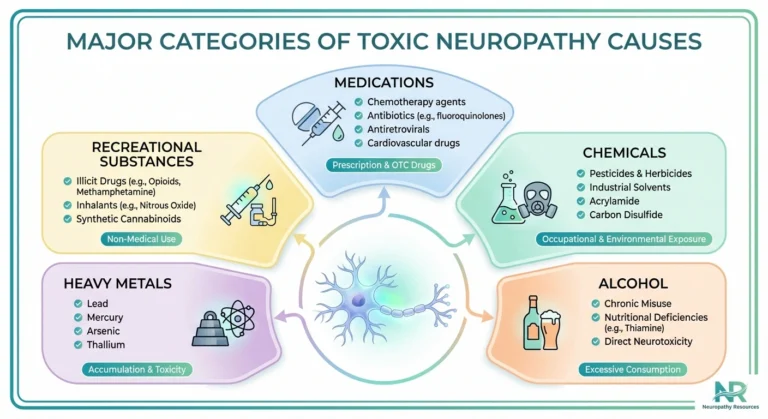
Browse all our types and causes of neuropathy guides for more articles like this one.
Hereditary Neuropathy and Charcot-Marie-Tooth Disease: Symptoms, Testing, and Daily Life
Getting told you may have a hereditary neuropathy can feel overwhelming fast. Most people immediately ask: “What does this mean for my future?” “Is this definitely from my family?” “Will my kids get it?” Those are all valid questions. Hereditary neuropathies are not one single condition—they are a group of genetic nerve disorders, and Charcot-Marie-Tooth disease (CMT) is the most common form.
The good news is that while there is no cure yet, there are many tools that may help you protect mobility, reduce falls, preserve hand function, and plan your next steps with clarity.
What “Hereditary Neuropathy” Actually Means
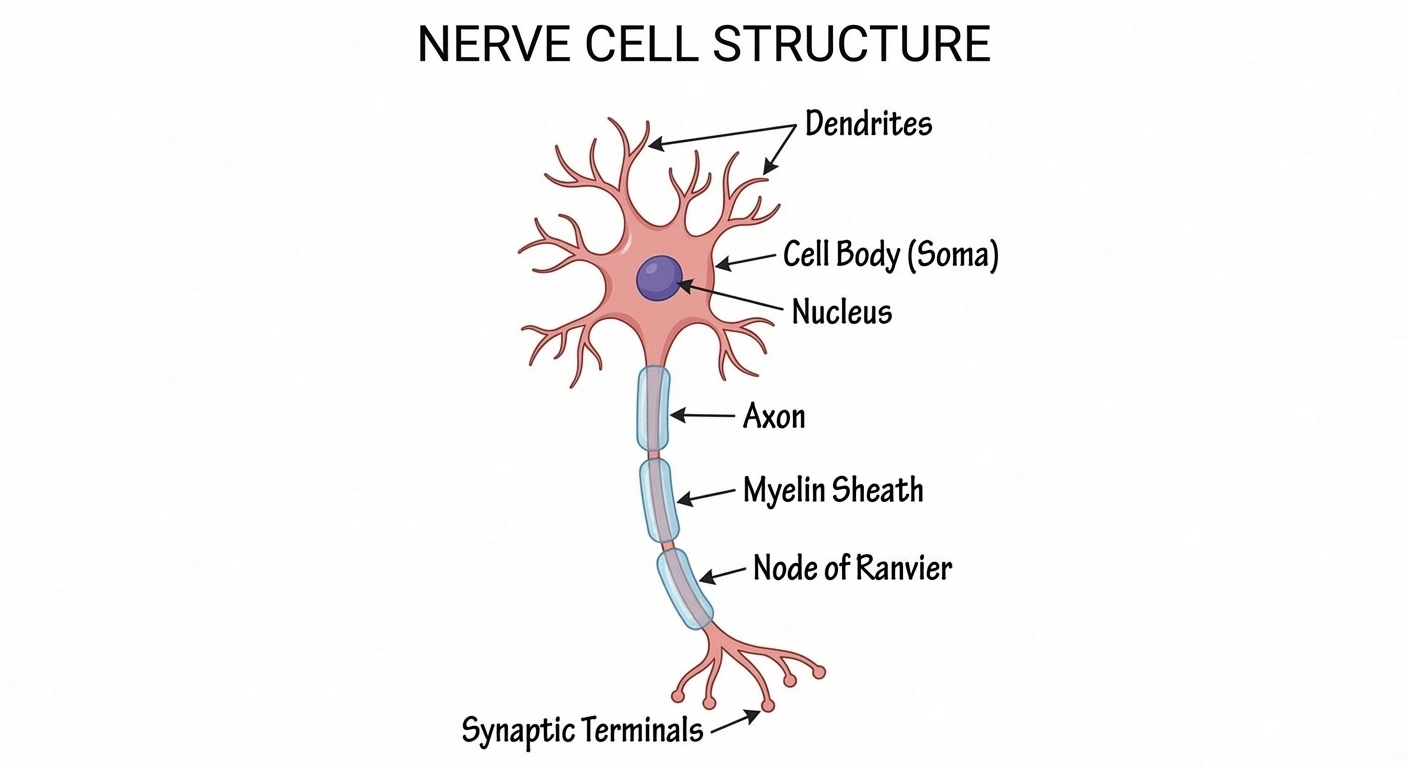
Hereditary neuropathy means a nerve disorder linked to inherited or new genetic variants affecting peripheral nerves. These nerves carry movement and sensation signals between your brain/spinal cord and your limbs. When the nerve fiber (axon), myelin sheath, or both are affected, signals can slow down or weaken over time.
According to NINDS and MedlinePlus Genetics, CMT is the most common inherited neuropathy and can involve many different genes and inheritance patterns (NINDS; MedlinePlus).
Simple frame: “Hereditary neuropathy” is the umbrella. “CMT” is a major subgroup under that umbrella.
Common Symptoms and Typical Pattern
Symptoms vary by subtype and person, but the usual pattern starts in the feet/lower legs and progresses gradually. Many people first notice tripping, ankle instability, toe curling, high arches, or unusual fatigue when walking.
