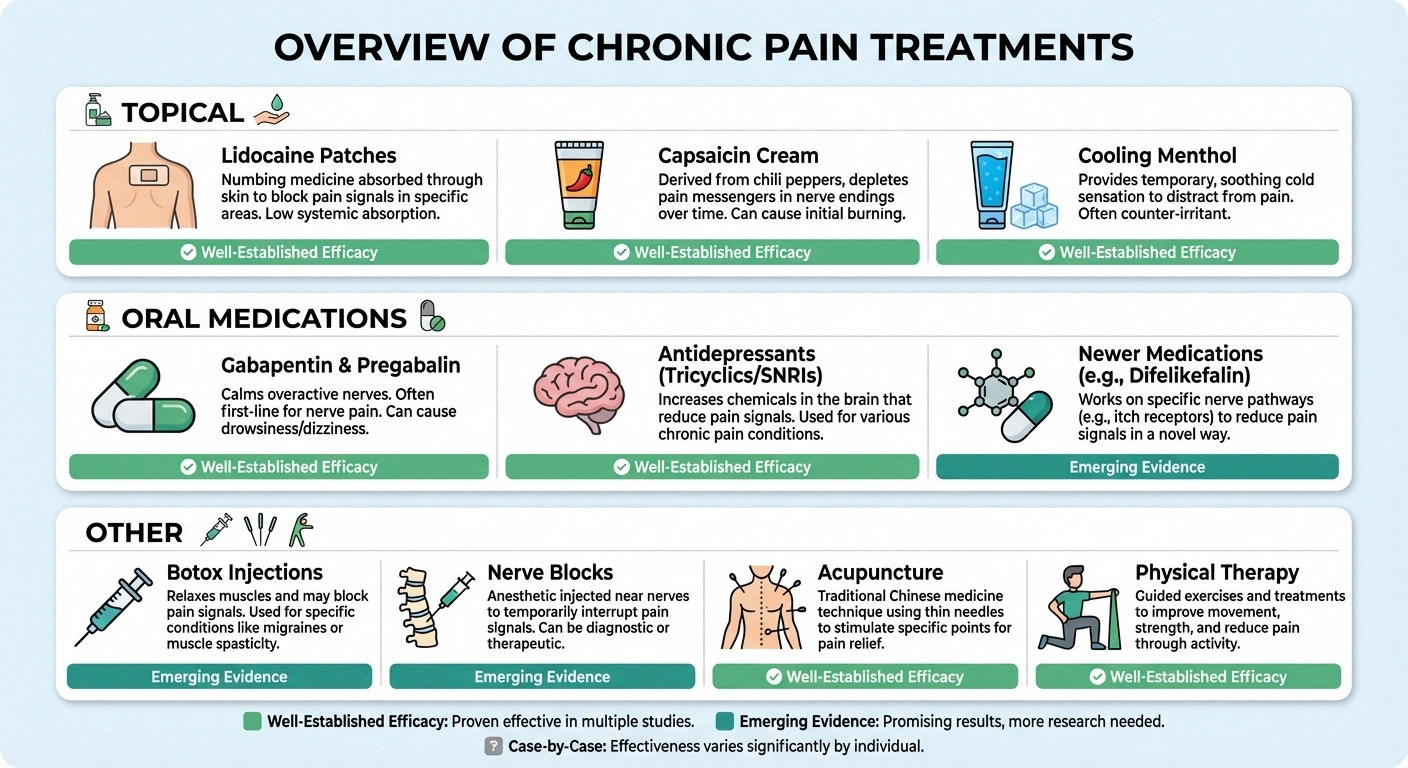
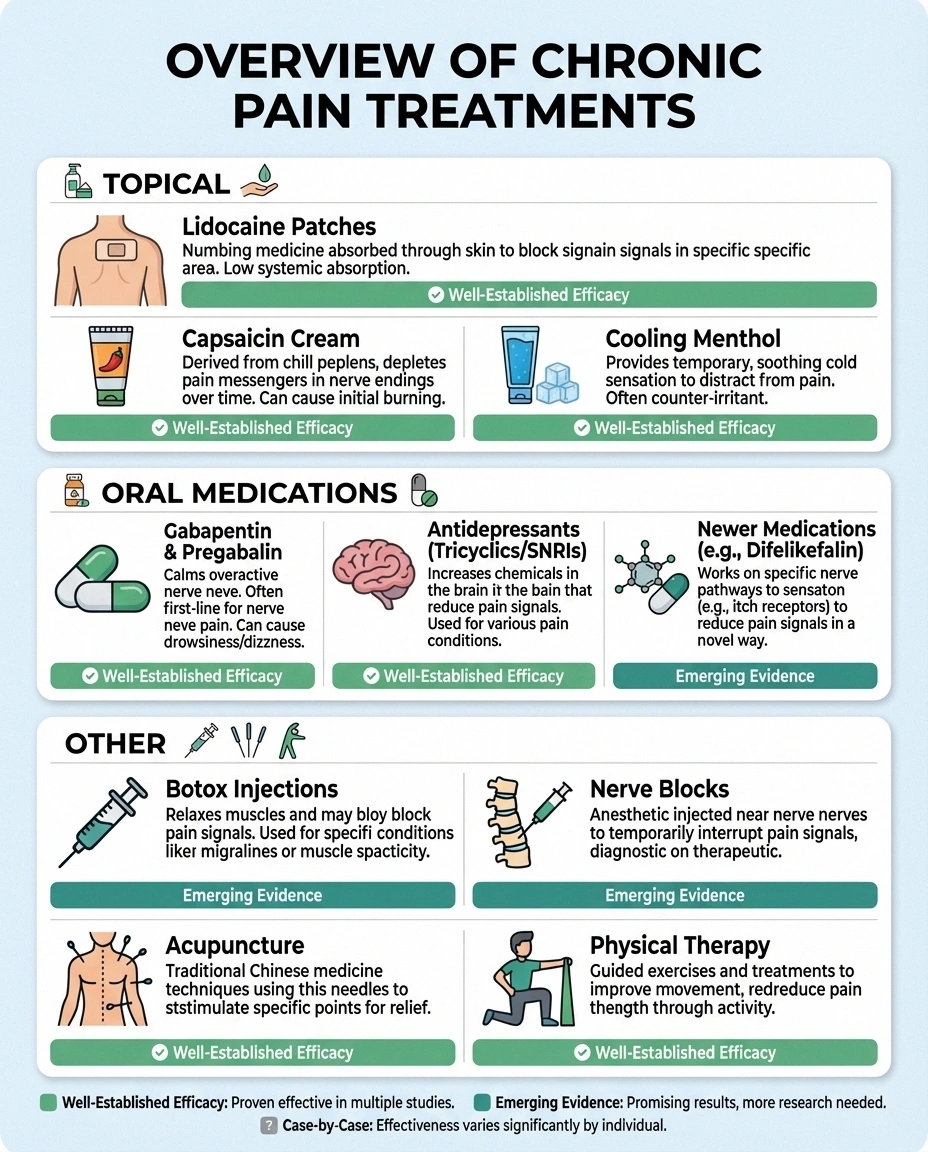
Research Says
Unlike regular itch (mediated by histamine), neuropathic itch has its own distinct pathway in the nervous system. This is why antihistamines don't work — and why medications like gabapentin and capsaicin, which target nerve signaling, are more effective for this type of itch.
Topical Treatments
- Lidocaine patches or cream: Local anesthetics can numb the affected area and reduce itch signals. These are often a first-line treatment because they have few systemic side effects.
- Capsaicin cream: Made from chili peppers, capsaicin works by depleting substance P—a neurotransmitter involved in both pain and itch signaling. It burns at first (sometimes significantly), but consistent use over several weeks can provide lasting relief. Some dermatologists note that capsaicin may cause permanent changes to nerve fibers that reduce itch long-term.
