
It started with a strange feeling — like I was always wearing invisible socks. Then came the pins and needles that never quite went away. Eventually, the burning set in, turning simple things like walking across a cold floor into something I dreaded. If any of this sounds familiar, you're not alone, and you've come to the right place.
Neuropathy in the feet is one of the most common forms of peripheral neuropathy, and there's a reason it hits our feet first. The nerves traveling from your spine to your toes are the longest in your body — sometimes over three feet long — making them the most vulnerable to damage. When something goes wrong with nerve health, these distant endpoints are usually the first to show it.
An estimated twenty to thirty percent of Americans will experience some form of neuropathy in their lifetime, with the feet being the most frequently affected area. In this guide, I'll share everything I've learned about foot neuropathy — the symptoms to watch for, the causes your doctor should investigate, and the relief strategies that actually make a difference.
What Does Neuropathy in Feet Actually Feel Like?
One of the hardest things about foot neuropathy is describing it to someone who hasn't experienced it. The sensations are strange, sometimes contradictory, and they can change from day to day. Here's what the neuropathy community most commonly reports — and what I've felt myself:
of Americans will experience neuropathy — with the feet affected first in most cases
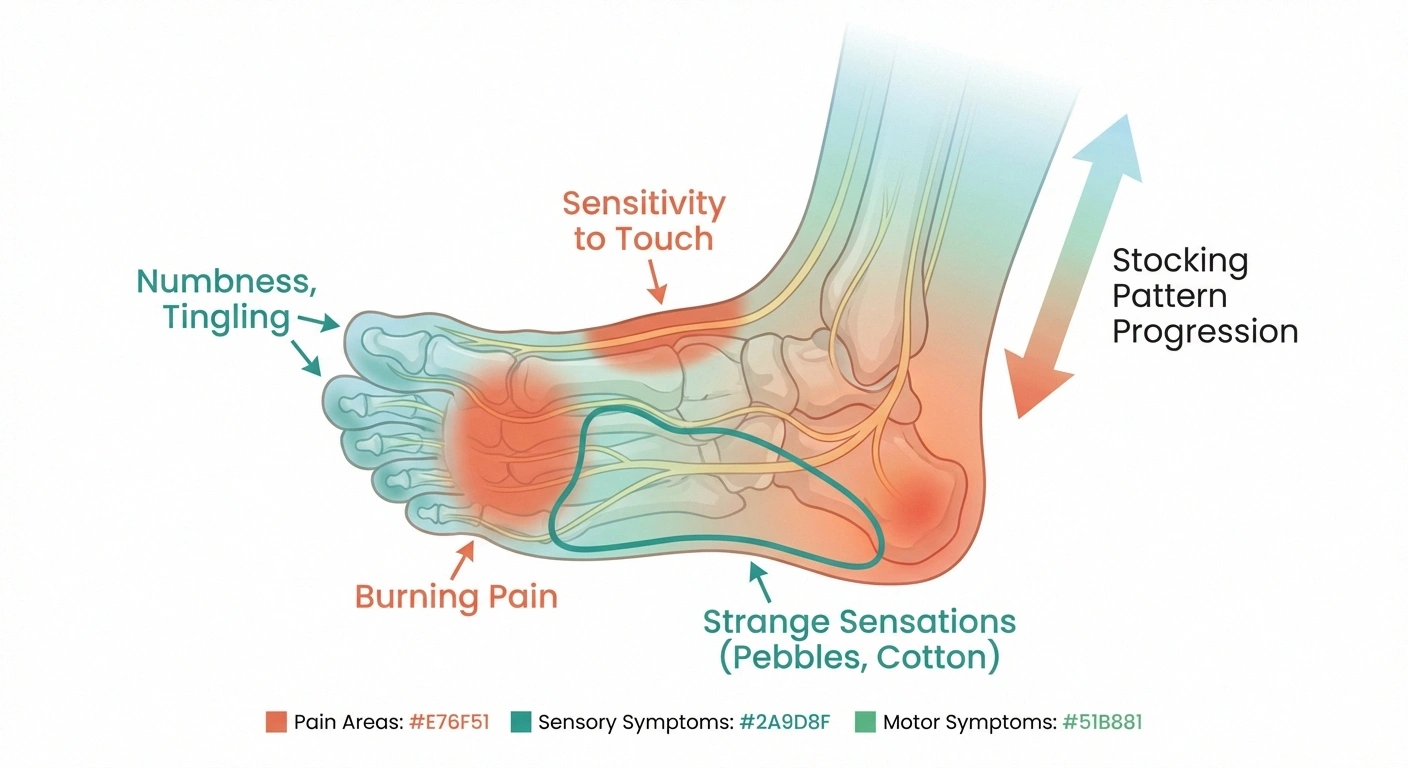
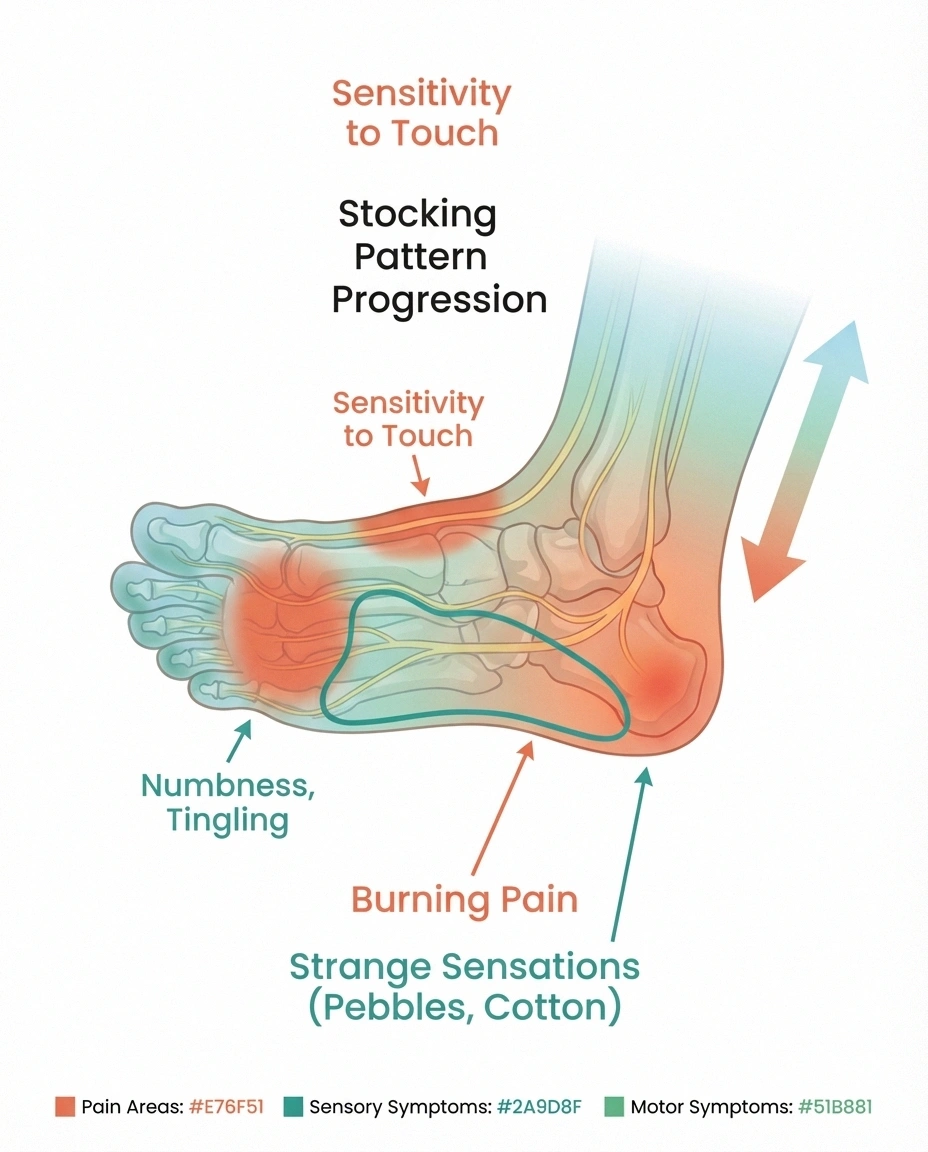
Numbness and loss of sensation: This often starts in the toes and gradually spreads. You may notice you can't feel the texture of carpet beneath your feet or that you're less aware of temperature changes. Some people describe it as walking on cotton balls or through deep sand. This numbness is more than uncomfortable — it's a safety concern because you may not feel cuts, blisters, or injuries on your feet.