- Foot drop or difficulty lifting the front of the foot
- Frequent ankle sprains or falls
- High arches or hammertoes
- Calf muscle thinning (“inverted champagne bottle” appearance)
- Numbness, tingling, or reduced vibration sense
- Later hand weakness affecting buttons, writing, or grip
Severity can differ widely—even among relatives with the same nerve conduction testing for CMT. Some people have mild symptoms for decades; others need braces or surgical support earlier.
Is It Always Inherited? Not Always.
Many hereditary neuropathies are inherited (autosomal dominant, autosomal recessive, or X-linked patterns), but a person can also have a new genetic change without a known family history. So “nobody in my family has this” does not rule CMT out.
Genetic counseling can help you understand recurrence risk and what testing may be useful for relatives, including timing and emotional readiness.
How Diagnosis Usually Happens
Diagnosis is usually stepwise, not one test in isolation. Most clinicians combine exam findings with electrodiagnostics and, when appropriate, genetic testing.
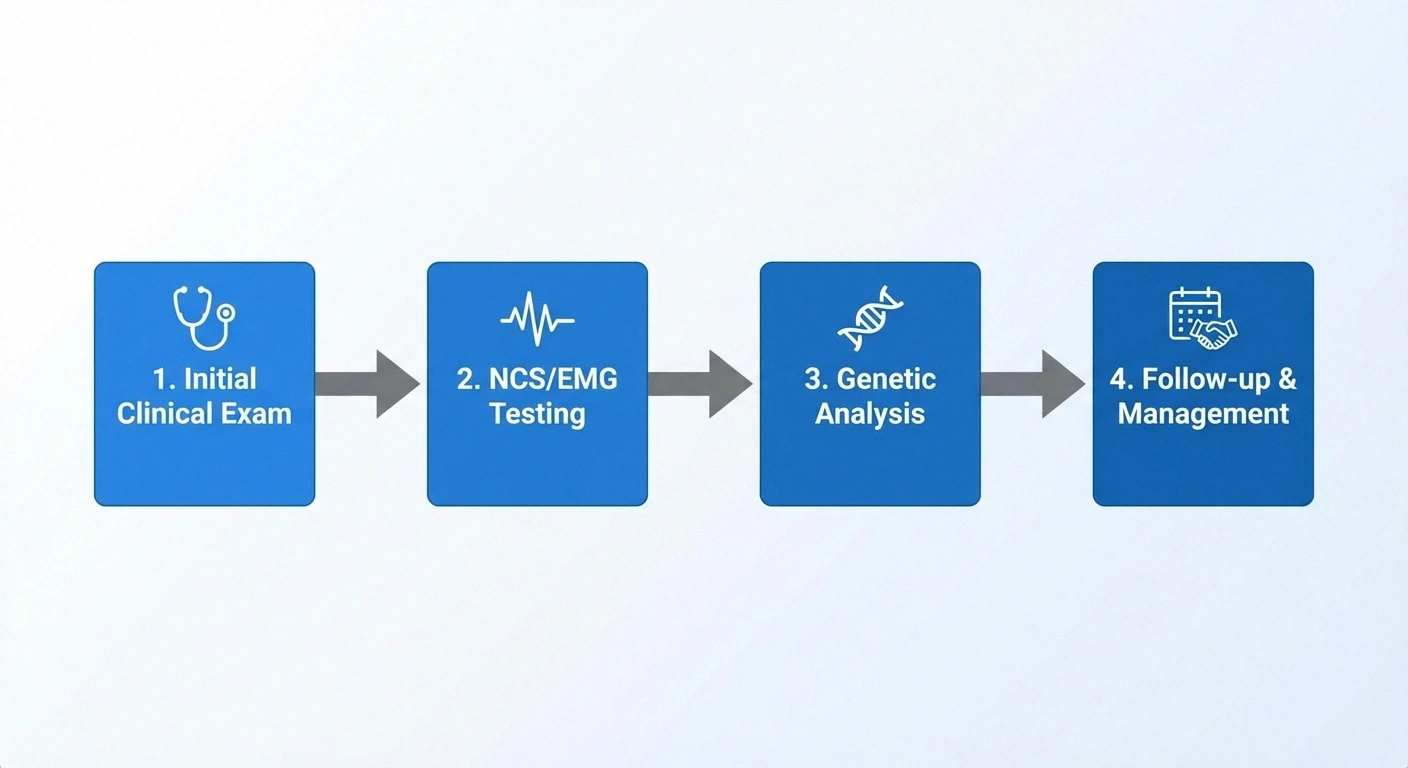
Typical diagnostic workflow
- Neurologic history + physical exam (pattern of weakness/sensation)
- Nerve conduction studies / EMG (demyelinating vs axonal clues)
- Targeted or panel genetic testing
- Additional tests only if needed to rule out acquired causes
Many people worry genetic testing means “nothing can be done.” In reality, diagnosis may still change your treatment plan, safety planning, and family counseling path.
What Treatment Looks Like Without a Cure
