
When my doctor first mentioned that my vitamin D levels might be contributing to my nerve pain, I was skeptical. Vitamin D? The sunshine vitamin? How could that have anything to do with the burning in my feet? But as I dug into the research — and then watched my own symptoms shift after supplementation — I realized this connection deserves far more attention than it gets.
Vitamin D deficiency is remarkably common, affecting an estimated one billion people worldwide. And emerging research suggests it may play a far more significant role in nerve health than we once understood. For people living with neuropathy — especially diabetic neuropathy — this is a connection worth exploring with your healthcare provider.
How Vitamin D Supports Your Nervous System
Most people associate vitamin D with strong bones. But researchers have discovered that vitamin D receptors are found throughout the nervous system, including in the peripheral nerves — the very nerves affected by neuropathy. These receptors bind with calcitriol, the active form of vitamin D, to influence several critical processes for nerve health:
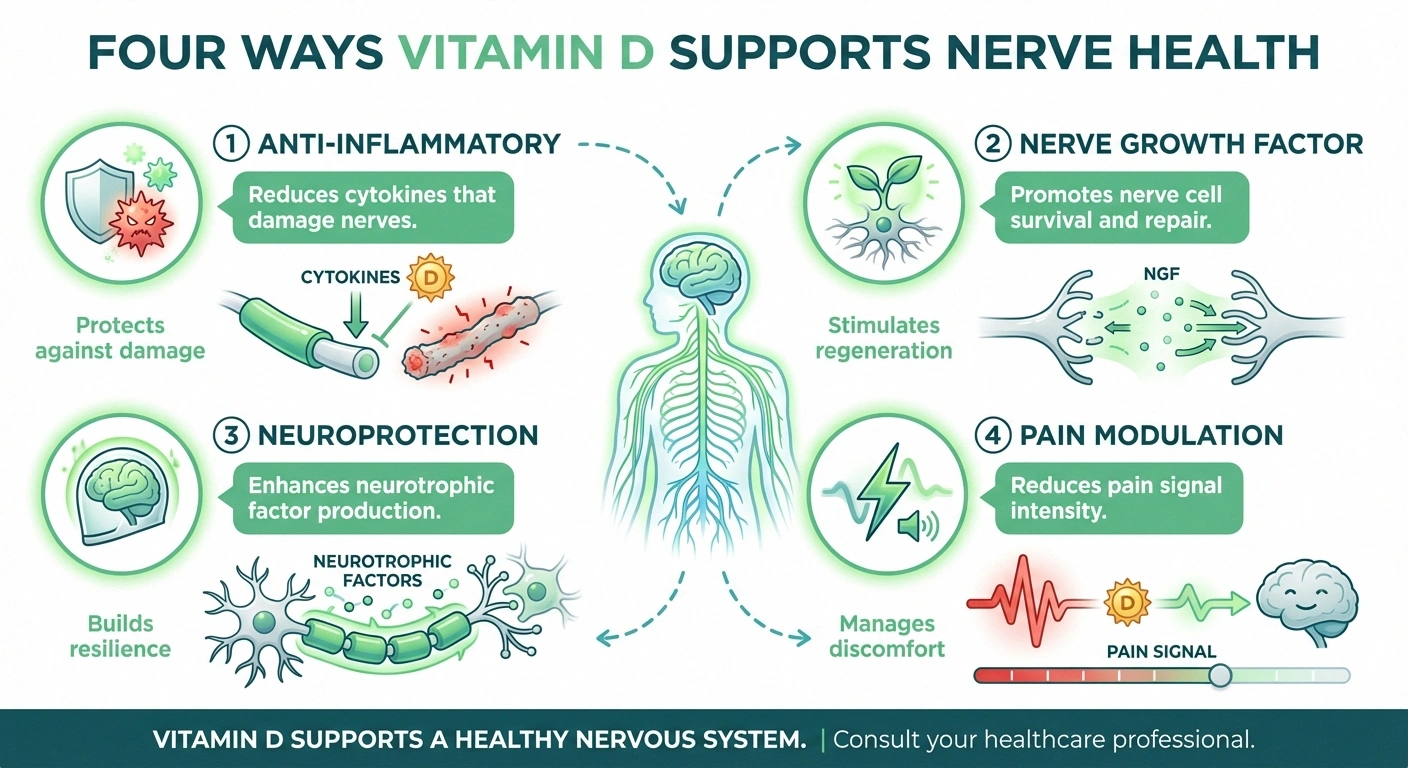
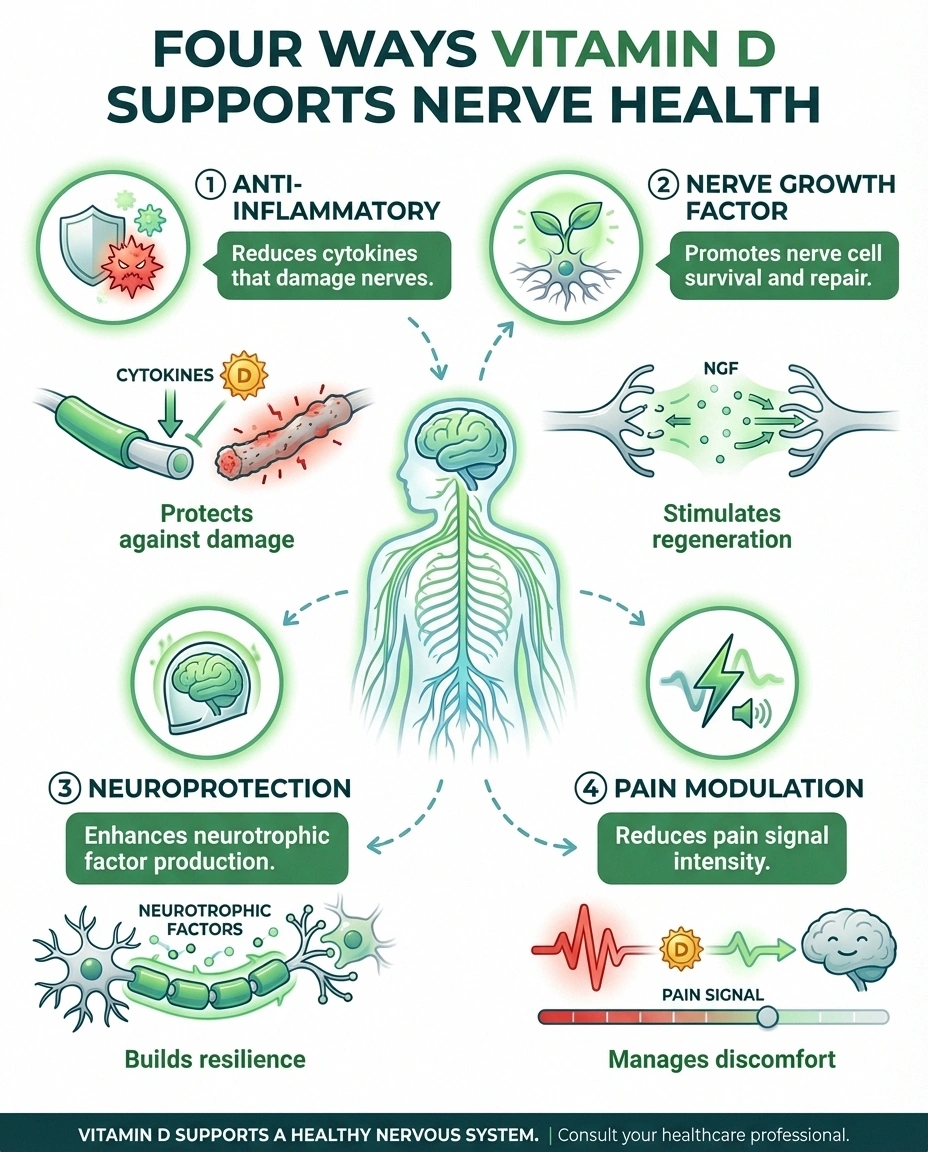
people worldwide are estimated to have vitamin D deficiency — a modifiable risk factor for neuropathy
Anti-inflammatory protection: Chronic inflammation is one of the primary drivers of nerve damage in many types of neuropathy. Vitamin D modulates the immune response and reduces the release of pro-inflammatory molecules called cytokines. By keeping inflammation in check, adequate vitamin D levels may help protect nerves from ongoing damage and slow the progression of neuropathy.
Nerve growth factor production: Research published in the Journal of Pain Research shows that vitamin D supplementation increases nerve growth factor (NGF), a protein essential for the survival, growth, and maintenance of nerve cells. NGF promotes nerve regeneration and repair — exactly what damaged peripheral nerves need.
Neuroprotective effects: Beyond reducing inflammation and supporting nerve growth, vitamin D enhances the production of neurotrophic factors — specialized proteins that help nerve cells survive and function properly. These protective effects may explain why people with adequate vitamin D levels tend to have better nerve function and fewer neuropathy symptoms.
Pain modulation: The vitamin D receptors present in nerve tissue may directly influence how pain signals are transmitted and perceived. Several studies suggest that correcting vitamin D deficiency can reduce the intensity and frequency of neuropathic pain, making it a potentially valuable addition to pain management strategies.