Tingling and pins-and-needles: That prickling sensation you get when your foot “falls asleep” — except it doesn't go away. For many people, this is the earliest sign of foot neuropathy. It may come and go at first, then gradually become constant. It's especially common in the toes and the ball of the foot.
Burning pain: Perhaps the most distressing symptom. A persistent, hot, burning sensation in the feet that's often worse at night when you're trying to sleep. The burning may feel like your feet are on fire or like you're walking on hot coals. This happens because damaged nerves send faulty pain signals to your brain even when there's nothing actually harming your feet.
Sharp, shooting, or electric-shock pain: Sudden jolts of intense pain that come without warning. These can be triggered by light touch — even the weight of a bedsheet — or they may strike randomly. This extreme sensitivity to touch is called allodynia, and it's one of the most disruptive symptoms of foot neuropathy.
Strange sensations: Many people report feeling like they're wearing socks when they're barefoot, stepping on pebbles on a smooth floor, or experiencing a “tightness” or “squeezing” around their feet. These abnormal sensations, called dysesthesias, are a hallmark of nerve damage.
Beyond Sensation: Motor and Autonomic Symptoms
Foot neuropathy isn't just about strange feelings. As nerve damage progresses, it can affect the muscles in your feet and the autonomic functions that keep your feet healthy:
Do You Recognize These Signs?
Persistent numbness or tingling in toes that won't go away
Burning sensation in feet, especially at night
Sharp or electric-shock-like pain in feet
Feeling like you're wearing socks when you're barefoot
Difficulty with balance or unsteady walking
Excessively dry feet or changes in skin color
Cuts or blisters on feet that heal slowly
If you checked 2 or more, consider scheduling an evaluation with your doctor or neurologist.
Muscle weakness and foot drop: Damaged motor nerves can weaken the muscles in your feet, making it difficult to lift the front of your foot when walking — a condition called foot drop. You may find yourself tripping more often or adopting a high-stepping gait to compensate. Over time, muscle wasting can change the shape of your feet.
Balance problems: Your feet are your body's primary balance sensors. When the nerves in your feet can't accurately report your position and the surface beneath you, balance becomes unreliable. Falls are a serious concern — research shows that people with foot neuropathy have a significantly higher fall risk than those without it.
Autonomic changes: The nerves that control sweating, blood flow, and skin health in your walking aids for foot neuropathy can also be affected. This may cause excessively dry feet, skin color changes, temperature fluctuations, and — most concerning — slow wound healing. For people with diabetes, impaired wound healing in the feet can lead to serious complications.
What Causes Neuropathy in the Feet?
