
Intermittent fasting has become one of the most talked-about health trends of the past decade — and increasingly, research is exploring whether it might benefit people with neuropathy. A landmark 2022 study from Imperial College London found that intermittent fasting changed gut bacteria in ways that boosted nerve regeneration by 50% in animal models. Headlines were exciting. But as someone who lives with neuropathy and has learned the hard way to separate hype from evidence, I wanted to dig deeper into what the research actually shows — the promising findings, the disappointing results, and the important safety warnings that most articles leave out.
The honest answer is that the science on intermittent fasting and neuropathy is still early, with both encouraging and cautionary results. This article gives you the full picture so you and your doctor can make informed decisions about whether intermittent fasting might have a role in your neuropathy management plan.
What Is Intermittent Fasting?
Intermittent fasting (IF) isn't about what you eat — it's about when you eat. Instead of restricting specific foods, IF cycles between periods of eating and periods of fasting. The most common approaches include:
IF Is About When, Not What
Intermittent fasting doesn't restrict what you eat — it structures when you eat. The most beginner-friendly approach is 16:8: eat within an 8-hour window (e.g., noon to 8 PM) and fast for 16 hours. Not all protocols have been studied for neuropathy, so results from one approach don't necessarily apply to another.
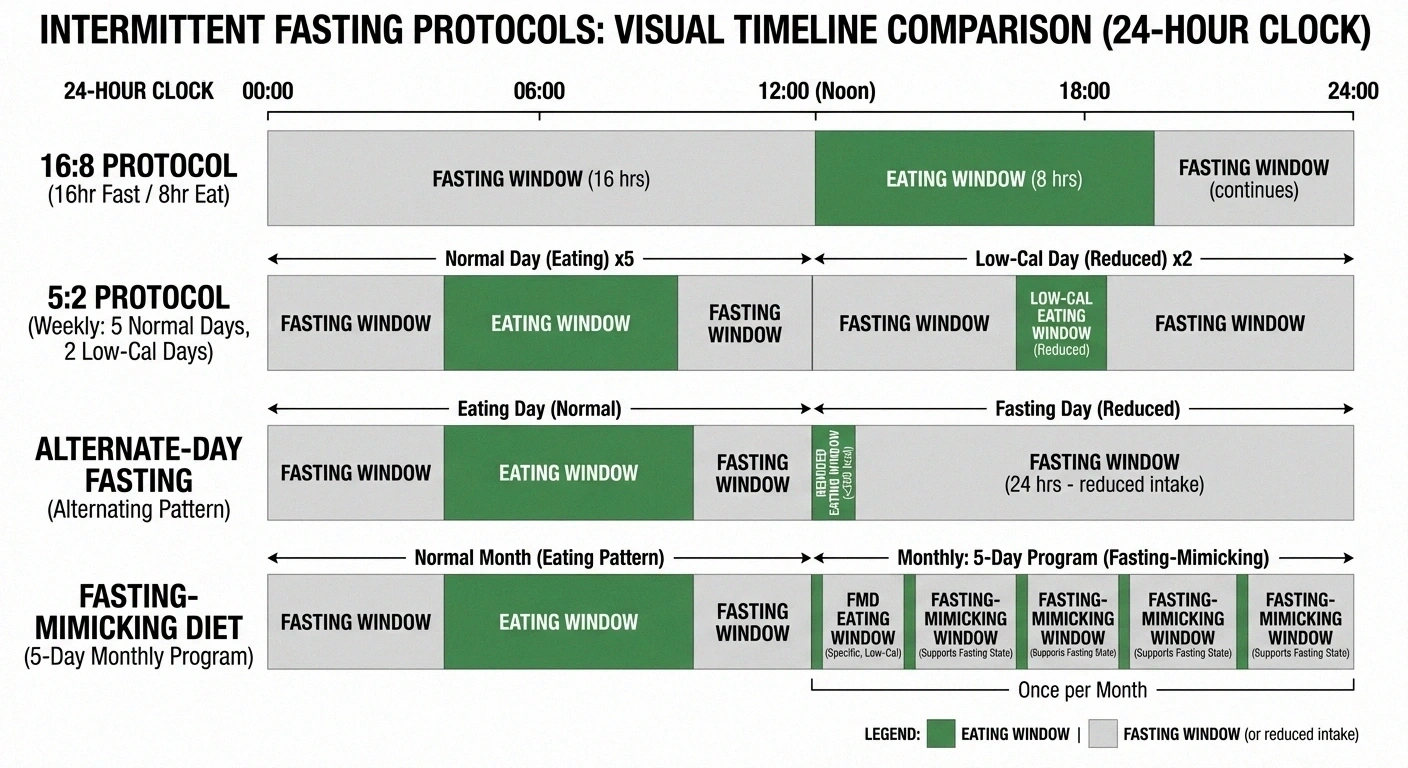
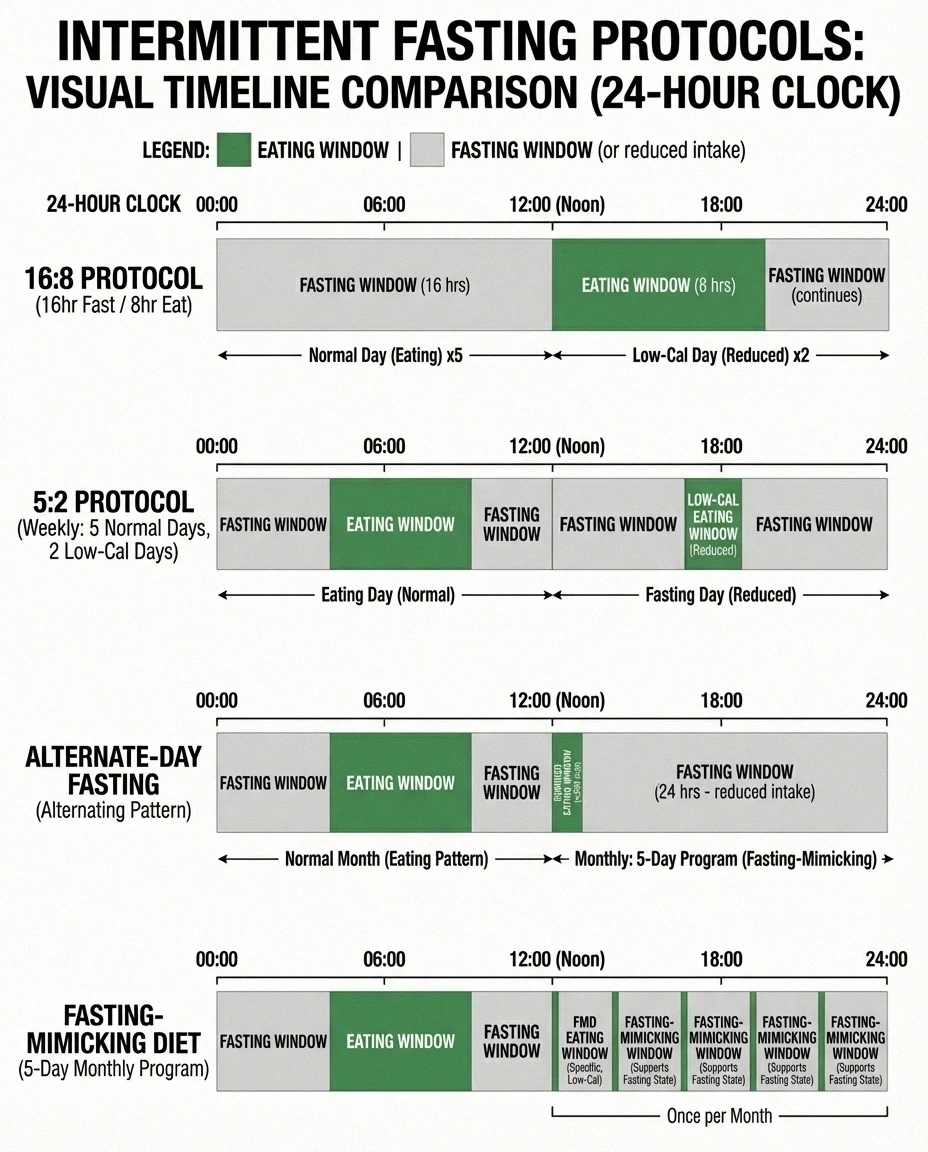
16:8 (time-restricted eating): You eat within an 8-hour window each day and fast for the remaining 16 hours. For example, eating between noon and 8 PM. This is the most popular and generally easiest-to-follow IF protocol.
5:2 method: You eat normally five days a week and significantly reduce calories (about 500-600) on two non-consecutive days.
Alternate-day fasting: You alternate between normal eating days and fasting or very-low-calorie days.
Fasting-mimicking diet: A structured program (typically 5 days per month) that uses specific low-calorie, low-protein, high-fat food to trigger fasting-like metabolic responses while still eating some food.
Each protocol triggers somewhat different metabolic responses, which matters when we look at the neuropathy research — not all fasting approaches have been studied equally, and results from one protocol don't necessarily apply to another.