There is currently no cure for CMT, but management can be highly practical and effective. The goal is preserving function and reducing injury risk over time.

- Physical therapy: gait training, balance work, mobility and strength support
- Occupational therapy: hand strategies, adaptive tools for daily tasks
- Orthotics: ankle-foot orthoses for foot drop and improved walking safety
- Footwear changes: roomier toe box, stable base, custom support
- Pain management: neuropathic pain plans when needed
- Orthopedic referral: for deformity-related pain or severe instability
Patients often do best with early intervention rather than waiting for major decline. Small changes now can reduce future fall burden.
Daily Living: What Helps Most in Real Life
- Fall-proof high-risk areas at home (loose rugs, dim hallways, cluttered stairs)
- Build in pacing and recovery breaks for longer walking days
- Use grip aids and button hooks before hand fatigue gets severe
- Track symptom changes every month to catch progression early
- Review medications with your clinician before starting anything new

Safety tip: If falls are increasing, prioritize gait/brace reassessment quickly instead of waiting for your annual visit.
Related Neuropathy Guides
- Neuropathy Diagnosis: Tests Your Doctor May Order
- small fiber nerve damage
- What Are the Stages of Neuropathy?
- Neuropathy and Balance: Fall Prevention Strategies
CMT Types in Plain English
You may hear clinicians mention CMT1, CMT2, CMTX, or intermediate forms. These labels describe whether the primary issue looks more demyelinating (myelin sheath), axonal (nerve fiber), mixed, or X-linked in inheritance pattern. Knowing your subtype helps set expectations for progression and testing.
