Neuropathy and Pets: How Animal Companionship Helps Manage Nerve Pain
When I was first diagnosed with neuropathy, one of the hardest parts wasn't the burning in my feet or the numbness in my hands — it was the isolation. The days shrank. I stopped accepting invitations, stopped taking walks, stopped doing the small things that once made a day feel full. Then my daughter brought over a rescue dog named Biscuit, “just for the weekend.” That weekend turned into something that quietly changed the way I live with this condition. Biscuit didn't cure anything, but he gave me a reason to move, a warm presence on the hard days, and a kind of companionship that doesn't require me to explain what neuropathy feels like.
If you're living with peripheral neuropathy and wondering whether a pet might help — or if you already have a pet and want to make the most of that relationship — this guide is for you. We'll look at what the research says about animal companionship and chronic pain, explore different types of animal-assisted support, and share practical strategies for pet ownership when your body doesn't always cooperate.
The Science Behind Pets and Chronic Pain Relief
The idea that animals help us feel better isn't just sentiment — it's supported by a growing body of research. A 2019 systematic review published in BMC Psychiatry found that pet ownership was associated with significant improvements in mental health outcomes, including reductions in depression and anxiety — two conditions that commonly intensify neuropathic pain.
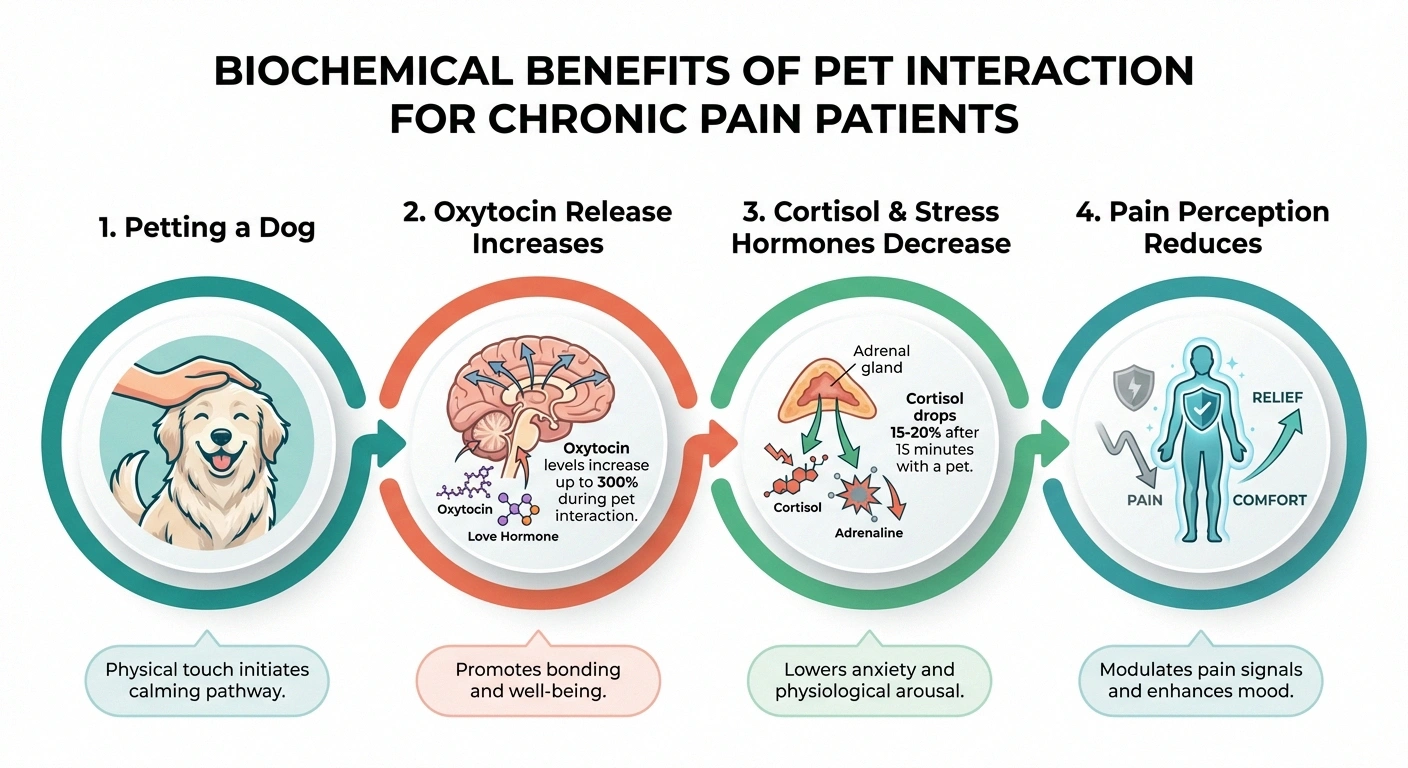
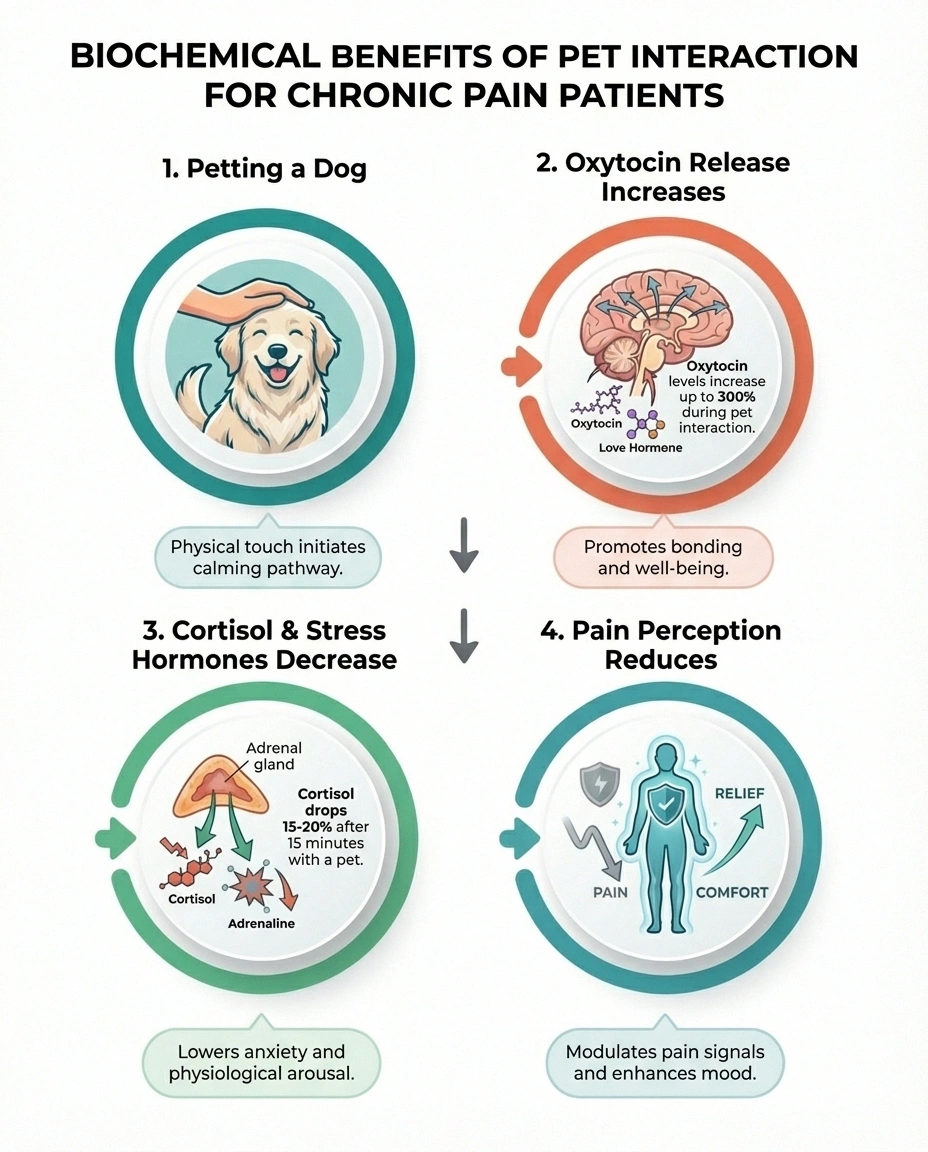
When you pet or cuddle an animal, your body releases oxytocin, sometimes called the “bonding hormone.” This neurochemical response does more than make you feel warm and fuzzy. Oxytocin has been shown to modulate pain perception, reduce cortisol levels (your primary stress hormone), and lower blood pressure. For people with neuropathy, where stress and anxiety frequently amplify pain signals, this biochemical shift may genuinely blunt the experience of nerve pain.
