
Scalp Neuropathy: When Tingling and Burning Affect Your Head
Most people think of neuropathy as a foot or hand problem. So when the tingling, burning, or crawling sensation shows up on your scalp, it can be genuinely alarming. Is your neuropathy spreading to your head? Is this something completely different? Should you be worried?
Scalp neuropathy — sometimes called scalp dysesthesia or burning scalp syndrome — is more common than most people realize. A 2022 study in the Journal of the European Academy of Dermatology and Venereology described it as an abnormal sensation of the scalp characterized by burning, tingling, and itching in the absence of visible skin problems. If your scalp looks perfectly normal but feels like it's on fire, you're not imagining things.
This guide covers everything you need to know about neuropathy-related scalp symptoms: what causes them, how they connect to your existing neuropathy, when to worry, and what actually helps.
What Is Scalp Neuropathy?
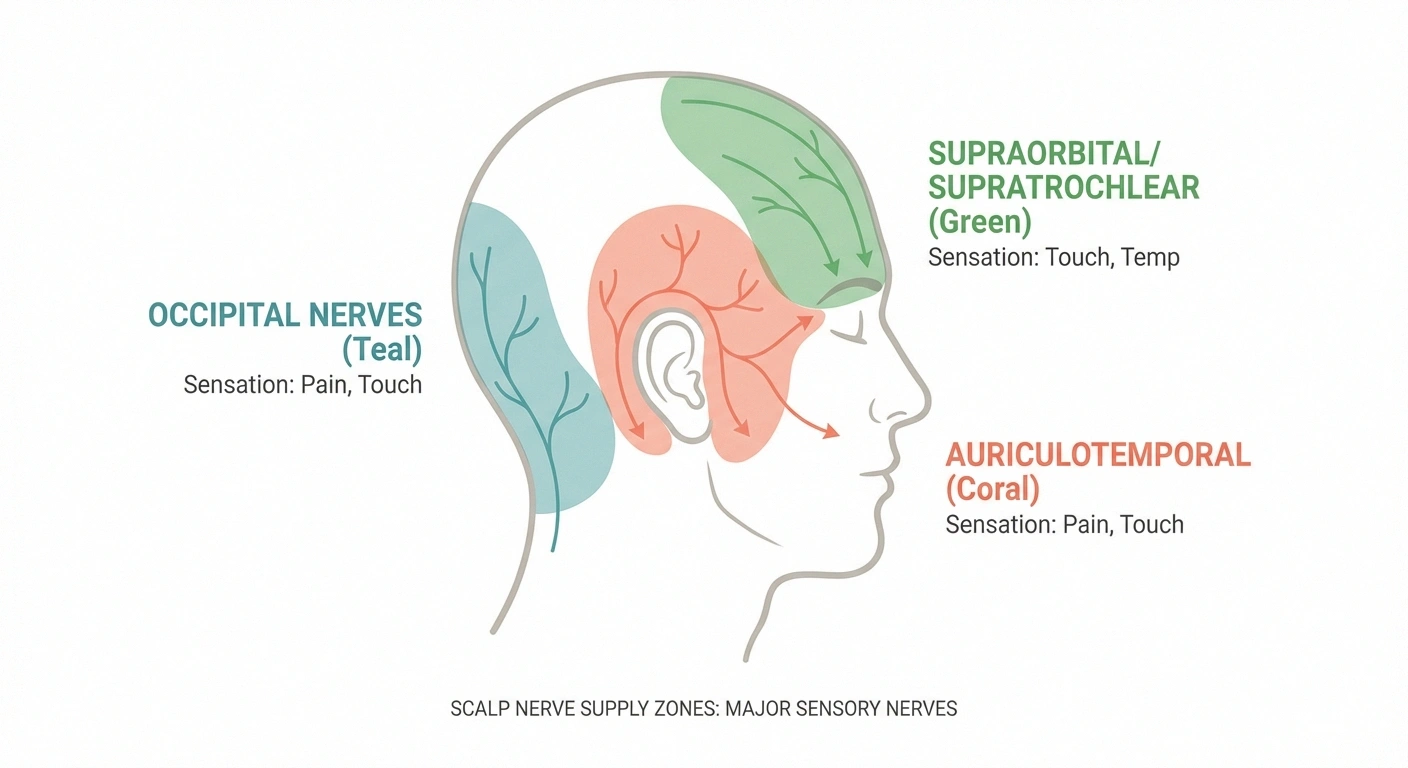
Scalp neuropathy is nerve dysfunction affecting the nerves that supply sensation to your scalp. Your scalp has an incredibly dense network of sensory nerves — it's one of the most nerve-rich areas of your body. The major nerves serving the scalp include the greater and lesser occipital nerves (back of the head), the supraorbital and supratrochlear nerves (forehead), and the auriculotemporal nerve (temples and sides).
