
I still remember the first time I noticed it — lying awake at three in the morning, the burning in my feet impossible to ignore, my mind racing through every worst-case scenario. What if the numbness spreads? What if I can't walk next year? What if this never gets better? The more I worried, the worse the pain seemed to get. And the worse the pain got, the more I worried. It took me years to understand that I wasn't imagining this connection — it's real, it's backed by science, and most importantly, it can be broken.
If you're living with neuropathy and find yourself caught in a similar spiral of pain and biofeedback for neuropathy-related anxiety, you're far from alone. Research suggests that 30 to 60 percent of people with chronic pain develop significant anxiety or depression. That's not a personal failing — it's how the human nervous system responds when it's under constant stress. And understanding this connection is the first step toward feeling better.
The Pain-Anxiety Connection: Why Neuropathy and Worry Feed Each Other
To understand why neuropathy and anxiety become so intertwined, it helps to know a little about how your brain processes pain. The same regions of your brain that handle physical pain — particularly the amygdala and the insula — also process emotions like fear and anxiety. These aren't separate systems running in parallel. They're deeply interconnected, sharing neural pathways and chemical messengers.
of people with chronic pain develop significant anxiety or depression
When you experience chronic nerve pain, these brain areas become hyperactive. They're on high alert all the time, which means emotional signals get amplified right alongside physical ones. A 2024 review in Neuroscience & Biobehavioral Reviews confirmed that anxiety is strongly correlated with pain intensity in neuropathic conditions — the fear of pain itself can trigger stress, irritability, and social withdrawal.
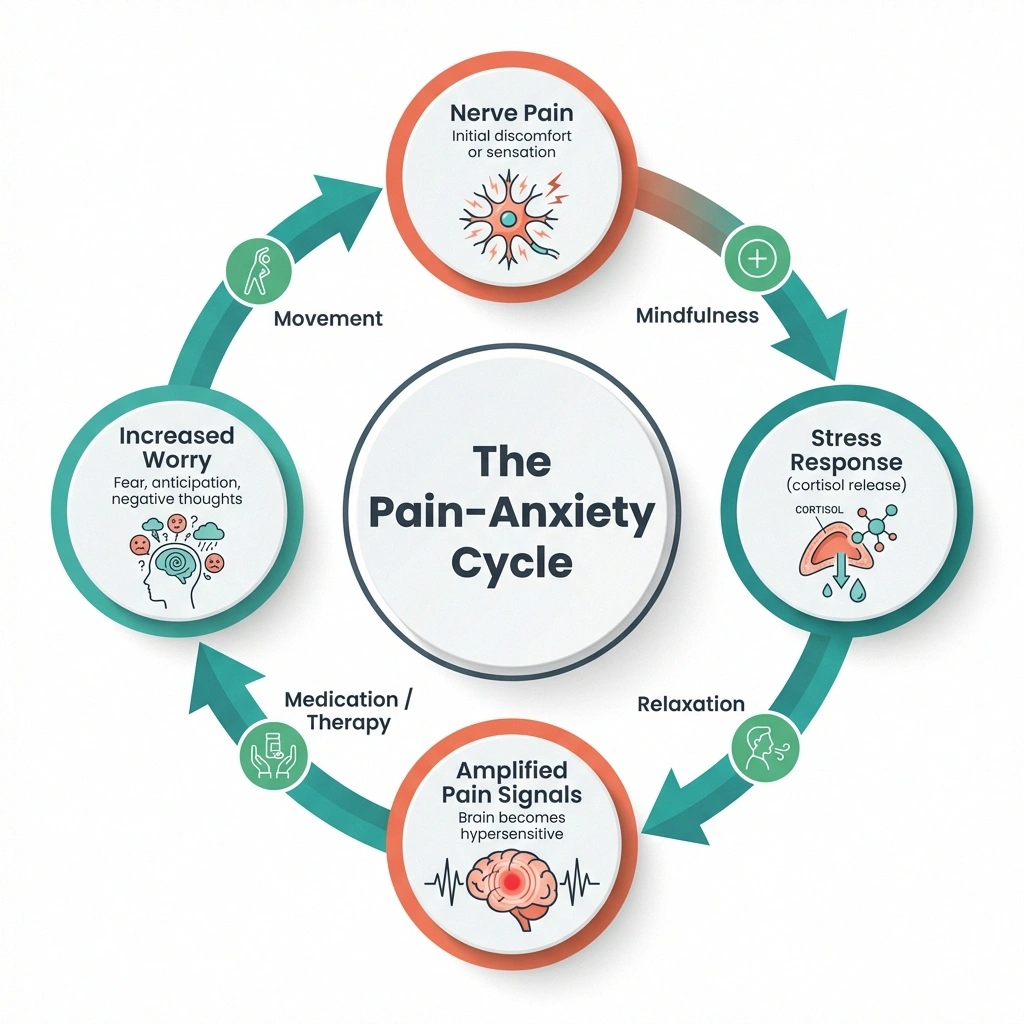
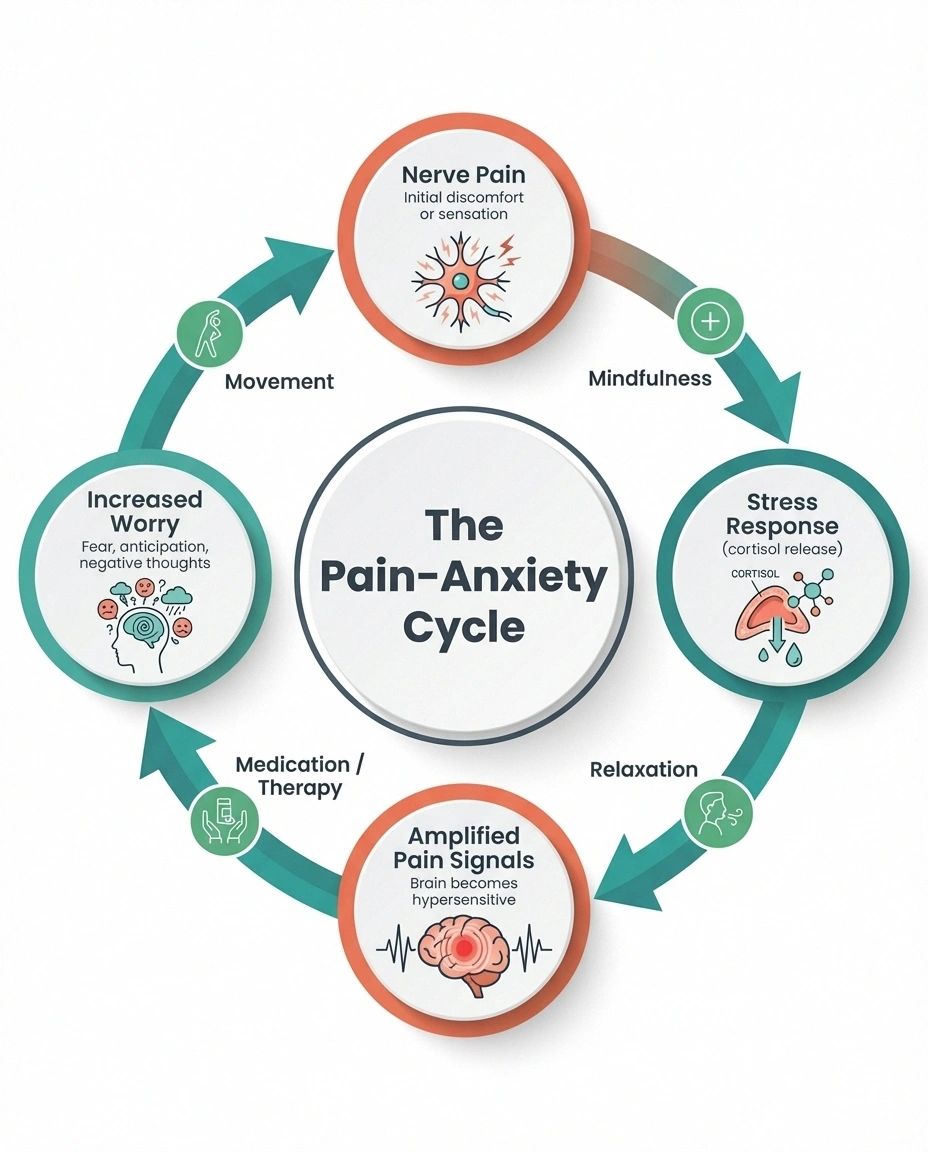
Here's how the cycle typically works:
- Nerve damage creates pain signals — burning, tingling, or shooting sensations that are genuinely difficult to endure
- Your brain interprets these as a threat — triggering the stress response, releasing cortisol and adrenaline
- Stress hormones amplify nerve signaling — making the pain feel more intense than it would otherwise
- Increased pain fuels more worry — about the future, about disability, about whether it will ever improve
- The worry keeps your nervous system on high alert — and the cycle repeats
This isn't something you can just “think your way out of.” It's a physiological feedback loop involving real chemical changes in your brain. But the encouraging news is that because both sides of the loop are biological, interventions that address either side — the pain or the anxiety — can help break the cycle.
Central Sensitization: When Your Nervous System Turns Up the Volume
