
Foods That Trigger Neuropathy Pain: What to Avoid and Why
I still remember the afternoon I ate a plate of birthday cake and fried appetizers at my niece's party, then spent the rest of the evening with my feet burning like they were on hot coals. At the time, I chalked it up to a bad day. But after it happened again—and again—I started connecting the dots between what I was eating and how my nerves were reacting.
If you live with peripheral neuropathy, you already know that symptoms can fluctuate from day to day. What many people don't realize is that certain foods may be quietly making those symptoms worse. Not because the food directly “damages” your nerves in a single meal, but because specific dietary patterns fuel the very processes—inflammation, blood sugar spikes, nutrient depletion—that drive nerve damage forward.
This isn't about perfection or giving up everything you enjoy. It's about understanding which foods are most likely to trigger flare-ups so you can make informed choices. Let's walk through the biggest offenders, the science behind why they hurt, and what you can reach for instead.
How Food Affects Your Nerves
Before we get into specific foods, it helps to understand the three main pathways through which diet influences neuropathy symptoms:
Blood sugar spikes, chronic inflammation, and nutrient depletion — the three ways food worsens neuropathy
Blood sugar dysregulation. When blood glucose spikes rapidly, it creates oxidative stress that damages small nerve fibers. This is the primary mechanism behind diabetic neuropathy, but it affects anyone with neuropathy—even without a diabetes diagnosis. A study published in Clinical Autonomic Research found that dietary and exercise interventions not only help prevent diabetic neuropathy but may also improve symptoms in those already affected.
Chronic inflammation. Inflammatory compounds in certain foods activate immune responses that can irritate and damage peripheral nerves. Over time, this systemic inflammation compounds the nerve damage you're already dealing with.
Nutrient depletion. Some foods actively block or deplete the vitamins and minerals your nerves depend on for repair and function—particularly B vitamins, magnesium, and antioxidants.
