I still remember the first time my neurologist suggested a lidocaine patch. I was skeptical — how could a sticky patch on my skin do anything about the nerve pain that kept me up at night? But after years of trying different oral medications and dealing with their side effects, I was willing to try just about anything. That first patch changed how I thought about pain management entirely.
Lidocaine patches have become one of the most talked-about options for people living with neuropathy, and for good reason. Unlike pills that travel through your entire body, these patches deliver relief right where you need it — with far fewer side effects. But they're not a magic solution for everyone. In this guide, I'll walk you through exactly how lidocaine patches work, who benefits most, what the research actually shows, and the practical tips I wish someone had told me from the start.
What Are Lidocaine Patches and How Do They Work?
Lidocaine is a local anesthetic — the same type of numbing medication your dentist uses before a procedure. When delivered through a transdermal patch, lidocaine works by blocking sodium channels on damaged or sensitized nerve fibers directly beneath the skin. This quiets the abnormal electrical signals that cause neuropathic pain without numbing the area completely.
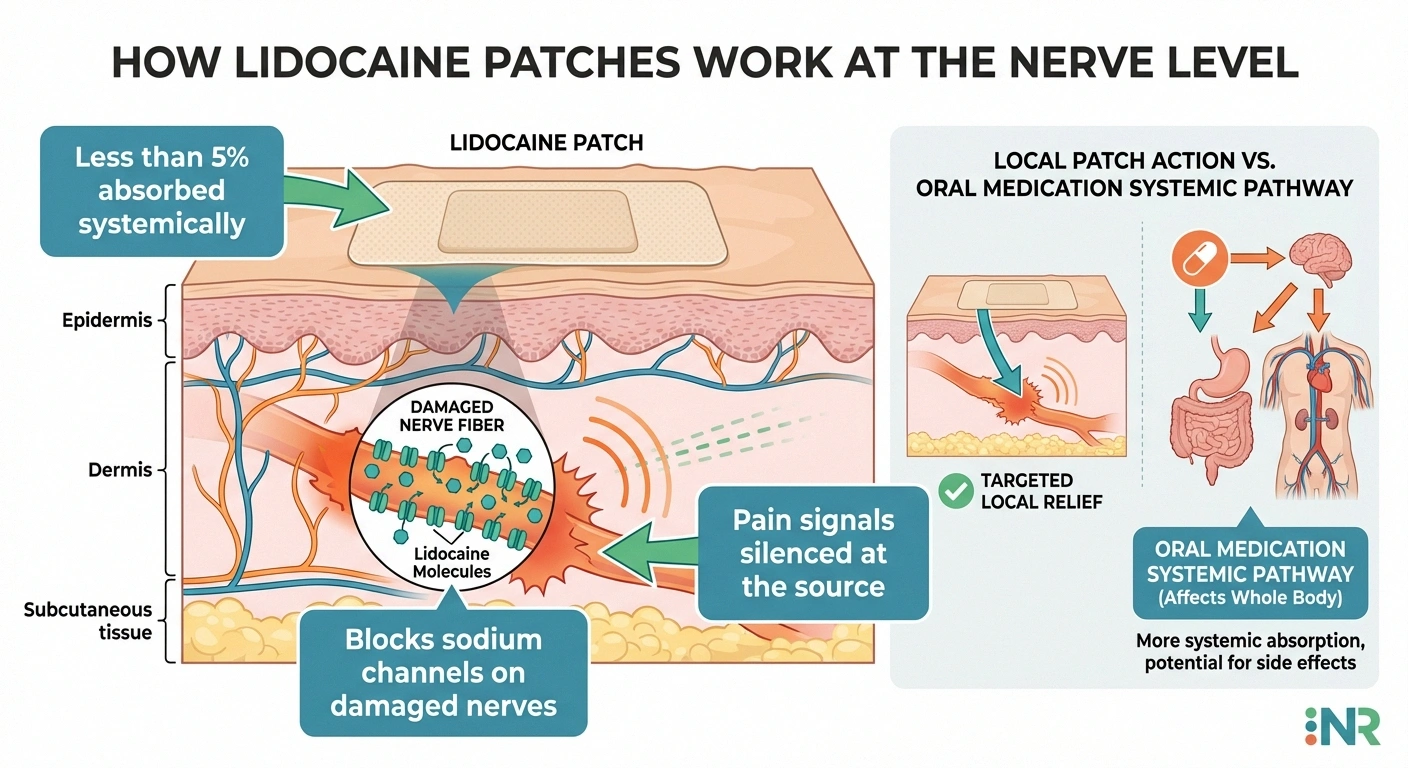
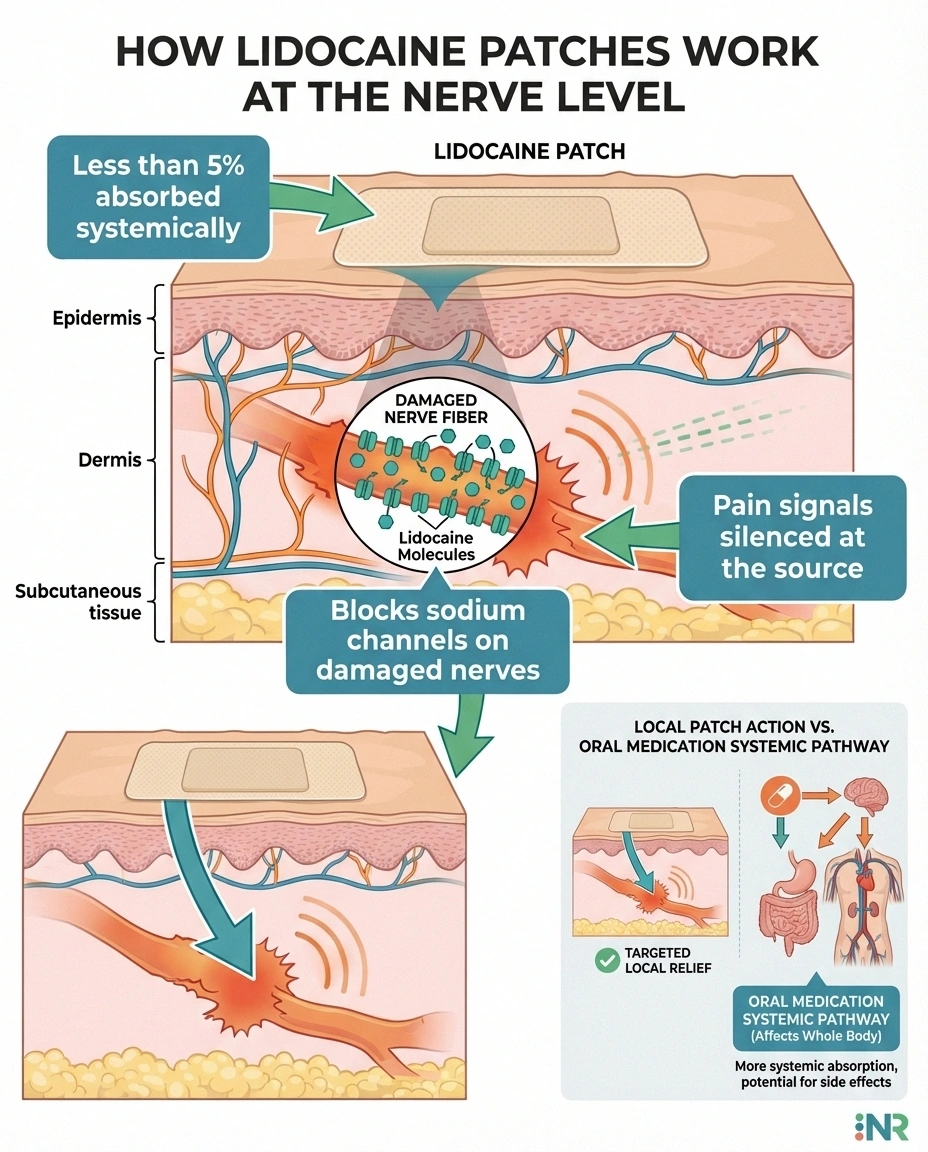
of lidocaine from patches enters the bloodstream — keeping side effects local, not systemic
What makes lidocaine patches unique among neuropathy treatments is their mechanism. According to research published in the journal Current Medical Research and Opinion, the lidocaine patch is the first available treatment that directly targets injured cutaneous nociceptors — the pain-sensing nerve endings in your skin. Less than five percent of the lidocaine actually absorbs into your bloodstream, which is why systemic side effects are so rare compared to oral medications like gabapentin or pregabalin.
Think of it this way: oral medications are like turning down the volume on your entire nervous system. Lidocaine patches are more like putting a silencer on the specific nerves that are misfiring. You stay alert, clear-headed, and functional — something that matters enormously when you're managing a chronic condition.