The Landmark Gut-Nerve Connection Study
The study that put intermittent fasting and neuropathy on the map was published in Nature in 2022 by researchers at Imperial College London. Here's what they found, and why it matters:
The Gut-Nerve Pathway
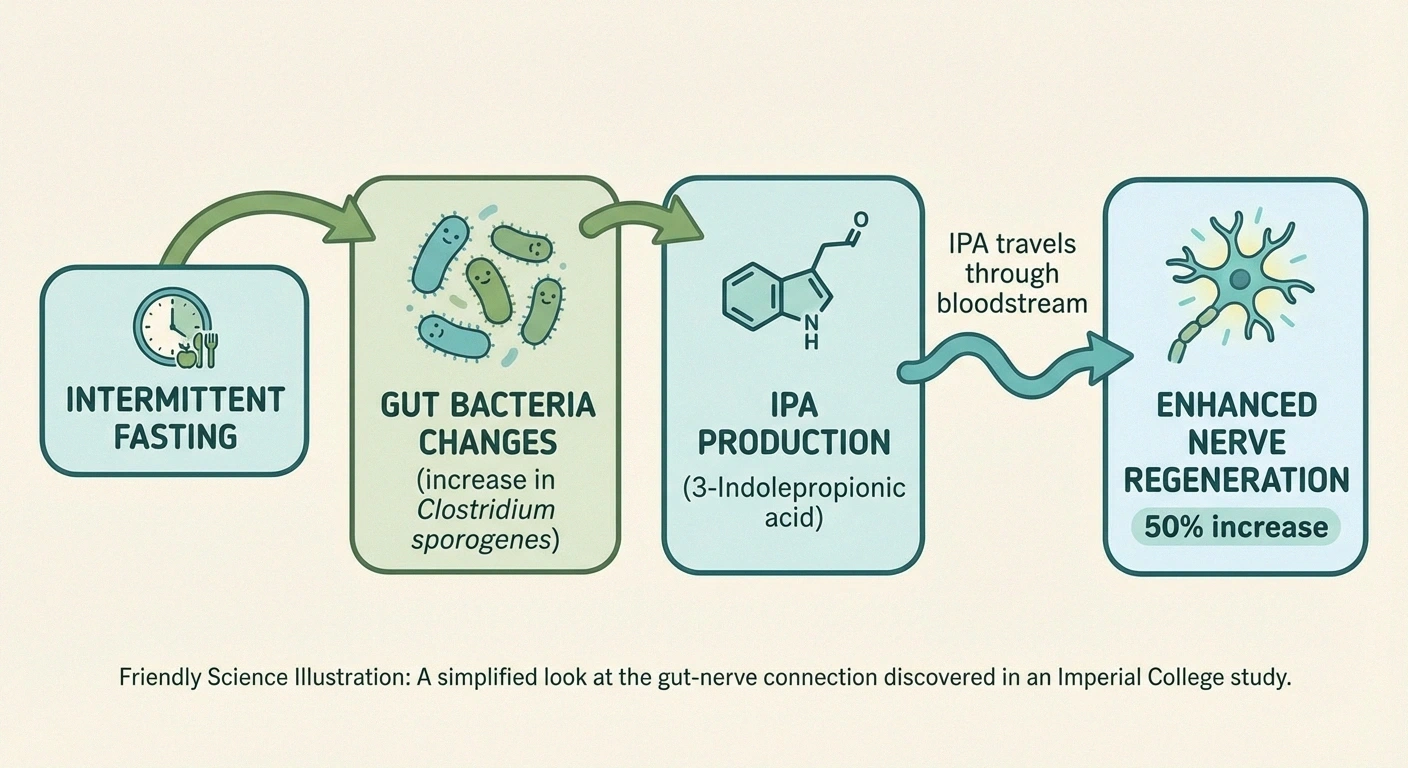
Researchers studied mice that had undergone sciatic nerve crush injuries — a model used to study nerve regeneration. Mice that were placed on an intermittent fasting regimen (alternate-day fasting) showed approximately 50% greater axon regrowth compared to mice fed normally.
The mechanism was fascinating and unexpected. IF didn't act directly on the nerves. Instead, it changed the composition of gut bacteria. Specifically, fasting increased the abundance of a bacterium called Clostridium sporogenes, which produces a metabolite called 3-Indolepropionic acid (IPA). When IPA traveled through the bloodstream to the site of nerve damage, it enhanced the regeneration process.
The researchers confirmed this gut-nerve connection through several elegant experiments: they showed that giving mice IPA directly (without fasting) produced similar nerve regeneration benefits, and that eliminating gut bacteria with antibiotics blocked the fasting benefit. This strongly suggests it's the gut metabolite IPA, not fasting itself, that's the active ingredient for nerve repair.
This is genuinely exciting science. It identifies a specific molecular pathway connecting diet, gut bacteria, and nerve regeneration. But there are important caveats: this was a mouse study, the nerve damage model (crush injury) is different from the gradual, diffuse damage of neuropathy, and the results have not yet been replicated in human neuropathy patients.
The Klotho Gene Connection
A more recent 2025 study published in Springer added another piece to the puzzle. Researchers found that 16:8 intermittent fasting reversed diabetic neuropathy in mice through activation of the Klotho gene — sometimes called the “anti-aging gene.”
Klotho protein has been shown to have neuroprotective properties, including reducing oxidative stress and inflammation — both of which contribute to nerve damage in diabetic neuropathy. The study found that IF upregulated Klotho expression, which in turn reduced markers of nerve damage and improved nerve function in diabetic mice.
This study is significant because it used the 16:8 protocol (the most practical IF approach for humans) and specifically studied diabetic neuropathy (the most common type). However, the same caveat applies: these are mouse results, and animal studies don't always translate to humans.
