
The Anti-Inflammatory Diet for Neuropathy: Complete Guide
If I could distill twenty years of reading about neuropathy into one biological truth, it would be this: chronic inflammation is one of the most consistent drivers of nerve damage. Not the acute inflammation that heals a cut or fights an infection — that's your immune system doing its job. I'm talking about the low-grade, persistent inflammation that simmers beneath the surface, damaging tissues slowly over months and years without any obvious symptoms until the damage is done.
The connection between inflammation and peripheral neuropathy is well-established in the research. A 2020 review in Frontiers in Pharmacology documented that neuroinflammation — inflammation specifically affecting nerve tissue — plays a central role in the development and progression of multiple types of neuropathy, including diabetic, chemotherapy-induced, and idiopathic forms. What you eat either fuels this inflammation or helps control it. An anti-inflammatory diet doesn't replace medical treatment, but it addresses one of the root mechanisms that drive nerve damage.
This guide covers the science behind inflammation and nerve damage, the specific dietary pattern that best controls it, practical meal planning, and how to transition without feeling like you're on a restrictive diet. If you haven't already, our general neuropathy diet overview provides additional context, and diet for neuropathy prevention covers prevention-specific strategies.
How Inflammation Damages Your Nerves
Understanding the mechanism helps you see why dietary changes matter. Chronic inflammation damages peripheral nerves through several interconnected pathways:
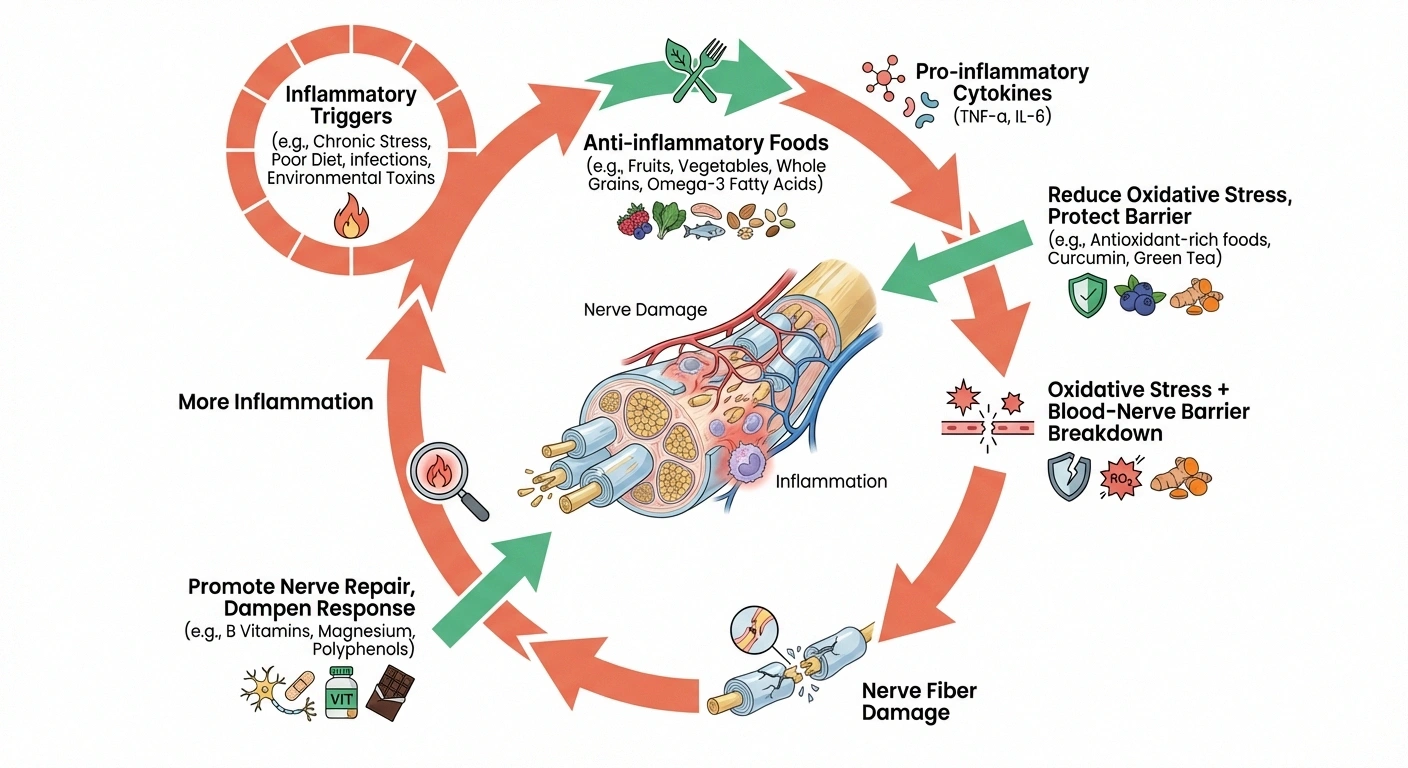
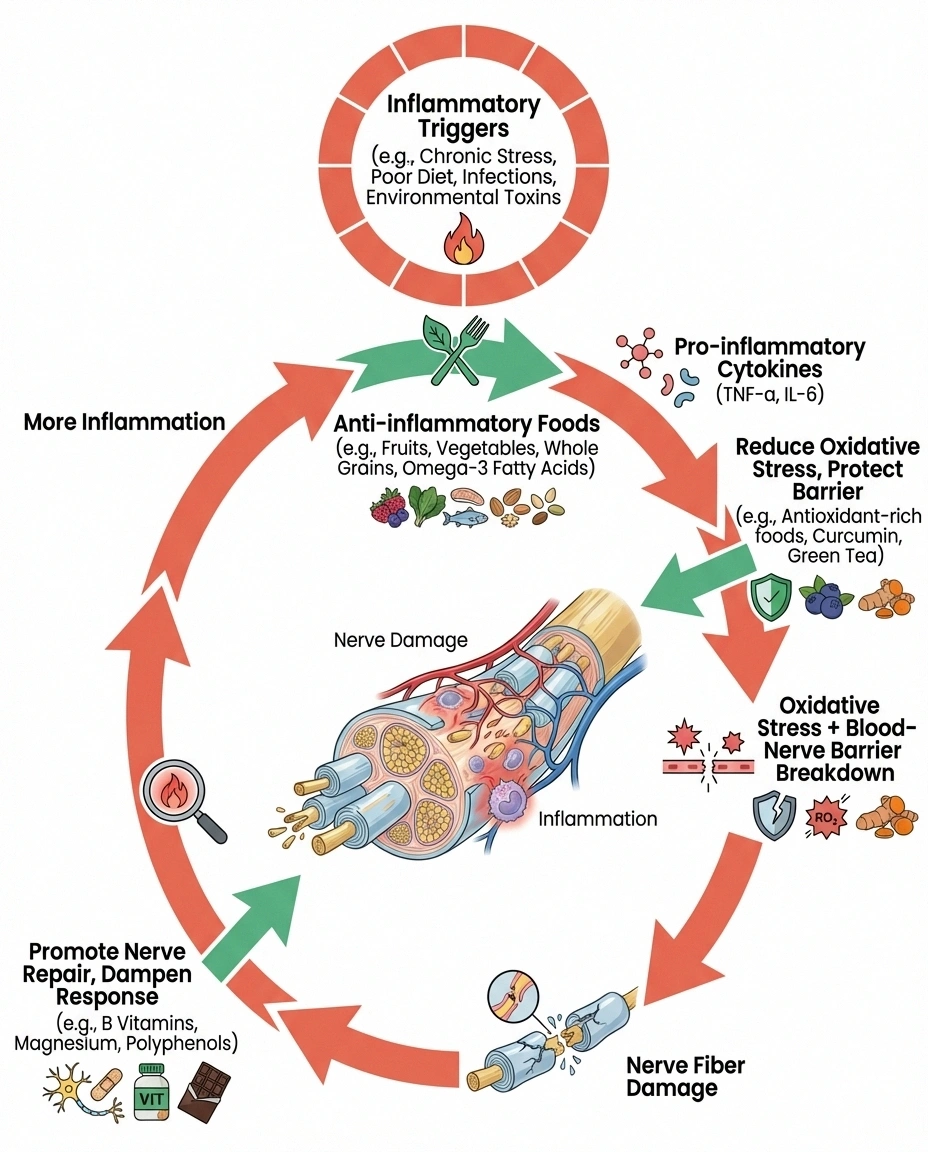
The Inflammation Connection
Chronic inflammation damages nerves through 4 pathways: reactive oxygen species attack nerve membranes, pro-inflammatory cytokines degrade nerve fibers, the blood-nerve barrier breaks down, and Schwann cells can't repair myelin fast enough. An anti-inflammatory diet targets all four.