Prescription vs. Over-the-Counter: Understanding Your Options
Not all lidocaine patches are created equal, and understanding the difference can save you time and money. There are currently three main options available in the United States:
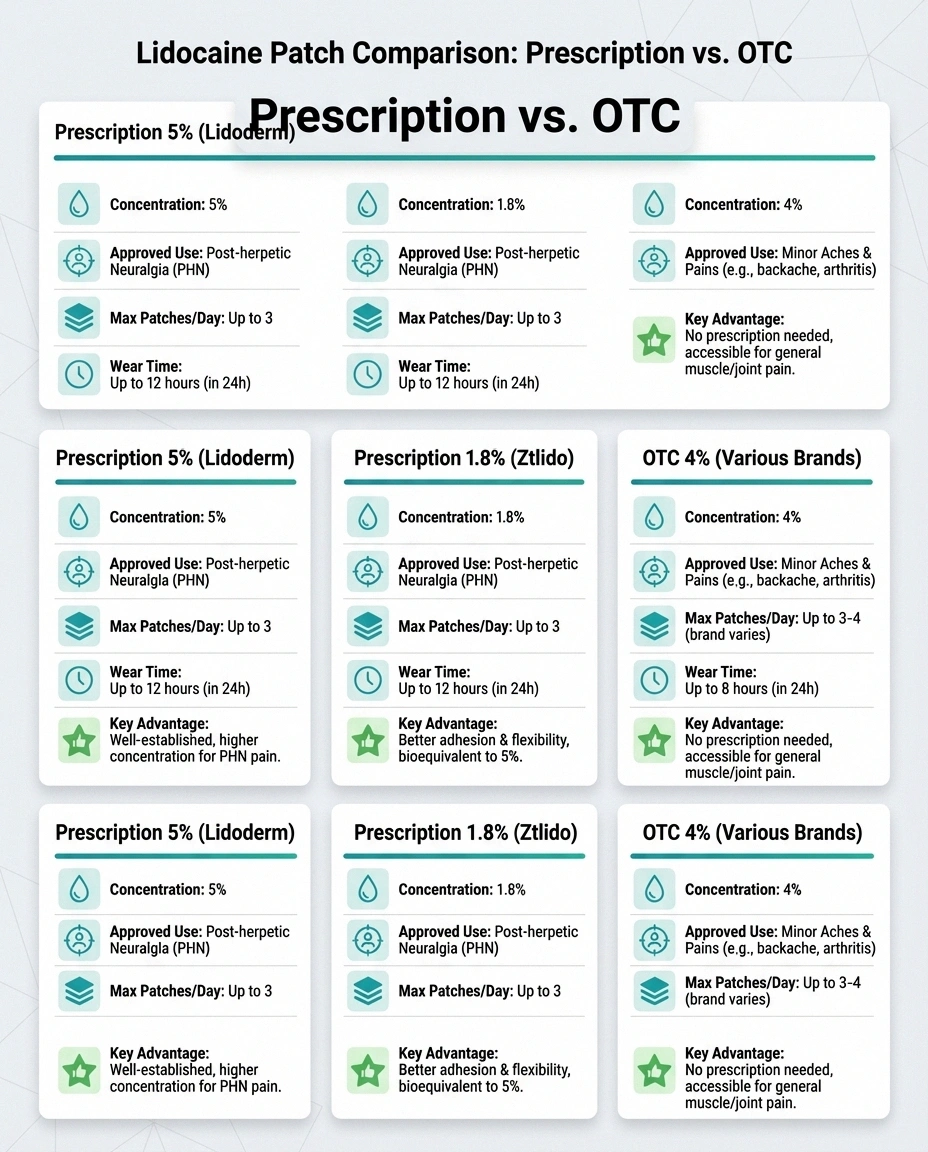
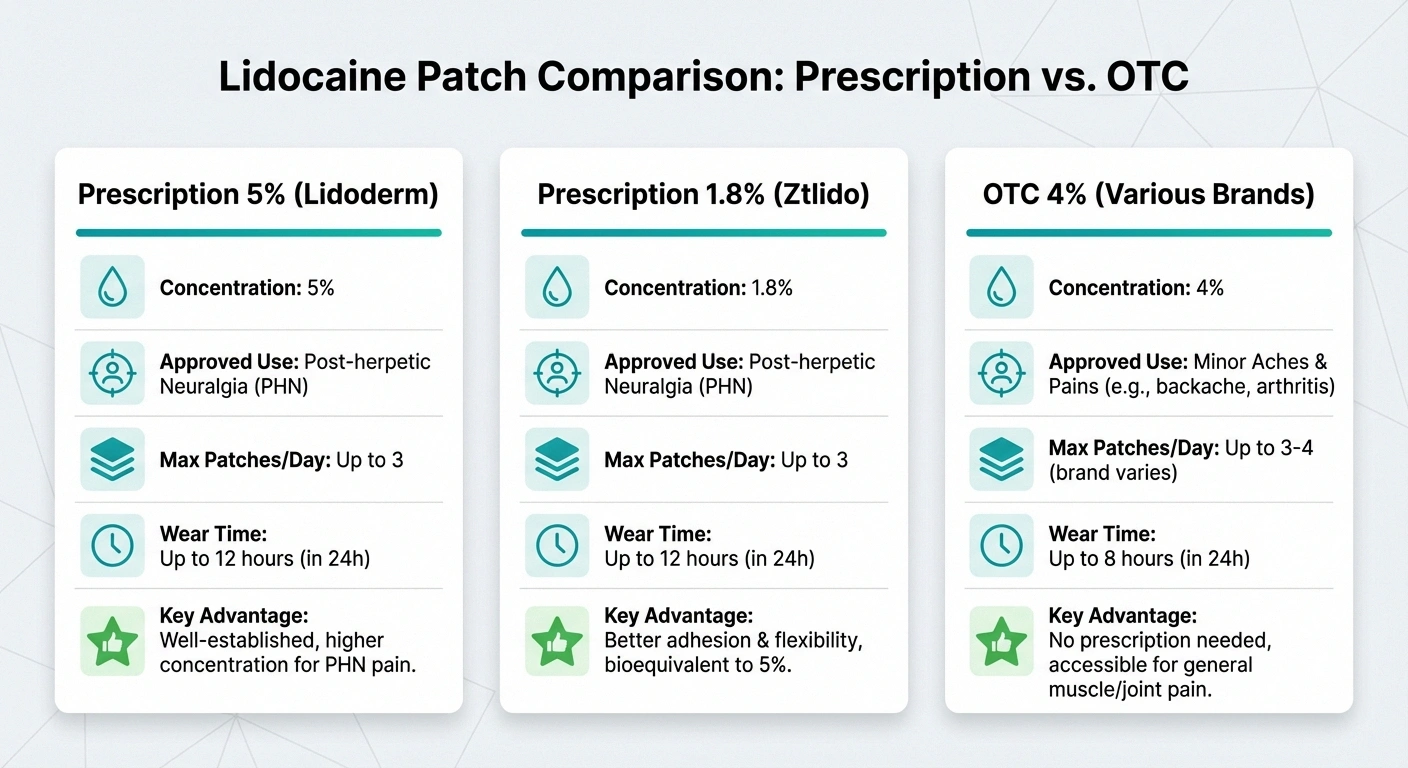

💊 Prescription 5%
Lidoderm / Dermalid
FDA-approved for post-herpetic neuralgia. Up to 3 patches, 12 hrs on/12 hrs off. Most clinically studied option.
🔄 Prescription 1.8%
Ztlido
Thinner, more flexible. Can wear briefly during showers. Same 12-hour schedule. Different adhesive system.
🏪 OTC 4%
Aspercreme / Salonpas
No prescription needed. Lower concentration. Up to 8 hrs per application. No clinical trials for neuropathy specifically.
Prescription 5% lidocaine patch (Lidoderm, Dermalid): This is the original and most studied formulation. Each patch contains 700 mg of lidocaine in a 10×14 cm adhesive patch. It's FDA-approved specifically for post-herpetic neuralgia — the nerve pain that can linger for months or years after a shingles outbreak. However, doctors frequently prescribe it off-label for other types of neuropathic pain.
Prescription 1.8% lidocaine topical system (Ztlido): A thinner, more flexible alternative to the traditional patch. It contains the same total amount of lidocaine but in a different delivery system that may adhere better to certain body areas and can even be worn briefly during showers.
Over-the-counter 4% lidocaine patches (Aspercreme, Salonpas, others): Available at most pharmacies without a prescription. These contain a lower concentration of lidocaine and are marketed for general minor pain relief. Currently, there are no published clinical studies comparing the OTC 4% patches directly to the prescription 5% patches for neuropathic pain. If you're managing significant neuropathy symptoms, starting with a conversation with your doctor about the prescription option may give you more reliable results.