There's a concept in pain science called central sensitization that helps explain why anxiety makes neuropathy feel so much worse. Normally, your nervous system has a kind of volume control — it can filter out minor sensations so you can focus on what matters. But when you've been in pain for a long time, and especially when anxiety is part of the picture, that volume control can get stuck on high.
Research Says
Central sensitization lowers your pain threshold — meaning sensations that wouldn't normally hurt start to feel painful. Chronic stress and anxiety accelerate this process by keeping cortisol levels elevated, which promotes inflammation and nerve sensitivity.
Central sensitization means your spinal cord and brain start amplifying incoming nerve signals. Sensations that wouldn't normally register as painful — a light touch, the weight of a bedsheet, a change in temperature — suddenly feel uncomfortable or even agonizing. Your nervous system essentially becomes more efficient at producing pain, not less.
Anxiety accelerates this process. When you're stressed, your body produces cortisol — a hormone that, in the short term, helps you respond to danger, but in the long term can inflame nerves and lower your pain threshold. A nervous system that's already dealing with damaged nerves becomes even more reactive. It's like having a smoke detector that not only goes off when there's a fire, but also when someone makes toast.
This is why some people with neuropathy notice their symptoms are dramatically worse during stressful periods — a difficult week at work, a family conflict, financial worries — even though nothing has physically changed with their nerves. The pain increase is real, but it's being driven by central sensitization, not new nerve damage.
What Anxiety Looks Like When You Have Neuropathy
Anxiety in the context of neuropathy doesn't always look like what people picture — it's not always a panic attack or hyperventilating. More often, it's a quiet, constant hum of worry that colors everything. Based on conversations with hundreds of people in my support groups over the years, here are the most common forms it takes:

Do You Recognize These Anxiety Patterns?
Constant worry about whether your neuropathy will get worse
Checking your feet or hands frequently for changes in sensation
Avoiding activities or social events because of pain fears
Dreading bedtime because symptoms get worse at night
Searching symptoms online late at night and feeling worse afterward
Withdrawing from friends and family because you feel like a burden
If you checked 3 or more, the pain-anxiety cycle may be significantly affecting your quality of life. Consider discussing these patterns with your doctor.
Fear of progression. This is probably the single biggest anxiety trigger I hear about. “Will this get worse? Will I end up in a wheelchair? Am I going to lose the feeling in my hands too?” These are natural questions, but when they loop in your mind constantly, they become their own source of suffering.
Hypervigilance about symptoms. Checking your feet constantly. Analyzing every new tingle. Catastrophizing any change as a sign that things are deteriorating. This hyperawareness actually amplifies pain perception — the more attention you direct at a painful area, the louder those signals become in your brain.