With those mechanisms in mind, here are the foods most likely to worsen your neuropathy symptoms.
Added Sugars and Sugary Foods
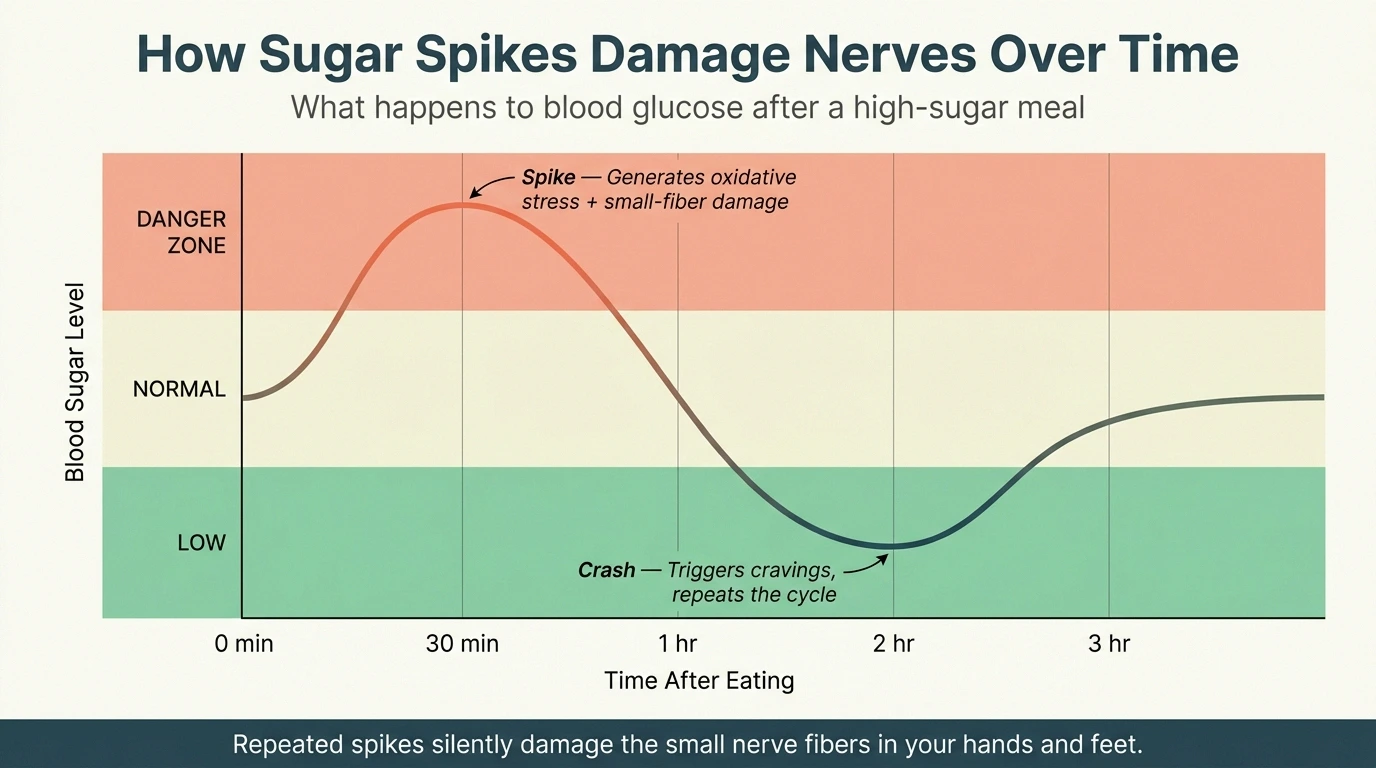
If there's one category of food that consistently worsens neuropathy across the board, it's added sugar. And the mechanism is straightforward: sugar spikes blood glucose, which generates oxidative stress and damages the tiny blood vessels that supply your nerves.
Here's what happens to your blood glucose in the hours after a high-sugar meal — and why repeated spikes silently damage nerves over time:
The damage isn't theoretical. Compare a healthy nerve fiber bed to one degraded by years of glucose spikes — the small fibers that detect sensation in your hands and feet are the first to go:
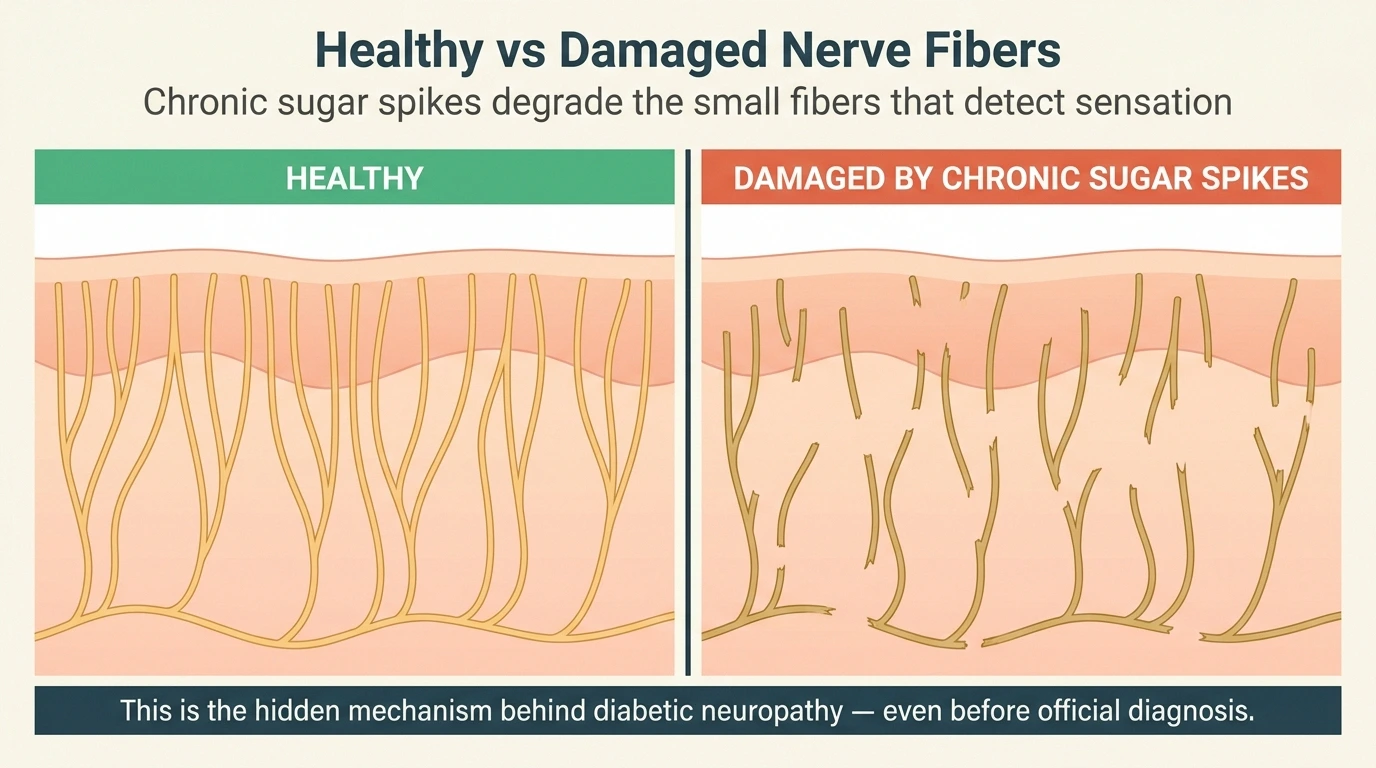
These are the foods most likely to trigger sharp glucose surges. Eliminating them is one of the most direct ways to slow nerve damage:

Hidden Sugar Alert
A single bottle of sweetened iced tea can contain more sugar than a candy bar. Always check nutrition labels — and look for names like high fructose corn syrup, dextrose, maltose, and sucrose. Sugar hides under dozens of names.
This isn't limited to people with diabetes. Research shows that even in people without a diabetes diagnosis, repeated blood sugar spikes can damage small nerve fibers over time. A pilot study funded by the NIH found that participants who followed a low-fat, plant-based diet experienced meaningful reductions in neuropathic pain after just a few months—and one of the biggest changes was the dramatic reduction in sugar intake.
The worst offenders include:
- Sodas and sweetened beverages (including “healthy” fruit juices with added sugar)
- Candy, cookies, cakes, and pastries
- Sugary breakfast cereals and flavored yogurts
- Condiments like ketchup, barbecue sauce, and many salad dressings
- Energy drinks and sweetened coffee beverages
What makes sugar particularly sneaky is how it hides. A single bottle of sweetened iced tea can contain more sugar than a candy bar. Always check nutrition labels—and look for names like high fructose corn syrup, dextrose, maltose, and sucrose.