The Human Study That Showed No Benefit
Here's where we need to be completely honest — because most articles promoting IF for neuropathy conveniently skip this one.
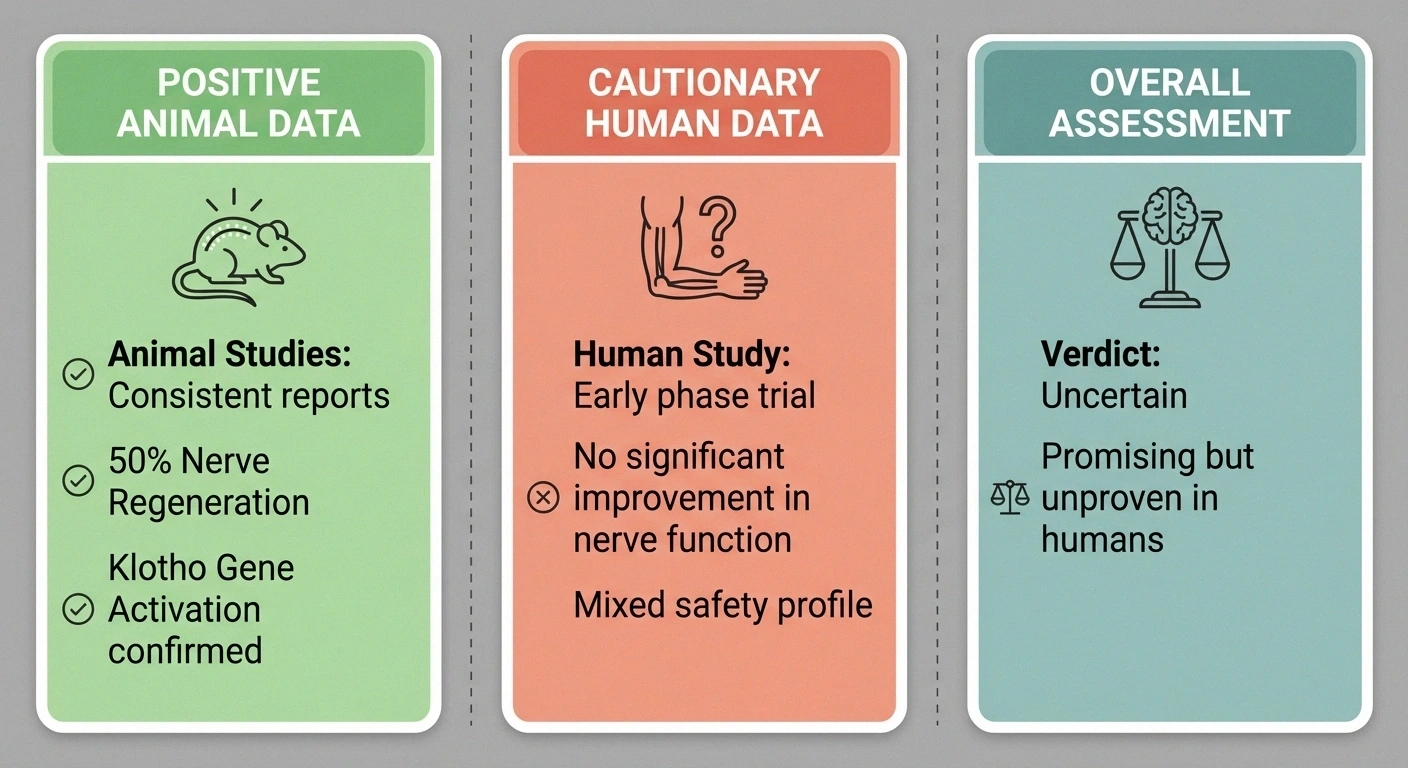
The Evidence So Far — Honest Assessment
A 2023 study published in Frontiers in Endocrinology examined whether a fasting-mimicking diet (a structured program that triggers fasting-like metabolic responses) affected nerve function in people with type 2 diabetes. Participants followed the fasting-mimicking protocol for 6 months.
The result: the fasting-mimicking diet did not significantly affect somatosensory nerve function in these patients. Nerve conduction measurements showed no meaningful improvement compared to the control group.
This is important context. It doesn't necessarily mean IF can't help neuropathy — there are legitimate reasons why this particular study might not have shown benefit:
— The fasting-mimicking diet is not the same protocol as the alternate-day fasting used in the Imperial College mouse study or the 16:8 protocol from the Klotho study
— Six months may not be long enough to show nerve regeneration changes, given that nerves regenerate at just 1 to 3 millimeters per day
— The participants had established type 2 diabetes, meaning their neuropathy was likely more advanced
But the honest takeaway is this: we currently have zero controlled human studies showing that any form of intermittent fasting improves neuropathy symptoms or nerve function. The positive results are all from animal models. That matters, and it should calibrate your expectations.