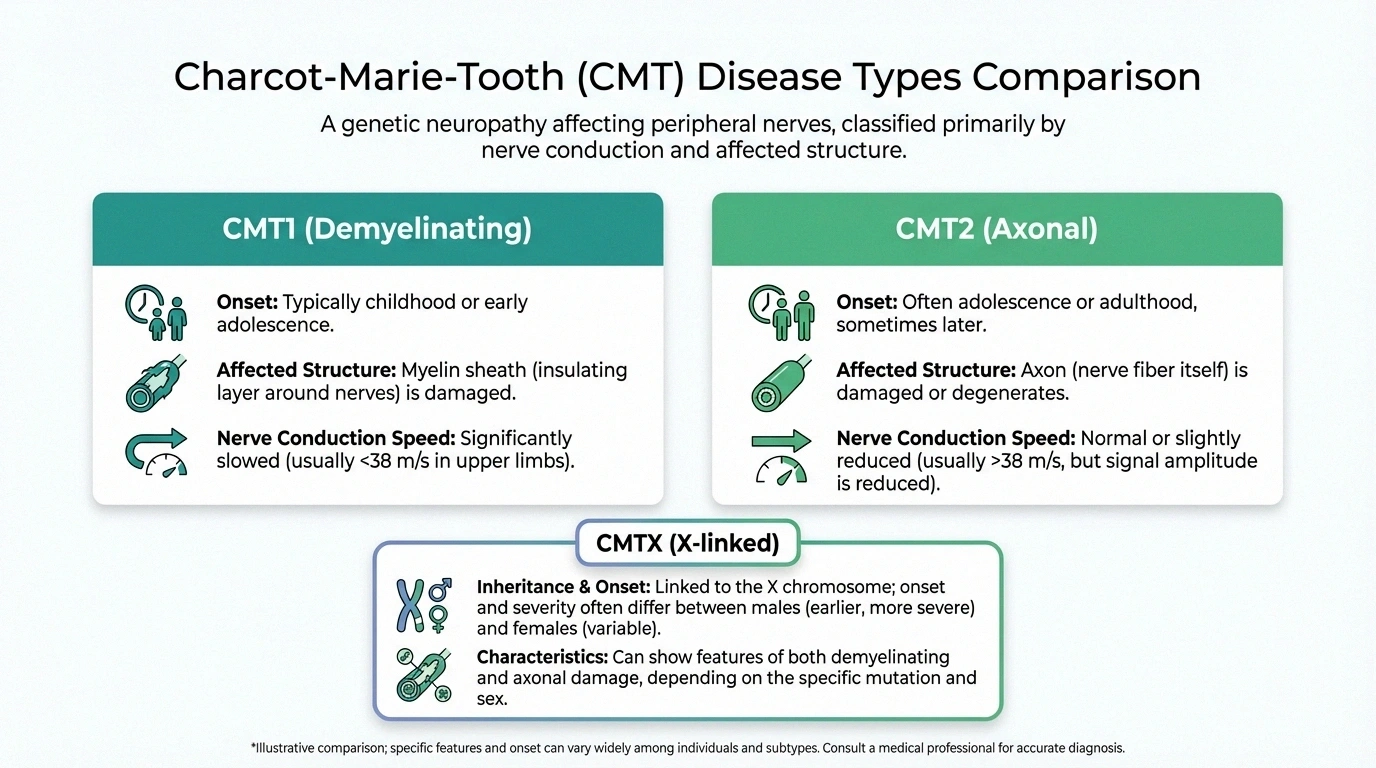
- CMT1: often demyelinating pattern with slowed nerve conduction.
- CMT2: often axonal pattern with lower signal amplitude.
- CMTX: linked to genes on the X chromosome; severity can differ by sex.
- Intermediate forms: mixed electrodiagnostic features.
You do not need to memorize every subtype to make progress. Start with what changes your care now: safety, mobility, fatigue management, hand function, and monitoring plan.
The First 30 Days After Diagnosis
The first month is often the hardest emotionally. Many people bounce between relief (“I finally have an explanation”) and fear (“What if this gets worse fast?”). A concrete 30-day plan can reduce that uncertainty.

- Week 1: confirm diagnosis details, subtype clues, and immediate safety risks.
- Week 2: schedule PT/OT evaluations and footwear/orthotic assessment.
- Week 3: home safety walkthrough, including stairs, bathroom, and nighttime lighting.
- Week 4: set follow-up intervals and identify progression markers to track.