Better choices: Fresh berries, apples, and pears satisfy sweet cravings with fiber that slows sugar absorption. Herbal teas and sparkling water with a squeeze of citrus replace sugary drinks without the blood sugar impact.
Refined Carbohydrates and White Flour Products
Refined carbohydrates act almost identically to sugar in your body. When grain is processed and stripped of its fiber and nutrients, what remains is essentially a fast-acting glucose delivery system. Your body breaks down white bread, white pasta, and white rice nearly as quickly as it would a spoonful of table sugar.
The result? The same blood sugar spikes, the same oxidative stress, and the same nerve-damaging cascade. According to research on carbohydrate digestion, refined carbohydrates may also contribute to obesity-related conditions like type 2 diabetes—which itself is the leading cause of neuropathy.
Foods to watch for:
- White bread, bagels, and rolls
- Regular pasta (non-whole-grain)
- White rice
- Crackers and pretzels made from refined flour
- Pancakes, waffles, and muffins made with white flour
- Pizza dough
Better choices: Whole-grain bread, brown rice, quinoa, oatmeal, and whole-wheat pasta all provide the fiber that slows glucose absorption and keeps blood sugar steadier. The difference in how you feel may surprise you.
Processed and Ultra-Processed Foods
Highly processed foods are a triple threat for neuropathy. They tend to be high in sodium (which restricts blood flow to nerves), loaded with preservatives and artificial additives (which may trigger inflammation), and nearly devoid of the B vitamins, magnesium, and other nutrients your nerves need to function and repair.

The category includes:
- Frozen prepared meals and TV dinners
- Packaged snack foods (chips, cheese puffs, snack mixes)
- Processed meats like bacon, sausage, hot dogs, and deli slices
- Instant noodles and boxed meal kits
- Fast food in general
One of the most overlooked aspects of processed foods is sodium. High sodium intake contributes to high blood pressure and reduced circulation. When blood flow to your peripheral nerves is restricted, those nerves receive less oxygen and fewer nutrients—a recipe for increased pain and worsened symptoms.
