Ozempic and Neuropathy: Can GLP-1 Drugs Cause or Help Nerve Damage?
If you're taking Ozempic, Wegovy, Mounjaro, or another GLP-1 medication and you've started noticing tingling in your feet or new numbness in your hands, you're not imagining it — and you're definitely not alone. The relationship between these wildly popular medications and nerve health is complicated, and the truth is that GLP-1 drugs may both help and harm your nerves depending on the circumstances.
As someone who has spent years helping people navigate neuropathy, I've been watching the research on GLP-1 receptor agonists closely. The science is genuinely exciting — and genuinely concerning — in equal measure. Let me walk you through what we know so far.
What Are GLP-1 Medications and Why Are They Everywhere?
GLP-1 receptor agonists (GLP-1 RAs) are a class of medications originally developed for type 2 diabetes. They mimic a natural hormone called glucagon-like peptide-1, which helps regulate blood sugar by stimulating insulin release, slowing stomach emptying, and reducing appetite. The most well-known names include semaglutide (sold as Ozempic for diabetes and Wegovy for weight loss), tirzepatide (Mounjaro/Zepbound), liraglutide (Victoza/Saxenda), and dulaglutide (Trulicity).
These medications exploded in popularity around 2023 when their dramatic weight-loss effects became widely known. Today, millions of people use them — not just for diabetes, but increasingly for obesity management. And that massive user base is why questions about their effects on nerves are becoming urgent.
The Dual Relationship: GLP-1 Drugs and Your Nerves
Here's what makes this topic so confusing: GLP-1 medications appear to have a genuinely dual relationship with neuropathy. Research suggests they may protect nerves in some situations while potentially contributing to nerve problems in others. Understanding this paradox requires looking at two separate mechanisms.
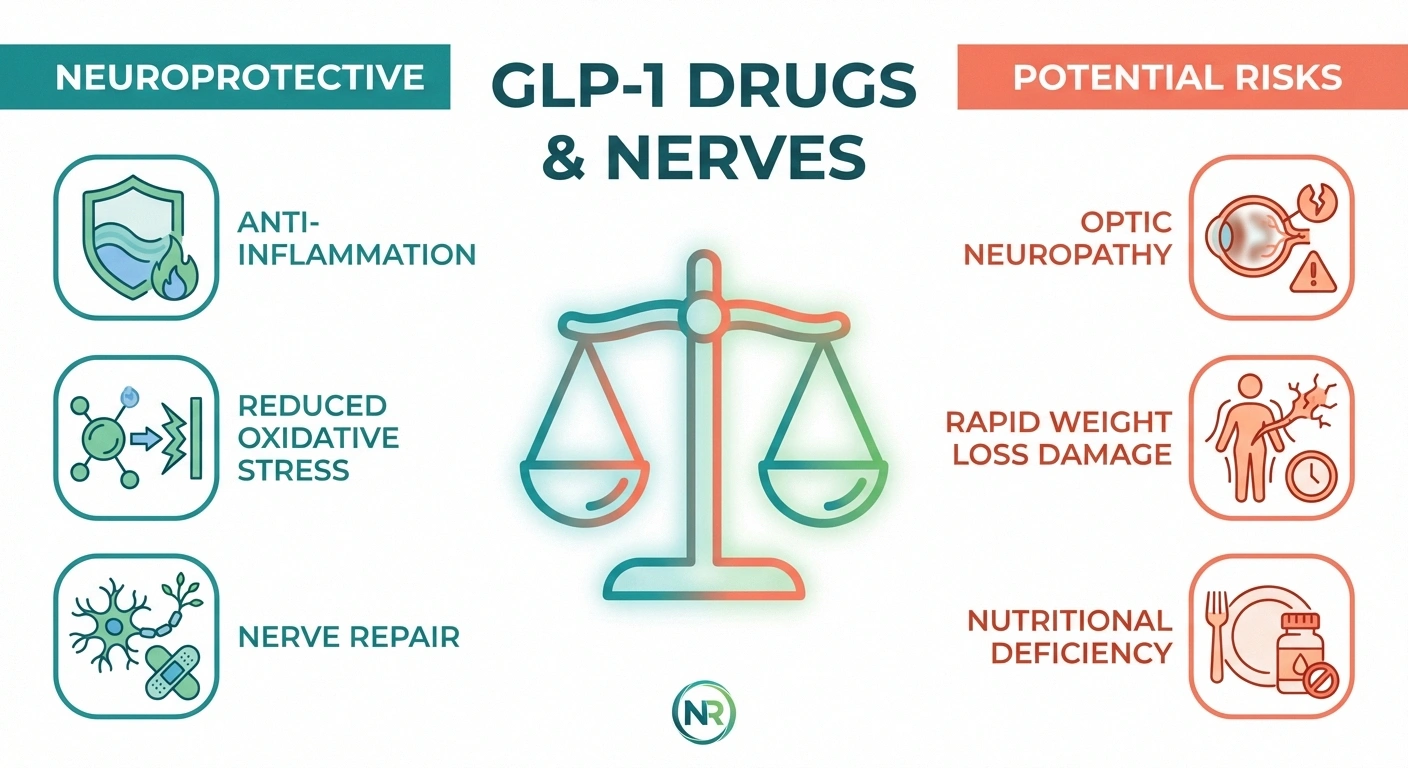
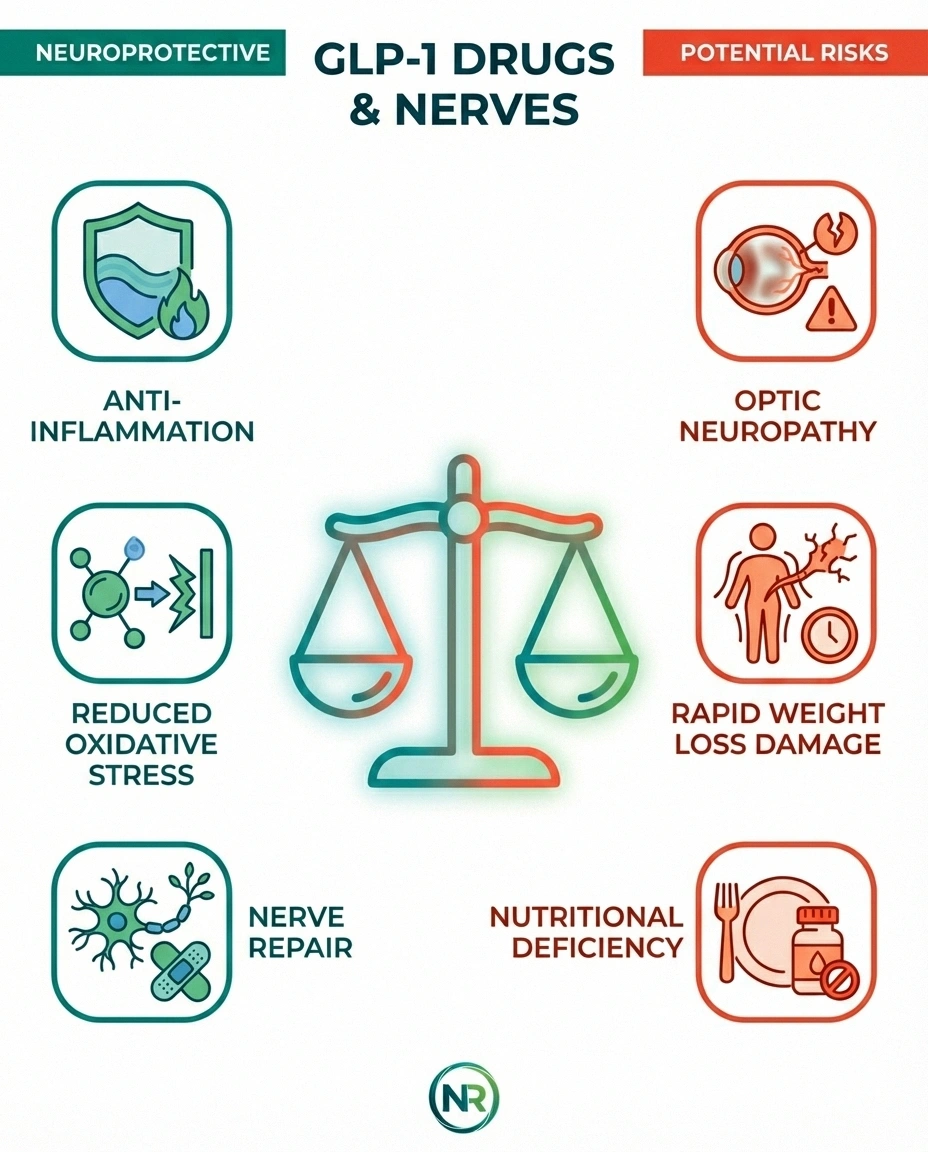
The Neuroprotective Side
A growing body of research suggests GLP-1 receptor agonists may actually help protect and even repair damaged nerves. A 2023 review published in PMC found that GLP-1 RAs demonstrate anti-inflammatory, antioxidative, and neuroprotective properties in preclinical models. These drugs appear to reduce the neuroinflammation and oxidative stress that drive diabetic nerve damage.