Anticipatory anxiety. Dreading activities because of how they might affect your pain. Turning down social invitations because you're worried about triggering a flare-up. Avoiding exercise because you're afraid it will make things worse (even though gentle movement may actually help).
Sleep anxiety. Many people with neuropathy find their symptoms are worst at night, which can create a specific dread around bedtime. You lie down knowing the pain is coming, and the stress-related scalp tingling about not sleeping makes it even harder to drift off — a vicious mini-cycle within the larger one.
Social withdrawal. Pulling away from friends and family because you feel like a burden, because you can't keep up, or because you're tired of explaining a condition that nobody can see. Isolation then feeds depression and more pets reduce neuropathy-related anxiety. If this resonates, know that connecting with others who understand can make an enormous difference.
Medical anxiety. Fear about doctor appointments, test results, or the possibility that your doctor won't take your pain seriously. Some people avoid medical care altogether because the anxiety of going is worse than the anxiety of not knowing. If this describes you, our guide on how to talk to your doctor about neuropathy pain may help you feel more prepared.
The Science Behind the Cycle: What Happens in Your Brain
For those who find it helpful to understand the mechanisms at work, here's a closer look at what's happening neurologically when pain and anxiety reinforce each other.
The amygdala — your brain's threat detection center — becomes overactive in people with chronic pain. It processes incoming nerve signals and tags them with emotional significance. When the amygdala is running hot, neutral signals can get tagged as threatening, making you more reactive to sensations that wouldn't have bothered you before.
The prefrontal cortex — the part of your brain responsible for rational thinking and emotional regulation — can become less effective under chronic stress. This means your ability to talk yourself down from anxiety, to evaluate a situation calmly, is literally diminished. It's not a character flaw — it's a brain that's been worn down by constant pain signaling.
Neurotransmitter changes also play a role. Chronic pain can deplete serotonin and norepinephrine — chemicals that your brain needs for mood regulation and pain modulation. Lower levels of these neurotransmitters mean more pain and more anxiety simultaneously. This is why medications like duloxetine and pregabalin, which affect these chemical systems, can help both conditions at once.
The hypothalamic-pituitary-adrenal (HPA) axis — your body's stress response system — can become dysregulated. In a healthy system, cortisol spikes briefly during stress and then returns to baseline. In people with chronic pain and anxiety, the system may stay activated, flooding the body with cortisol that promotes inflammation and nerve sensitivity.
Breaking the Cycle: Strategies That Actually Help