Reactive oxygen species (ROS). Inflammatory processes generate free radicals that attack nerve cell membranes, mitochondria, and the myelin sheath. Over time, this oxidative damage degrades nerve structure and function. Research shows that people with neuropathy have significantly higher markers of oxidative stress compared to those without nerve damage.
Pro-inflammatory cytokines. Substances like tumor necrosis factor-alpha (TNF-α), interleukin-6 (IL-6), and interleukin-1β directly damage nerve fibers and sensitize pain receptors. Elevated levels of these cytokines have been found in the blood and nerve tissue of people with various types of neuropathy. A review in Frontiers in Cellular Neuroscience confirmed that these inflammatory mediators contribute to both nerve degeneration and neuropathic pain.
Blood-nerve barrier disruption. Like the better-known blood-brain barrier, peripheral nerves have a blood-nerve barrier that protects them from harmful substances in the bloodstream. Chronic inflammation degrades this barrier, allowing inflammatory cells and toxins to infiltrate nerve tissue and cause damage from within.
Impaired nerve repair. Inflammation disrupts the processes that nerve cells use to repair themselves. Schwann cells — the cells responsible for producing and maintaining the myelin sheath — are particularly sensitive to inflammatory signaling. When inflammation is persistent, myelin repair slows down, and nerve signals degrade.
What Is an Anti-Inflammatory Diet?
An anti-inflammatory diet isn't a branded program or a rigid set of rules. It's a dietary pattern built around foods that reduce systemic inflammation while minimizing foods that trigger it. The most studied version is the Mediterranean dietary pattern, which has decades of clinical evidence behind it — including the landmark PREDIMED trial showing a 30% reduction in cardiovascular events.
Not a Fad Diet
An anti-inflammatory diet isn't a branded program. It's the Mediterranean dietary pattern — the most studied eating approach in nutrition science, with decades of clinical evidence including the landmark PREDIMED trial.
The core principles:
- Abundant vegetables and fruits — 7-10 servings daily, emphasizing variety and color (each color represents different anti-inflammatory phytonutrients)
- Healthy fats as primary fat source — extra-virgin olive oil, avocados, nuts, and seeds replace butter, margarine, and processed oils
- Fatty fish 2-3 times per week — the omega-3 EPA and DHA are among the most potent dietary anti-inflammatory compounds available
- Whole grains over refined — oats, quinoa, brown rice, farro, and whole wheat provide fiber and nutrients without the inflammatory spike of refined carbs
- Legumes regularly — beans, lentils, and chickpeas are high in fiber, plant protein, and polyphenols
- Herbs and spices generously — turmeric, ginger, rosemary, garlic, and cinnamon have documented anti-inflammatory properties
- Limited red meat — 1-2 times per week maximum, with lean cuts preferred
- Minimal processed foods, added sugar, and refined flour
The Most Powerful Anti-Inflammatory Foods for Nerve Health
While the overall pattern matters more than any single food, certain foods have particularly strong evidence for reducing inflammation relevant to neuropathy:
The typical Western omega-6 to omega-3 ratio. Optimal for nerve health is 4:1 or lower. The anti-inflammatory diet corrects this imbalance.
Fatty Fish
Salmon, mackerel, sardines, herring, and anchovies are the dietary gold standard for anti-inflammatory eating. Their omega-3 fatty acids (EPA and DHA) reduce production of pro-inflammatory prostaglandins, leukotrienes, and cytokines. A systematic review of omega-3 supplementation found significant reductions in CRP (a key inflammation marker) and improvements in nerve conduction in people with neuropathy. The Foundation for Peripheral Neuropathy recommends at least two 3-4 oz servings of fatty fish per week.

Extra-Virgin Olive Oil
EVOO contains oleocanthal, a compound that functions similarly to ibuprofen in suppressing inflammatory pathways. Research published in Nature found that 50ml of extra-virgin olive oil provides roughly 10% of the anti-inflammatory dose of ibuprofen. Using EVOO as your primary cooking and finishing oil delivers this benefit with every meal. Choose cold-pressed, extra-virgin — refined olive oils lose much of their anti-inflammatory potency.