The Vitamin D–Neuropathy Link: What the Research Shows
Let me walk you through what the science actually says — including where the evidence is strong and where questions remain.


Key Research Finding
Each 1 ng/mL increase in serum vitamin D is correlated with a 2.2% decrease in the presence and a 3.4% decrease in the severity of nerve conduction velocity impairment. Higher vitamin D levels = better nerve function.
The diabetic neuropathy connection is well-established: Multiple large studies have found a clear association between low vitamin D levels and diabetic peripheral neuropathy. A 2012 study of 210 patients with type 2 diabetes found that those with peripheral neuropathy had significantly lower mean vitamin D levels than those without it — and concluded that vitamin D deficiency is an independent risk factor for diabetic neuropathy. This finding has been confirmed by the NHANES survey, studies from Shanghai, Sheffield, Liverpool, and a 2021 meta-analysis of over 6,000 participants.
Supplementation shows promise: A study published in BMJ Open Diabetes Research & Care found that a single high-dose vitamin D treatment in patients with painful diabetic neuropathy led to significant decreases in pain symptoms. A case report in The Permanente Journal documented a patient whose neuropathy symptoms — including pain, numbness, and paresthesia — improved “tremendously” after vitamin D supplementation. And a systematic review concluded that vitamin D supplementation could be an added value in treating painful peripheral diabetic neuropathy.
The relationship is dose-dependent: An analysis of the data found that each 1 ng/mL increase in serum vitamin D was correlated with a 2.2% decrease in the presence and a 3.4% decrease in the severity of nerve conduction velocity impairment. In other words, the more you raise your vitamin D levels (within the healthy range), the more your nerve function may improve.
But some studies show limitations: A study of Egyptian prediabetic individuals found that while vitamin D supplementation improved peripheral neuropathy, the correlation between vitamin D levels and neuropathy severity wasn't statistically significant. And a recent study found no correlation between vitamin D levels and the severity of idiopathic peripheral neuropathy. This suggests that vitamin D's impact may be strongest in people with diabetes or specific deficiencies, rather than being a universal neuropathy treatment.