What Does the Research Actually Show?
Let me be straightforward about what the evidence says — and what it doesn't. The research on lidocaine patches is a mixed picture, and I think you deserve to know that upfront.
What the Evidence Shows
Lidocaine 5% patches show a 10–20 point improvement on a 100-point pain scale for post-herpetic neuralgia in controlled trials. For other neuropathy types, clinical experience is promising but high-quality trial data is still limited.
Strong evidence for post-herpetic neuralgia: Multiple randomized, placebo-controlled trials have shown that lidocaine 5% patches provide modest but significant pain relief for post-herpetic neuralgia. Studies typically show a 10 to 20 point improvement on a 100-point pain scale — meaningful, though not dramatic. A landmark open-label study found that the patches provided clinically meaningful relief in most patients with various neuropathic pain conditions, with only one patient reporting a side effect (mild skin irritation).
Mixed evidence for diabetic neuropathy: A study published in JAMA Neurology found that the 5% lidocaine patch improved pain, quality of life, and sleep in people with painful diabetic polyneuropathy. However, the Palliative Care Network of Wisconsin notes that there is strong evidence the patch is not effective for painful diabetic neuropathy in controlled trials. The discrepancy may partly reflect the challenge of separating true analgesic effect from placebo response — the physical sensation of wearing a patch can itself provide comfort.
