Browse all our treatments and therapies guides for more articles like this one.
When most people hear “therapy for neuropathy,” they think of medications, supplements, or maybe physical therapy. But there's another type of therapy that often flies under the radar — and for many people with neuropathy, it turns out to be the one that makes the biggest difference in everyday life. I'm talking about occupational therapy.
Occupational therapy (OT) isn't about finding you a job — despite what the name might suggest. It's about helping you do the things that fill your day: getting dressed, cooking meals, writing a note, opening a jar, driving safely, and dozens of other tasks that neuropathy can quietly steal from you. Where physical therapy focuses on strength, mobility, and exercise, occupational therapy focuses on function — the practical ability to live your life the way you want to.
If neuropathy has been changing how you manage adaptive cooking tools from OT tasks — if you've been dropping things, burning yourself while cooking, struggling with buttons, or avoiding activities you used to enjoy — occupational therapy may be exactly what you didn't know you needed.
What Is Occupational Therapy?
Occupational therapy is a healthcare profession focused on helping people perform meaningful activities — called “occupations” — despite physical, cognitive, or sensory challenges. In the context of neuropathy, an occupational therapist (OT) works with you to:
- Identify which daily tasks have become difficult or unsafe due to numbness, pain, or weakness
- Teach new techniques or workarounds for those tasks
- Recommend and train you on adaptive equipment
- Design exercises to improve hand strength, dexterity, and coordination
- Help you modify your home and work environments for safety
- Address the emotional impact of losing independence