Understanding what's causing your foot neuropathy is the single most important step toward managing it effectively. The cause determines the treatment, the prognosis, and — in some cases — whether the damage can be reversed. Here are the most common culprits:
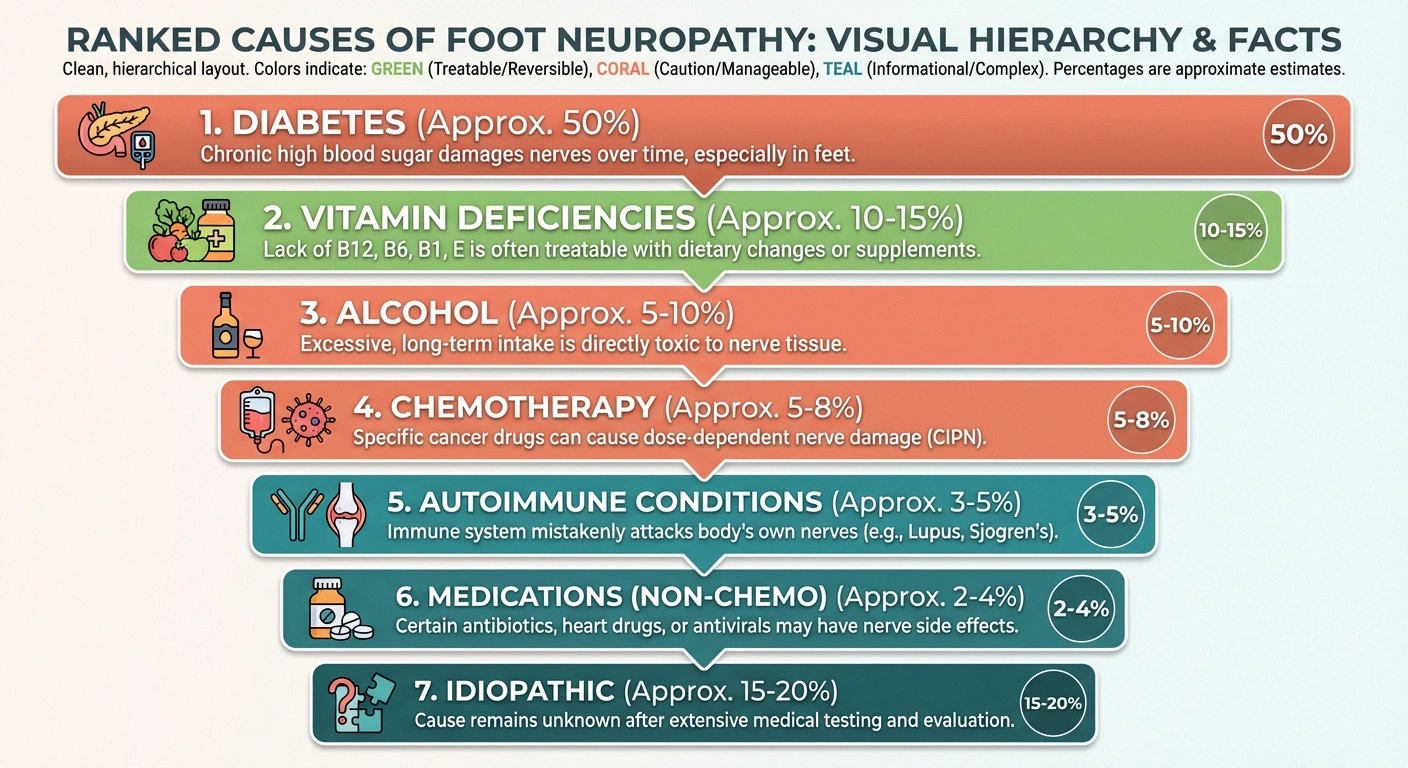

Diabetes and prediabetes: Diabetes is the leading cause of peripheral neuropathy in developed countries. Approximately fifty percent of people with diabetes will develop some form of neuropathy, with the feet almost always affected first. Chronically elevated blood sugar damages the small blood vessels that nourish nerves, gradually starving them of oxygen and nutrients. What many people don't realize is that nerve damage can begin during the prediabetes stage — before you've even received a diabetes diagnosis. Tight blood sugar control can slow progression and, in some cases, improve symptoms.
Vitamin deficiencies: Several vitamins are essential for nerve health, and falling short can directly cause foot neuropathy. Vitamin B12 deficiency is the most common nutritional cause and is particularly prevalent in older adults, vegetarians, and people taking certain medications like metformin or proton pump inhibitors. The good news: B12-related neuropathy can be fully reversible with treatment if caught early. Vitamins B1 (thiamine), B6, and E deficiencies can also contribute.
Alcohol use: Chronic alcohol consumption damages nerves through both direct toxic effects and the nutritional deficiencies that often accompany heavy drinking. Alcoholic neuropathy typically starts in the feet and may improve with abstinence and nutritional supplementation.
Chemotherapy: Chemotherapy-induced peripheral neuropathy (CIPN) is a common side effect of many cancer treatments, particularly platinum-based drugs, taxanes, and vinca alkaloids. It often starts in the feet during treatment and may persist for months or years after chemotherapy ends.
Autoimmune conditions: Diseases like Guillain-Barré syndrome, chronic inflammatory demyelinating polyneuropathy (CIDP), lupus, and rheumatoid arthritis can cause the immune system to attack the nerves themselves. These forms are often treatable with immunotherapy.