Even more compelling: a 2025 study published in the Journal of Neurophysiology found that GLP-1 RA therapy improved both clinical outcomes and nerve function measurements in patients with diabetic peripheral neuropathy. The researchers suggested these drugs may reverse axonal dysfunction by improving sodium-potassium pump function — essentially restoring the basic electrical machinery that damaged nerves need to communicate.
A separate 2024 study in Diabetologia demonstrated that GLP-1 receptor agonists could actually reverse nerve morphological abnormalities in diabetic peripheral neuropathy, meaning the physical structure of damaged nerves showed measurable improvement.
The Concerning Side
On the flip side, there are legitimate concerns. The most notable involves the optic nerve. A study from Massachusetts Eye and Ear (Harvard Medical School) found that people taking semaglutide were approximately twice as likely to develop non-arteritic anterior ischemic optic neuropathy (NAION) — a condition where reduced blood flow damages the optic nerve, potentially causing sudden, permanent vision loss. The optic nerve contains GLP-1 receptors, which may make it vulnerable to unintended effects from these drugs.
There's also the issue of rapid weight loss itself, which we'll discuss in detail below.
“Ozempic Feet”: When Weight Loss Unmasks or Triggers Nerve Symptoms
“Ozempic feet” isn't an official medical term, but it describes a real phenomenon that many patients report. When people lose weight rapidly on GLP-1 medications, several things can happen to their feet and peripheral nerves:

Fat pad loss: Your feet have natural cushioning — fatty pads that protect the bones and nerves. Rapid weight loss can strip away this protective padding, leaving nerves more exposed to pressure and compression. This doesn't mean the drug caused neuropathy — it may have unmasked nerve sensitivity that was always there but was cushioned.
Nutritional deficiencies: GLP-1 medications work partly by reducing appetite and slowing digestion. If you're eating significantly less, you may develop deficiencies in B12, B1 (thiamine), folate, or other nutrients essential for nerve health. Vitamin deficiencies are one of the most common — and most fixable — causes of neuropathy.
Rapid weight loss neuropathy: This is a well-documented condition, separate from any medication effect, where losing weight too quickly can directly damage peripheral nerves. The exact mechanism isn't fully understood, but it's thought to involve sudden metabolic shifts, nutrient depletion, and changes in how the body processes fats that help maintain nerve insulation.
Peroneal nerve compression: Significant weight loss can change your body's pressure points. The peroneal nerve, which wraps around the outside of your knee, is particularly vulnerable. Rapid loss of protective tissue around this area can lead to compression, causing foot drop or numbness along the outer leg and top of the foot.
How GLP-1 Drugs May Protect Against Diabetic Neuropathy
For people with type 2 diabetes — the population these drugs were originally designed for — the neuroprotective potential is particularly significant. Diabetic neuropathy affects up to 50% of people with diabetes, and it's driven by a toxic combination of high blood sugar, inflammation, and oxidative stress.
GLP-1 receptor agonists appear to address multiple pathways simultaneously:
Blood sugar control: By lowering and stabilizing blood glucose, these drugs reduce the primary driver of diabetic nerve damage. Every point of HbA1c reduction matters.