An occupational therapist typically holds a master's or doctoral degree and is licensed to practice in their state. Many OTs who work with neuropathy patients have additional training in hand therapy or neurological rehabilitation.
How Is OT Different From Physical Therapy?
This is one of the most common questions I hear, and it's a good one. Both physical therapy (PT) and occupational therapy (OT) are valuable for people with neuropathy, but they focus on different things:
🏋️ Physical Therapy
Focuses on mobility, balance, lower body strength, gait training, and pain reduction through exercise. Great for walking, fall prevention, and overall fitness.
🤲 Occupational Therapy
Focuses on daily activities: dressing, cooking, writing, gripping objects, home safety. Includes adaptive equipment training, hand therapy, and sensory re-education.
- Physical therapy focuses on mobility, strength, balance, and pain reduction through exercise. A PT might work with you on walking safely, building leg strength, or improving balance to prevent falls.
- Occupational therapy focuses on the activities of daily life. An OT might work with you on buttoning a shirt, holding a pen, gripping a steering wheel, or safely using kitchen tools when your hands are numb.
Many people with neuropathy benefit from both — PT to address the bigger movements and OT to address the finer ones. If your doctor has only referred you to physical therapy, it's worth asking about OT as well, particularly if hand function, dexterity, or daily task performance are among your challenges.
How Neuropathy Affects Daily Activities
To understand why occupational therapy matters, it helps to look at how neuropathy disrupts the small tasks most people take for granted:
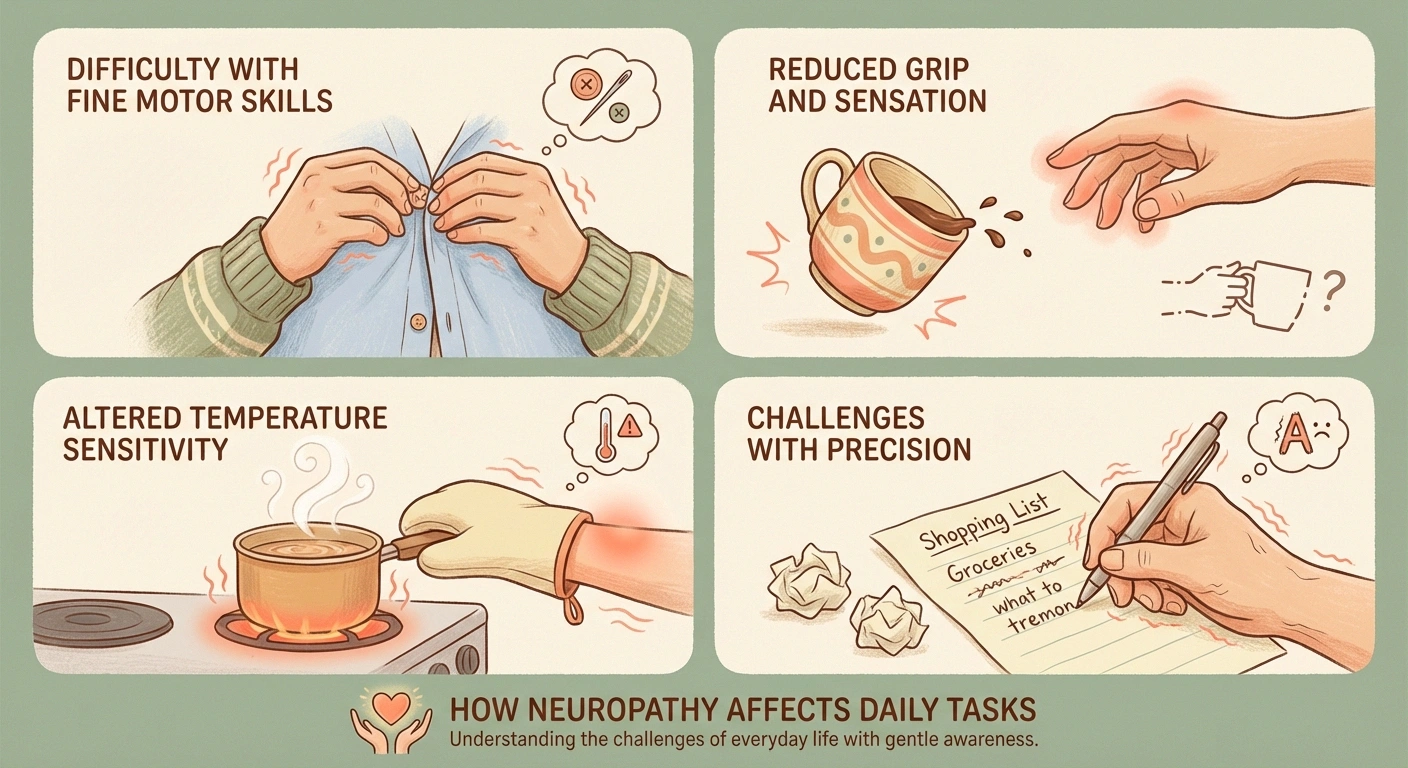
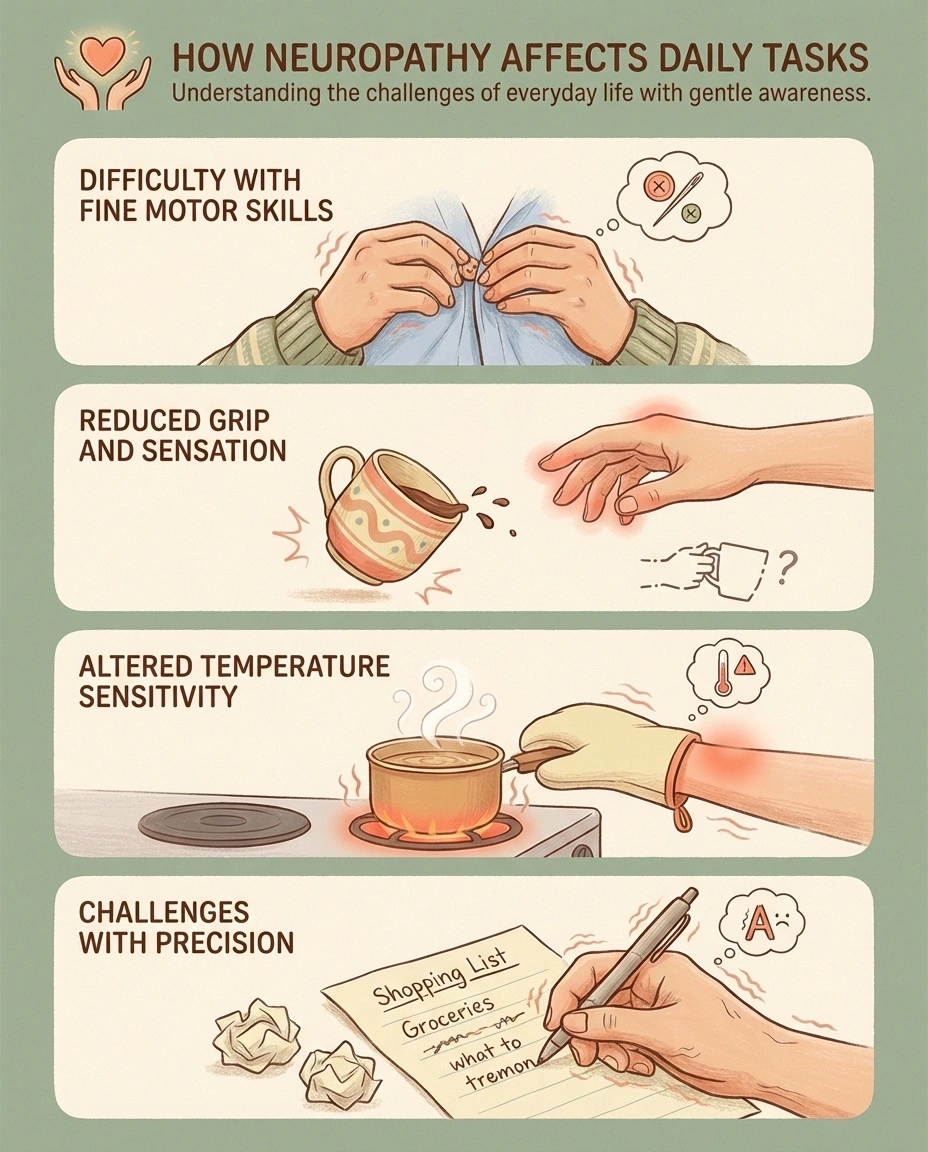
Are These Tasks Getting Harder?