The most effective approach treats both the pain and the anxiety — not as separate problems, but as interconnected parts of the same challenge. Here are strategies that research and real-world experience support.
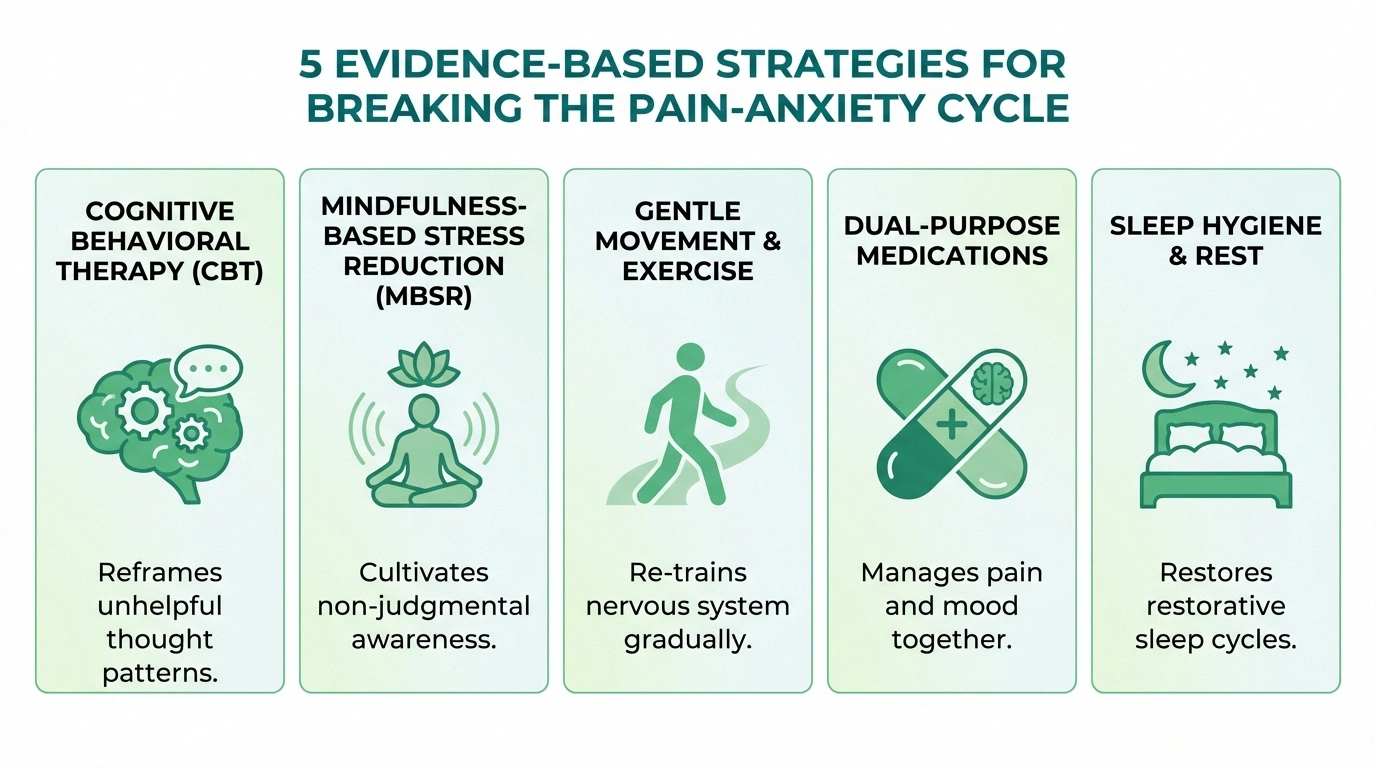
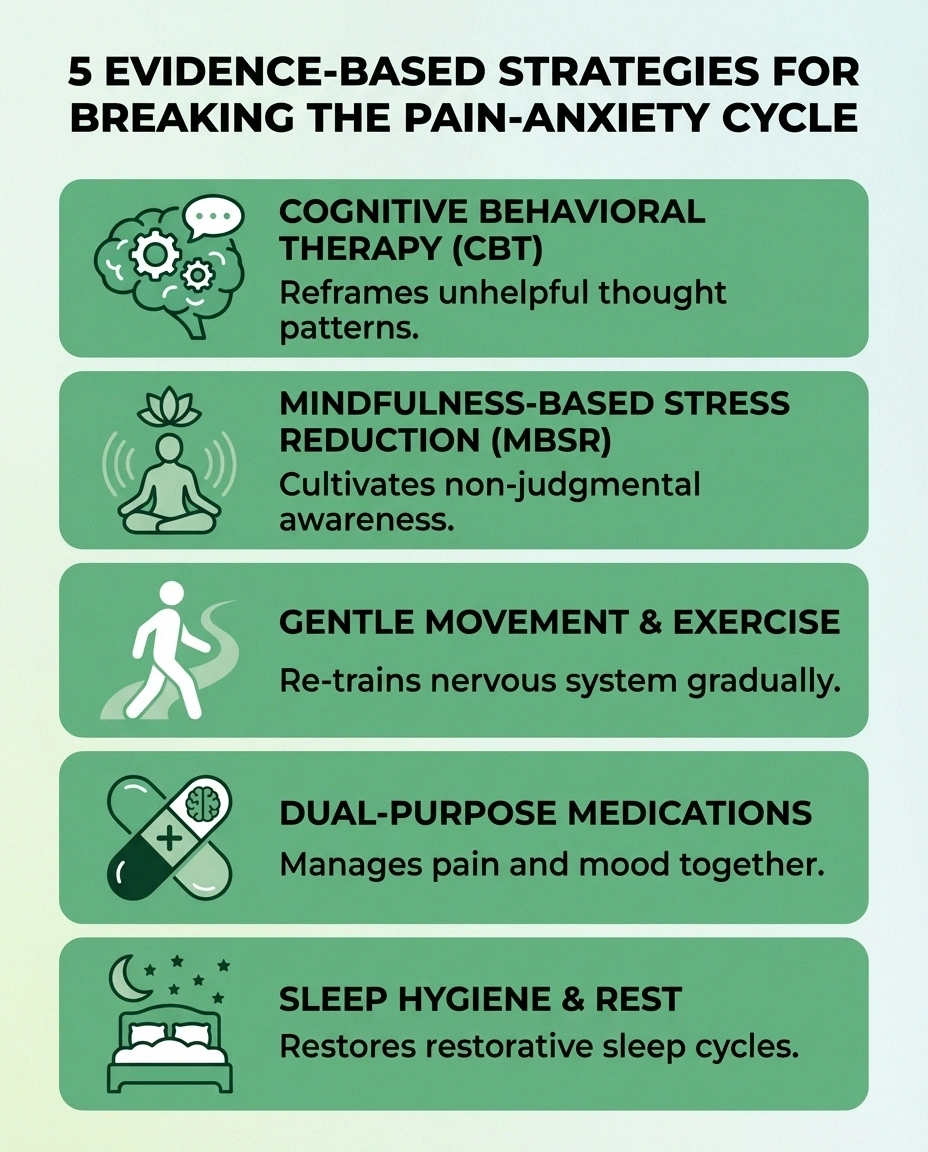
Key Takeaway
The most effective approach treats both the pain and the anxiety together. Medications like duloxetine and pregabalin can address both simultaneously, while CBT and mindfulness work on the psychological side of the cycle.
Cognitive Behavioral Therapy (CBT)
CBT is the most well-studied psychological intervention for chronic pain, and there's strong evidence it helps with the anxiety component too. It works by helping you identify thought patterns that amplify your suffering — catastrophizing, all-or-nothing thinking, fortune-telling about your prognosis — and replace them with more balanced perspectives.
This isn't about pretending the pain isn't there or “thinking positive.” It's about learning to respond to pain without the layer of panic that makes it so much worse. For example, replacing “This burning means my nerves are dying and I'll be disabled” with “This is nerve pain. It's uncomfortable, but my doctor says my condition is stable” doesn't eliminate the sensation — but it can significantly reduce how much you suffer.
Many people with neuropathy find that even 8 to 12 sessions of CBT make a meaningful difference in their daily quality of life. Ask your doctor about pain-focused CBT programs, or look for psychologists who specialize in chronic pain management.
Mindfulness-Based Stress Reduction (MBSR)
Mindfulness meditation has moved from alternative therapy to mainstream medicine over the past decade, and with good reason. MBSR programs, typically structured as eight-week courses, teach you to observe pain and anxiety without reacting to them — to notice sensations without the automatic spiral of fear.
This might sound vague, but the science is concrete. Mindfulness practice has been shown to reduce activity in the amygdala and strengthen the prefrontal cortex — literally reversing some of the brain changes caused by chronic pain. Regular practitioners report lower pain intensity, less anxiety, and improved sleep quality.
You don't need to become a meditation guru. Even ten minutes a day of guided mindfulness practice can begin to shift the pain-anxiety dynamic. Apps and online programs make this accessible even if you can't attend an in-person course.
Gentle Physical Movement
Exercise is one of the most powerful anxiety reducers available — and it also has direct benefits for neuropathy symptoms. Physical activity releases endorphins, your body's natural painkillers, and helps regulate the stress response system that drives the pain-anxiety cycle.
The key is finding forms of movement that work with your body, not against it. Gentle yoga combines movement with breath awareness and can be particularly effective for both anxiety and nerve pain. Swimming and water therapy provide exercise without the impact that may aggravate sensitive feet. Even regular walking, if you can tolerate it, has documented benefits for both conditions.