- Cooling agents: Menthol-based creams and lotions can temporarily reduce itch by activating cold-sensing nerves, which may compete with and override itch signals.
Oral Medications
- Gabapentin and pregabalin: These anti-seizure medications are the workhorses of neuropathic symptom treatment. By calming overactive nerve signals, they can reduce both neuropathic pain and itch. An important study in Brain confirmed their effectiveness for neuropathic itch.
- Certain antidepressants: Tricyclic antidepressants like amitriptyline and SNRIs like duloxetine can help by modifying how the nervous system processes both pain and itch signals.
- Difelikefalin: This newer medication, which works on kappa opioid receptors, has shown promise in clinical trials for specific forms of neuropathic itch like notalgia paresthetica.
Other Treatments
- Botox injections: In some cases, botulinum toxin injections in the affected area have provided significant relief from neuropathic itch.
- Nerve blocks: Targeted anesthetic injections near the affected nerves can provide temporary but sometimes dramatic relief.
- Acupuncture: Some patients report improvement with acupuncture, which may work by modifying nerve signaling pathways.
- neuropathy physical therapy exercises: For nerve compression-related itch (like notalgia paresthetica), strengthening and stretching exercises can help realign the spine and reduce nerve irritation.
Home Strategies for Managing the Itch
While medical treatment addresses the underlying nerve dysfunction, these daily strategies can help you cope between appointments and reduce the impact on your quality of life:

Quick Relief Tip
Cold is your best friend for neuropathic itch. Cold compresses and menthol-containing creams decrease nerve excitability and may activate cold-sensing nerves that compete with itch signals. Keep a gel pack in the refrigerator for quick access during flare-ups.
Cold is your friend. Cold compresses, cooling gel packs, or even running cold water over the affected area can provide significant temporary relief. Cold decreases nerve excitability and may activate cold-sensing nerves that compete with itch signals. Keep a gel pack in the refrigerator for quick access during flare-ups.
Protect your skin from scratching. Keep fingernails trimmed very short. Wear cotton gloves at night if you scratch in your sleep. Cover vulnerable areas with soft bandages or long sleeves. These aren't elegant solutions, but they prevent the skin damage that makes everything worse.
Avoid heat. Warm or hot temperatures can dramatically worsen neuropathic itch. Take lukewarm (not hot) showers, avoid saunas and hot tubs, and be mindful of how heat affects your symptoms during summer months.
Keep skin moisturized. While dry skin isn't causing your neuropathic itch, dry and irritated skin can amplify the sensation. Regular moisturizing with a gentle, fragrance-free lotion helps keep the skin barrier intact.
Wear loose, soft clothing. Tight clothing and rough fabrics can irritate sensitive nerve endings and trigger itching episodes. Cotton and bamboo fabrics tend to be the most comfortable against irritated skin.
Practice distraction and mindfulness. This might sound dismissive, but it isn't—the itch signal is being generated by your nervous system, and techniques like deep breathing, meditation, and focused distraction genuinely can reduce how intensely your brain perceives the itch. Cognitive behavioral therapy (CBT) has shown benefit for chronic itch management.
The Emotional Toll
We need to talk about something that doesn't appear in most medical articles: the psychological impact of chronic, unrelenting itch. It's real, it's significant, and if you're experiencing it, your frustration is completely justified.

Neuropathic itch can:
- Destroy your sleep. The itch often intensifies at night, making it difficult to fall asleep and easy to be woken up by the urge to scratch.
- Erode your mood. Constant, unrelieved itching leads to frustration, irritability, anxiety, and depression. This is a normal response to a genuinely distressing symptom.
- Create social embarrassment. Visible scratching, skin damage, or wearing protective coverings can make you self-conscious in social situations.
- Feel dismissive when misunderstood. “It's just an itch” is something people say when they've never experienced this kind of itch. The dismissal from others—sometimes even from healthcare providers—adds to the emotional burden.