The Telltale Sign
The defining feature of scalp neuropathy: your scalp looks completely normal — no rash, no redness, no flaking — but feels like it's burning, tingling, or crawling. If your scalp looks normal but feels abnormal, the problem is neurological, not dermatological.
When these nerves malfunction — from damage, compression, inflammation, or systemic neuropathic conditions — you can experience a range of abnormal sensations:
- Burning — a hot, stinging sensation, often described as feeling like a sunburn even though the skin looks normal
- Tingling — pins and needles across part or all of the scalp
- Itching — a deep, persistent itch that scratching doesn't relieve (neuropathic itch)
- Crawling sensations — feeling like something is moving on or under the skin
- Tenderness — the scalp feels sore to the touch, making hair brushing or wearing hats uncomfortable
- Numbness — reduced sensation in patches of the scalp
The defining feature of scalp neuropathy, versus a skin condition like psoriasis or dermatitis, is that the scalp looks normal. There's no rash, no flaking, no redness — just abnormal sensations coming from the nerves themselves. If you do have visible scalp changes, the cause may be dermatological rather than neurological, though both can co-exist.
Causes of Scalp Tingling and Burning
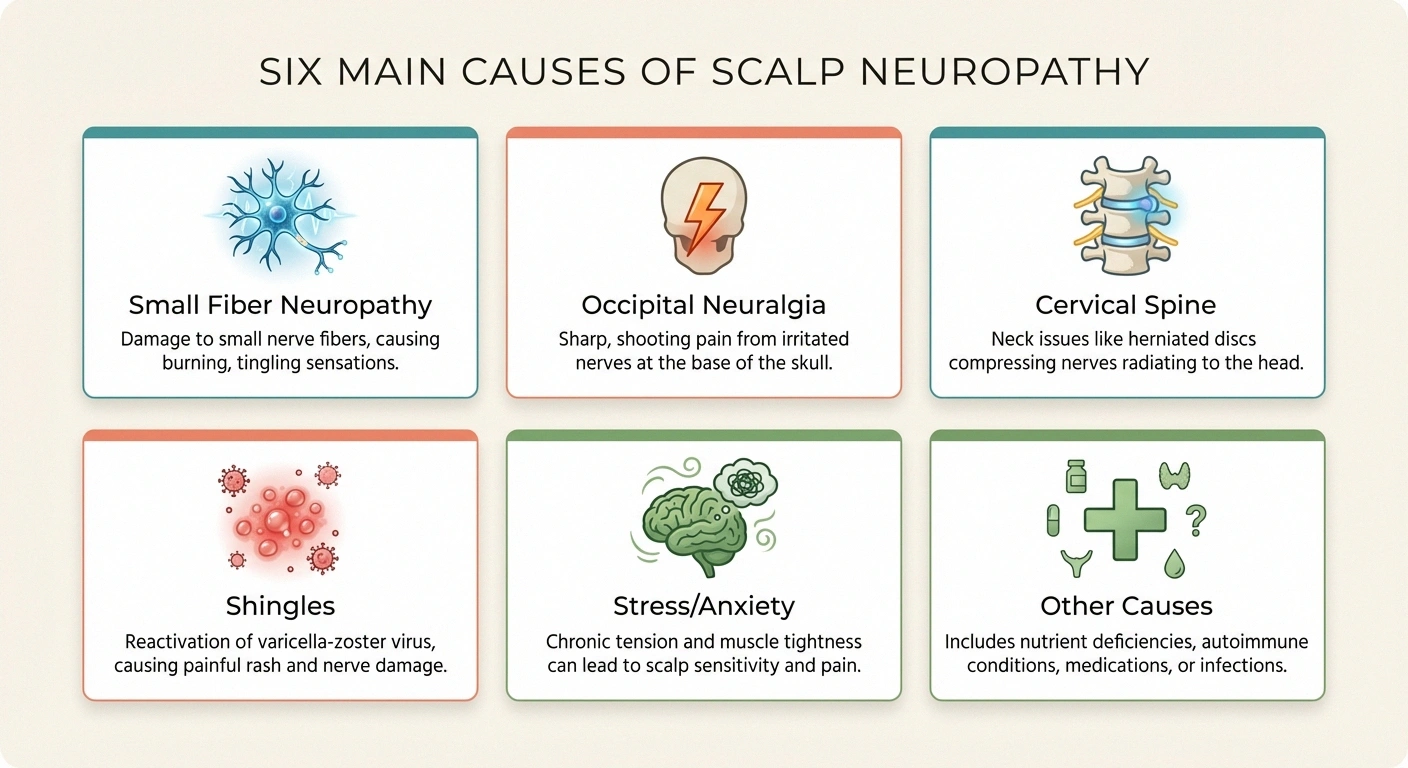
Scalp neuropathy can result from several different mechanisms. Understanding which one applies to you is the first step toward the right treatment.
Which Cause Matches Your Symptoms?
Diffuse tingling + existing hand/foot neuropathy → Small fiber neuropathy spreading
Sharp shooting pain from skull base upward → Occipital neuralgia
One-sided + changes with neck position → Cervical spine issue
Burning followed by a rash → Possible shingles (see doctor within 72 hours)
Whole-scalp tingling that fluctuates with stress → Stress/anxiety-related
Small Fiber Neuropathy