The goal isn't to push through pain — it's to move consistently at a level your body can handle. Start small and build gradually. Many people find that the anxiety about exercise is worse than the exercise itself.
Medications That Address Both
Several medications used for neuropathic pain also have anti-anxiety properties, which makes them particularly valuable for people caught in the pain-worry cycle:
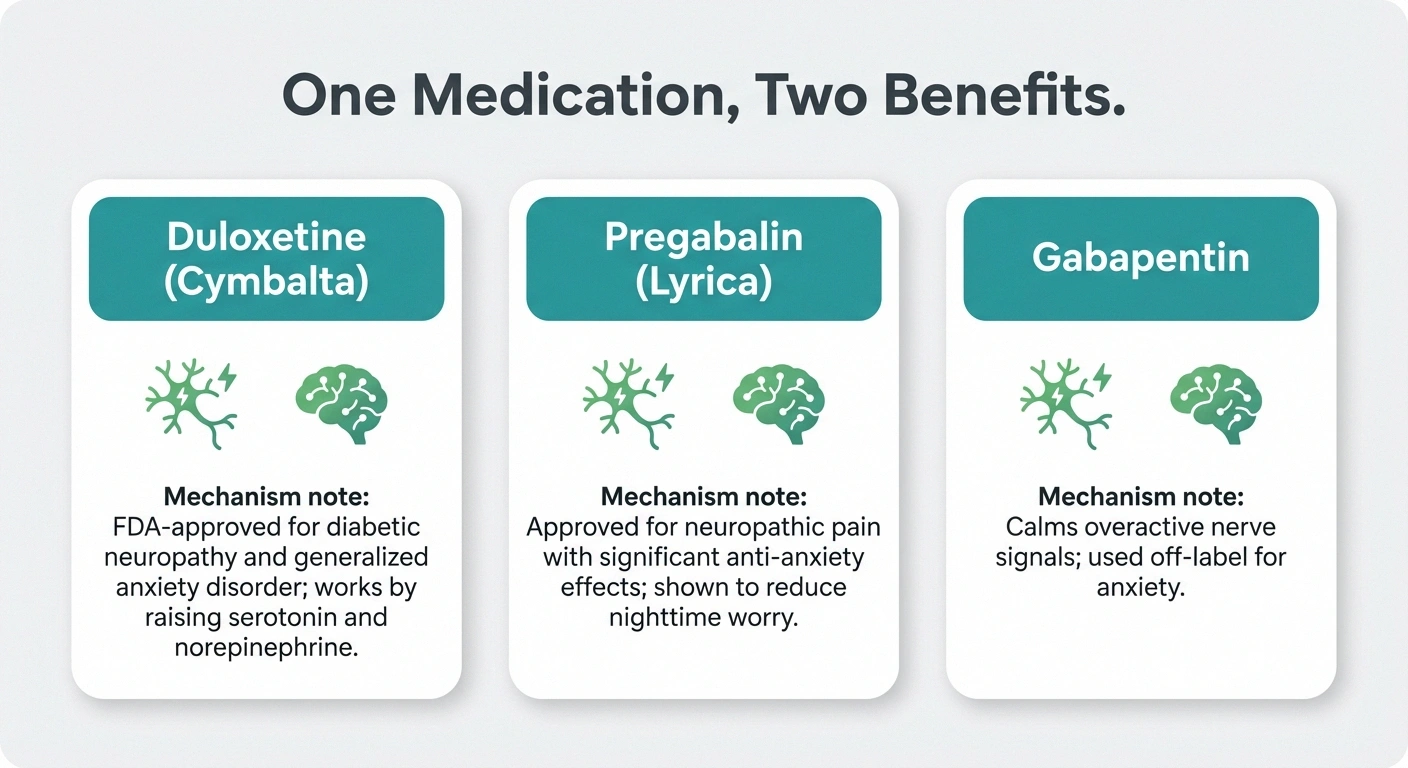
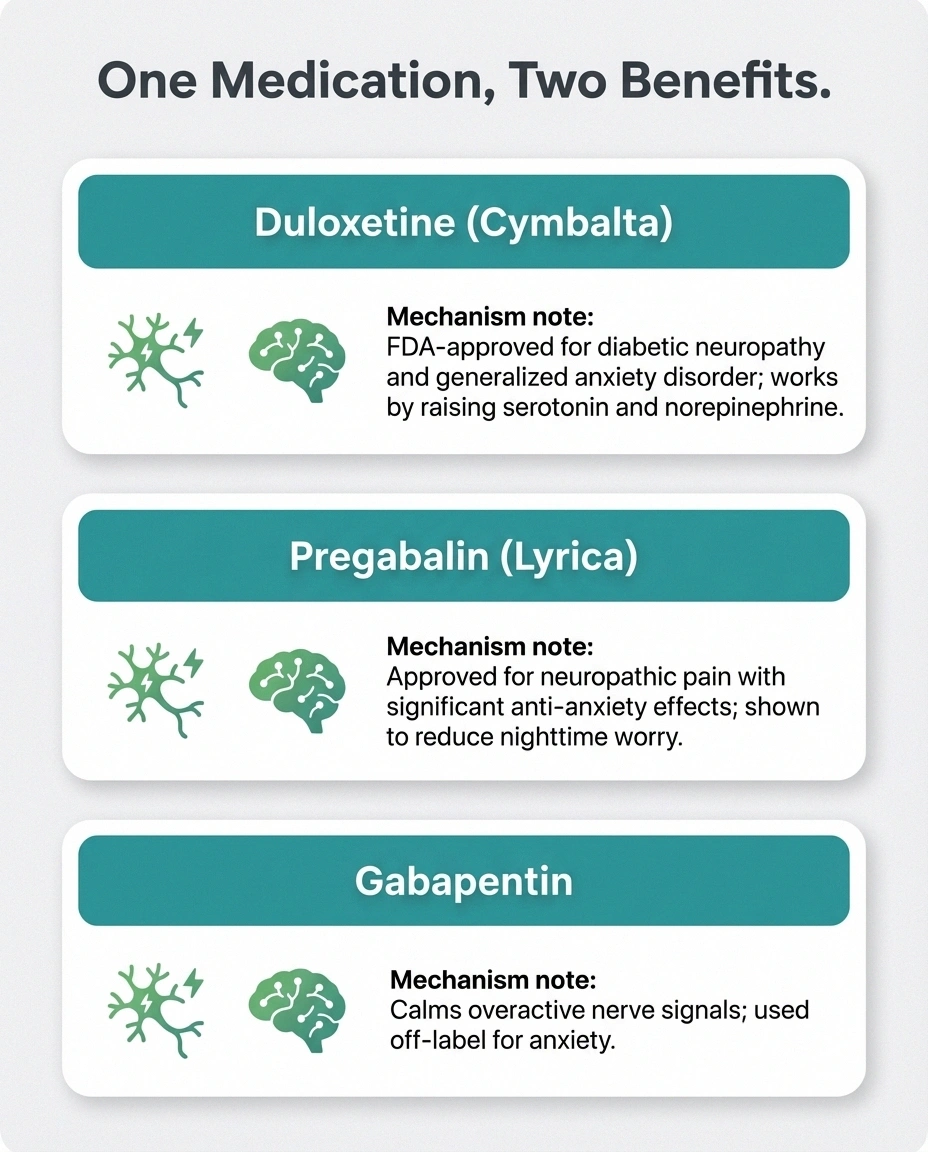
- Duloxetine (Cymbalta) — An SNRI antidepressant that is FDA-approved for both neuropathic pain and generalized anxiety disorder. It works by increasing serotonin and norepinephrine levels in the brain.