Buttoning shirts, zipping jackets, or fastening clasps
Gripping cups, utensils, or cooking tools securely
Writing legibly or using a keyboard comfortably
Opening jars, bottles, or medication containers
Feeling temperature when cooking or bathing (burn risk)
Feeling completely drained by mid-afternoon despite light activity
If you checked two or more, talk to your doctor about an occupational therapy referral.
Fine Motor Skills
Neuropathy in the hands — whether from diabetes, chemotherapy, or other causes — can make it difficult to perform tasks that require precision. Buttoning a shirt, zipping a jacket, typing on a keyboard, writing a check, threading a needle — these all require a level of finger coordination and sensation that neuropathy directly undermines.
Grip Strength
Many people with neuropathy in their hands notice that they've lost grip strength. They drop cups, struggle to open jars, or find that their handwriting has become shaky and difficult to read. This isn't just frustrating — it can be dangerous when handling hot pans, sharp knives, or medications.
Sensation and Safety
Reduced sensation creates hidden dangers. If you can't feel how hot a pot handle is, you could burn yourself without realizing it until you see the blister. If you can't feel the edge of a knife or the sharpness of a tool, cuts become more likely. People with neuropathy in their feet may not feel injuries from stepping on objects around the house.
Energy and Fatigue
Neuropathy-related fatigue is real and often underestimated. When every task requires extra concentration because your senses aren't reliable, mental and physical fatigue builds up quickly. By mid-afternoon, many people with neuropathy feel completely drained — not because they've been physically active, but because their nervous system has been working overtime to compensate for what it's lost.
What Happens in an Occupational Therapy Session
If you've never been to an OT, here's what you can generally expect:


Initial Evaluation
Your first session will typically be an evaluation where the OT assesses your current abilities and challenges. This usually includes:
- Sensation testing: Using tools like monofilaments, tuning forks, or textured objects to determine which areas of your hands and feet have reduced sensation
- Strength testing: Measuring grip strength and pinch strength using a dynamometer
- Dexterity testing: Tasks like picking up small objects, stacking pegs, or manipulating coins to assess fine motor function
- Activity assessment: Going through your typical daily routine to identify where you're struggling — dressing, cooking, grooming, driving, work tasks
- Home and work environment review: Discussing the layout of your home and any safety concerns
Treatment Plan
Based on the evaluation, your OT will create a personalized treatment plan. This typically includes a combination of therapeutic exercises, adaptive equipment training, and environmental modifications — all tailored to your specific needs and goals.
Key OT Interventions for Neuropathy
Here's where occupational therapy really shines. The interventions are practical, specific, and designed to produce real improvements in daily functioning:

Sensory Re-Education
Sensory re-education is one of the most fascinating aspects of OT for neuropathy. It involves training your brain and nervous system to better interpret the sensation signals you still have. Techniques include:
- Texture discrimination exercises: Touching and identifying different textures (sandpaper, silk, cotton, corduroy) with eyes closed, then open, to retrain sensory pathways
- Vibration therapy: Using vibrating tools to stimulate nerve endings and improve sensory awareness
- Temperature discrimination: Practicing the ability to distinguish warm from cool objects — a critical safety skill for cooking and bathing
- Object identification: Reaching into a bag and identifying objects by touch alone (coins, buttons, keys) to improve tactile processing
Sensory re-education doesn't regenerate damaged nerves, but it may help your brain make better use of the nerve signals that remain — an approach that research from the University of Nebraska Medical Center supports as part of a comprehensive rehabilitation program.