Are You at Risk for Vitamin D Deficiency?
Understanding your risk factors for vitamin D deficiency is the first step toward knowing whether this might be contributing to your neuropathy symptoms. Several groups are at higher risk:
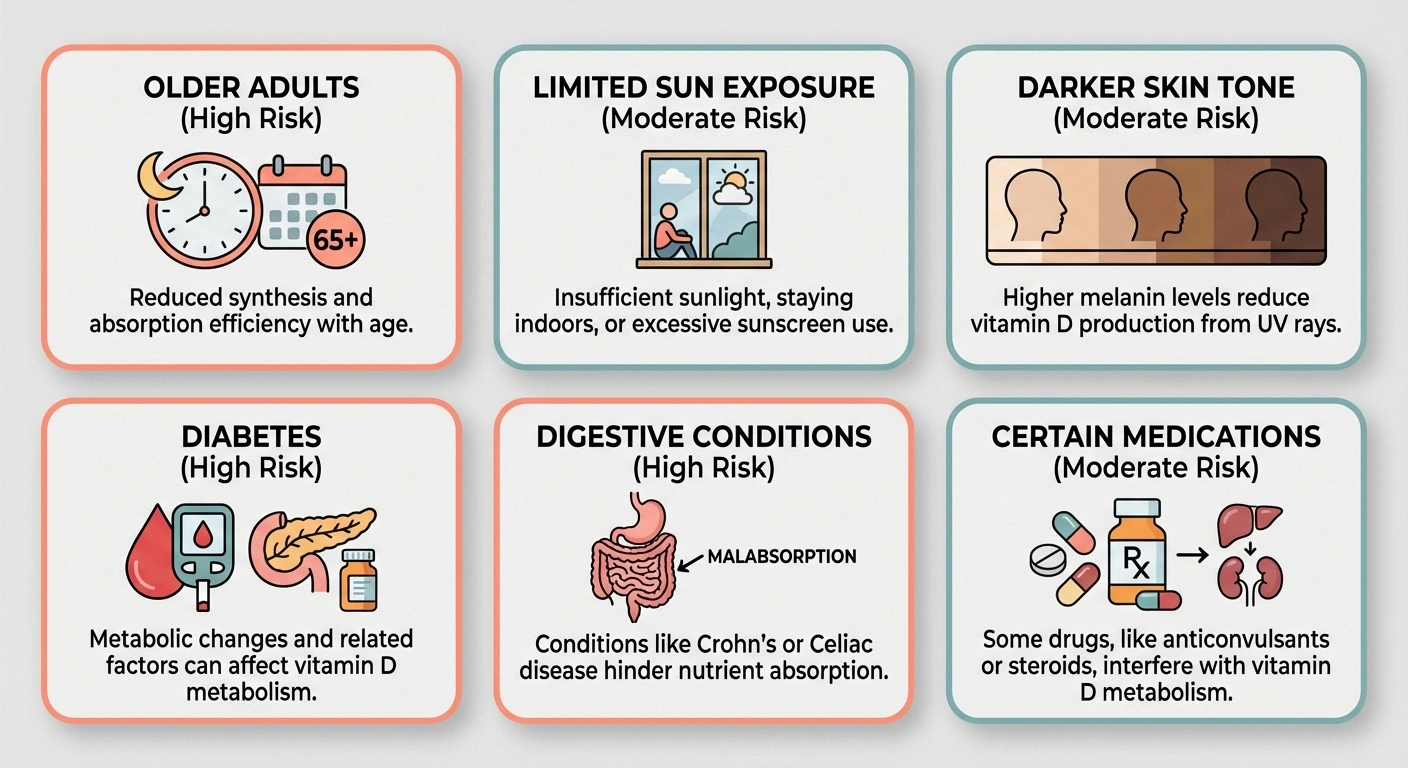
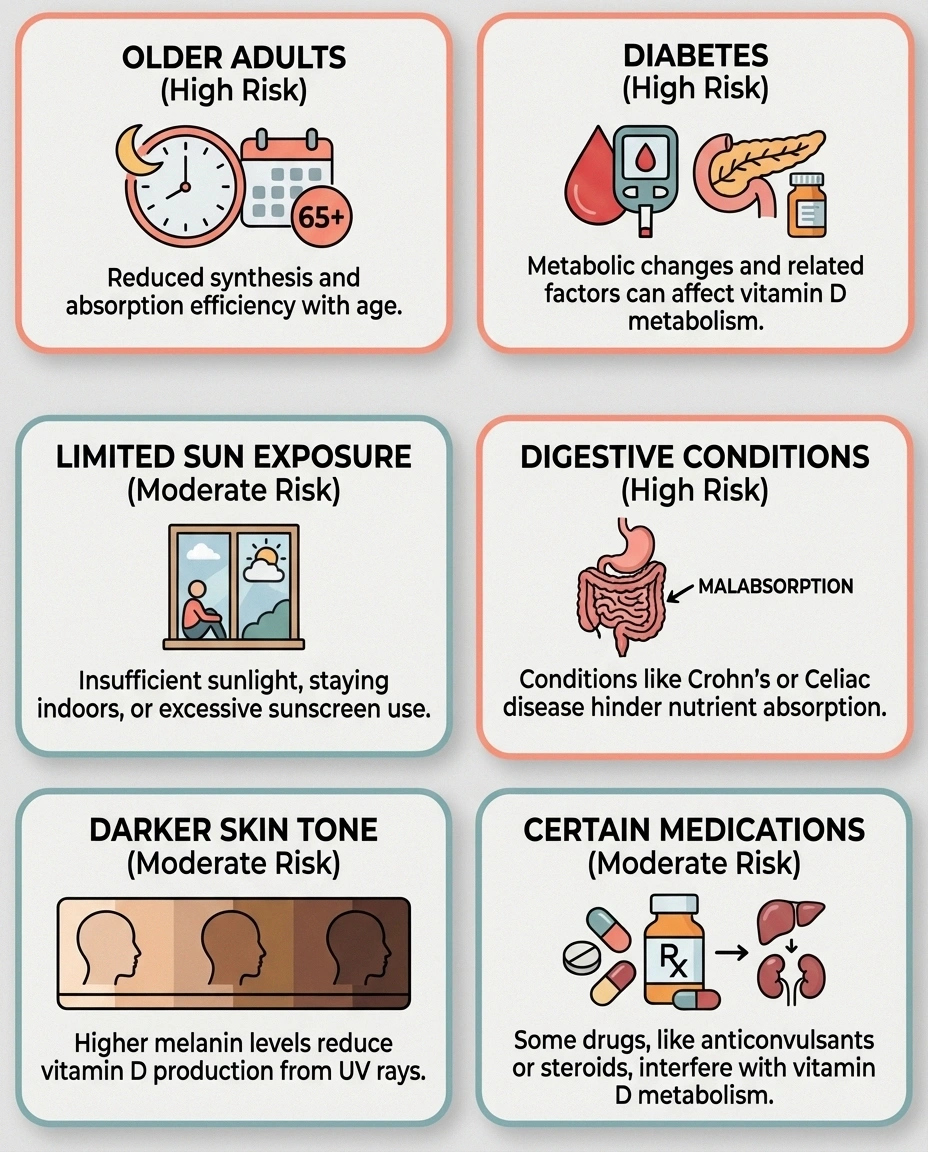
Older adults: As we age, our skin becomes less efficient at producing vitamin D from sunlight, and our kidneys become less effective at converting it to its active form. People over 65 are at significantly higher risk of deficiency — and this is also the age group most affected by peripheral neuropathy.
People with limited sun exposure: If you live in northern latitudes (above the 37th parallel — roughly north of Atlanta or Los Angeles), spend most of your time indoors, or consistently use sunscreen, your body may not produce enough vitamin D from sunlight alone. Winter months are particularly problematic in these regions.
People with darker skin: Higher levels of melanin reduce the skin's ability to produce vitamin D from sunlight. Studies show that vitamin D deficiency rates are significantly higher in Black and Hispanic populations.
People with diabetes: Metabolic changes associated with diabetes can affect vitamin D metabolism and utilization. Given the strong link between vitamin D deficiency and diabetic neuropathy, testing is especially important for people with diabetes.
People with digestive conditions: Celiac disease, Crohn's disease, and other conditions that affect fat absorption can impair vitamin D uptake, since vitamin D is fat-soluble. Gastric bypass surgery can also reduce absorption.
Those taking certain medications: Some medications — including certain anti-seizure drugs, glucocorticoids, and cholestyramine — can interfere with vitamin D metabolism.