- Pregabalin (Lyrica) — Originally developed for seizures, pregabalin is approved for neuropathic pain and also has significant anti-anxiety effects. Many people find it helps with both their pain and their nighttime how catastrophizing feeds neuropathy anxiety.
- Neurontin (gabapentin) — Similar to pregabalin, gabapentin may help calm overactive nerve signals and has been used off-label for anxiety.
Talk to your doctor about whether a dual-purpose medication might be appropriate for your situation. Sometimes addressing both conditions with one medication is more effective than treating each separately.
Sleep Hygiene
Poor sleep is both a symptom of the pain-anxiety cycle and a fuel source for it. When you don't sleep well, your pain threshold drops, your emotional resilience weakens, and your anxiety increases — which then makes it even harder to sleep the next night.
Prioritizing sleep isn't a luxury — it's a core strategy for managing both neuropathy and anxiety. Key approaches include keeping a consistent sleep schedule, making your bedroom cool and dark, avoiding screens before bed, and addressing nighttime pain proactively (for example, with cooling foot soaks or positioning aids before the pain escalates). If melatonin interests you, it may help with both sleep onset and has some preliminary evidence for nerve pain relief.
Building a Support Network
Isolation is one of the most reliable accelerators of both anxiety and pain perception. Humans are social creatures, and when we withdraw — whether because of embarrassment, fatigue, or fear of being a burden — we lose a critical buffer against suffering.
Neuropathy support groups, whether in-person or online, provide something that friends and family often can't: genuine understanding from people who know exactly what you're going through. The simple act of hearing someone say “I have that too” can reduce anxiety more than you might expect.
When Anxiety Might Be Something More
It's important to recognize the difference between situational anxiety — the natural worry that comes with having a chronic condition — and a clinical anxiety disorder that may need professional treatment. Consider talking to your doctor or a mental health professional if:

Seek Help Now
If you're having thoughts of self-harm or feeling that life isn't worth living, please reach out immediately. 988 Suicide & Crisis Lifeline: call or text 988. Crisis Text Line: text HOME to 741741. You are not alone, and help is available right now.
- Your worry feels out of proportion to your actual medical situation
- Anxiety is preventing you from activities you could physically manage
- You're experiencing panic attacks — sudden intense fear with physical symptoms like racing heart, shortness of breath, or chest tightness
- You've been avoiding medical appointments because of anxiety
- Anxiety is significantly disrupting your sleep most nights
- You're using alcohol or other substances to manage your worry
- You have thoughts of self-harm or feel that life isn't worth living
There is absolutely no shame in seeking help. Just as you would see a specialist for your neuropathy, seeing a mental health professional for anxiety is simply getting the right expert for the problem. Many primary care doctors can also screen for and treat anxiety disorders. The connection between neuropathy and mental health is well-established — your doctor won't be surprised by the conversation.
What Not to Do: Traps That Make the Cycle Worse
While we're talking about what helps, it's equally important to recognize patterns that feel like they're helping but actually deepen the pain-anxiety cycle:
❌ Traps That Worsen the Cycle
- Constant symptom monitoring
- Late-night symptom searching
- Avoiding all activity
- Self-medicating with alcohol
- Hiding anxiety from your doctor
✓ Habits That Break the Cycle
- Scheduled “worry windows”
- Daily mindfulness practice
- Gradual, gentle movement
- Open conversations with your doctor
- Connecting with support groups
Constant symptom monitoring. Checking your feet every hour, running your hands over your legs to test sensation, obsessively cataloguing every tingle. This keeps your brain's attention locked onto pain signals, amplifying them. It's hard to stop, but learning to redirect your attention — even briefly — starves the cycle of fuel.
Dr. Google spirals. Searching symptoms at 2 AM almost never makes anxiety better. The internet is full of worst-case scenarios, and your anxious brain will selectively absorb the most frightening information while dismissing anything reassuring. If you need medical information, get it from your doctor or from trusted health resources during daylight hours.
Avoidance of everything. Staying home, dropping hobbies, canceling plans. While pacing yourself is wise, complete avoidance tells your brain that the world is dangerous, reinforcing anxiety. The goal is gradual engagement — doing what you can, not what you can't.