Research from the Human Animal Bond Research Institute (HABRI) has documented that interacting with animals can decrease levels of epinephrine and norepinephrine — the neurotransmitters responsible for the “fight or flight” response that often heightens chronic pain. For those of us whose nervous systems are already misfiring, anything that calms that overactive stress response is worth paying attention to.
A 2020 study in the journal Pain Medicine found that patients who participated in animal-assisted therapy sessions reported significantly lower pain intensity scores compared to control groups. While much of this research examines chronic pain broadly rather than neuropathy specifically, the mechanisms — reduced stress hormones, improved mood, increased physical activity — are directly relevant to how we experience nerve pain.
How Pets Help With Neuropathy Symptoms Beyond Pain
Pain is the headline symptom of neuropathy, but it's rarely the whole story. The emotional toll of neuropathy — depression, anxiety, social withdrawal, disrupted sleep — often does as much damage to quality of life as the nerve pain itself. This is where animal companionship shows its broadest benefits.
Combating Social Isolation and Loneliness
Neuropathy can slowly shrink your world. When walking hurts, when your hands won't cooperate, when fatigue flattens you by mid-afternoon, it's easy to withdraw. Pets provide consistent, unconditional companionship that doesn't depend on you being “well enough.” A cat curled on your lap at 3 AM when the burning in your feet won't let you sleep — that matters more than people realize. Studies consistently show that pet owners report lower levels of loneliness and greater feelings of social connectedness, even when their human social circles have contracted.
Creating Structure and Routine
One of the subtler gifts of pet ownership is the structure it imposes on your day. Dogs need to be walked, cats need to be fed, fish tanks need maintenance. When neuropathy makes every day feel the same blur of discomfort, having a living creature that depends on you creates natural rhythms. That routine can be protective against the depression that so often accompanies chronic pain conditions.
Improving Sleep Quality
Sleep disruption is one of the most common — and most underappreciated — consequences of neuropathy. The burning, tingling, and electric-shock sensations that define nerve pain often intensify at night. Research from the Mayo Clinic suggests that sleeping with a pet in the bedroom (though not necessarily in the bed) may improve sleep efficiency for some adults. The rhythmic breathing of a sleeping dog or the purring of a cat can serve as a natural form of white noise that soothes the hypervigilant nervous system many neuropathy patients develop.
Encouraging Physical Activity
This one is particularly important for neuropathy management. Regular walking and gentle movement are among the most consistently recommended strategies for managing neuropathy symptoms — yet pain and fatigue make it profoundly difficult to motivate yourself. Dog owners consistently walk more than non-dog owners. A 2019 study from the University of Liverpool found that dog owners were four times more likely to meet recommended physical activity guidelines. That extra movement improves circulation, supports nerve health, and may help slow neuropathy progression.

Types of Animal-Assisted Support for Neuropathy Patients
Not all animal relationships serve the same purpose, and understanding the distinctions can help you find the right fit for your situation.