Getting Tested: Know Your Numbers
The only reliable way to know your vitamin D status is through a blood test called the 25-hydroxyvitamin D test (also written as 25(OH)D). This is a routine blood draw that your doctor can order alongside other tests.
Your Vitamin D Level Guide
Below 20 ng/mL — Deficient
Supplementation strongly recommended. Associated with increased neuropathy risk.
20–29 ng/mL — Insufficient
Borderline low. Supplementation may improve neuropathy symptoms.
30–50 ng/mL — Sufficient ✓
Target range. Best balance of nerve health benefits without toxicity risk.
Above 100 ng/mL — Caution
Potentially harmful. Can cause calcium buildup. Medical monitoring required.
Test: 25-hydroxyvitamin D blood test — ask your doctor at your next visit
Here's how to interpret your results:
Deficient: Below 20 ng/mL (50 nmol/L) — Your levels are too low and supplementation is strongly recommended. This level is associated with increased neuropathy risk in people with diabetes.
Insufficient: 20–29 ng/mL (50–72 nmol/L) — Borderline low. Supplementation may improve symptoms and is worth discussing with your doctor.
Sufficient: 30–50 ng/mL (75–125 nmol/L) — This is the target range for most people. Research suggests this range provides the best balance of nerve health benefits without toxicity risk.
Potentially harmful: Above 100 ng/mL (250 nmol/L) — Excessive vitamin D can cause calcium buildup and other complications. This is why testing and medical guidance matter.
If you have neuropathy and haven't had your vitamin D tested, ask your doctor. It's a simple, inexpensive test that could reveal a very treatable factor in your nerve health.