If the emotional impact of chronic itch is affecting your quality of life, consider joining a neuropathy support group where others understand what you're going through. Speaking with a therapist who specializes in chronic pain or chronic illness can also provide meaningful coping strategies. You can read more about the emotional side of neuropathy in our article on neuropathy and mental health.
How Long Does Neuropathic Itch Last?
The duration depends entirely on the underlying cause:
- Shingles-related: May resolve within weeks to months, but can persist for years in post-herpetic neuralgia
- Medication-related: May stop once the medication is changed or discontinued
- Nerve compression: Physical therapy or targeted injections may bring relief within months
- Stroke or spinal cord injury: May persist longer-term, sometimes for years, though it often improves gradually
- Peripheral neuropathy: Tends to follow the course of the underlying neuropathy—managing the root cause (blood sugar control, B12 supplementation, etc.) can improve the itch over time
Neuropathic itch can be cyclical, with periods of improvement followed by flare-ups triggered by stress, heat, fatigue, or illness. Managing triggers and maintaining treatment consistency gives you the best chance of keeping it under control.
Frequently Asked Questions
How do I know if my itch is neuropathic or just dry skin?
Key differences include the absence of any visible skin problem in the itchy area, the itch feeling deep rather than surface-level, scratching providing no lasting relief, and the itch being accompanied by other nerve symptoms like tingling or burning. If moisturizers and anti-itch creams haven't helped after several weeks, a neurological cause is worth investigating with your doctor.
Can neuropathic itch be dangerous?
The itch itself is not dangerous, but the scratching it provokes can be. Aggressive scratching can break the skin, leading to wounds, infections, and scarring. In severe cases, some people scratch deeply enough to cause significant self-injury, especially during sleep when they are not consciously aware of scratching. Protective measures like keeping nails short and wearing gloves at night are important safety steps.

Do antihistamines work for neuropathic itch?
Generally not. Antihistamines like diphenhydramine (Benadryl) work by blocking histamine, which is involved in allergic and inflammatory itching. Neuropathic itch is caused by nerve damage rather than histamine release, so antihistamines typically provide little to no relief. Medications that target nerve signaling, such as gabapentin or pregabalin, are more appropriate for neuropathic itch.
Is neuropathic itch the same as neurodermatitis?
No, they are different conditions. Neurodermatitis (lichen simplex chronicus) involves an itch-scratch cycle that leads to thickened, leathery skin patches. While nerves play a role in neurodermatitis, the condition involves significant skin changes. Neuropathic itch originates purely from nerve damage and the skin typically appears normal in the affected area, at least initially, before any scratching damage occurs.
Can stress cause neuropathic itch?
Stress doesn't cause neuropathic itch directly, but it is one of the most common triggers for flare-ups. Stress activates the sympathetic nervous system, which can amplify nerve signals including itch. Many people with neuropathic itch notice a clear pattern between stressful periods and worsened symptoms. Stress management techniques like deep breathing, meditation, and regular exercise can help reduce the frequency and intensity of itch flare-ups.
Should I see a dermatologist or neurologist for neuropathic itch?
Ideally, both. Start with a dermatologist to rule out skin-related causes of itching. If the dermatologist cannot find a skin condition causing the itch, ask for a referral to a neurologist. Some cases benefit from both specialists working together, especially when there are both skin changes from chronic scratching and underlying nerve damage driving the itch.
You Deserve to Be Heard
If you've been dealing with an itch that won't respond to any cream, any lotion, any remedy you've tried—please know that this is a real, recognized medical symptom with real treatment options. You're not being overly dramatic. Your nerves are literally misfiring.
The path to relief often starts with getting the right diagnosis, which means talking to the right doctors and providing them with the specific information they need. Document your symptoms, note what makes them better or worse, and advocate for yourself if you feel your concerns aren't being taken seriously.
Neuropathic itch may be less well-known than neuropathic pain, but it's every bit as real and every bit as treatable. Don't give up on finding something that works for you.
For more information on understanding and managing neuropathy symptoms, explore our guides to the stages of neuropathy, neuropathy diagnosis and testing, and natural remedies for nerve pain.