Thyroid disorders: Both underactive and overactive thyroid conditions have been linked to peripheral neuropathy. Hypothyroidism is the more common culprit, causing fluid retention that can compress nerves.
Medications: Beyond chemotherapy, several common medications can cause neuropathy as a side effect, including certain antibiotics (fluoroquinolones, metronidazole), statins, and some HIV medications.
Idiopathic neuropathy: In roughly twenty-five to thirty percent of cases, no specific cause is found despite thorough testing. This is called idiopathic neuropathy, and while the label can be frustrating, it doesn't mean nothing can be done about the symptoms.
When Should You See a Doctor?
If you're experiencing any of the symptoms described above, a medical evaluation is important. But certain situations call for urgency:
Seek Immediate Medical Attention
If you develop rapid weakness in your legs along with spreading numbness, seek emergency care immediately. These symptoms could indicate Guillain-Barré syndrome, a treatable but urgent condition that requires prompt intervention.
See your doctor soon if: You notice persistent numbness, tingling, or burning in your feet that lasts more than a few weeks. Early evaluation gives you the best chance of identifying a treatable cause and preventing further damage. Your doctor can refer you to a neurologist and order the appropriate tests.
Seek urgent medical attention if: You develop rapid weakness in your feet or legs (progressing over days rather than weeks), experience sudden inability to lift your foot, or notice numbness rapidly spreading up your legs. These could signal Guillain-Barré syndrome or another acute inflammatory condition that requires emergency treatment.
If you have diabetes: Any foot wound, blister, or sore that doesn't heal normally warrants immediate medical attention. Neuropathy-related foot complications are the leading cause of non-traumatic amputations, but they're largely preventable with early intervention.
Getting a Diagnosis: What Tests to Expect
Diagnosing foot neuropathy involves several steps, and understanding the process can help you feel more prepared. Your evaluation will likely include:

Your Diagnostic Journey
Neurological Exam
Sensation testing with monofilament, vibration, and temperature. Reflex and strength checks.
Blood Work
Screening for diabetes, vitamin deficiencies, thyroid issues, autoimmune markers, and more.
Nerve Conduction Studies & EMG
Electrical tests measuring nerve signal speed and strength. Gold standard for large fiber neuropathy.
Skin Biopsy (If Needed)
Definitive test for small fiber neuropathy when standard tests are normal but symptoms persist.
Neurological examination: Your doctor will test sensation in your feet using a monofilament (a thin nylon fiber), vibrating tuning fork, and temperature testing. They'll also check your reflexes (often reduced in neuropathy) and assess muscle strength. This basic exam can tell a lot about which types of nerve fibers are affected.
Nerve conduction studies and EMG: These electrical tests measure how well and how fast your nerves conduct signals. They're the gold standard for diagnosing large fiber neuropathy and can help determine the type, severity, and pattern of nerve damage. The tests involve mild electrical stimulation and thin needles — uncomfortable but not unbearable.
Blood work: A comprehensive panel will screen for common causes: blood sugar and HbA1c (diabetes), vitamin B12 and other B vitamins, thyroid function, kidney and liver function, inflammatory markers, and specific autoimmune antibodies. These tests are crucial because many causes of foot neuropathy are treatable once identified.
Skin biopsy for small fiber neuropathy: If your symptoms are significant but nerve conduction studies come back normal, you may have small fiber neuropathy. A small skin biopsy — typically a painless punch biopsy from your ankle — can measure the density of small nerve fibers and provide a definitive diagnosis.
Treatment: Addressing the Root Cause
The most important treatment for foot neuropathy isn't a pain medication — it's addressing whatever is damaging your nerves in the first place:
Key Takeaway
The most important treatment for foot neuropathy isn't a pain medication — it's identifying and treating the underlying cause. Vitamin deficiencies, uncontrolled blood sugar, and medication side effects are all reversible or manageable causes that can be addressed with proper testing.
Blood sugar control: For diabetic and prediabetic neuropathy, tightening glucose control is essential. This may involve medication adjustments, dietary changes, and regular monitoring. Some patients experience improvement in neuropathy symptoms when HbA1c levels are brought down to target range.