Other Research Supporting the Fasting-Nerve Connection
Beyond the headline studies, several other lines of research provide context:
A 2013 study in the Proceedings of the National Academy of Sciences found that dietary restriction supports peripheral nerve health through improved protein quality control — essentially, fasting helps cells clean out damaged proteins and replace them with functional ones. This process, called autophagy, is one of the most well-established biological benefits of fasting.
Research on blood sugar control consistently shows that IF may improve insulin sensitivity and reduce blood glucose levels, which could indirectly benefit neuropathy patients whose nerve damage is driven by high blood sugar. Better blood sugar control means less ongoing damage to nerves.
Fasting has also been shown to reduce systemic inflammation — and chronic inflammation is a known contributor to nerve damage. An anti-inflammatory approach to eating may support nerve health through multiple pathways, and IF's anti-inflammatory effects could be part of this picture.
A Critical Safety Warning: Slimmer's Palsy
Before anyone with neuropathy jumps into intermittent fasting, there's a safety concern that demands attention.
Safety Warning: Slimmer's Palsy
Rapid weight loss from aggressive fasting has been documented to cause bilateral peroneal nerve palsy (foot drop) by depleting protective fat around the peroneal nerve near the knee.
For neuropathy patients: Your nerves are already compromised. Gradual weight loss (1-2 lbs/week max) is essential.
Stop fasting and contact your doctor immediately if you notice new weakness, foot drop, or worsening symptoms.
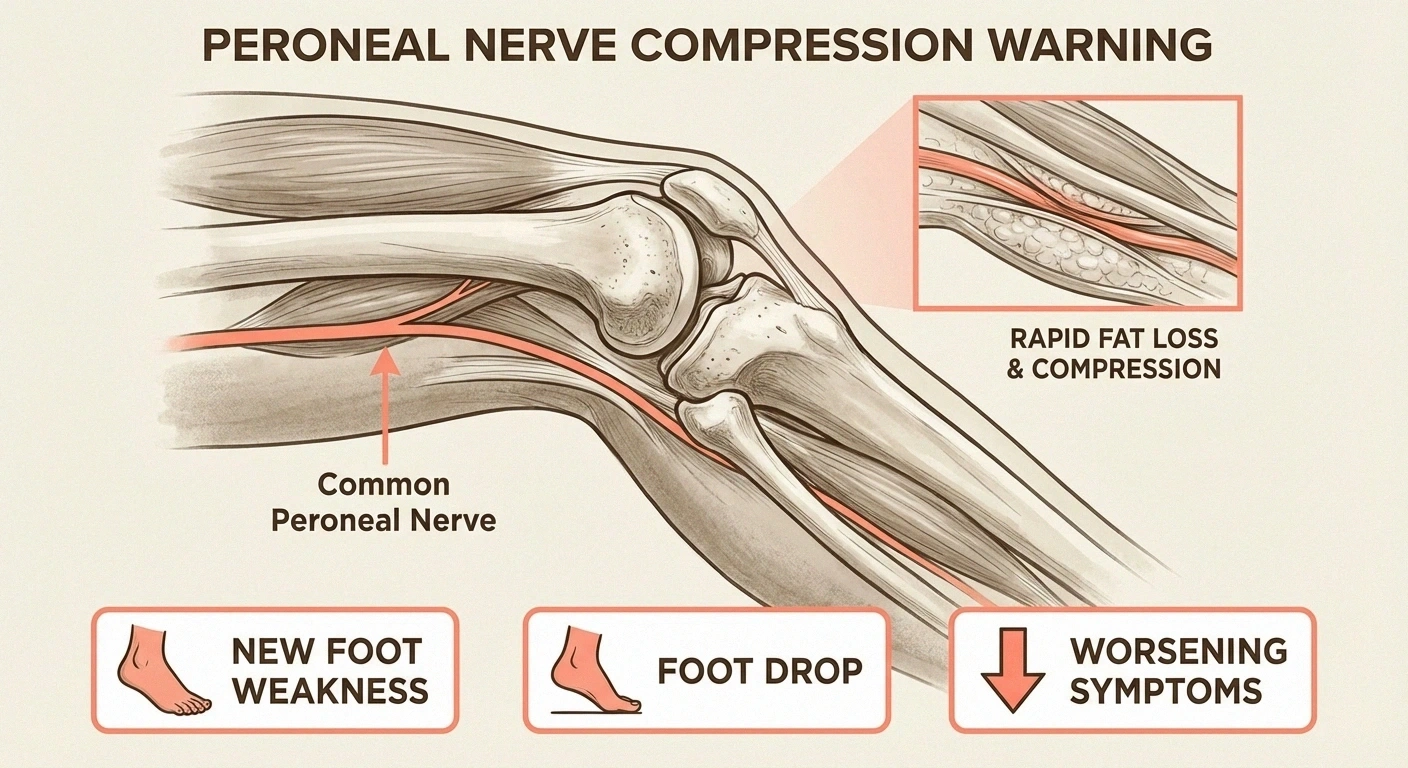
Case reports have documented a condition called “slimmer's palsy” — where rapid weight loss (sometimes associated with aggressive fasting protocols) caused bilateral peroneal nerve palsy, resulting in foot drop in both feet. The peroneal nerve, which runs near the knee, is vulnerable to compression when the protective fat cushion around it is lost too quickly.