Anti-inflammatory effects: GLP-1 RAs reduce levels of pro-inflammatory cytokines and suppress neuroinflammation. Chronic inflammation is a key mechanism in nerve degeneration, and reducing it may slow or halt progressive damage.
Oxidative stress reduction: These medications appear to enhance antioxidant defense systems in nerve tissue, reducing the oxidative damage that breaks down nerve fibers over time.
Direct neuroprotection: GLP-1 receptors exist on nerve cells themselves. When activated, they may trigger protective signaling pathways that help neurons survive under metabolic stress. This is an area of active research, and clinical trial data from Vertex's CagriSema trial is specifically testing whether GLP-1 combinations can reduce neuropathic pain in diabetic patients.
The Optic Neuropathy Concern: NAION and Semaglutide
The link between semaglutide and non-arteritic anterior ischemic optic neuropathy (NAION) deserves careful attention. NAION occurs when blood flow to the optic nerve is disrupted, causing sudden vision loss — usually in one eye. About 6,000 new cases occur annually in the U.S., making it the most common cause of acute optic neuropathy in people over 50.
The Massachusetts Eye and Ear study, published in 2024, found that semaglutide users had roughly double the risk of NAION compared to non-users. While the absolute risk remains low, this is concerning because:
- NAION can cause permanent, irreversible vision loss
- The optic nerve has GLP-1 receptors, meaning these drugs may directly affect it
- Millions of people now use semaglutide-based medications
- Risk factors for NAION (diabetes, hypertension, sleep apnea) overlap heavily with the population taking GLP-1 drugs
What this means for you: If you're taking a GLP-1 medication and experience any sudden changes in vision — blurriness, loss of vision in one eye, or a shadow or curtain effect — seek immediate medical attention. Report any visual symptoms to your prescribing doctor.
What to Do If You Develop Nerve Symptoms on a GLP-1 Medication
If you're experiencing new tingling, numbness, burning, or pain in your feet, hands, or elsewhere while taking Ozempic or another GLP-1 medication, here's a practical action plan:

1. Don't stop your medication without talking to your doctor. The benefits of blood sugar control for nerve health may outweigh the risks. Stopping abruptly can cause blood sugar spikes that are worse for your nerves than continuing the medication.
2. Get your nutrient levels checked. Ask for a comprehensive panel including B12, folate, B1 (thiamine), B6, vitamin D, and a complete metabolic panel. Nutritional deficiencies from reduced food intake are the most common — and most treatable — cause of new neuropathy symptoms on GLP-1 drugs. Read more about B vitamins and neuropathy.
3. Assess your rate of weight loss. If you're losing more than 2-3 pounds per week consistently, that pace may be contributing to nerve symptoms. Your doctor may adjust your dose or recommend dietary changes to slow the rate of loss while maintaining the metabolic benefits.
4. Request a nerve evaluation. An EMG and nerve conduction study can establish a baseline and determine whether you have measurable nerve damage versus symptoms from fat pad loss or other mechanical changes.
5. Protect your feet. Whether your symptoms are from nerve damage or from lost cushioning, properly fitted shoes with extra cushioning and attention to daily foot care can make a significant difference.
Who Is Most at Risk?
Not everyone on a GLP-1 medication will develop nerve problems. Certain factors increase your risk:


- Pre-existing diabetes: If you already have diabetic neuropathy (even mild), you're starting from a more vulnerable position
- Rapid weight loss: Losing more than 1-2 pounds per week significantly increases the risk of weight-loss-related neuropathy
- Existing nutritional deficiencies: If your B12, thiamine, or other key nutrients are already low, reduced food intake can push you into deficiency territory quickly
- History of bariatric surgery: People who have had gastric bypass or similar procedures already have altered nutrient absorption
- Alcohol use: Even moderate alcohol consumption combined with reduced nutrition amplifies the risk
The Research Pipeline: What's Coming Next
The research into GLP-1 drugs and neuropathy is moving fast. Several developments are worth watching:

Vertex Pharmaceuticals is running a clinical trial with CagriSema — a combination of a GLP-1 agonist and an amylin analogue — specifically to test whether it reduces neuropathic pain in people with diabetic peripheral neuropathy. This is one of the first trials designed specifically to study the nerve-protective potential of GLP-1 drugs.