Limited evidence for other types of neuropathy: Case reports suggest benefit for various neuropathic conditions, but high-quality controlled trials are lacking for most. This doesn't mean the patches don't work — it means the rigorous scientific proof hasn't caught up with clinical experience yet.
What does this mean for you? If you have post-herpetic neuralgia, lidocaine patches have solid evidence behind them. For other types of neuropathy, they may still be worth trying — the low side effect profile means the risk is minimal. But set realistic expectations: these patches typically reduce pain, not eliminate it.
Who Benefits Most From Lidocaine Patches?
In my years connecting with others in the neuropathy community, I've noticed that lidocaine patches tend to work best in specific situations:
People with localized pain: If your neuropathy pain is concentrated in a specific area — your feet, a patch of skin on your back after shingles, or a particular spot on your legs — lidocaine patches can target that area directly. They're less practical if your pain is widespread across large areas of your body.
Those who struggle with oral medication side effects: Many neuropathy medications cause drowsiness, dizziness, weight gain, or cognitive fog. If you've found that duloxetine, amitriptyline, or anticonvulsants make you feel unlike yourself, lidocaine patches offer pain relief without those systemic effects.
Older adults on multiple medications: Drug interactions are a real concern when you're already taking several medications. Because so little lidocaine enters the bloodstream from a patch, the risk of interactions is minimal — making it an attractive option for people who are already managing complex medication regimens.
As part of a multimodal approach: Lidocaine patches work well alongside other treatments. Many people use them in combination with oral medications, physical therapy, or other natural remedies to achieve better overall pain control than any single approach provides alone.
How to Use Lidocaine Patches Correctly
Getting the most out of lidocaine patches comes down to using them properly. Here's what I've learned from my own experience and from talking with healthcare providers:

Application basics: Apply the patch to clean, dry, intact skin over the painful area. Never apply to open wounds, irritated skin, or active rash. You can cut prescription patches to fit smaller areas if needed — just cut them before removing the backing liner. Wash your hands after handling the patch.
Timing matters: For the prescription 5% patch, the standard recommendation is 12 hours on, 12 hours off. You can use up to three patches at a time, but never more. The 1.8% Ztlido system follows the same 12-hour schedule. OTC 4% patches typically recommend up to 8 hours per application, up to 3 times daily.
Avoid heat exposure: This is critically important. According to the Mayo Clinic, heat can cause the lidocaine in the patch to absorb faster into your body, potentially causing serious side effects. While wearing a lidocaine patch, avoid heating pads, electric blankets, hot tubs, saunas, and prolonged sun exposure over the patch area. This is especially relevant for people with heat-sensitive neuropathy.
Placement strategy: The patch works best when placed directly over the most painful area. For foot neuropathy, many people place patches on the tops of their feet or along the soles. For post-herpetic neuralgia, the patch goes over the affected dermatome. Experiment with exact positioning — sometimes shifting the patch by an inch or two makes a noticeable difference.
Give it time: Pain relief typically begins within a few hours of application. Some people notice improvement with the first patch, while others need several days of consistent use before the benefit becomes clear. The patch doesn't just block pain during the 12 hours it's on — patients often report continued relief during the 12-hour off period, especially after using patches consistently.
Side Effects and Safety Considerations
One of the biggest advantages of lidocaine patches is their favorable safety profile. Because the medication stays mostly local, the side effects tend to be mild and limited to the application site:
Heat Warning
Never use heating pads, electric blankets, hot tubs, or saunas while wearing a lidocaine patch. Heat increases absorption, which can lead to serious side effects or overdose. Remove the patch before applying heat to the area.
Common side effects: Mild skin irritation, redness, or a temporary burning sensation at the application site. These are usually minor and resolve when the patch is removed. In clinical studies, only about one in twenty patients reported any skin reaction at all.
Less common side effects: Blistering, bruising, or a rash at the application site. If you notice blistering, stop using the patch on that area and let your skin heal completely before trying again.
Rare but serious concerns: Using too many patches simultaneously or leaving them on for too long can lead to excessive lidocaine absorption. Signs of lidocaine toxicity include dizziness, drowsiness, blurred vision, ringing in the ears, nausea, or — in extreme cases — irregular heartbeat. Following the prescribed dosing schedule (no more than 3 patches, no longer than 12 hours) virtually eliminates this risk.
Allergic reactions: Tell your doctor before starting lidocaine patches if you have a known allergy to any local anesthetic, including benzocaine, bupivacaine, or procaine. While allergic reactions to lidocaine itself are uncommon, adhesive allergies are more frequent — if the patch adhesive bothers your skin, ask about the Ztlido system, which uses a different adhesive.