Better choices: Cooking at home more often is the single biggest shift you can make. Even simple meals—baked chicken with roasted vegetables, a bean soup, a salad with grilled fish—give your nerves dramatically better nutrition than anything from a freezer box or drive-through window. For neuropathy-friendly meal ideas, see our guide to the best neuropathy diet.
Fried Foods and Unhealthy Fats
Fried foods and foods high in trans fats or saturated fats are potent drivers of systemic inflammation—which directly worsens nerve pain. Trans fats are particularly damaging: they increase LDL (“bad”) cholesterol, reduce HDL (“good”) cholesterol, and impair circulation throughout your body, including to your peripheral nerves.
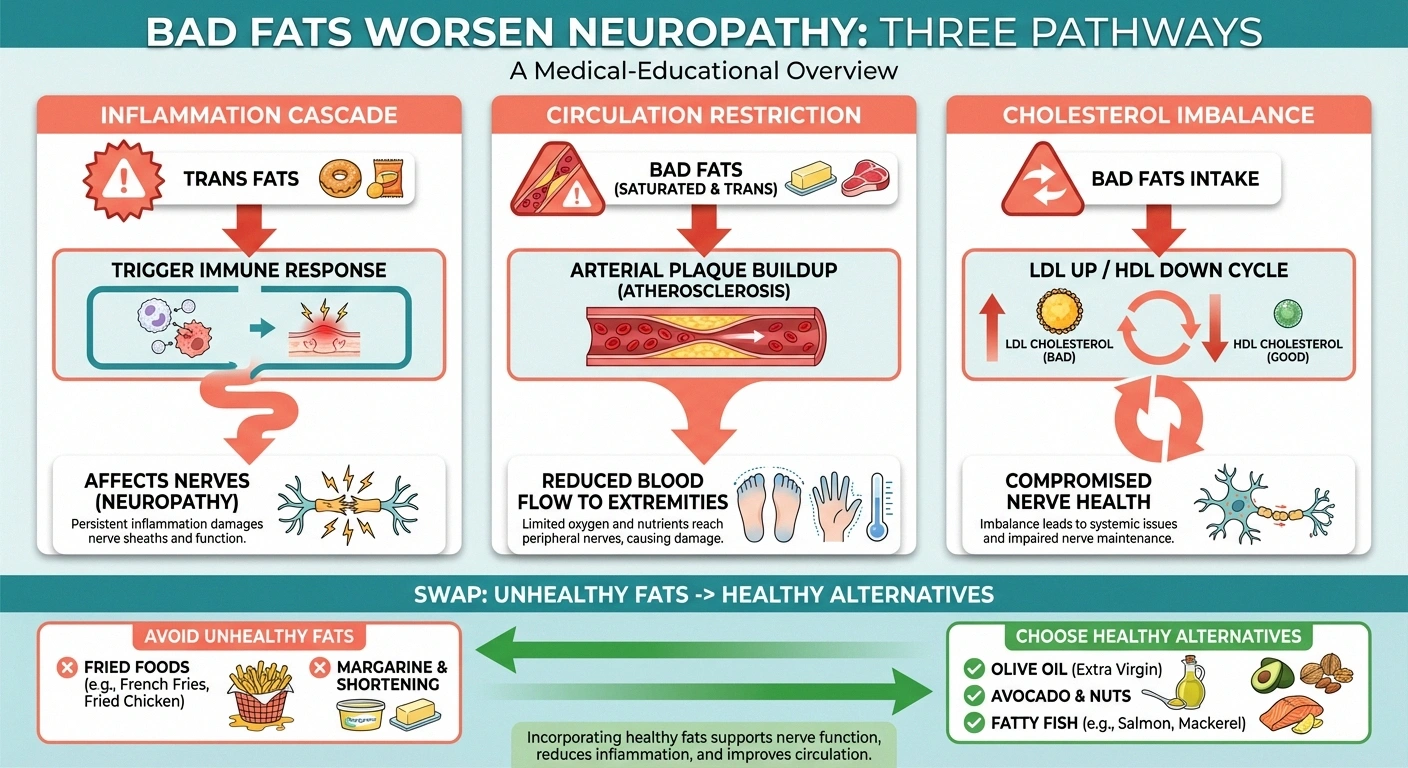

❌ Fats That Hurt Nerves
Trans fats, hydrogenated oils, deep-fried foods, fatty red meat, and processed baked goods. These increase inflammation, raise LDL cholesterol, and restrict blood flow to nerves.