Hand Strengthening and Coordination Exercises
An OT will design exercises specifically to target the muscles and movements you need most. Common exercises include:
- Theraputty exercises: Squeezing, rolling, and pinching therapeutic putty to build grip and pinch strength
- Finger opposition drills: Touching each fingertip to your thumb in sequence to improve coordination
- Peg board activities: Placing and removing small pegs to work on dexterity and precision
- Clothespin exercises: Opening and closing clothespins to strengthen the muscles used for gripping
- Rubber band exercises: Stretching rubber bands around fingers to strengthen hand extensors
These exercises are typically done daily at home between sessions, and progress is tracked over time. Many people notice improvements in hand function within four to six weeks of consistent practice.
Adaptive Equipment and Assistive Devices
Sometimes the smartest solution isn't rebuilding what you've lost — it's finding a better tool for the job. Occupational therapists are experts at matching you with adaptive equipment that can make daily tasks safer and easier:
How It Works
Sensory re-education doesn't regenerate damaged nerves — it trains your brain to make better use of the signals that remain. Through repeated texture, temperature, and touch exercises, your nervous system can learn to “listen harder” to reduced input, improving your functional sensation over time.
- Built-up handle utensils: Forks, knives, and spoons with thick, padded handles that are easier to grip when your fingers are numb or weak
- Button hooks and zipper pulls: Simple tools that let you fasten clothing without needing fine finger dexterity
- Jar openers: Rubber grip pads or electric jar openers that compensate for reduced grip strength
- Ergonomic writing tools: Pens and pencils with wider, cushioned grips
- Rocker knives: Kitchen knives that cut with a rocking motion rather than a pressing motion, reducing the grip strength needed
- Long-handled reachers: Tools that let you grab items from shelves or the floor without bending — useful for both hand and foot neuropathy
- Non-slip mats: Placed under cutting boards, plates, or mixing bowls to keep them stable when your grip isn't reliable
Your OT can also recommend splints or braces for your hands or wrists. For people with ulnar neuropathy, for example, a nighttime splint can prevent the nerve from being compressed while you sleep, reducing morning numbness and tingling.
Home Safety Modifications
An OT can evaluate your home environment and suggest changes that reduce injury risk:
- Kitchen safety: Installing oven mitts that go up the forearm, using a thermometer to test water temperature, replacing glass dishes with unbreakable alternatives
- Bathroom safety: Adding grab bars, shower chairs, non-slip mats, and adjusting water heater temperature to prevent scalding
- Bedroom setup: Placing a nightlight on the path to the bathroom, organizing clothing so it's easy to access, using Velcro closures instead of buttons on pajamas
- General clutter reduction: Clearing pathways to reduce tripping hazards — this works hand-in-hand with fall prevention strategies
Energy Conservation and Pacing
OTs are trained in energy conservation techniques — strategies that help you accomplish more throughout the day without hitting a fatigue wall. These include:
- Task prioritization: Doing your most demanding activities during your best energy hours
- Workstation setup: Sitting instead of standing for tasks that don't require it, keeping frequently used items within easy reach
- Activity simplification: Breaking complex tasks into smaller steps with rest breaks between them
- Batch processing: Grouping similar tasks together to reduce the number of transitions (for example, prepping all meals for the week in one session)
OT for Specific Types of Neuropathy
Occupational therapy can be tailored to address the specific challenges of different neuropathy types:

Diabetic Neuropathy
For people with nerve damage from diabetes, OT often focuses on foot safety (inspecting feet, choosing proper footwear), hand dexterity for blood sugar testing, and kitchen safety for meal preparation. Energy conservation is also critical, since diabetes-related fatigue compounds neuropathy-related fatigue.
Chemotherapy-Induced Neuropathy
CIPN often affects both hands and feet, creating a wide range of functional challenges. OT for CIPN typically includes sensory re-education, fine motor exercises, and adaptive equipment for daily tasks. Because CIPN can improve after chemotherapy ends, the OT approach may include both compensatory strategies (working around the problem) and restorative exercises (rebuilding function as nerves recover).
Ulnar and Other Focal Neuropathies
For ulnar neuropathy and other focal nerve conditions, OT is particularly effective because the problem is localized. Targeted splinting, nerve gliding exercises, and ergonomic workplace modifications can produce significant improvements. An OT with hand therapy certification is especially well-suited for these cases.
How to Get Started With Occupational Therapy
Getting started with OT is usually straightforward:

How to Start Occupational Therapy
Get a Referral
Ask your doctor specifically for occupational therapy — not just physical therapy.