Compared to the drowsiness, weight gain, and cognitive effects common with oral neuropathy medications, the side effect profile of lidocaine patches is remarkably clean. This is one of the main reasons many neurologists reach for them early in treatment, particularly for older patients.
Lidocaine Patches vs. Other Topical Treatments
Lidocaine patches aren't the only topical option for neuropathy. Understanding how they compare to alternatives can help you and your doctor choose the best approach:
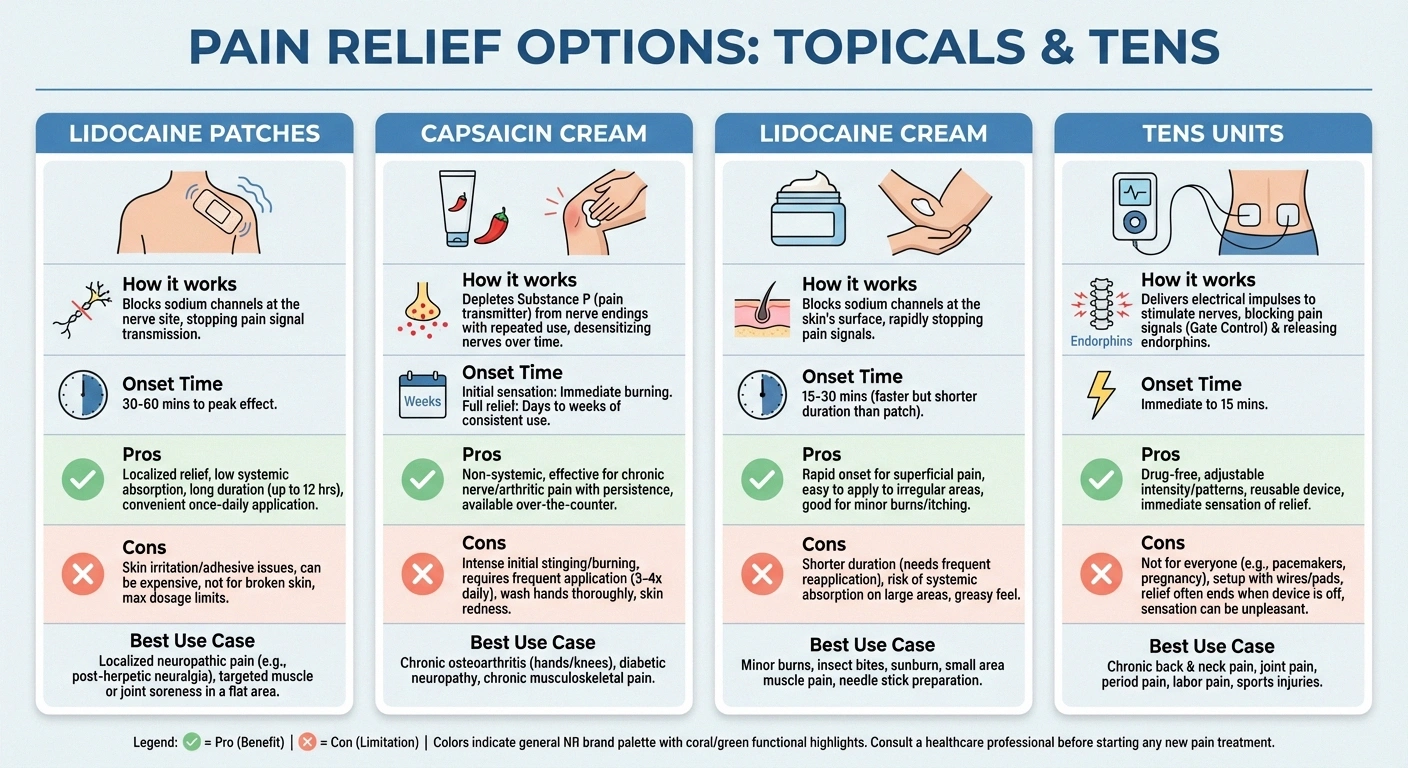
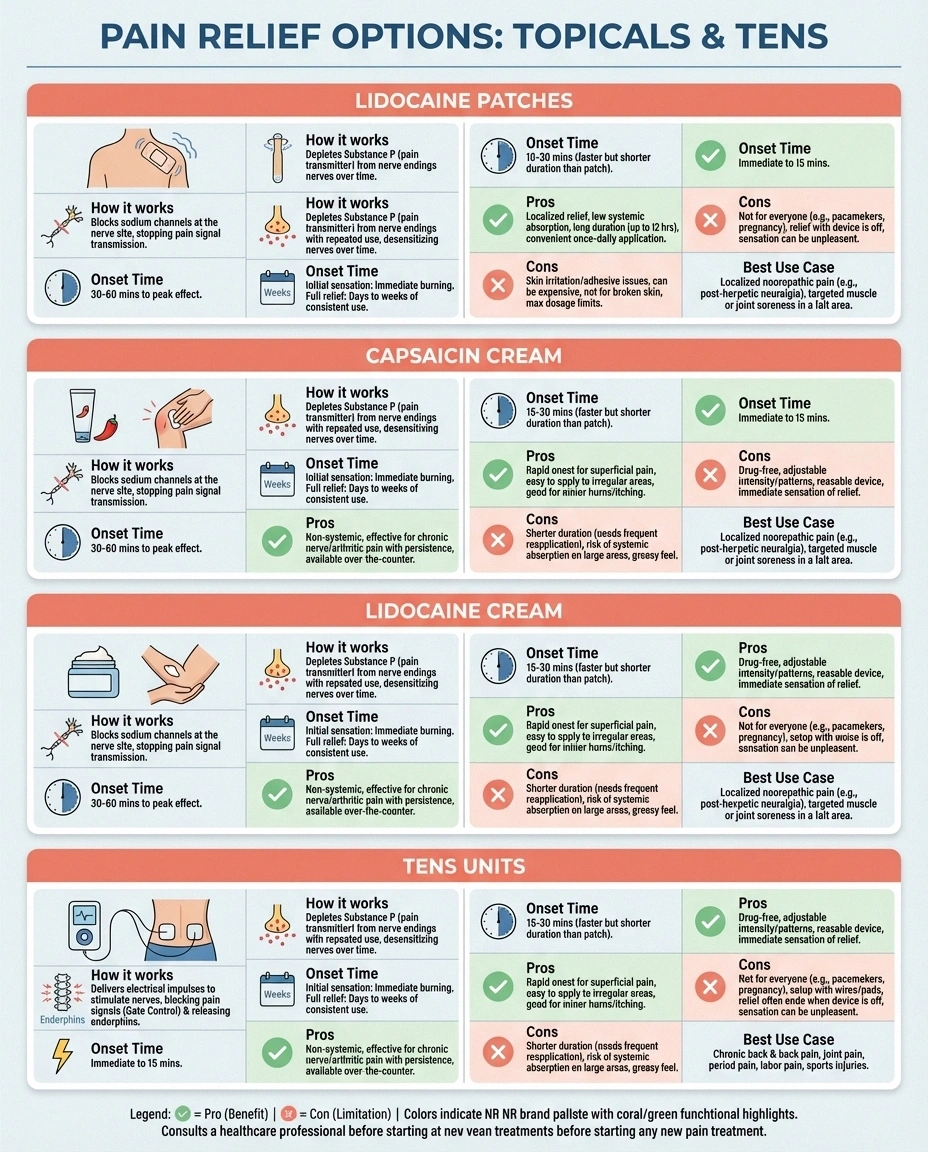
Lidocaine vs. capsaicin: Capsaicin cream works by depleting substance P, a pain neurotransmitter, from nerve endings. It requires consistent application over weeks to build effectiveness and causes a burning sensation that some people find intolerable. Lidocaine patches provide more immediate relief without the burn, but capsaicin may offer longer-lasting nerve desensitization over time. Some people use both — capsaicin cream during the day and lidocaine patches at night.
Lidocaine patches vs. lidocaine cream: Both contain the same active ingredient, but patches offer several practical advantages: consistent dosing over 12 hours, no need to reapply, and they create a physical barrier that can provide additional comfort. Creams can be useful for areas where patches don't adhere well or when you need to treat an irregularly shaped area.