Vitamin supplementation: If a deficiency is identified, supplementation can stop progression and sometimes reverse damage. B12 injections work faster than oral supplements for severe deficiency. Alpha-lipoic acid has shown promise for diabetic neuropathy specifically.
Stopping the offending agent: If medications are causing your neuropathy, your doctor may be able to switch you to alternatives. If alcohol is the cause, abstinence combined with nutritional support gives your nerves the best chance of recovery.
Immunotherapy: For autoimmune-related neuropathies, treatments like intravenous immunoglobulin (IVIg), plasma exchange, or immunosuppressive medications can reduce inflammation and protect nerves from further immune-mediated damage.
Managing Foot Neuropathy Pain
While addressing the underlying cause is the priority, most people also need strategies to manage the pain and discomfort of foot neuropathy. Here's what the evidence supports:
Oral medications: The first-line medications for neuropathic foot pain include gabapentin, pregabalin, and duloxetine. Each works differently and suits different patients. Amitriptyline, an older tricyclic antidepressant, is also effective and inexpensive. Finding the right medication often takes trial and adjustment — be patient with the process.
Topical treatments: Capsaicin cream, lidocaine patches, and other topical creams can provide localized relief with fewer systemic side effects than oral medications. These work particularly well for foot neuropathy because the pain is accessible on the skin surface.
Physical therapy and strength training: Physical therapy can improve balance, strengthen foot and leg muscles, and reduce fall risk. Gentle exercises like toe curls, heel raises, and ankle circles help maintain foot mobility. Regular walking, swimming, and yoga all show benefits for neuropathy symptoms and overall nerve health.
TENS therapy: Transcutaneous electrical nerve stimulation uses mild electrical currents to disrupt pain signals. Many people find it helpful for foot pain, and home TENS units are widely available and affordable.
Complementary approaches: Acupuncture, foot massage, warm foot soaks, and essential oils may provide additional comfort alongside conventional treatments. While the evidence varies, these approaches carry minimal risk and many people find them helpful.
Daily Foot Care: Protecting Numb Feet
When you can't fully feel your feet, daily care becomes critically important. Proper foot care prevents the small injuries that can become serious problems:

❌ Without Daily Care
Unnoticed cuts and blisters, infections, falls from balance problems, progressive muscle weakness, and — in severe cases — foot deformities or amputations.
✓ With Consistent Care
Early detection of skin changes, prevented infections, reduced fall risk through balance exercises, maintained mobility, and preserved foot health for years to come.
Inspect your feet daily. Look at the tops, bottoms, heels, and between the toes for cuts, blisters, redness, swelling, or any changes. Use a mirror to see the bottoms if flexibility is limited. Make this a non-negotiable part of your routine.
Wear proper footwear. Supportive shoes with wide toe boxes protect against pressure points and injuries. Never walk barefoot — not even indoors. Check inside your shoes before putting them on to make sure there's nothing that could cause a wound you wouldn't feel.
Keep skin healthy. Moisturize your feet daily to prevent cracking, but avoid lotion between the toes (it can promote fungal growth). Trim toenails straight across to prevent ingrown nails. If you have diabetes, consider seeing a podiatrist for nail care.
Test water temperature. Numb feet can't accurately sense heat. Always test bath and shower water with your hand or elbow before stepping in. Burns from water that's too hot are a common and preventable complication.
Manage swelling. Elevate your feet when sitting and consider compression socks if edema is an issue. Swelling can worsen nerve compression and increase pain.
Lifestyle Strategies That Support Nerve Health
Beyond medical treatments, your daily choices play a significant role in how foot neuropathy affects your life:

Anti-inflammatory nutrition: A nerve-supporting diet rich in fruits, vegetables, whole grains, lean proteins, and omega-3 fatty acids while limiting processed foods, sugar, and inflammatory triggers can help reduce nerve inflammation. Several studies suggest that the Mediterranean dietary pattern may benefit people with neuropathy.
Targeted supplements: Beyond correcting deficiencies, certain supplements may support nerve health. Alpha-lipoic acid (600 mg daily) has the most evidence for diabetic neuropathy. Magnesium, acetyl-L-carnitine, and omega-3 fatty acids also show promise. Always discuss supplements with your doctor, especially if you take other medications.