Vitamin D Supplementation: A Practical Guide
If testing reveals low vitamin D levels, here's what you should know about supplementation:
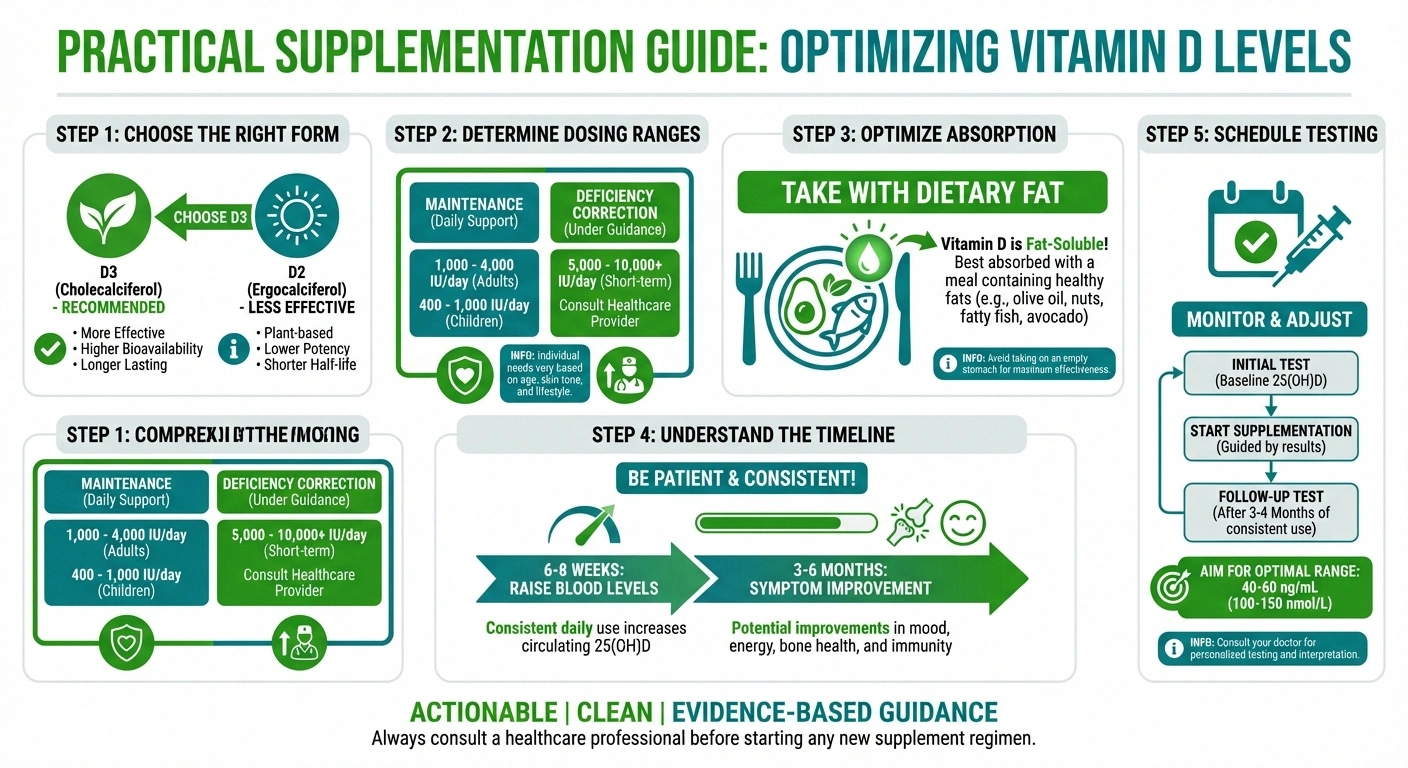
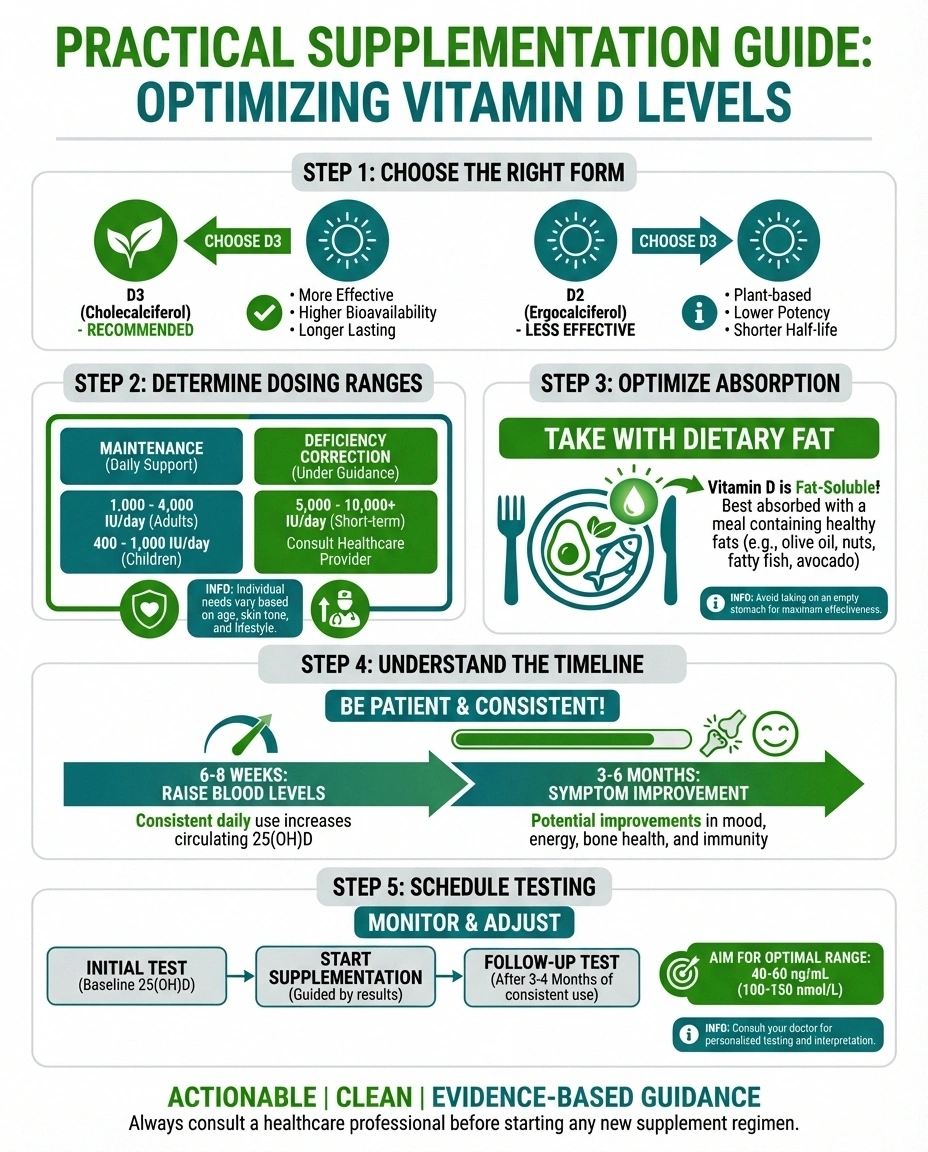
Absorption Tip
Take vitamin D with your largest meal of the day. As a fat-soluble vitamin, it absorbs significantly better when consumed with vitamin D-rich meals for nerves fat. Studies show this simple change can increase absorption by up to 50%.