Self-medicating with alcohol. Alcohol might numb anxiety temporarily, but it is directly toxic to nerves and can worsen neuropathy. If you find yourself relying on alcohol to manage worry, that's an important signal to discuss with your doctor. (If you're curious about how alcohol affects neuropathy, our article on alcoholic neuropathy covers the science.)
Suffering in silence. Not telling your doctor about the anxiety because you're afraid they'll think the pain is “all in your head.” This is one of the most damaging misconceptions in chronic pain. Your pain is real. Anxiety makes it worse, but that doesn't mean the pain is imaginary. A good doctor understands this distinction.
A Day-by-Day Approach to Managing Both
Breaking the pain-anxiety cycle isn't something that happens overnight — it's a gradual process of building habits that calm your nervous system over time. Here's a practical framework many people in my support groups have found helpful:
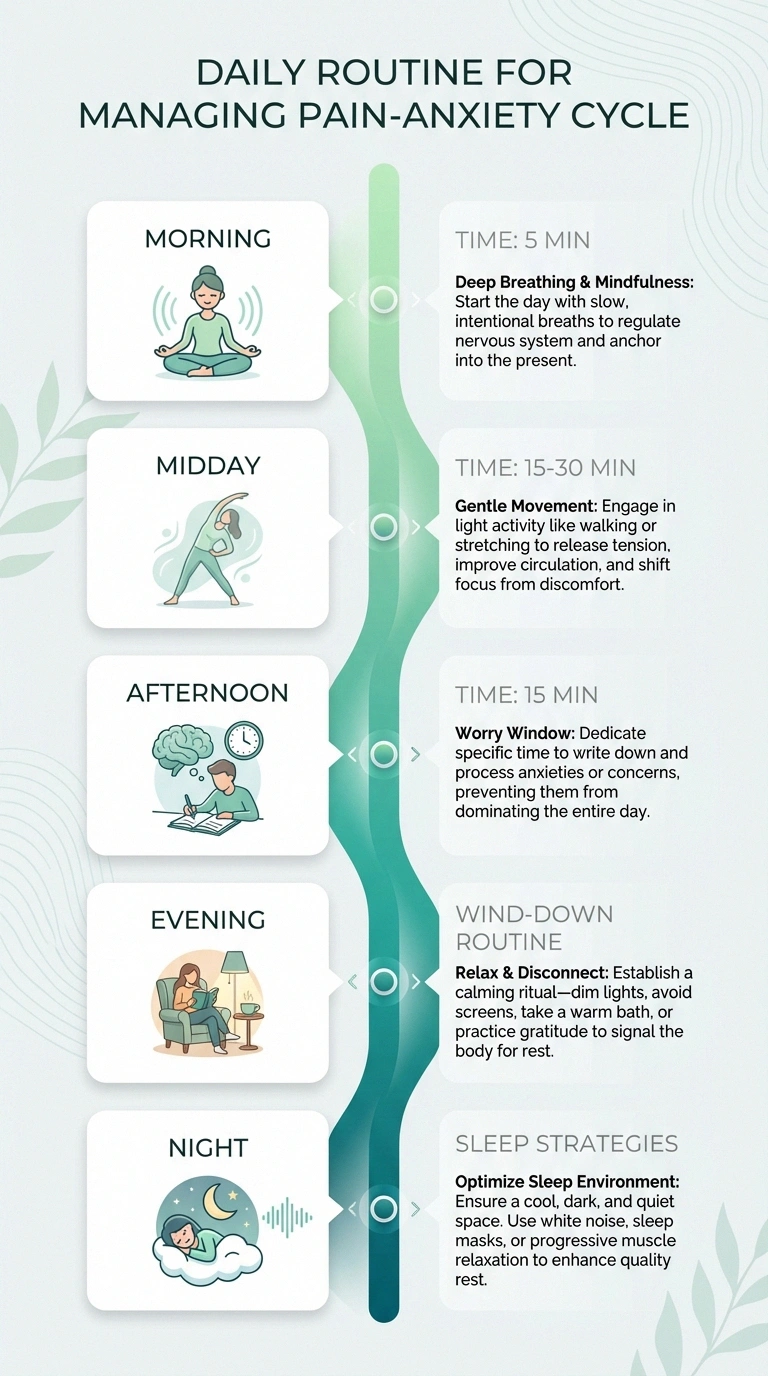
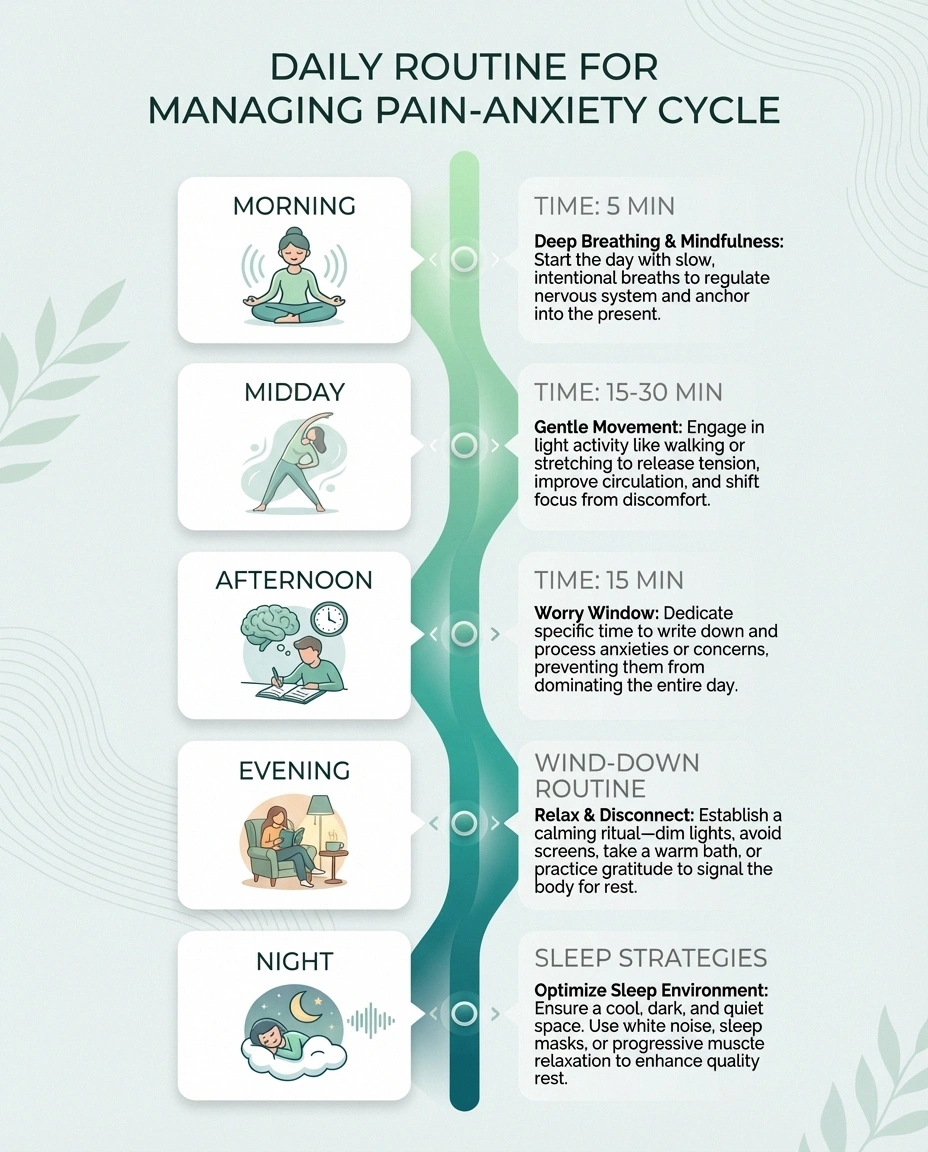
Morning: Start with five minutes of deep breathing or guided meditation before getting out of bed. This activates your parasympathetic nervous system — your body's “rest and digest” mode — counteracting the stress response before your day even begins.
Midday: Incorporate 15 to 30 minutes of gentle movement — a walk, stretching, or seated exercises if mobility is limited. Physical activity during the day helps regulate cortisol and improves sleep quality that night.
Afternoon: Practice a “worry window.” Instead of letting anxiety run unchecked all day, designate 15 minutes to write down your concerns. Outside of that window, when a worry arises, acknowledge it and remind yourself you'll address it during your worry time. This technique comes from CBT and can significantly reduce the constant background hum of anxiety.
Evening: Begin your wind-down routine at least an hour before bed. This might include a warm foot soak, gentle stretching, reading, or listening to calming music. Avoid checking neuropathy forums or symptoms online in the evening — save that for daytime if you need to.
Night: If you wake up with pain and anxiety, have a plan ready. A guided meditation app on your phone, a breathing exercise you've practiced, or a simple grounding technique (naming five things you can see, four you can hear, three you can touch) can interrupt the panic spiral and help you return to sleep.
Frequently Asked Questions
Can anxiety actually cause neuropathy?
Anxiety does not directly damage nerves or cause structural neuropathy. However, chronic anxiety can produce nerve-like symptoms including tingling, numbness, and burning sensations due to nervous system hyperactivation. If you're experiencing these symptoms, it's important to get evaluated by a doctor to determine whether there's actual nerve damage present or whether anxiety may be driving or amplifying the sensations.
Does anxiety make neuropathy pain physically worse, or does it just feel worse?