✓ Fats That Help Nerves
Olive oil, avocados, nuts, seeds, and fatty fish like salmon. These reduce inflammation, support nerve regeneration, and provide omega-3 fatty acids.
Foods in this category include:
- Deep-fried foods (french fries, fried chicken, doughnuts, onion rings)
- Commercially baked goods (many contain hydrogenated oils)
- Margarine and shortening containing trans fats
- Fatty cuts of red meat
- Full-fat processed dairy products
The connection between unhealthy fats and neuropathy runs deeper than just inflammation. Poor circulation caused by arterial plaque buildup—fueled by trans and saturated fats—means less blood reaching your extremities, exactly where neuropathy pain tends to concentrate. If you're dealing with burning feet or tingling hands, what you eat may be reducing the blood supply those nerves desperately need.
Better choices: Olive oil, avocados, nuts, seeds, and fatty fish like salmon provide healthy fats that actually reduce inflammation. Omega-3 fatty acids from fish have been shown to support nerve regeneration and calm inflammatory responses.
Alcohol and Neuropathy
Alcohol is uniquely harmful to nerves because it attacks from multiple angles simultaneously. It's directly toxic to peripheral nerve tissue. It depletes vitamin B1 (thiamine)—essential for nerve function. It impairs absorption of B12 and folate. And chronic use can lead to alcoholic neuropathy, a distinct form of nerve damage that can become permanent.
Even moderate drinking can be problematic when you already have nerve damage from another cause. Alcohol lowers your pain threshold, disrupts sleep (already difficult with neuropathy), and can interact with medications like gabapentin and pregabalin commonly prescribed for nerve pain.
If you're not ready to give up alcohol entirely, limiting yourself to one drink on occasion is far better than regular consumption. And if you notice your symptoms worsen after drinking—even a single glass—your nerves may be telling you they need a break.
Gluten (For Some People)
Gluten sensitivity and neuropathy have a more nuanced relationship than many articles suggest. Not everyone with neuropathy needs to go gluten-free. But for a specific subset of people—those with celiac disease or non-celiac gluten sensitivity—gluten can be a direct trigger for nerve damage.

The condition is sometimes called “gluten neuropathy,” and it occurs when the autoimmune response triggered by gluten damages peripheral nerves. Research published in medical journals has documented cases where people with unexplained neuropathy tested positive for anti-gliadin antibodies and experienced significant symptom improvement after adopting a strict gluten-free diet.
You might consider investigating a gluten connection if:
- Your neuropathy has no clear cause (idiopathic peripheral neuropathy)
- You also experience digestive symptoms like bloating, gas, or irregular bowel movements
- You have a family history of celiac disease or autoimmune conditions
- Standard treatments haven't been effective
Talk to your doctor about testing for celiac disease and gluten sensitivity before eliminating gluten on your own. If testing is positive, a gluten-free diet isn't just a dietary preference—it's a treatment.
Gluten-free alternatives: Rice, quinoa, millet, buckwheat, oats (certified gluten-free), and corn-based products.
High-Sodium Foods
Sodium doesn't get as much attention as sugar in neuropathy discussions, but it should. High sodium intake raises blood pressure and reduces circulation—particularly to the small blood vessels that supply your peripheral nerves. When those nerves are already damaged, reduced blood flow means reduced oxygen and nutrients reaching the areas that need them most.
The biggest sources of sodium in the average diet aren't the salt shaker on your table. They're hiding in:
- Canned soups and broths
- Deli meats and cured meats
- Soy sauce and teriyaki sauce
- Potato chips, pretzels, and salted nuts
- Cheese (especially processed cheese)
- Restaurant and takeout food
Better choices: Season with herbs, spices, lemon juice, and vinegar instead of salt. Choose low-sodium versions of canned goods. When eating out, ask for sauces on the side and choose grilled over fried options.