Companion Pets
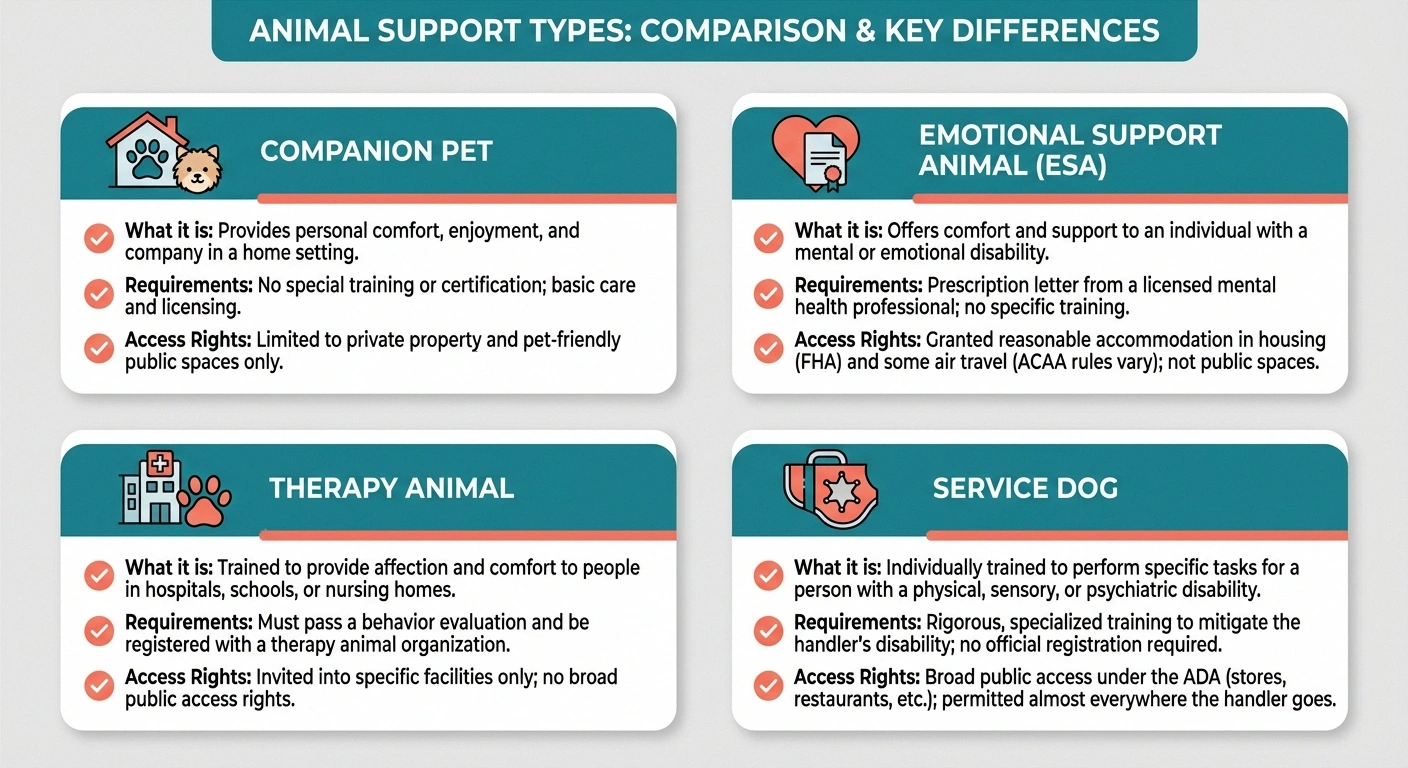
The most common and accessible option. A companion pet is simply your pet — the dog who greets you at the door, the cat who claims your lap, the bird who chatters while you read. No special training or certification is needed. The benefits come from the daily relationship: the routine, the affection, the sense of being needed. For most people with neuropathy, a well-chosen companion pet provides the majority of the benefits research has documented.
Emotional Support Animals (ESAs)
An emotional support animal is prescribed by a mental health professional as part of a treatment plan for a diagnosed mental health condition — such as the depression or anxiety that frequently accompanies neuropathy. ESAs don't require specialized training, but the letter from your provider may entitle you to housing accommodations under the Fair Housing Act. If neuropathy-related anxiety is significantly impacting your daily life, discussing an ESA designation with your therapist or psychiatrist may be worthwhile.