Turmeric and Ginger
Turmeric's active compound, curcumin, is one of the most studied natural anti-inflammatory agents. It inhibits NF-κB, a key molecule that activates inflammatory genes. Ginger contains gingerols and shogaols, which also suppress inflammatory pathways. For nerve health specifically, animal studies have shown that curcumin may protect Schwann cells and support myelin maintenance. Pair turmeric with black pepper (piperine increases curcumin absorption by up to 2,000%).
Berries
Blueberries, strawberries, raspberries, and blackberries contain anthocyanins — antioxidant compounds that both reduce oxidative stress and suppress inflammatory signaling. The Nurses' Health Study found that women who ate the most blueberries and strawberries had lower inflammatory markers. For neuropathy prevention, berries' combination of anti-inflammatory and antioxidant effects targets two of the primary mechanisms of nerve damage simultaneously.
Leafy Greens
Spinach, kale, Swiss chard, and collard greens are packed with polyphenols, carotenoids, folate, and magnesium — all of which contribute to inflammation control. A study in the Journal of Nutrition found that higher intake of green leafy vegetables was associated with lower CRP and IL-6 levels.
Nuts and Seeds
Walnuts (rich in ALA omega-3s), almonds (rich in vitamin E), and flaxseeds (rich in both ALA and lignans) consistently show anti-inflammatory effects in clinical studies. The PREDIMED trial found that participants who ate 30g of mixed nuts daily had significantly lower inflammatory markers. A daily handful of mixed nuts is one of the simplest anti-inflammatory habits you can build.
Foods That Fuel Inflammation
Eliminating or significantly reducing these foods is as important as adding anti-inflammatory ones:

Hidden Inflammation Sources
A single can of soda contains ~39g of sugar — well above the WHO's 25g daily limit. Processed meats, refined vegetable oils, and fast food are loaded with AGEs, omega-6s, and sodium that fuel the chronic inflammation damaging your nerves.
Refined sugars and high-fructose corn syrup: Sugar triggers the release of inflammatory cytokines and promotes AGE formation. Sodas, candy, pastries, and sweetened cereals are the primary culprits. A single can of soda contains roughly 39 grams of reducing sugar protects nerves — well above the World Health Organization's recommended 25-gram daily limit.
Refined carbohydrates: White bread, white rice, and white pasta behave like sugar in your body — rapid blood sugar spikes followed by inflammatory cascades. Swap for whole-grain versions.
Processed and fried foods: Many processed foods contain inflammatory vegetable oils (soybean, corn, sunflower) high in omega-6 fatty acids. While omega-6s aren't inherently harmful, the modern diet's ratio of omega-6 to omega-3 (typically 15:1 or higher) promotes anti-inflammatory mocktail recipes. A ratio closer to 4:1 or lower supports omega-3 fatty acids reduce inflammation balance.
Processed meats: Hot dogs, bacon, sausage, and deli meats contain advanced glycation end products (AGEs), nitrates, and saturated fat — all of which trigger inflammatory responses. Research consistently links processed meat consumption to higher levels of CRP and inflammatory markers.
Excessive alcohol: Alcohol is both directly neurotoxic and inflammatory. It disrupts gut barrier function, allowing inflammatory bacterial compounds to enter the bloodstream (a process called endotoxemia). Even moderate drinking increases inflammatory markers in some people.
A 7-Day Anti-Inflammatory Meal Plan for Neuropathy
This sample week demonstrates how to apply anti-inflammatory principles practically. Adjust portions based on your caloric needs and any dietary restrictions.