Artificial Sweeteners and Food Additives
This category is more controversial than the others, and the scientific evidence is less conclusive. However, many people with neuropathy report that certain artificial additives seem to trigger or worsen their symptoms.

Aspartame, in particular, has been reported by some patients to worsen nerve pain symptoms—though clinical studies have not consistently confirmed this link. Similarly, monosodium glutamate (MSG) has been associated with reports of increased nerve sensitivity in some individuals.
While the evidence is mixed, the logic is simple: if you notice a pattern between consuming certain artificial ingredients and symptom flares, keeping a food diary can help you identify your personal triggers. Everyone's nervous system responds differently, and your experience is valid data.
Better choices: If you're trying to reduce sugar but want to avoid artificial sweeteners, natural alternatives like stevia, monk fruit, or small amounts of honey may be worth exploring.
Dairy Products (In Some Cases)
Dairy is another food category where individual response matters more than blanket advice. Full-fat dairy products like butter, cream, and aged cheeses are high in saturated fats that can promote inflammation. But dairy also provides calcium, vitamin D, and protein that support overall health.
The people most likely to benefit from reducing dairy are those who:
- Notice increased inflammation or digestive discomfort after consuming dairy
- Have a diagnosed dairy intolerance or sensitivity
- Rely heavily on full-fat dairy as a primary food source
If you're unsure, try a two-week elimination period. Remove all dairy, note your symptom levels, then gradually reintroduce it and see if symptoms change. This is far more informative than guessing.
Better choices: If you reduce dairy, look for calcium-fortified plant milks, leafy greens (a great source of calcium), and consider a vitamin D supplement if needed.
How to Identify Your Personal Trigger Foods
Here's what I've learned after years of managing neuropathy: no two people react to food in exactly the same way. The categories above are backed by science, but your body is the final authority on what triggers your symptoms.

Your Food & Symptom Diary Plan
Track Everything for 2-3 Weeks
Record what you eat, quantities, and timing. Include drinks, condiments, and snacks.
Rate Symptoms Daily (1-10)
Note specific symptoms: burning, tingling, numbness, pain level. Track timing of flare-ups.
Identify Patterns
Look for connections between specific foods and symptom flares 2-6 hours after eating.
Test One Trigger at a Time
Remove one suspected trigger for 2 weeks, then reintroduce it and observe. Share your findings with your doctor.
The most effective tool I've found is a simple food and symptom diary. Here's how to do it:
- Track everything you eat for two to three weeks. Include quantities and timing.
- Rate your symptoms daily on a 1-10 scale. Note specific symptoms (burning, tingling, numbness, pain level).
- Look for patterns. Do symptoms consistently worsen 2-6 hours after certain meals? Do they improve on days when you eat differently?
- Test one category at a time. Remove a suspected trigger for two weeks, then reintroduce it and observe the response.
- Share your diary with your doctor. This data is valuable for both of you when making treatment decisions.
This approach takes patience, but it gives you personalized information that no article can provide. Your triggers may include foods from every category on this list—or only one or two.
Foods That May Actually Help Your Nerves
This article focuses on what to avoid, but it's worth noting that the flip side is equally important. Certain foods actively support nerve health by reducing inflammation, stabilizing blood sugar, and providing essential nutrients for nerve repair.