Therapy Animals
Therapy animals are trained and certified to provide comfort in institutional settings — hospitals, rehabilitation centers, nursing homes, and chronic pain clinics. If you're undergoing treatment at a facility that offers animal-assisted therapy programs, these structured sessions can provide measurable pain relief and mood improvement. Ask your treatment team whether animal-assisted therapy is available in your area.
Service Dogs for Neuropathy
Service dogs are individually trained to perform specific tasks for people with disabilities. For neuropathy patients, this might include balance assistance (critical for those with neuropathy-related balance problems), alerting to temperature dangers when you can't feel heat or cold, retrieving dropped objects when hand numbness makes gripping difficult, or providing bracing support during transfers. Service dogs have legal access rights under the Americans with Disabilities Act (ADA) and can accompany you in public spaces, including stores, restaurants, and medical facilities.

Choosing the Right Pet When You Have Neuropathy
Selecting a pet when you have a chronic condition requires honest self-assessment. The wrong pet — one whose care demands exceed your physical capacity — can add stress rather than relieve it. Here's how to think through the decision.
Care level: High (walks, grooming, training)
Consider: Smaller, calm breeds for stability
Evidence: Strongest research for health benefits
Care level: Moderate (feeding, litter, vet visits)
Consider: Purring frequencies (25-150 Hz) linked to pain reduction
Evidence: Strong for stress and anxiety reduction
Care level: Low to moderate
Consider: Fish tanks lower BP and heart rate; rabbits offer tactile comfort
Evidence: Moderate for stress reduction
Dogs: The Most Studied Option
Dogs offer the strongest evidence for health benefits, largely because they encourage physical activity and social interaction. Consider breed size and energy level carefully. A high-energy border collie that needs two hours of daily exercise is probably not the right match if you're dealing with significant foot pain. Breeds to consider include cavalier King Charles spaniels, Shih Tzus, pugs, and older rescue dogs of various breeds — animals that are content with moderate activity and thrive on close human companionship. Smaller dogs also pose less risk if you have balance issues, since they're less likely to pull you off your feet on a leash.
Cats: Low-Maintenance Companionship
Cats are an excellent option for people whose neuropathy makes dog walking difficult or impossible. Their purring has been studied as a potential therapeutic mechanism — cats purr at frequencies between 25 and 150 Hz, a range that has been associated with pain reduction and even bone healing in some preliminary research. Cats don't require outdoor walks, are generally less physically demanding to care for, and provide warm, gentle contact that many neuropathy patients find soothing — especially when a cat settles on aching feet or rests against sore legs.

Small Animals and Fish
Don't overlook smaller options. Watching fish in an aquarium has been shown to lower blood pressure and heart rate. Rabbits, guinea pigs, and hamsters provide tactile comfort without the physical demands of larger pets. If hand numbness makes handling small animals difficult, consider species that are content to be observed rather than held.
Practical Tips for Pet Care With Neuropathy
Owning a pet with neuropathy requires some creative problem-solving. The goal is to enjoy the benefits of companionship without pushing your body past its limits.

Adapting Daily Pet Care Tasks
Many common pet care tasks — opening cans, pouring food, bending to fill water bowls — can be challenging when your hands are numb or your balance is unreliable. Consider these adaptations:
• Auto feeders — Backup for high-pain days
• Hands-free leash — Clips to belt, no grip required
• Self-cleaning litter — Eliminates scooping
• Easy-grip brushes — Built-up handles for grooming
- Elevated feeding stations — Raised food and water bowls eliminate the need to bend down, reducing fall risk and back strain
- Automatic feeders and water fountains — Reduce the daily physical demands of pet feeding, especially useful on high-pain days
- Easy-grip tools — Built-up handles on scoops, brushes, and leashes make tasks manageable when hand numbness is severe
- No-bend litter boxes — Top-entry or self-cleaning litter boxes minimize bending and scooping
- Slip-on leash attachments — Hands-free leash systems that clip to a belt or wrap around the wrist are safer than traditional grip-dependent leashes when your grip strength is compromised
Managing Walks With Neuropathy
If you have a dog, walking is likely both a challenge and an opportunity. Use proper footwear designed for neuropathy to maximize stability. Keep walks short and consistent rather than long and infrequent — 10 to 15 minutes twice a day is often better than one 30-minute walk that leaves you exhausted. Choose flat, even terrain. Consider a walking aid or cane if your balance is affected, and use a no-pull harness on your dog to prevent sudden jolts that could throw you off balance.