If you already have small fiber neuropathy (SFN) in your feet or hands, scalp symptoms may represent the same condition spreading to other areas. Small nerve fibers are found throughout the body, including the scalp. SFN can affect these fibers anywhere, though the feet and hands are typically affected first because they have the longest nerves.
People with systemic small fiber neuropathy — especially from autoimmune causes, diabetes, or idiopathic neuropathy — may eventually develop scalp symptoms as the condition progresses. This is concerning but not dangerous — it's the same process that's happening in your extremities, not a sign of brain involvement.
Occipital Neuralgia
Occipital neuralgia involves the greater or lesser occipital nerves that run from the upper neck up over the back of the skull. When these nerves become irritated or compressed, they cause shooting, electrical pain and tingling that radiates from the base of the skull up over the back and top of the head.
According to Johns Hopkins Medicine, the pain is often described as a sharp, jabbing, or electric-shock sensation similar to trigeminal neuralgia, but on the scalp instead of the face. It can be triggered by neck movements, pressure on the back of the head (like resting against a headboard), or muscle tension.
Common causes of occipital neuralgia include neck muscle tension, cervical spine arthritis, whiplash injuries, and nerve entrapment from tight neck muscles.
Cervical Spine Issues
The nerves supplying your scalp originate in the upper cervical spine (C2 and C3 vertebrae). Disc herniations, bone spurs, or arthritis in the cervical spine can compress or irritate these nerve roots, sending tingling, burning, or shooting pain up into the scalp.
Cervical-related scalp symptoms tend to be one-sided, may worsen with certain neck positions, and are often accompanied by neck pain or stiffness. If your scalp tingling changes when you turn or tilt your head, cervical involvement should be investigated.