Sleep optimization: Neuropathy pain and poor sleep create a vicious cycle — pain disrupts sleep, and sleep deprivation increases pain sensitivity. Establish a consistent bedtime routine, keep your bedroom cool, and talk to your doctor if nighttime pain is significantly affecting your rest.
Stress management: Chronic stress amplifies pain perception through elevated cortisol and inflammatory pathways. Mindfulness, meditation, gentle yoga, and deep breathing exercises can help break the stress-pain connection. Many people in our community report that addressing the emotional aspects of living with neuropathy improves their physical symptoms too.
Quit smoking: Smoking constricts blood vessels, reduces oxygen delivery to nerves, and increases inflammation. Research suggests smoking independently increases neuropathy risk by nearly one hundred fifty percent. Quitting — at any point — reduces these harmful effects.
Frequently Asked Questions
Can neuropathy in the feet be reversed?
It depends on the cause and how early treatment begins. Neuropathy caused by vitamin deficiencies, especially B12, can often be fully reversed with supplementation if caught early. Diabetic neuropathy progression can be slowed or stopped with tight blood sugar control, though existing damage is harder to reverse. Neuropathy from medications often improves after the offending drug is stopped. The key is early diagnosis and addressing the root cause.
Why is neuropathy in my feet worse at night?
Nighttime worsening is extremely common. Several factors contribute: fewer daytime distractions mean you notice pain more, lying down changes blood flow patterns to the feet, body temperature drops slightly at night which can affect nerve signaling, and cortisol levels naturally decrease in the evening, reducing your body's natural anti-inflammatory response. Bedtime routines like warm foot soaks, gentle massage, and lidocaine patches can help.
What is the difference between neuropathy and poor circulation in the feet?
Neuropathy involves damage to the nerves themselves, causing numbness, tingling, burning, and pain. Poor circulation (peripheral vascular disease) involves reduced blood flow to the feet, causing cold feet, color changes, cramping with walking, and slow wound healing. The two conditions often coexist, especially in people with diabetes, but they require different treatments. Your doctor can distinguish between them with appropriate testing.
Should I see a neurologist or a podiatrist for foot neuropathy?
Ideally, both. A neurologist can diagnose the type of neuropathy, identify the underlying cause, and prescribe appropriate medications. A podiatrist specializes in foot care and can help with protective footwear, wound prevention, nail care, and monitoring for complications. Many people with foot neuropathy benefit from a team approach that includes both specialists.
Is neuropathy in the feet a sign of something serious?
Foot neuropathy is always worth investigating because it can signal underlying conditions that need treatment — diabetes, vitamin deficiencies, autoimmune diseases, or thyroid problems. The neuropathy itself also requires management to prevent complications like falls and foot injuries. While the condition is manageable for most people, ignoring it can lead to progressive damage and quality of life decline.
Can exercise make foot neuropathy worse?
Appropriate exercise generally improves neuropathy symptoms rather than worsening them. Low-impact activities like walking, swimming, and cycling promote blood flow to nerves, reduce inflammation, and improve balance. However, high-impact activities or exercises that put excessive pressure on numb feet can cause injuries you might not feel. Start gradually, wear proper footwear, and check your feet after exercise for any signs of injury.
Living Well With Foot Neuropathy
Foot neuropathy changes how you move through the world — literally. But it doesn't have to define your life. The combination of identifying and treating the underlying cause, managing symptoms effectively, protecting your feet daily, and supporting your nerve health through lifestyle choices gives you a powerful toolkit.

I've lived with foot neuropathy for years, and I won't pretend it's easy. There are bad days when the burning seems relentless and good days when I almost forget about it. The difference between those days often comes down to how consistently I follow my management routine — the foot care, the exercise, the nutrition, the medications working in the background.
If you're newly diagnosed, take a breath. There are more options than you think. If you've been managing this for years, don't stop exploring new approaches — the science keeps advancing, and what didn't work before might work differently in combination with something new.
Your feet carry you through life. They deserve your attention and care, now more than ever.