A 2024 review in Frontiers in Endocrinology concluded that GLP-1 RAs show promise for managing diabetic peripheral neuropathy through their anti-inflammatory and neuroprotective properties, but emphasized that large-scale clinical trials are still needed to confirm these benefits in humans.
Meanwhile, the FDA and European Medicines Agency are both monitoring the NAION signal and may update labeling for semaglutide-based drugs as more data becomes available.
The Bottom Line
GLP-1 medications represent a genuine paradox for neuropathy patients. The research increasingly suggests these drugs have real neuroprotective properties — they may reduce inflammation, protect nerve cells, and even reverse some types of nerve damage in people with diabetes. At the same time, the rapid weight loss they cause can trigger new nerve symptoms, and the emerging optic neuropathy signal demands careful monitoring.
If you're taking a GLP-1 medication, the most important thing you can do is stay informed and proactive. Monitor your symptoms, keep up with regular lab work, maintain adequate nutrition, and communicate openly with your healthcare team about any changes you notice. These drugs are genuinely powerful tools — but like any powerful tool, they require careful, informed use.
If you're living with neuropathy and considering a GLP-1 medication — or if you're already on one and noticing changes — talk to your neurologist or primary care doctor. Understanding your individual risk factors is the first step toward making the best decision for your nerve health.
Frequently Asked Questions
Can Ozempic cause peripheral neuropathy?
Ozempic itself has not been conclusively shown to directly cause peripheral neuropathy. However, the rapid weight loss it produces can lead to nutritional deficiencies, fat pad loss, and nerve compression that may trigger neuropathy symptoms. People with pre-existing diabetes are already at higher risk for neuropathy, which can make it difficult to distinguish medication effects from disease progression. If you develop new tingling, numbness, or pain while on Ozempic, talk to your doctor about testing your nutrient levels and evaluating your nerves.
Can I take a GLP-1 drug if I already have neuropathy?
Which GLP-1 drugs carry the optic neuropathy risk?
Do GLP-1 drugs help or hurt diabetic neuropathy?
The research suggests they may do both, depending on the context. For diabetic neuropathy specifically, emerging evidence shows GLP-1 receptor agonists have neuroprotective properties — they reduce inflammation, lower oxidative stress, and may improve nerve function. However, rapid weight loss and nutritional deficiencies from reduced food intake can worsen nerve symptoms. The net effect likely depends on individual factors like rate of weight loss, nutritional status, and baseline nerve health.
What is “Ozempic feet” and is it dangerous?
Ozempic feet is an informal term describing changes people notice in their feet while taking GLP-1 medications — typically from loss of the natural fat padding, changes in foot shape, and sometimes new pain or numbness. While uncomfortable, it is usually manageable with cushioned footwear and orthotics. However, any new numbness or tingling should be evaluated by a doctor to rule out actual nerve damage rather than just mechanical changes from weight loss.
Should I take supplements while on a GLP-1 medication to protect my nerves?
Getting regular blood work to check your nutrient levels is more important than blindly supplementing. That said, because GLP-1 medications reduce food intake, many doctors recommend a high-quality B-complex vitamin that includes B12, B1, and B6 as a reasonable precaution. Vitamin D and magnesium are also commonly monitored. Always discuss supplements with your prescribing doctor, as some can interact with medications.
Can GLP-1 drugs cause vision problems or optic neuropathy?
A 2024 study from Massachusetts Eye and Ear found that semaglutide users had approximately double the risk of developing NAION, a condition that affects blood flow to the optic nerve and can cause sudden vision loss. While the absolute risk remains low, anyone taking a GLP-1 medication should report sudden vision changes to their doctor immediately. Regular eye exams are also recommended.
How fast is too fast for weight loss when it comes to nerve health?
Losing more than 2-3 pounds per week on a sustained basis increases the risk of weight-loss-associated neuropathy. This risk exists regardless of whether weight loss comes from medication, surgery, or dieting. If you are losing weight rapidly on a GLP-1 medication, talk to your doctor about potentially adjusting the dose to slow the rate of loss while maintaining metabolic benefits.