Vitamin D3 vs. D2: Vitamin D3 (cholecalciferol) is generally preferred over D2 (ergocalciferol). D3 is the form your body naturally produces from sunlight, and research suggests it's more effective at raising and maintaining blood levels. Most over-the-counter supplements are D3.
Typical dosing: For maintenance, most experts recommend 1,000–2,000 IU daily for adults. For people with documented deficiency, doctors often prescribe higher loading doses — sometimes 5,000 IU daily or weekly high-dose prescriptions of 50,000 IU. The studies showing neuropathy improvement in diabetic patients used doses ranging from 2,000 to 5,000 IU daily. Your doctor will determine the right dose based on your blood levels.
Take it with fat: Vitamin D is fat-soluble, meaning it absorbs best when taken with a meal that contains some fat. A simple strategy: take your vitamin D supplement with your largest meal of the day.
Timeline for results: Don't expect overnight improvement. It typically takes six to eight weeks of consistent supplementation to significantly raise blood levels, and neuropathy symptoms may take three to six months to respond. The BMJ study that showed significant pain reduction followed patients over 20 weeks. Patience is part of the process.
Regular monitoring: Once you start supplementation, your doctor should recheck your levels after about three months to ensure you're reaching the target range without overshooting. Annual testing is generally sufficient after you've established a stable dose.
Food Sources of Vitamin D
While supplementation is often necessary to correct deficiency, incorporating vitamin D-rich foods into your neuropathy-friendly diet provides additional benefits and supports overall nerve health:

Best natural sources: Fatty fish lead the list — salmon, mackerel, sardines, and trout contain significant amounts of vitamin D. A 3-ounce serving of wild-caught salmon provides roughly 570 IU, nearly the entire daily recommended amount for most adults. Cod liver oil is another potent source, providing about 1,360 IU per tablespoon.
Other dietary sources: Egg yolks (about 40 IU each), beef liver, and certain mushrooms that have been exposed to UV light contribute smaller amounts. However, it's difficult to meet your vitamin D needs through these foods alone.
Fortified foods: Many common foods are fortified with vitamin D, including milk (about 120 IU per cup), orange juice, cereals, and yogurt. These can help boost your daily intake but rarely provide enough to correct a deficiency on their own.
Practical tip: A combination approach works best. Aim for two to three servings of fatty fish per week (which also provides anti-inflammatory omega-3 fatty acids — a bonus for nerve health), include fortified foods in your daily routine, and supplement as directed by your doctor. This three-pronged approach gives your nerves the best vitamin D support.
The Sunshine Factor: Safe Sun Exposure
Your body produces vitamin D when UVB rays from sunlight hit your skin — but getting enough sun without increasing skin cancer risk requires balance:

☀️ Fair Skin
10–15 minutes midday sun, 2–3× per week on arms and legs. No sunscreen during this brief window.
☀️ Medium Skin
20–30 minutes midday sun, 3× per week. May need supplementation year-round in northern climates.
☀️ Dark Skin
30–45 minutes midday sun, 3–4× per week. Supplementation recommended year-round, especially in northern latitudes.
Nov–Feb above 37th parallel: UVB too low for vitamin D production — rely on diet + supplements
How much sun you need: For most fair-skinned people, 10 to 15 minutes of midday sun exposure on the arms and legs, two to three times per week, may produce adequate vitamin D. People with darker skin may need three to five times longer. However, this varies enormously based on latitude, season, cloud cover, and skin type.
Winter challenges: If you live above the 37th parallel, the sun's angle during winter months (roughly November through February) is too low for your skin to produce meaningful vitamin D, regardless of how much time you spend outside. This is when supplementation becomes particularly important.
Safety first: The goal isn't to get sunburned — excessive UV exposure increases skin cancer risk. Brief, regular exposure is better than occasional long sessions. If you have a history of skin cancer or are at high risk, rely on diet and supplements rather than sun exposure for your vitamin D needs.