Lidocaine patches vs. TENS units: TENS units use electrical stimulation rather than medication to disrupt pain signals. They're reusable and medication-free but require you to wear a device. Lidocaine patches are more discreet and don't require any equipment. Both can be effective, and some people alternate between them.
Practical Tips From Someone Who Has Been There
After years of using lidocaine patches and hearing from hundreds of others in our support community, here are the practical tips that make the biggest difference:

Pro Tip
Apply your lidocaine patch 30 minutes before bedtime. The 12-hour on/12-hour off schedule aligns perfectly with a nighttime routine — helping you sleep through the worst of your neuropathy pain and removing the patch naturally when you wake up.
Skin preparation matters. Make sure the area is clean, dry, and free of lotions or oils before applying. Moisture is the number one reason patches fall off prematurely. If you shower before applying, wait until your skin is completely dry.
Rotate application sites. Using the same exact spot every day increases the risk of skin irritation. If your pain covers a broader area, shift the patch position slightly each day. This gives your skin time to recover between applications.
Nighttime use can be a game-changer. Many people with neuropathy find that their pain is worse at night. Applying a lidocaine patch before bed can help you fall asleep faster and stay asleep longer. The 12-hour on/12-hour off schedule works perfectly when you apply the patch at bedtime and remove it in the morning.