Day 1
Breakfast: Overnight oats with chia seeds, blueberries, walnuts, and a drizzle of honey
Lunch: Salmon salad with mixed greens, avocado, cherry tomatoes, and olive oil dressing
Dinner: Chicken breast with roasted turmeric-seasoned sweet potatoes and steamed broccoli
Day 2
Breakfast: Scrambled eggs with spinach and mushrooms, whole-grain toast
Lunch: Lentil soup with a side of whole-grain bread
Dinner: Baked mackerel with quinoa and roasted Brussels sprouts
Day 3
Breakfast: Greek yogurt with strawberries, ground flaxseed, and a handful of almonds
Lunch: Chickpea and vegetable stir-fry with brown rice
Dinner: Grass-fed beef stew with root vegetables, seasoned with rosemary and thyme
Day 4
Breakfast: Smoothie with spinach, banana, almond butter, and turmeric
Lunch: Sardines on whole-grain crackers with sliced cucumber and mixed greens
Dinner: Turkey meatballs with marinara sauce over zucchini noodles
Day 5
Breakfast: Omelette with bell peppers, onions, and feta cheese
Lunch: Black bean and sweet potato bowl with avocado and salsa
Dinner: Grilled salmon with asparagus and wild rice
Day 6
Breakfast: Whole-grain toast with mashed avocado and poached eggs
Lunch: Mediterranean salad — romaine, olives, cucumber, tomatoes, feta, and olive oil
Dinner: Baked cod with lemon, garlic, and roasted root vegetables
Day 7
Breakfast: Steel-cut oatmeal with walnuts, raspberries, and cinnamon
Lunch: Grilled chicken with tabbouleh (parsley, tomato, bulgur, lemon, olive oil)
Dinner: Shrimp and vegetable curry with coconut milk, served over brown rice
Anti-Inflammatory Spice Guide
Herbs and spices are underused anti-inflammatory tools. Each one below has documented anti-inflammatory properties in research:
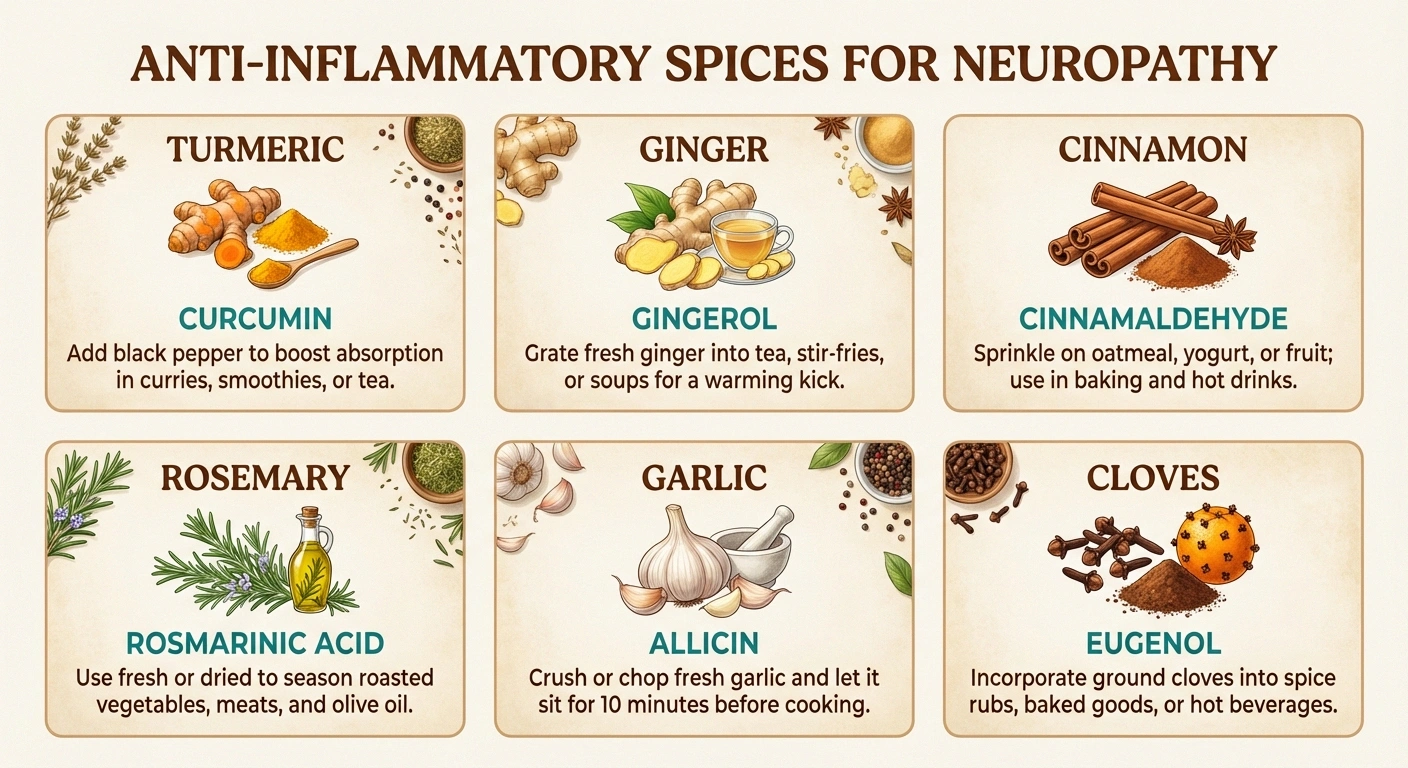


- Turmeric: Inhibits NF-κB and COX-2. Use 1/2 to 1 teaspoon daily in cooking. Always pair with black pepper.