Vitamin D and Other Neuropathy Supplements
Vitamin D works best as part of a broader nutritional strategy for nerve health. Here's how it fits alongside other evidence-based supplements:
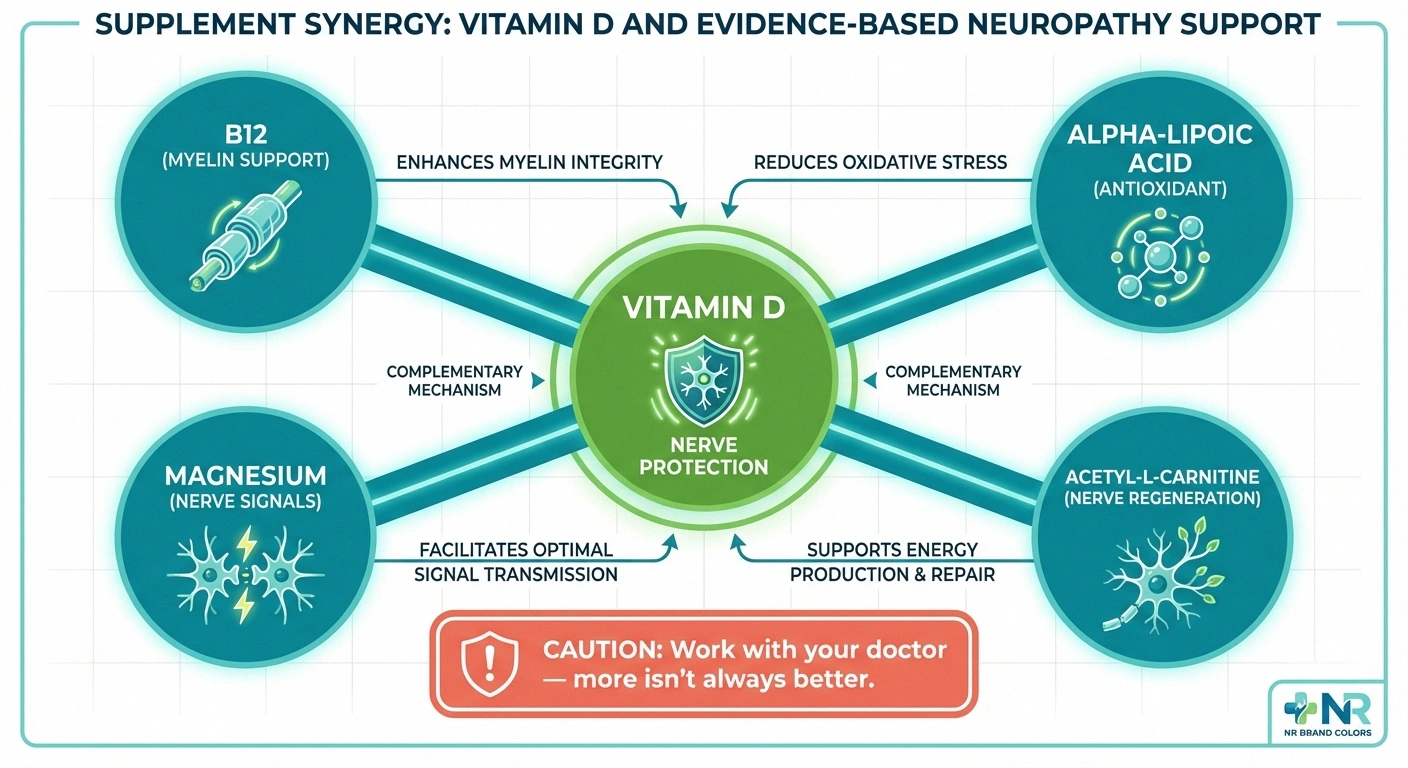
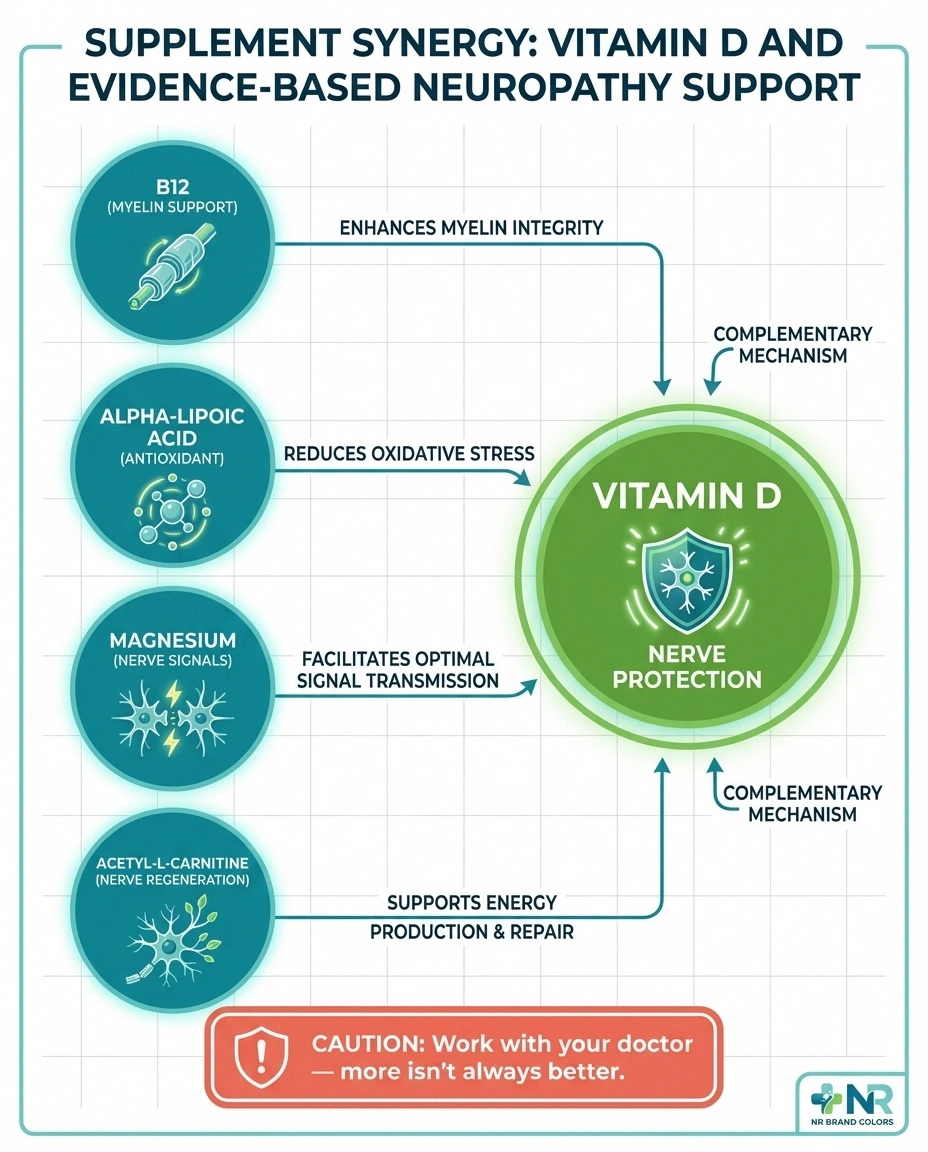
Vitamin B12: While vitamin D supports nerve protection and repair, vitamin B12 is essential for myelin sheath formation — the protective coating around nerve fibers. B12 deficiency is one of the most common and treatable causes of neuropathy. Both vitamins should be tested in anyone with neuropathy symptoms. B12 injections may be needed for severe deficiency.