Shingles (Herpes Zoster)
Shingles can affect the scalp when the varicella-zoster virus reactivates in the trigeminal nerve (V1 branch) or the cervical nerve roots. Scalp shingles typically produces a distinctive rash, but the burning and tingling can precede the rash by several days — during which it may be mistaken for neuropathy.
After the rash heals, some people develop post-herpetic neuralgia — ongoing nerve pain in the area where shingles occurred. This can cause persistent burning and tingling on the scalp that lasts months or even years after the initial infection.
Stress and Anxiety
Stress and anxiety can cause genuine scalp tingling through muscle tension (which compresses nerves), hyperventilation (which changes blood CO2 levels and triggers tingling), and central sensitization (where the nervous system becomes hyper-reactive to normal sensations). This doesn't mean the tingling is “in your head” — the physical sensations are real, even when the trigger is emotional.
Stress-related scalp tingling is often diffuse (affecting the whole scalp rather than a specific area), fluctuates with anxiety levels, and may be accompanied by other stress symptoms like jaw clenching, neck tension, or headaches.
Other Causes
- Giant cell arteritis (GCA) — an inflammatory condition of the blood vessels affecting people over 50, causing scalp tenderness, headaches, and jaw pain. Requires urgent treatment to prevent vision loss.
- Fibromyalgia — can cause allodynia (pain from normally non-painful touch) across the scalp
- Medication side effects — some medications can cause scalp paresthesias
- Vitamin deficiencies — particularly B12, iron, and zinc deficiency can contribute to scalp nerve dysfunction
- Alopecia areata — this autoimmune hair loss condition sometimes causes burning or tingling before or during hair loss episodes
Is Your Neuropathy Spreading to Your Head?
This is the question I hear most often from our community members. If you already have peripheral neuropathy in your feet and hands, scalp symptoms can feel terrifying — like the condition is marching upward toward your brain.

Reassuring Fact
Scalp neuropathy does NOT mean your brain is being affected. The nerves in your scalp are peripheral nerves — the same type as the ones in your feet and hands. Even if your neuropathy is spreading to the scalp, this is still a peripheral nerve issue, not a central nervous system problem.
Here's the reassuring reality: scalp neuropathy does not mean your brain is being affected. The nerves in your scalp are peripheral nerves, just like the ones in your feet and hands. Even if your neuropathy is progressing to involve the scalp, this is still a peripheral nerve issue — not a central nervous system problem.
That said, scalp involvement can indicate that your underlying neuropathy is more widespread than initially thought. It's worth mentioning to your neurologist because it may change the diagnostic workup. Conditions that tend to cause widespread neuropathy (including the scalp) include:
- Small fiber neuropathy (especially autoimmune-mediated)
- Diabetic neuropathy (advanced)
- Vitamin B12 deficiency (which affects central and peripheral nerves)
- Systemic autoimmune conditions (lupus, Sjögren's syndrome)
- Post-COVID neuropathy
The bottom line: scalp tingling deserves medical attention, but it's not a sign of brain damage or impending neurological catastrophe. It's the same type of nerve dysfunction that's happening elsewhere — just in a location that feels scarier because it's on your head.