Building a Support Network for Pet Care
On your worst neuropathy days, you may not be able to manage all pet care tasks alone — and that's okay. Build a support network in advance:
- Identify a neighbor, friend, or family member who can step in for dog walks during flare-ups
- Research local dog-walking services and pet-sitting options
- Consider a pet care exchange with another pet owner — you help on their tough days, they help on yours
- Look into volunteer programs through local animal shelters that sometimes offer assistance to disabled pet owners
The Emotional Bond: Why It Matters for Pain Management
There's a concept in pain research called the “pain-mood cycle” — pain worsens mood, worsened mood amplifies pain perception, and the spiral deepens. Pain catastrophizing — the tendency to ruminate on, magnify, and feel helpless about pain — is one of the strongest predictors of poor outcomes in chronic pain conditions, including neuropathy.

Pets interrupt this cycle in ways that are difficult to replicate with other interventions. A dog that demands a walk forces you out of rumination. A cat that purrs on your chest shifts your sensory focus from pain signals to pleasant touch. The unconditional acceptance animals provide counters the sense of being a burden that so many chronic pain patients carry.
This isn't about replacing medical treatment — it's about recognizing that living well with neuropathy involves managing the whole person, not just the damaged nerves. Mindfulness practices, social connection, physical activity, and emotional regulation all play roles in how we experience pain. Pets contribute to every single one of these domains.
Animal-Assisted Therapy Programs: What to Expect
If you're not ready for pet ownership — or if your living situation doesn't allow it — formal animal-assisted therapy programs offer a structured alternative. These programs bring trained therapy animals (usually dogs, but sometimes horses, rabbits, or even llamas) into clinical or community settings.

Sessions typically last 15 to 60 minutes and may be individual or group-based. During a session, you might pet and groom the animal, practice gentle exercises alongside them, or simply sit with the animal while discussing your pain management strategies with a therapist. Many chronic pain clinics, rehabilitation hospitals, and neuropathy support groups now incorporate animal-assisted activities.
Equine-assisted therapy (involving horses) is a particularly interesting option for neuropathy patients. The rhythmic movement of horseback riding provides proprioceptive input that may help retrain balance and body awareness — both commonly impaired in peripheral neuropathy. Several rehabilitation programs across the country now offer adaptive horseback riding specifically for adults with neurological conditions.
Safety Considerations for Pet Owners With Neuropathy
While the benefits of pets are substantial, there are real safety considerations to address when neuropathy affects your sensation, balance, or strength.