Alpha-lipoic acid: This powerful antioxidant has the strongest evidence among supplements for treating diabetic neuropathy specifically. It works through different mechanisms than vitamin D — primarily by reducing oxidative stress in nerves. The two may complement each other well.
Magnesium: Magnesium plays a role in nerve signal transmission and has anti-inflammatory properties. Many people with neuropathy are also magnesium-deficient. Magnesium glycinate is generally the best-tolerated form for supplementation.
Acetyl-L-carnitine: This amino acid derivative has shown promise for improving nerve fiber regeneration and reducing pain in several neuropathy studies. It's another supplement that may work synergistically with vitamin D.
A word of caution: More supplements aren't always better. Work with your healthcare provider to determine which ones are appropriate for your specific situation. Some supplements can interact with medications or with each other, and taking too many at once can be both expensive and potentially counterproductive.
Frequently Asked Questions
Can vitamin D deficiency actually cause neuropathy?
The relationship is complex. Vitamin D deficiency is strongly associated with increased neuropathy risk, particularly diabetic peripheral neuropathy, and is considered an independent risk factor. However, most researchers describe it as a contributing factor rather than a sole cause. Low vitamin D levels may make existing nerve damage worse, slow nerve repair, and increase pain sensitivity. Correcting a deficiency may improve symptoms but is unlikely to be a standalone cure.
How much vitamin D should I take for neuropathy?
There's no one-size-fits-all dose. The right amount depends on your current blood levels, body weight, age, and how well you absorb the vitamin. Most studies showing neuropathy benefits used doses between 2,000 and 5,000 IU of vitamin D3 daily. Always start with a blood test and work with your doctor to determine the appropriate dose for your situation. Taking too much vitamin D can cause toxicity.
How long does it take for vitamin D to help neuropathy symptoms?
Patience is key. It takes six to eight weeks of supplementation to meaningfully raise blood levels, and neuropathy symptoms may take three to six months to respond. The BMJ study that showed significant pain reduction in diabetic neuropathy patients tracked improvements over a 20-week period. Consistent daily supplementation rather than sporadic dosing gives you the best results.
Does vitamin D help non-diabetic neuropathy?
The strongest evidence links vitamin D to diabetic neuropathy specifically. For idiopathic (cause-unknown) neuropathy, recent research found no direct correlation between vitamin D levels and neuropathy severity. However, correcting a deficiency is still recommended for overall nerve health, as vitamin D supports anti-inflammatory pathways and nerve growth factor production regardless of the type of neuropathy.
Can I get enough vitamin D from food alone?
It's very difficult. You'd need to eat fatty fish almost daily and consistently include fortified foods to meet the recommended daily intake through diet alone. A 3-ounce serving of salmon provides about 570 IU, but many people need 1,000 to 2,000 IU or more daily. For most people — especially those with documented deficiency — a combination of dietary sources and supplementation is the most practical approach.
Should I take vitamin D with my neuropathy medications?
Vitamin D supplementation is generally safe alongside common neuropathy medications like gabapentin, pregabalin, and duloxetine. However, some medications can affect vitamin D metabolism, including certain anti-seizure drugs and corticosteroids. Always tell your doctor about all supplements you're taking, and take vitamin D with food for better absorption.
Taking the Next Step
The vitamin D–neuropathy connection is one of those areas where a simple, inexpensive blood test can potentially lead to meaningful improvement. If you're living with neuropathy and haven't had your vitamin D levels checked, it's one of the easiest conversations to have with your doctor.

Vitamin D supplementation isn't a cure for neuropathy. But for people who are deficient — and many neuropathy patients are — correcting that deficiency may reduce pain, support nerve repair, and improve overall quality of life. Combined with other evidence-based approaches like targeted supplements, a nerve-supporting diet, regular exercise, and appropriate medical treatment, vitamin D adds another tool to your neuropathy management toolkit.
The sunshine vitamin may not cure your nerve pain. But it might be one of the missing pieces you haven't explored yet. Ask your doctor. Get tested. And give your nerves what they need to heal.