Diagnosis: What Tests to Expect
Getting a diagnosis for scalp neuropathy can be frustrating because many doctors aren't familiar with it. Dermatologists may focus on skin conditions (which you may not have), while neurologists may focus on the extremities. Here's what a thorough evaluation should include:
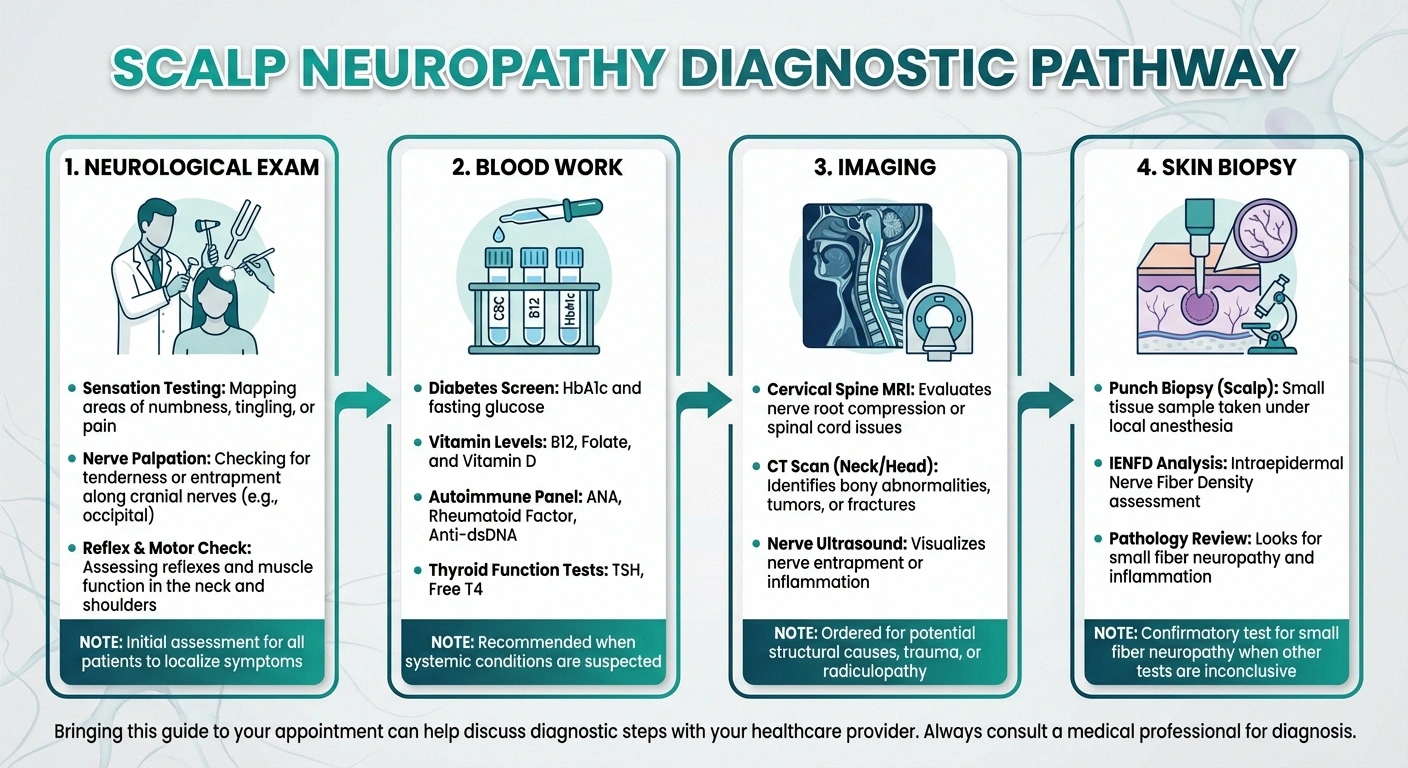
Neurological Examination
Your neurologist should test scalp sensation — light touch, pinprick, and temperature — in all nerve distribution areas. They should also assess neck range of motion, check for Tinel's sign over the occipital nerves (tapping the nerve to reproduce symptoms), and look for trigger points in the neck muscles.
Blood Work
Standard neuropathy blood panel: HbA1c, B12 with methylmalonic acid, thyroid function, CBC, ESR and CRP (inflammation markers, especially important to rule out giant cell arteritis if you're over 50), ANA (for autoimmune causes), iron studies, and zinc level.
Imaging
If cervical spine involvement is suspected, an MRI of the cervical spine can evaluate for disc herniations, bone spurs, or nerve root compression. Brain MRI is generally not needed for isolated scalp symptoms unless other neurological signs suggest a central cause.
Skin Biopsy
A scalp skin biopsy (punch biopsy) can measure nerve fiber density in the scalp, similar to the diagnostic biopsies done on the leg for small fiber neuropathy. This is not routinely performed but may be helpful in confirming neuropathic rather than dermatological causes.