For someone already living with neuropathy, this is particularly concerning. Your nerves are already compromised, and rapid weight loss could add mechanical nerve damage on top of your existing condition.
This doesn't mean intermittent fasting is inherently dangerous for neuropathy patients. The risk is specifically associated with rapid, significant weight loss, not with moderate, controlled fasting protocols. But it's a clear reason why:
— You should talk to your doctor before starting any fasting protocol
— Gradual weight loss (1-2 pounds per week maximum) is safer than aggressive approaches
— Extreme fasting protocols (extended water fasts, very-low-calorie diets) carry higher risk
— If you notice any new weakness, foot drop, or worsening symptoms, stop fasting and contact your doctor immediately
Medication Interactions and Safety Considerations
If you're taking medications for neuropathy or other conditions, intermittent fasting introduces additional considerations that your doctor needs to know about:
Medication Interactions to Discuss with Your Doctor
Diabetes medications. If you take insulin or sulfonylureas (glipizide, glimepiride), fasting significantly increases the risk of hypoglycemia — dangerously low blood sugar. This is especially relevant for neuropathy patients with diabetes, who may already have reduced awareness of hypoglycemic symptoms due to autonomic nerve damage. Never start fasting while on these medications without medical supervision.
Neuropathy medications. Gabapentin and pregabalin are typically taken with food. Fasting may affect absorption and timing. Duloxetine should be taken with food to reduce stomach upset. Discuss timing adjustments with your pharmacist or doctor.
Blood pressure medications. Fasting can lower blood pressure, and combining that with antihypertensive medications may cause dizziness or fainting — a real fall risk for people who already have balance issues from neuropathy.
Nutritional deficiency risk. If fasting reduces your overall food intake significantly, you may not get adequate B vitamins, magnesium, and other nutrients essential for nerve health. Ironically, fasting to help your nerves could worsen a nutritional deficiency that's damaging them. Talk to your doctor about whether supplementation is needed.
Practical Guidance If You Want to Try IF
If you've discussed it with your doctor and want to explore intermittent fasting, here's a practical, evidence-informed approach:
Safe IF Approach for Neuropathy Patients
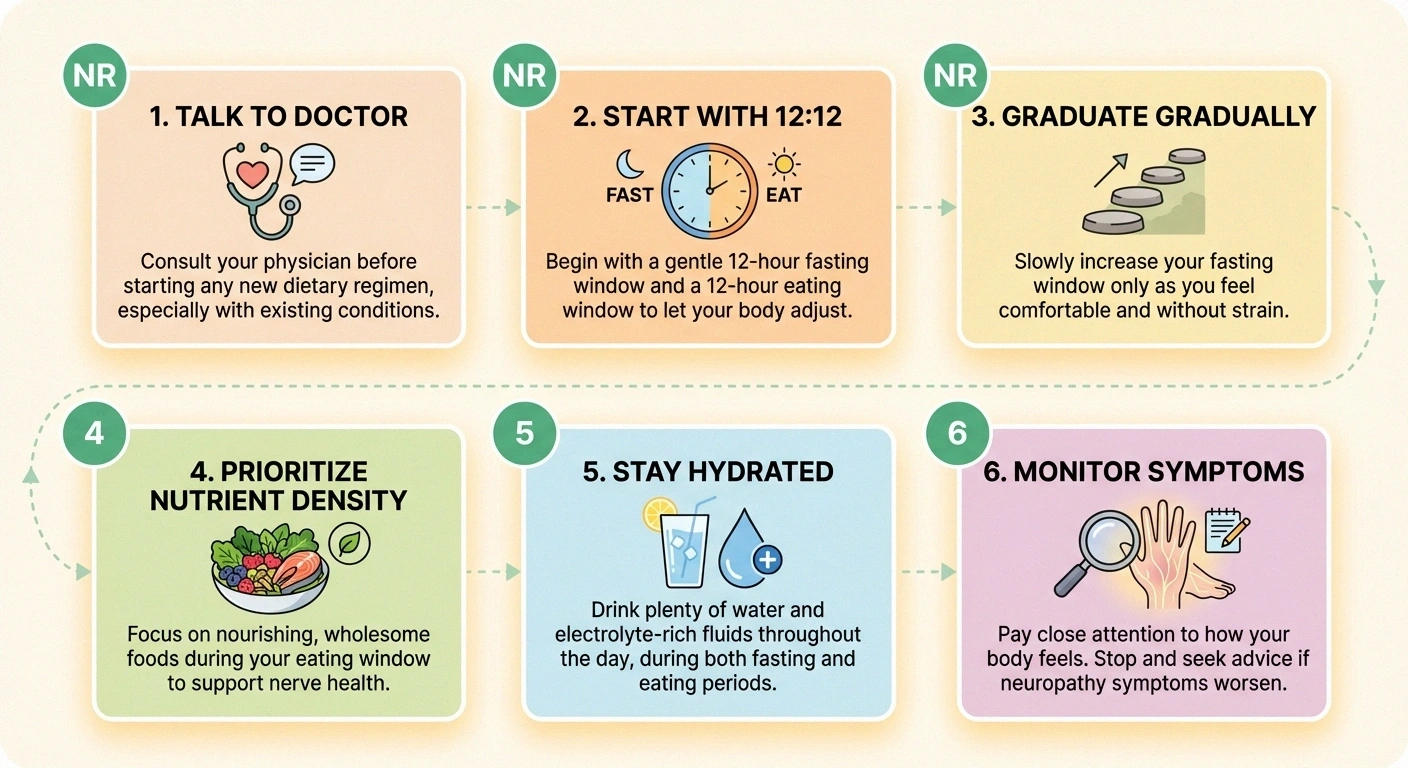
Start with 12:12. Before jumping to 16:8, try simply eating within a 12-hour window. This is mild enough that most people tolerate it well, and some research suggests benefits begin at this level. If you normally eat breakfast at 7 AM, finish dinner by 7 PM.