Fall Prevention Around Pets
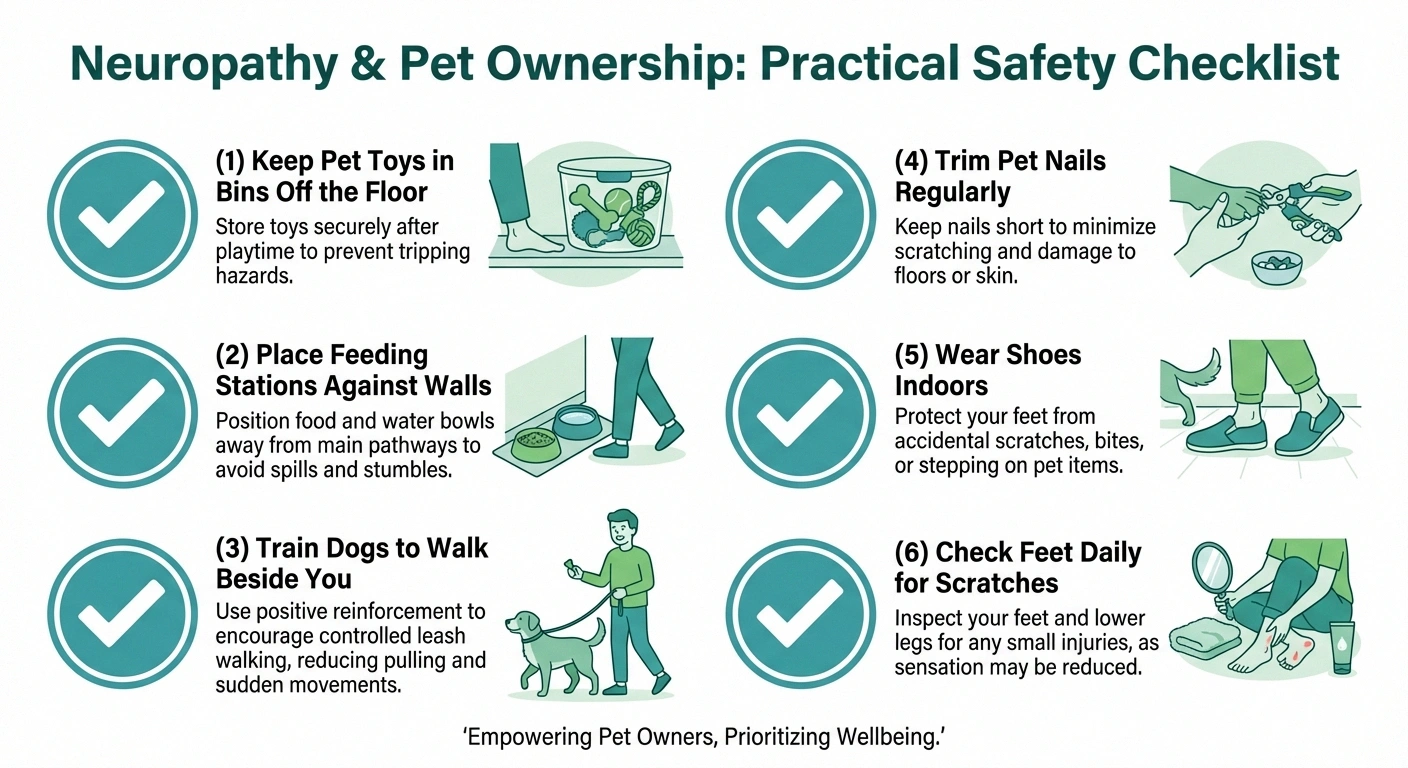
Pets and fall risk can be a dangerous combination. Small dogs that weave between your feet, cat toys left on the floor, and feeding stations in walkways all create tripping hazards. Practical steps include:
- Keep pet toys in designated bins, not scattered on the floor
- Place feeding stations against walls rather than in traffic areas
- Train dogs to walk beside you rather than darting in front
- Use pet gates to keep animals out of areas where you're most unsteady (stairs, bathroom)
- Install adequate lighting in areas where pets tend to rest on the floor — you can't step over what you can't see
Protecting Numb Extremities
When you can't feel your feet or hands fully, pet-related injuries can go unnoticed. Cat scratches on numb feet, dog bites that don't register as pain, or stepping on pet-related items without feeling them can all lead to wounds that, especially for people with diabetic neuropathy, carry serious infection risk. Check your hands and feet daily for any injuries, keep pets' nails trimmed, and wear protective footwear — even indoors — as part of your daily foot care routine.