Don't give up too quickly. Some people feel significant relief with the first patch. Others need a week or more of consistent use before noticing a meaningful difference. If the first few days are underwhelming, keep going for at least two weeks before making a judgment.
Talk to your doctor about cost. Prescription lidocaine patches can be expensive, especially without insurance. Generic versions are available and are significantly cheaper. Your doctor or pharmacist may also know about patient assistance programs. Meanwhile, OTC 4% patches are much more affordable and may be a reasonable first step for mild to moderate pain.
When Lidocaine Patches May Not Be Right for You
While lidocaine patches are generally safe and well-tolerated, there are situations where they may not be the best choice:
If your neuropathy causes widespread pain across large areas of your body, the patches can only cover so much. You'd need multiple patches, and there are limits on how many you can use at once. In these cases, systemic medications or a combination approach may be more practical.
People with significant skin conditions — including eczema, psoriasis, or open wounds in the pain area — may not be able to use lidocaine patches safely. The patch requires intact skin for both proper adhesion and safe medication delivery.
If you have liver disease, use caution. While systemic absorption is minimal, the lidocaine that does enter your bloodstream is metabolized by the liver. Your doctor can help determine whether the amount absorbed poses any risk for your specific situation.
Finally, if your neuropathy pain is primarily deep rather than superficial — for example, deep aching in the muscles rather than burning or tingling in the skin — lidocaine patches may be less effective. They work best on peripherally generated pain in or just under the skin surface.
Talking to Your Doctor About Lidocaine Patches
If you think lidocaine patches might help your neuropathy, here's how to have a productive conversation with your healthcare provider. Describe specifically where your pain is located, what it feels like (burning, tingling, shooting), and when it's worst. Mention any oral medications you've tried and what side effects were problematic. Ask about trying the prescription 5% patch if OTC options haven't provided sufficient relief.

Questions worth asking your doctor include: “Would a lidocaine patch work with my current medications?” “Should I try the OTC version first or go straight to prescription?” “How long should I try the patches before we reassess?” Your doctor can also discuss whether lidocaine patches fit into a broader management plan based on your neuropathy stage and progression.
Frequently Asked Questions
Can I use lidocaine patches on my feet for neuropathy?
Yes, many people apply lidocaine patches to the tops or bottoms of their feet for peripheral neuropathy pain. Make sure the skin is clean, dry, and intact. Some people find that wearing a loose sock over the patch helps keep it in place during the day. Remove the patch before bathing or showering if using the 5% prescription version.
How quickly do lidocaine patches start working?
Most people notice some pain relief within one to four hours of applying a lidocaine patch. However, the full benefit often builds over several days of consistent use. If you don't notice improvement after the first patch, continue using them daily for at least one to two weeks before deciding they aren't working for you.
Can I cut a lidocaine patch to fit a smaller area?
Prescription lidocaine 5% patches and 1.8% topical systems can be cut to fit smaller areas. Cut the patch before removing the release liner to avoid getting lidocaine on your hands. Over-the-counter patches may have different instructions, so check the packaging.
Are lidocaine patches safe to use long-term?
Lidocaine patches are generally considered safe for long-term use. Case reports indicate some patients have used them successfully for over a decade without developing tolerance or significant complications. The minimal systemic absorption means organ-related side effects are extremely unlikely with proper use. However, regular check-ins with your doctor are still recommended.
Do lidocaine patches interact with other neuropathy medications?
Because less than five percent of the lidocaine absorbs into the bloodstream, drug interactions are rare. Lidocaine patches can generally be used safely alongside gabapentin, pregabalin, duloxetine, amitriptyline, and other common neuropathy medications. Always inform your doctor about all medications you're using, including OTC patches.
What is the difference between the 4% OTC and 5% prescription patches?
The prescription 5% patch contains a higher concentration of lidocaine and has been studied in clinical trials for neuropathic pain. OTC 4% patches have a lower concentration and are marketed for general minor pain. There are currently no published studies directly comparing the two for neuropathy, so the prescription version may provide more reliable results for significant nerve pain.
Finding Your Path to Better Pain Management
Living with neuropathy means constantly searching for tools that give you back some control over your daily life. Lidocaine patches won't cure neuropathy — nothing can undo nerve damage that's already occurred. But for many people, they provide meaningful relief with remarkably few downsides. They're one piece of a larger puzzle that might include dietary changes, regular exercise, targeted supplements, and other treatments.

If you haven't tried lidocaine patches yet, they're worth discussing with your healthcare provider. And if you've tried them before without success, consider whether the timing, placement, or formulation might have been the issue rather than the medication itself. Sometimes the difference between “this doesn't work” and “this really helps” comes down to technique.
Your nerves may be damaged, but you still have options. Keep exploring them.