Find the Right OT
Look for one with experience in neurological conditions or hand therapy certification.
Check Insurance
Most plans (including Medicare) cover OT when prescribed. Confirm session limits and copays.
Prepare for Your First Visit
Write down specific tasks that are hardest: “I can't grip the knife” beats “cooking is hard.”
- Get a referral. Most insurance plans require a referral from your primary care doctor or neurologist. Ask specifically for occupational therapy — some doctors automatically default to physical therapy referrals.
- Find the right OT. Look for an occupational therapist who has experience with neurological conditions or hand therapy. You can search through the American Occupational Therapy Association's directory or ask your doctor for recommendations.
- Check your insurance coverage. Most health insurance plans cover OT when prescribed by a doctor. Medicare covers OT as well. Call your insurance to confirm how many sessions are covered per year.
- Prepare for your first visit. Write down the specific tasks that are hardest for you — the more specific, the better. “Cooking is hard” is less helpful than “I can't grip the knife firmly enough to chop vegetables” or “I've burned myself twice this month because I can't feel the pan handle.”
What to Expect: Timeline and Progress
Occupational therapy for neuropathy is typically an ongoing process rather than a quick fix. Here's a general timeline of what many people experience:
- Weeks one through two: Evaluation, baseline testing, and initial exercise introduction. You'll learn your home exercise program.
- Weeks three through six: Adaptive equipment training and early results from strengthening exercises. Many people begin noticing improvements in grip and dexterity.
- Weeks six through twelve: Home modifications are implemented, energy conservation strategies become habitual, and measurable gains in hand function are typical.
- Ongoing: Periodic check-ins to adjust exercises, introduce new adaptive tools as needs change, and address any new challenges.
The most important factor in success is consistency with your home exercise program. The exercises an OT prescribes are most effective when done daily, even when they feel simple or repetitive.
Frequently Asked Questions About Occupational Therapy for Neuropathy
Is occupational therapy covered by insurance?
Most health insurance plans, including Medicare, cover occupational therapy when it is prescribed by a doctor. Coverage varies by plan, so check with your insurer about the number of sessions covered per year, any copays, and whether a referral is required.
How is occupational therapy different from physical therapy for neuropathy?
Physical therapy primarily focuses on mobility, balance, and lower body strength. Occupational therapy focuses on the activities of daily living — particularly fine motor tasks, hand function, home safety, and adaptive strategies. Many people with neuropathy benefit from both types of therapy working together.
Can occupational therapy reverse neuropathy?
Occupational therapy does not reverse nerve damage. However, it can significantly improve your ability to function despite nerve damage by retraining your brain to use remaining sensation more effectively, strengthening weakened muscles, and providing tools and strategies to compensate for what has been lost.
What kind of exercises will an occupational therapist give me?
Common exercises include squeezing therapy putty, finger opposition drills, peg board activities, and texture discrimination exercises. The specific exercises depend on which areas are most affected and which daily tasks you want to improve. Your OT will design a personalized home exercise program.
How often do I need to go to occupational therapy?
Most people start with one to two sessions per week for six to twelve weeks, then transition to less frequent check-ins. The frequency depends on the severity of your symptoms, your goals, and your insurance coverage. Daily home exercises between sessions are essential for making progress.
Will my doctor know to refer me to OT, or do I need to ask?
You may need to ask. Many doctors automatically refer neuropathy patients to physical therapy but don't think to include occupational therapy. If fine motor tasks, hand function, or daily activity performance are challenges for you, specifically ask about an OT referral.
Getting Back to What Matters
Neuropathy takes things from you quietly — first it's the feeling in your fingertips, then it's the confidence to hold a coffee cup, then it's the willingness to cook dinner because you're afraid of burning yourself. It happens so gradually that some people don't realize how much they've lost until someone asks them about it.

Key Takeaway
Occupational therapy doesn't cure neuropathy — but it gives you the tools, techniques, and adaptations to keep doing the things that matter most to you. If daily tasks are getting harder, ask your doctor specifically about an OT referral. Most insurance plans cover it.
Occupational therapy is about reclaiming those pieces of your life, one practical solution at a time. It's a button hook that lets you dress yourself independently. It's a set of exercises that brings enough strength back to your hands to open a jar. It's a home setup that keeps you safe without making you feel like a patient in your own house.
If neuropathy has been quietly shrinking your world, an occupational therapist can help you push those boundaries back out. You don't have to accept “I just can't do that anymore” as the final answer.
Talk to your doctor about a referral to occupational therapy. This article is for informational purposes only and is not a substitute for professional medical advice.