Financial and Practical Considerations
Pet ownership has real costs, and managing neuropathy already strains many budgets. Before committing, consider:

• Volunteer at a local shelter — Regular interaction without ownership costs
• Foster programs — Shelter covers all medical and food expenses
• Animal-assisted therapy sessions — May be covered by health insurance
• Pet-sit for friends/family — Companionship on your schedule
- Veterinary costs — Annual checkups, vaccinations, and unexpected illnesses or injuries. Budget at least $500-$1,000 per year for routine veterinary care; more for older pets
- Food and supplies — Quality pet food, litter, bedding, and toys can run $50-$150 per month depending on the animal
- Pet insurance — May help manage unexpected veterinary costs; plans typically run $30-$60 per month
- Emergency backup care — If you're hospitalized or in a severe flare, who will care for your pet?
If finances are a concern, consider volunteering at a local animal shelter. You get regular animal interaction — and many of the psychological benefits — without the full financial commitment of ownership. Some shelters also offer “foster” programs where you temporarily house animals, with the shelter covering all medical and food costs.

Frequently Asked Questions
Can pets actually reduce neuropathy pain?
Pets may help reduce the perception of neuropathy pain through several mechanisms: lowering stress hormones (cortisol, epinephrine), increasing oxytocin release, encouraging physical activity, and interrupting the pain-mood cycle that amplifies chronic pain. While no animal can heal damaged nerves, the combined effects of companionship, stress reduction, and increased movement may meaningfully reduce how much pain dominates your daily experience.
What is the best type of pet for someone with neuropathy?
The best pet depends on your specific symptoms and physical capabilities. Dogs offer the most studied health benefits and encourage exercise, but require more physical care. Cats provide soothing companionship with lower physical demands. Small animals like rabbits or fish offer benefits with minimal care requirements. Consider your energy level, balance stability, hand function, and living situation when deciding.
Can I get a service dog for peripheral neuropathy?
Yes, you may qualify for a service dog if neuropathy substantially limits one or more major life activities. Service dogs can be trained for balance assistance, alerting to temperature dangers, retrieving objects, and providing physical support during walking. The process typically involves working with a service dog organization, and wait times can be one to two years. Costs vary from free (through nonprofit organizations) to $15,000 or more from private trainers.
Is it safe to have a pet if I have numbness in my feet?
Pet ownership is generally safe with numbness, but requires extra precautions. Keep floors clear of pet toys, trim your pet's nails regularly, wear protective footwear indoors, inspect your feet daily for unnoticed scratches or injuries, and ensure good lighting in areas where your pet rests on the floor. If you have diabetes-related neuropathy, be especially vigilant about any pet-related wounds on your feet, as these can develop into serious infections.
How do I manage pet care on bad neuropathy days?
Build a support network before you need it. Identify neighbors, friends, or family who can help with walks or feeding during flare-ups. Research local dog-walking services. Invest in automatic feeders and water fountains for backup. Consider a pet care exchange with another pet owner. For cats and small animals, prepare food and water for an extra day in advance so care can continue even when you cannot manage it yourself.
Does pet insurance cover therapy animals?
Standard pet insurance covers veterinary care for your animal regardless of its designation as a companion, ESA, or therapy animal. However, the costs associated with animal-assisted therapy sessions at clinics or hospitals are typically covered under your own health insurance, not pet insurance. Check with your health plan about coverage for complementary therapies, which sometimes include animal-assisted therapy programs.

Making the Decision: Is a Pet Right for You?
The research is clear that animal companionship offers real benefits for people living with chronic pain conditions like neuropathy. But the decision to bring a pet into your life should be grounded in an honest assessment of your current capabilities, your support network, and your financial situation.
Talk to your healthcare team — your neurologist, physical therapist, or mental health professional — about whether a pet might support your overall management plan. If ownership isn't feasible right now, explore alternatives: volunteering at shelters, participating in animal-assisted therapy programs, or simply spending time with friends' or family members' pets.
What I can tell you from experience is this: Biscuit didn't make my neuropathy go away. My feet still burn, my hands still go numb, and some mornings I wonder how I'll make it through the day. But having a warm, loyal companion who doesn't care about any of that — who just wants to sit beside me and be present — that changes the texture of a difficult life. And sometimes, changing the texture is enough.