Tracking monthly metrics (falls, walking endurance, hand dexterity, fatigue) gives objective data that helps your neurologist adjust care earlier.
Mobility Tools: Braces, Footwear, and Energy Pacing
Many people delay braces because they fear braces signal “decline.” In practice, the right brace often increases independence by reducing tripping, stabilizing gait, and conserving energy. Think of supports as tools, not labels.
- Ankle-foot orthoses can reduce toe catching and ankle rollover risk.
- Stable shoes with room for orthotics may reduce pressure points and fatigue.
- Trekking poles or canes can add confidence on uneven ground.
- Energy pacing (work-rest cycles) may prevent overuse crashes.
If a device feels uncomfortable, request reassessment. Fit quality is everything. Poorly fitted supports are a common reason people abandon tools that might otherwise help.
Hand Function and Work Adaptations
As symptoms affect hand strength or dexterity, small work and home modifications can protect function. Occupational therapy can help you test specific adaptations before frustration builds.

- Keyboard/mouse adjustments for reduced grip strain
- Larger-handle utensils and grooming tools
- Button hooks, zipper pulls, and jar-openers
- Voice dictation for high-volume typing tasks
- Task batching to avoid repetitive fatigue spikes
Ask your care team for documentation if workplace accommodations are needed. Early adjustments can preserve productivity and reduce pain flare-ups.
Family Planning and Genetic Counseling
Questions about children and relatives are emotionally loaded. Genetic counseling can help you understand inheritance probability, testing limitations, and the practical meaning of results. It is not only for people who are currently planning pregnancy. It can also help siblings and adult children make informed choices.
Counseling sessions often cover what a “positive” or “negative” result means, when testing is most useful, and how to communicate findings in families where symptoms vary a lot from person to person.
Mental Load Is Real — Build Support Early
Living with progressive uncertainty can be mentally exhausting. You may look “fine” to others while adapting constantly in private. Consider building support intentionally: counseling, peer communities, and regular check-ins with people who understand your day-to-day reality.
Emotional resilience is not separate from physical care. It supports treatment adherence, safe decision-making, and quality of life over the long term.
Long-Term Monitoring: What to Track Year Over Year
Because hereditary neuropathies are often progressive, long-term tracking is one of the most useful tools you have. Objective trends can reveal change sooner than memory alone and make follow-up visits far more productive. Instead of relying on “I think things are worse,” you can show specific shifts in mobility, sensation, hand function, and fatigue.
- Number of falls or near-falls each month
- Walking distance before fatigue rises sharply
- Time needed for stairs or repeated sit-to-stand tasks
- Grip endurance for daily tasks (jar opening, typing, handwriting)
- Foot pain, shoe comfort, and pressure-point issues
- Night symptoms and sleep disruption frequency
Bring this log to neurology and therapy visits. It helps clinicians decide whether to adjust orthotics, update exercise plans, repeat testing, or screen for added contributors such as vitamin issues or compressive injuries. A steady plan with small adjustments often works better than large, infrequent changes.
It is also worth rechecking your support system annually. Progressive conditions can change role demands at home and work. Revisit practical supports early: transportation options, household task modifications, mobility aids for long distances, and backup plans for bad symptom days.
Long-term management is a marathon, not a sprint. Measured tracking, flexible support, and regular reassessment can help maintain independence and confidence for many years.
FAQ
Is CMT always inherited from a parent?
No. Many cases are inherited, but some arise from new genetic variants even when there is no known family history.
Can someone have CMT and not know it for years?
Yes. Mild forms may progress slowly and be recognized late, especially if symptoms are subtle early on.
Which tests are most useful?
Clinical exam, nerve conduction/EMG, and genetic testing are the usual core tools. Your neurologist chooses the sequence.
Is CMT life-shortening?
In most cases, life expectancy is not significantly reduced, but mobility and function can be affected over time.
Does exercise help or hurt?
Appropriately guided exercise often helps function and confidence. Overexertion without guidance may worsen fatigue or injury risk.
Should family members be tested immediately?
That decision is personal and best made with genetic counseling, considering age, symptoms, and readiness for results.
Takeaway
Hereditary neuropathy and CMT are manageable conditions, even though they are lifelong for many people. Early diagnosis, practical support, and consistent follow-up may help you stay safer and more independent. This is educational information, not personal medical advice—talk to your doctor or neurologist for individualized care.