- Ginger: Reduces TNF-α and IL-6. Add fresh ginger to stir-fries, teas, and smoothies.
- Cinnamon: Improves insulin sensitivity and reduces inflammatory markers. Add to oatmeal, coffee, or roasted vegetables.
- Rosemary: Contains carnosic acid, which reduces oxidative stress. Use liberally with roasted meats and vegetables.
- Garlic: Contains allicin, which modulates immune and inflammatory responses. Use fresh garlic daily in cooking.
- Cloves: Among the highest antioxidant content of any spice. Use in small amounts in baking and savory dishes.
Measuring Your Inflammatory Status
If you want objective data on how your diet is affecting inflammation, ask your doctor about these blood tests:
- High-sensitivity C-reactive protein (hs-CRP): The most commonly used marker. Optimal is below 1.0 mg/L. Above 3.0 indicates elevated inflammation.
- Erythrocyte sedimentation rate (ESR): Another general inflammation marker. Elevated values suggest systemic inflammation.
- Omega-3 index: Measures the percentage of omega-3 fats in your red blood cell membranes. Optimal is 8% or above (most Americans are between 4-5%).
- HbA1c: While primarily a blood sugar marker, elevated HbA1c correlates with inflammatory damage to nerves.
Testing before and 3-6 months after dietary changes gives you concrete evidence of the diet's impact. Many people see measurable CRP reduction within 8-12 weeks of consistent anti-inflammatory eating.
How to Transition Without Overwhelm
Overhauling your diet overnight rarely works. Here's a practical 4-week transition plan:
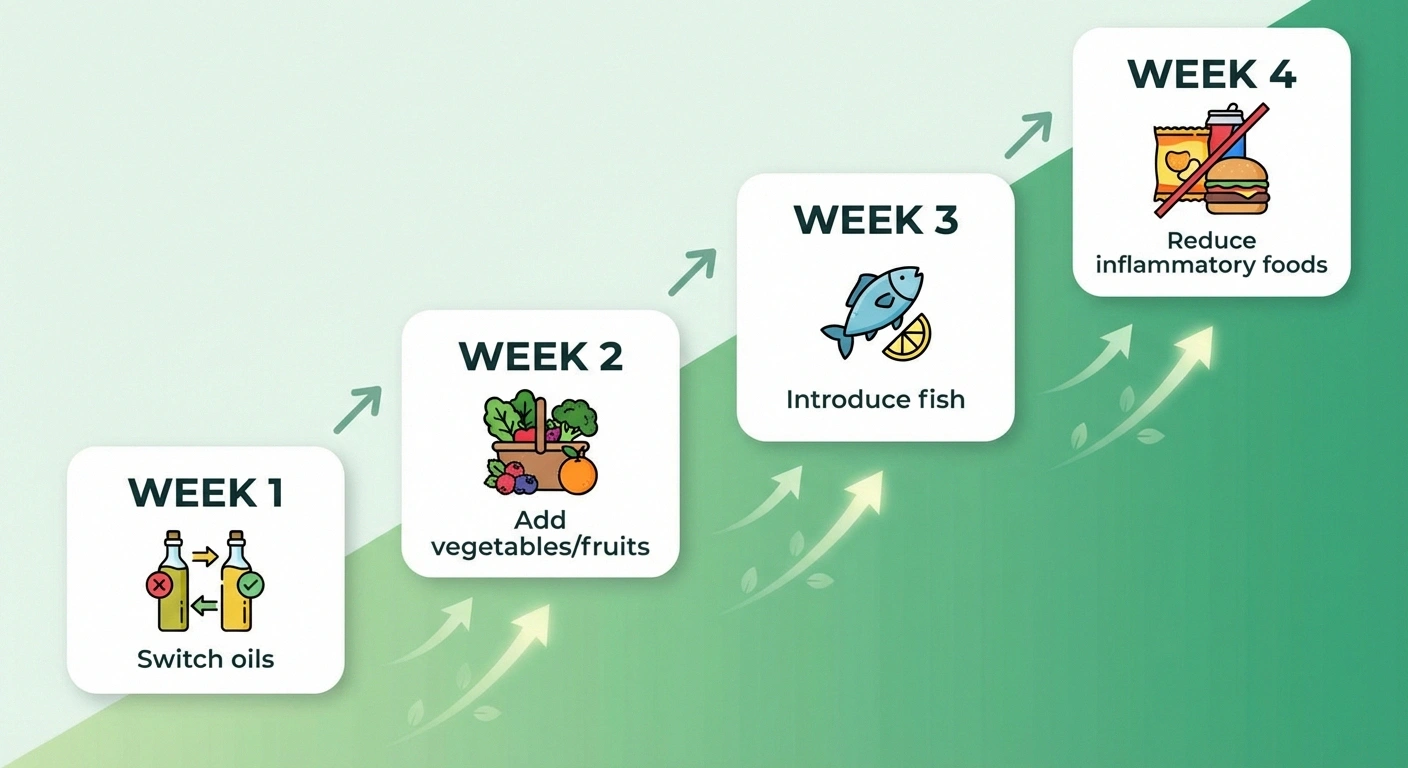
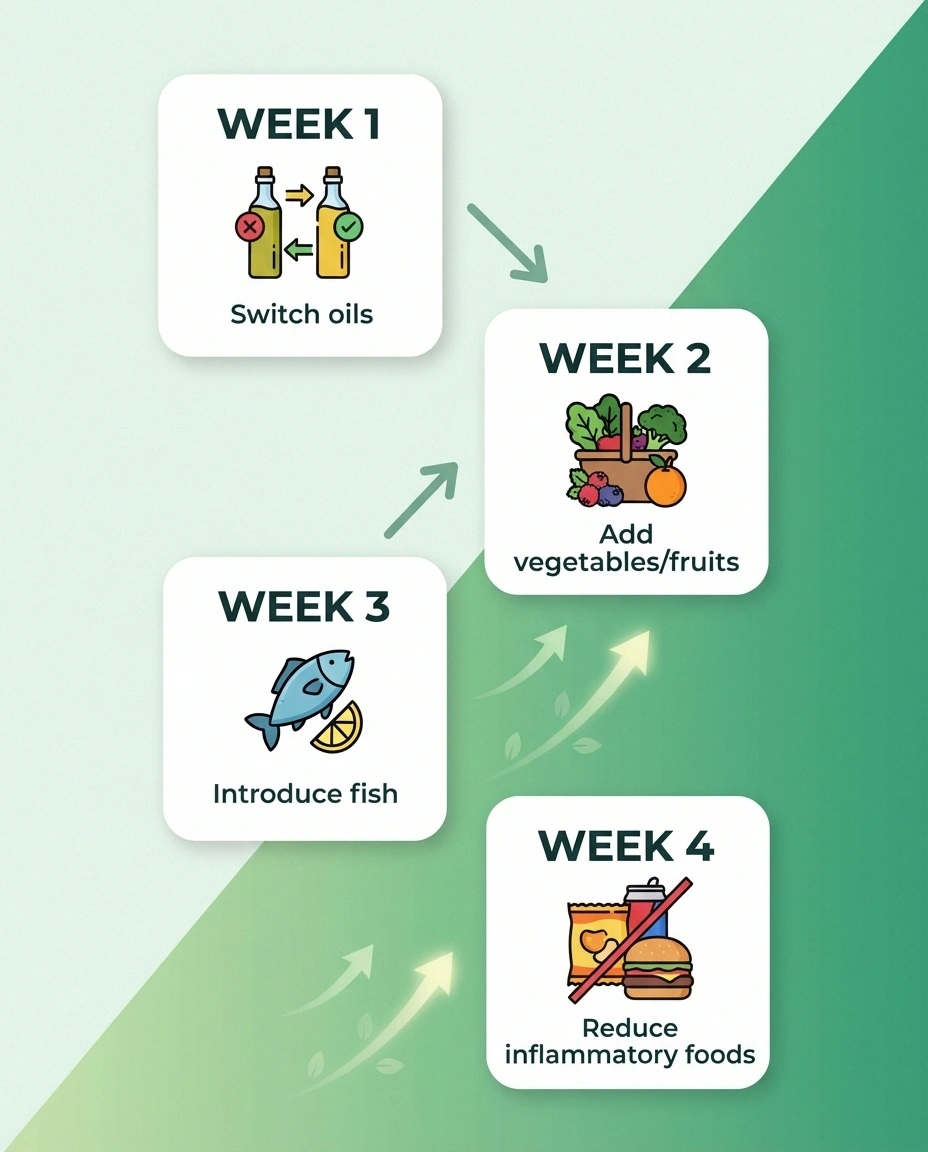
4-Week Transition Plan
Switch Your Oils
Extra-virgin olive oil for cooking/dressing. Daily handful of mixed nuts.