Both, really. Anxiety triggers the release of cortisol and other stress hormones that increase inflammation and lower your pain threshold — so the pain genuinely is more intense, not just perceived differently. Central sensitization means your brain and spinal cord process the same nerve signals as more painful when anxiety is elevated. The subjective and physical aspects are deeply intertwined.
Will treating my anxiety help my neuropathy symptoms?
For many people, yes. Reducing anxiety may lower cortisol levels, decrease central sensitization, and improve sleep — all of which can lead to meaningful reductions in pain intensity. This doesn't mean anxiety treatment replaces neuropathy treatment, but addressing both together tends to produce better results than treating either one alone.
What type of therapist should I look for?
Look for a psychologist or therapist who specializes in chronic pain management. Pain-focused cognitive behavioral therapy is the most evidence-supported approach. If you can't find a chronic pain specialist, someone experienced in anxiety disorders can also be helpful. Many therapists now offer telehealth sessions, making access easier if mobility is a challenge.
Are anti-anxiety medications safe to take with neuropathy medications?
Many neuropathy medications like duloxetine and pregabalin already have anti-anxiety effects. If additional anxiety treatment is needed, your doctor can prescribe options that are safe alongside your current medications. Always discuss your full medication list with your doctor before adding anything new, including over-the-counter supplements.
My family doesn't understand why I'm so anxious. How do I explain it?
You might explain that chronic pain changes the brain in measurable ways — it's not a choice or a weakness. The pain-anxiety cycle is a well-documented medical phenomenon, not a personal shortcoming. Sharing this article or similar resources can help family members understand that what you're experiencing is a normal neurological response to living with ongoing pain.
Moving Forward: You Don't Have to Choose Between Managing Pain and Managing Anxiety
If there's one thing I want you to take away from this article, it's this: you don't have to accept the pain-worry cycle as permanent. The connection between neuropathy and anxiety is real and well-understood — which means it can be addressed with real strategies that actually work.

You deserve to be treated for both your physical symptoms and the emotional toll they take. These aren't competing priorities — they're two sides of the same coin, and treating both together is the most effective path forward.
Start with one thing. Maybe that's a conversation with your doctor about the anxiety you've been hiding. Maybe it's downloading a meditation app. Maybe it's joining a support group where you can finally talk to people who get it. Whatever it is, know that breaking the cycle is possible — and that the first step is simply acknowledging that both your pain and your relationship anxiety from living with neuropathy deserve attention.
Want to understand more about the how neuropathy grief fuels anxiety side of neuropathy? Read our complete guide to neuropathy and mental health.