Treatment Options for Scalp Neuropathy
Treatment depends on the underlying cause. When a specific cause is identified and treated — correcting B12 deficiency, treating an autoimmune condition, decompressing a cervical nerve root — scalp symptoms often improve significantly.
Medications
The same medications used for neuropathy elsewhere in the body may help scalp symptoms:
- Gabapentin or pregabalin — first-line neuropathic pain medications
- Duloxetine or amitriptyline — antidepressants with neuropathic pain benefits
- Topical lidocaine — can be applied directly to the scalp for localized relief
- Topical capsaicin — depletes substance P from nerve endings, reducing pain signals over time
For occipital neuralgia specifically, occipital nerve blocks (injections of local anesthetic and corticosteroid near the occipital nerves) can provide significant relief lasting weeks to months.
Lifestyle and Home Remedies
- Gentle scalp massage — may help by improving circulation and reducing muscle tension around the nerves. Use gentle pressure and avoid vigorous rubbing that could irritate sensitive skin.
- Cool compresses — a cool (not ice-cold) cloth on the scalp can provide temporary relief from burning
- Stress reduction — since stress can trigger and worsen scalp symptoms, practices like mindfulness meditation may help
- Gentle hair care — avoid tight hairstyles, harsh chemicals, and rough brushing. Use a soft-bristle brush and gentle, fragrance-free shampoo.
- Neck stretches and posture correction — if cervical tension is contributing, regular neck stretches and ergonomic adjustments can reduce nerve compression
- Heat therapy for neck muscles — warm compresses on the upper neck (not the scalp itself) can relax tight muscles that may be compressing the occipital nerves
Supplements That May Help
If nutritional deficiencies are contributing to your scalp neuropathy, targeted supplementation may help. Always confirm a deficiency with blood work before supplementing:

Quick Relief Strategies
🧊 Cool Compress
Apply a cool (not ice-cold) cloth to the scalp for temporary burning relief.
🧘 Stress Reduction
Mindfulness and relaxation techniques can reduce stress-triggered scalp symptoms.
💆 Gentle Scalp Massage
Improves circulation and reduces muscle tension around scalp nerves. Use light pressure.
- Vitamin B12 — if levels are below 400 pg/mL with neurological symptoms
- Magnesium — may help with nerve signaling and muscle tension
- Alpha-lipoic acid — antioxidant with evidence for neuropathic pain relief
- Zinc — if deficiency is documented, supplementation may support nerve health
For a comprehensive overview, see our complete supplement guide for nerve health.
When to See a Doctor Urgently
Most scalp neuropathy is uncomfortable but not dangerous. However, certain symptoms require prompt medical attention:
Urgent: Giant Cell Arteritis
If you're over 50 and experience sudden, severe scalp tenderness with headache and jaw pain — see a doctor urgently. Giant cell arteritis (GCA) requires emergency steroid treatment to prevent permanent vision loss. This condition can cause blindness if not treated quickly.
- Sudden, severe scalp tenderness with headache in someone over 50 — may indicate giant cell arteritis (GCA), which requires emergency steroid treatment to prevent permanent vision loss. GCA can cause blindness if untreated.
- Scalp burning with a developing rash — may be shingles, which responds best to antiviral medication started within 72 hours
- Scalp symptoms with vision changes, weakness, or confusion — suggests a central nervous system cause that needs urgent evaluation
- Rapidly progressive numbness spreading down the body — may indicate a spinal cord problem requiring immediate attention
Living with Scalp Neuropathy
For many people, scalp neuropathy becomes a chronic condition that waxes and wanes. Learning to manage it — both physically and emotionally — is part of the journey. Some practical tips from our community:

- Choose your hat materials carefully. Soft, breathable fabrics like cotton or bamboo are less irritating than synthetic materials or wool.
- Sleep on a silk or satin pillowcase. The smooth surface creates less friction against a sensitive scalp.