Add Vegetables & Fruits
Extra serving at lunch and dinner. Keep berries for snacking.
Introduce Fatty Fish
Replace 2 meat dinners with salmon, mackerel, or sardines per week.
Reduce Inflammatory Foods
Cut sugary drinks to zero. Swap refined grains for whole grains. Replace processed snacks.
Week 1: Add the oils. Switch to extra-virgin olive oil for cooking and salad dressing. Add a daily handful of mixed nuts (walnuts, almonds, pecans).
Week 2: Increase vegetables and fruits. Add one extra serving of vegetables to lunch and dinner. Keep berries in the fridge for snacking.
Week 3: Introduce fatty fish. Replace two meat-based dinners with salmon, mackerel, or sardines. Experiment with simple preparations (baked salmon with lemon is a gateway recipe).
Week 4: Reduce inflammatory foods. Cut sugary drinks to zero. Swap refined grains for whole grains. Reduce processed snacks and replace with nuts, fruit, or hummus with vegetables.
After these four weeks, you'll have naturally adopted most of the anti-inflammatory pattern without feeling restricted. From there, continue refining: add more legume-based meals, experiment with anti-inflammatory spices, and gradually reduce processed food purchases.
For more on the specific nutrients that support nerve health, visit our supplements guide. For broader prevention strategies beyond diet, see the complete prevention guide.
Frequently Asked Questions
How is an anti-inflammatory diet different from a regular healthy diet?
There is significant overlap. An anti-inflammatory diet is a healthy diet with specific emphasis on maximizing omega-3 fatty acids, antioxidants, and polyphenols while minimizing omega-6 heavy oils, refined sugars, and processed foods. The key differences are the intentional focus on the omega-6 to omega-3 ratio, the generous use of anti-inflammatory spices, and the explicit prioritization of foods with documented effects on inflammatory markers like CRP and IL-6.

Can an anti-inflammatory diet reduce neuropathy pain?
Some people report meaningful pain reduction after adopting an anti-inflammatory diet, typically within 4-12 weeks. The mechanism is plausible: reducing pro-inflammatory cytokines and oxidative stress can decrease nerve sensitization and pain signaling. However, results vary significantly between individuals. Diet is most effective as one component of a comprehensive pain management approach that may include medications, physical therapy, and other treatments.
Do I need to follow this diet perfectly to see benefits?
No. Research on the Mediterranean diet consistently shows benefits at partial adherence levels — meaning you do not need to follow it perfectly. Aiming for 80% compliance while allowing flexibility for social eating, travel, and personal preferences is realistic and effective. The goal is shifting your overall dietary pattern, not achieving rigid perfection at every meal.
Are anti-inflammatory supplements like fish oil as effective as dietary changes?
Supplements can complement dietary changes but generally do not replicate the full benefit of an anti-inflammatory eating pattern. Whole foods contain thousands of compounds that work synergistically — a salmon fillet provides omega-3s, vitamin D, B12, selenium, and astaxanthin together. A fish oil capsule provides only the omega-3s. That said, supplements like fish oil, curcumin, and alpha-lipoic acid have evidence supporting their anti-inflammatory effects and may be valuable additions to an anti-inflammatory diet.
Is the anti-inflammatory diet safe for everyone?
The anti-inflammatory diet is generally safe and appropriate for most adults. However, people on blood-thinning medications should discuss increased omega-3 intake with their doctor, as omega-3s have mild anticoagulant effects. People with fish or shellfish allergies need alternative omega-3 sources. Those with kidney disease may need to limit certain high-potassium foods. Always consult your healthcare provider before making significant dietary changes, especially if you take medications or have chronic health conditions.