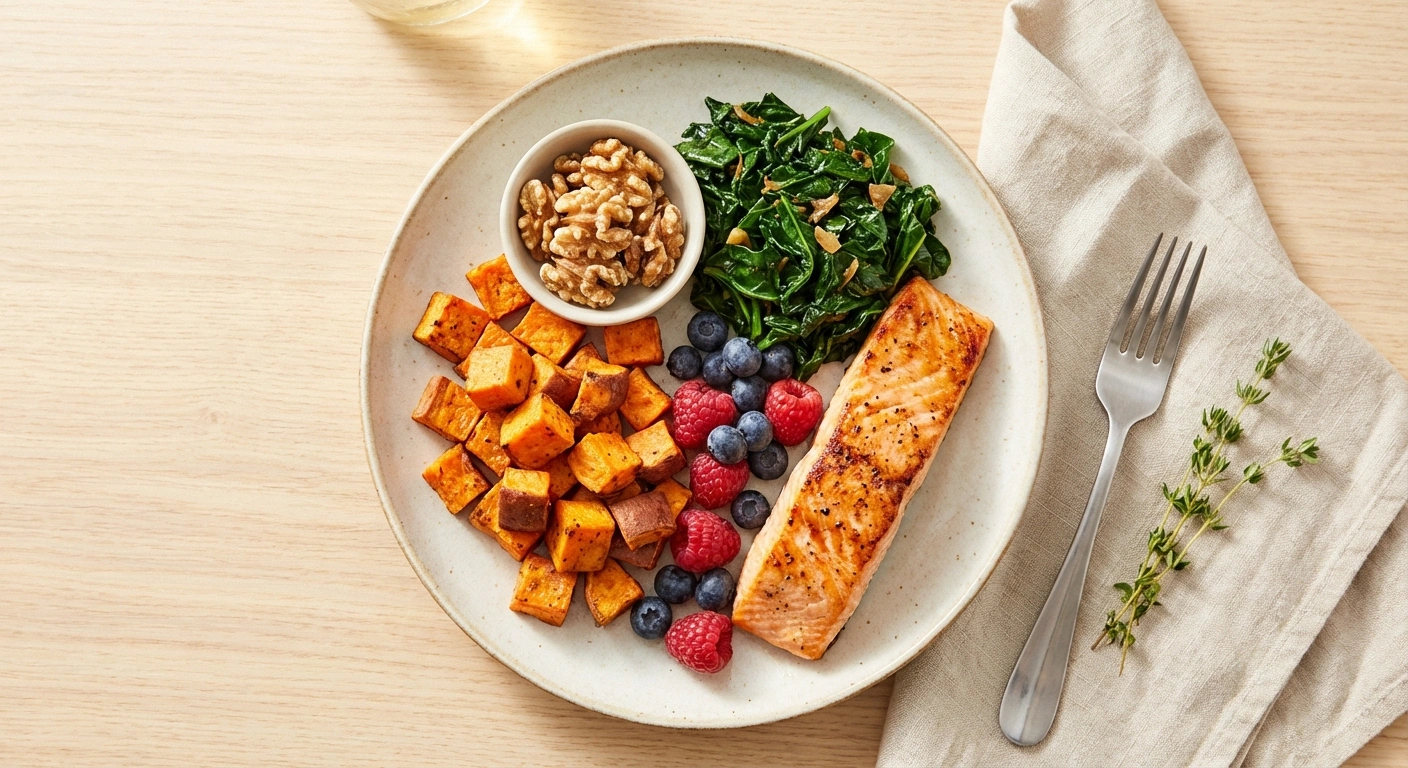
The nerve-friendliest foods include:
- Fatty fish (salmon, sardines, mackerel) — rich in omega-3 fatty acids that reduce inflammation and may support nerve regeneration
- Leafy greens (spinach, kale, collard greens) — packed with magnesium, B vitamins, and vitamin C
- Nuts and seeds (walnuts, almonds, flaxseeds) — provide healthy fats and B vitamins
- Berries (blueberries, strawberries, raspberries) — high in antioxidants that combat oxidative stress
- Lean proteins (chicken, turkey, legumes, tofu) — supply B12 and amino acids for nerve repair
- Whole grains (brown rice, oats, quinoa) — provide steady energy without blood sugar spikes
- Turmeric and ginger — natural anti-inflammatory compounds that may help reduce nerve pain
For a complete guide to building a neuropathy-supportive diet, read our detailed article on the best neuropathy diet.
Making Changes Without Overwhelm
I want to be honest: changing your diet when you're already dealing with chronic pain is hard. The last thing you need is someone telling you to overhaul everything at once. That's not realistic, and it's not necessary.

Key Takeaway
You don't have to overhaul your entire diet overnight. Start with the biggest offender (usually sugar), make one swap per week, and focus on what you're adding — not just what you're removing. Small changes compound over time, and your nerves will notice the difference.
Here's what actually works:
Start with the biggest offender. For most people with neuropathy, that's sugar. Reducing added sugar—even partially—tends to produce the most noticeable improvement in symptoms.
Make one swap per week. Replace white bread with whole grain. Switch from soda to sparkling water. Choose baked over fried. Small changes compound over time.