Graduate to 14:10, then 16:8 gradually. Narrow your eating window by an hour every 1 to 2 weeks. This gives your body time to adapt and reduces the risk of blood sugar drops, especially if you're on medications.
Prioritize nutrient density during eating windows. When you do eat, focus on foods that support nerve health: fatty fish, leafy greens, nuts, seeds, whole grains, and colorful vegetables. Your neuropathy diet matters more than ever when eating windows are restricted. Every meal needs to count nutritionally.
Stay well hydrated. Drink water, herbal tea, and other non-caloric beverages throughout the fasting period. Dehydration can worsen neuropathy symptoms and increase fall risk.
Monitor your symptoms. Keep a journal tracking your neuropathy symptoms, energy levels, sleep quality, and any new or worsening issues. Look for trends over weeks, not days. If symptoms worsen, stop and reassess with your doctor.
Don't combine IF with calorie restriction unless medically supervised. IF is about when you eat, not how much. Eating adequate calories during your window is important, especially if you're already at a healthy weight. Aggressive calorie restriction increases the slimmer's palsy risk.
Consider the IPA shortcut. Since the Imperial College research suggests IPA (the gut metabolite) is the key player, some researchers speculate that increasing IPA through probiotic approaches or IPA-producing dietary patterns might offer similar benefits without fasting. This is still theoretical, but foods high in tryptophan (turkey, eggs, cheese, nuts) provide the raw material that Clostridium sporogenes converts to IPA. More research is needed here, but it's a line of investigation worth watching.
Who Should NOT Try Intermittent Fasting
Intermittent fasting is not appropriate for everyone, and certain neuropathy patients should avoid it entirely unless specifically cleared by their doctor:
Who Should NOT Fast Without Medical Clearance
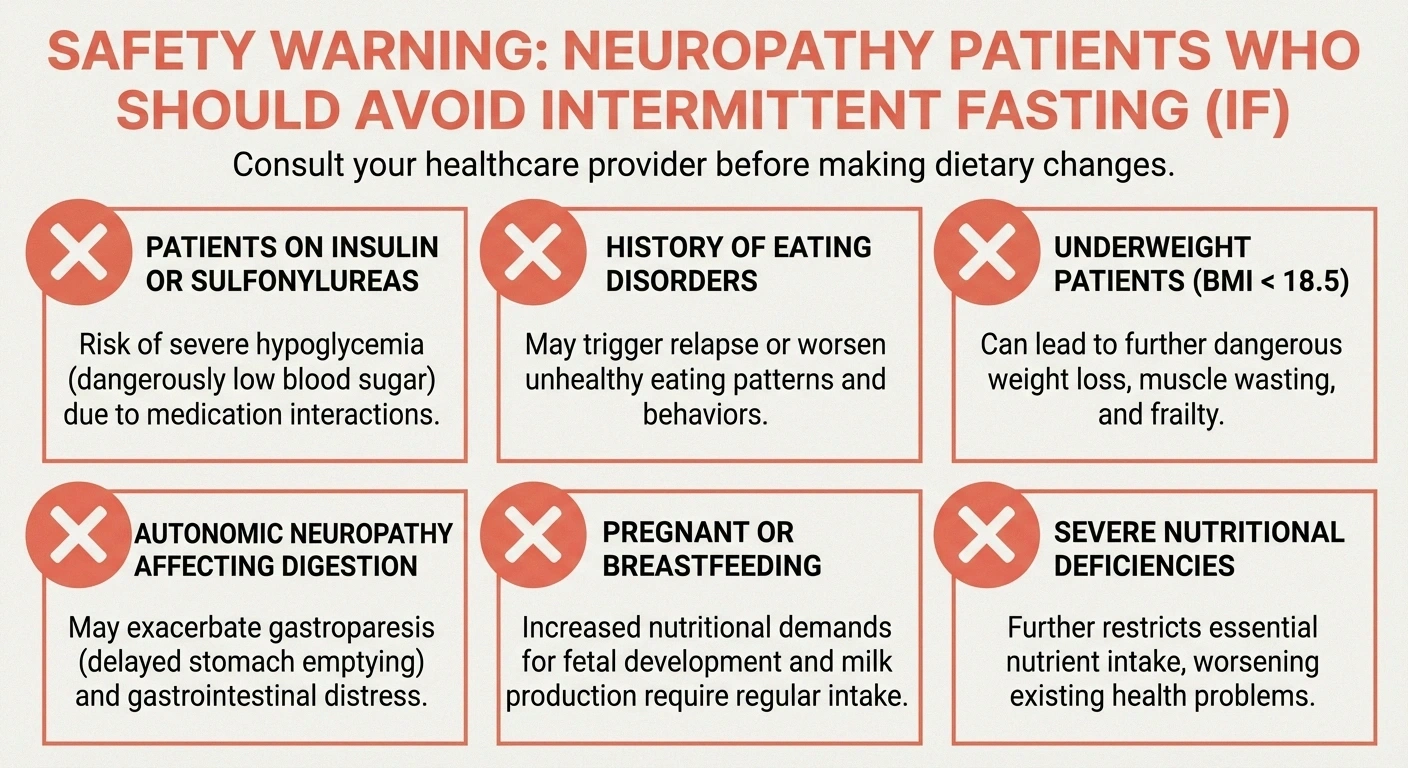
— Patients on insulin or sulfonylureas — hypoglycemia risk is serious
— Anyone with a history of eating disorders — fasting can trigger or worsen disordered eating patterns
— Patients who are underweight or experiencing unintended weight loss
— People with autonomic neuropathy affecting digestion — delayed gastric emptying already disrupts eating patterns, and adding fasting windows adds complexity
— Pregnant or breastfeeding women
— Anyone experiencing severe nutritional deficiencies that need aggressive correction
The Bottom Line
The research on intermittent fasting and neuropathy is genuinely interesting but still in its early stages. Animal studies show promising mechanisms — particularly the gut-nerve connection through IPA and the Klotho gene pathway — but the one human study that specifically looked at nerve function found no benefit. The science isn't settled.