- Keep a symptom diary. Track what triggers your scalp symptoms — stress, weather changes, certain foods, sleep quality — so you can identify and avoid patterns.
- Be upfront with your hairdresser. Let them know about your scalp sensitivity so they can adjust their techniques, avoid harsh chemicals, and use gentle water temperature.
- Give yourself permission to be bothered by it. Scalp neuropathy is invisible to others, which can make it feel isolating. Our support community includes others who understand exactly what this feels like.
Frequently Asked Questions
Can neuropathy in the feet spread to the scalp?
Neuropathy does not literally spread from one area to another like an infection. However, the underlying condition causing your neuropathy — such as diabetes, autoimmune disease, or small fiber neuropathy — can affect nerves throughout the body, including the scalp. If you already have neuropathy in your feet and develop scalp symptoms, it likely means the same systemic process is affecting a wider distribution of nerves. This is worth discussing with your neurologist to reassess the underlying cause.
Does scalp tingling mean I have a brain tumor?
Scalp tingling alone is very rarely caused by a brain tumor. Brain tumors typically cause symptoms related to brain function — seizures, personality changes, visual disturbances, weakness on one side of the body, or severe headaches with nausea. The nerves that supply scalp sensation are peripheral nerves, not brain structures. If your only symptom is scalp tingling with no other neurological symptoms, a brain tumor is extremely unlikely as the cause.
Why does my scalp burn even though it looks completely normal?
This is the hallmark of neuropathic pain — the nerves themselves are malfunctioning and sending pain signals even though there is no visible damage to the skin. In neuropathy, the small sensory nerve fibers fire inappropriately, creating sensations of burning, tingling, or itching without any external cause. This is different from a skin condition, where you would see redness, scaling, or inflammation. The fact that your scalp looks normal but feels abnormal actually points toward a neuropathic cause.
Is occipital neuralgia the same as scalp neuropathy?
Not exactly. Occipital neuralgia is one specific cause of scalp neuropathy involving the occipital nerves at the back of the head. Scalp neuropathy is a broader term that includes any nerve dysfunction affecting the scalp, from any cause. Occipital neuralgia tends to cause sharp, shooting pain starting at the base of the skull, while other forms of scalp neuropathy may cause diffuse burning or tingling across larger areas. Both are treatable, but the approaches differ.
Can stress alone cause scalp tingling?
Yes. Stress and anxiety can cause genuine scalp tingling through several mechanisms: muscle tension in the neck and scalp that compresses nerves, hyperventilation that changes blood chemistry and triggers paresthesias, and central sensitization that amplifies normal nerve signals into perceived tingling. The tingling is physically real even when the trigger is emotional. If your scalp tingling correlates strongly with periods of stress and has no other neurological symptoms, stress is a likely contributor.
What type of doctor should I see for scalp neuropathy?
Start with your primary care doctor for initial evaluation and blood work. If a neurological cause is suspected, a neurologist is the most appropriate specialist. For occipital neuralgia specifically, neurologists and pain management specialists can perform diagnostic and therapeutic nerve blocks. If you are over 50 with new scalp tenderness and headaches, see your doctor urgently to rule out giant cell arteritis, which needs immediate treatment.
The Bottom Line
Scalp neuropathy is real, it's more common than most people think, and it's treatable. The fact that it's on your head can make it feel scarier than neuropathy elsewhere, but the same principles apply: identify the underlying cause, treat it if possible, and manage symptoms with the right combination of medication and lifestyle adjustments.
Don't let anyone dismiss your scalp symptoms as “just stress” without proper testing, but also don't panic — scalp tingling is a peripheral nerve issue, not a sign of brain damage. Get the blood work, see a neurologist if needed, and know that effective treatments exist.
For more on understanding how neuropathy affects different parts of the body, explore our guides on neuropathy in hands, neuropathy in feet, and neuropathic itch — a closely related condition that many people with scalp neuropathy also experience.