Don't aim for perfection. A birthday party, a holiday dinner, a stressful day—life happens. One meal doesn't undo weeks of good choices. What matters is the overall pattern.
Focus on what you're adding, not just removing. Instead of mourning the loss of fried food, celebrate discovering that roasted sweet potato fries with olive oil are delicious. Abundance mindset beats deprivation every time.
When to Talk to Your Doctor About Diet and Neuropathy
Dietary changes are a powerful complement to medical treatment, but they don't replace it. You should discuss your diet with your healthcare provider if:
- You have diabetes and are making significant dietary changes (blood sugar medication may need adjusting)
- You suspect you may have celiac disease or gluten sensitivity
- You're considering eliminating entire food groups
- You're experiencing frequent flare-ups despite dietary changes
- You want a referral to a registered dietitian who understands neuropathy
A registered dietitian can create a personalized eating plan that accounts for your specific type of neuropathy, any other health conditions, and your food preferences. If you have diabetes, some insurance plans—including Medicare—cover medical nutrition therapy sessions.
Frequently Asked Questions
Can certain foods actually cause neuropathy, or do they just make it worse?
Most foods don't directly cause neuropathy, but they can worsen it or accelerate its progression. The two exceptions are chronic excessive alcohol consumption, which can cause alcoholic neuropathy on its own, and gluten in people with celiac disease, where the autoimmune response can damage peripheral nerves. For most other foods on this list, the effect is making existing neuropathy symptoms worse through inflammation, blood sugar spikes, or nutrient depletion.
How quickly will I notice a difference after changing my diet?
Most people begin noticing some improvement within two to four weeks of consistent dietary changes, particularly if they significantly reduce sugar and processed food intake. However, nerve healing is slow, and it may take several months to see the full benefit. Blood sugar stabilization produces the fastest noticeable results, while inflammation reduction and nerve repair take longer.
Is coffee bad for neuropathy?
Plain coffee in moderate amounts is generally not considered a neuropathy trigger for most people. However, sweetened coffee drinks with added syrups, whipped cream, and flavored creamers can contain significant amounts of sugar. If you drink coffee, black coffee or coffee with a small amount of unsweetened milk or cream is a better choice. Some people find that caffeine can interfere with sleep, which indirectly worsens neuropathy symptoms.

Should I take supplements if I change my diet?
Diet changes and supplements serve different purposes. A healthy diet provides the foundation, while specific supplements may address targeted deficiencies. B12, alpha-lipoic acid, and magnesium are among the most commonly discussed supplements for neuropathy. However, supplements should complement a good diet, not replace one. Talk to your doctor about testing for specific deficiencies before starting any supplement regimen.
Are organic foods better for neuropathy than conventional foods?
There is no strong evidence that organic foods provide specific benefits for neuropathy beyond those of their conventional counterparts. What matters most for nerve health is the type of food you eat, not whether it carries an organic label. A conventional apple is far better for your nerves than an organic cookie. Focus your budget on the food categories that matter most: fresh produce, lean proteins, whole grains, and healthy fats.
Can a vegetarian or vegan diet help neuropathy?
Plant-based diets can be excellent for neuropathy because they tend to be naturally low in saturated fats and high in anti-inflammatory compounds. The NIH-funded study mentioned earlier found that a low-fat plant-based diet significantly reduced neuropathic pain. However, vegans need to be especially careful about B12 supplementation, since B12 deficiency itself can cause neuropathy. If you follow a plant-based diet, regular B12 monitoring is essential.
Taking Control, One Meal at a Time
Living with neuropathy can feel like so much is out of your control—the nerve damage, the unpredictable symptoms, the limitations on activities you used to enjoy. But what you put on your plate is something you can control, and the evidence suggests it makes a real difference.
You don't need to become a health food purist overnight. Start by identifying the one or two food categories on this list that you consume most often, and make small, sustainable changes. Pay attention to how your body responds. Keep a diary. Share what you learn with your doctor.
Your nerves may have been damaged, but they still respond to how you nourish them. Every meal is a chance to either fan the flames or help cool them down. Choose wisely, be patient with yourself, and know that these changes add up over time.
For more strategies on managing neuropathy through lifestyle changes, explore our guides to managing neuropathy flare-ups, natural remedies for nerve pain, and the best supplements for nerve health.