What we can say is that IF may offer indirect benefits for neuropathy through improved blood sugar control, reduced inflammation, and enhanced cellular cleanup (autophagy). These are real mechanisms that could support nerve health as part of a broader management strategy.
But IF is not a cure for neuropathy, it carries real risks for certain patients (especially those on diabetes medications), and the slimmer's palsy risk means aggressive fasting protocols are genuinely dangerous for people with compromised nerves.
If you're interested, the safest approach is to talk to your doctor, start slowly with a 12:12 pattern, prioritize nutrition during eating windows, monitor your symptoms, and view IF as a potential complement to — never a replacement for — your established neuropathy management plan.
Frequently Asked Questions
Can intermittent fasting help with neuropathy?
Animal studies show promising results, including a 2022 Nature study where IF enhanced nerve regeneration by 50 percent in mice through gut bacteria changes. However, a human trial using a fasting-mimicking diet found no significant improvement in nerve function after 6 months. The science is promising but unproven in humans. IF may offer indirect benefits through improved blood sugar control and reduced inflammation.
What is IPA and how does it relate to nerve repair?
IPA (3-Indolepropionic acid) is a metabolite produced by gut bacteria, specifically Clostridium sporogenes. The 2022 Imperial College London study found that intermittent fasting increased IPA production, and that IPA enhanced nerve regeneration in mice. Researchers showed that giving IPA directly produced similar nerve repair benefits even without fasting, suggesting IPA is the active ingredient in the fasting-nerve connection.
Is intermittent fasting safe for people with diabetic neuropathy?
It depends on your medications. If you take insulin or sulfonylureas, fasting significantly increases the risk of dangerously low blood sugar and should only be attempted under close medical supervision. If you manage diabetes through diet, metformin, or other medications with lower hypoglycemia risk, IF may be safer but still requires your doctor's guidance. Start gradually and monitor blood sugar closely.
What is slimmer's palsy and should I be concerned?
Slimmer's palsy is nerve damage, specifically peroneal nerve palsy, caused by rapid weight loss. When protective fat around the nerve near the knee is lost too quickly, the nerve can be compressed, leading to foot drop. This risk is associated with aggressive, rapid weight loss rather than moderate fasting protocols. Neuropathy patients should aim for gradual weight loss of no more than 1 to 2 pounds per week and contact their doctor if they notice new weakness or foot drop.
Which intermittent fasting protocol is best for neuropathy patients?
No specific IF protocol has been proven best for neuropathy in humans. The 16:8 protocol (eating within an 8-hour window) was used in the Klotho gene mouse study and is generally considered the most practical and well-tolerated approach. Starting with 12:12 and gradually narrowing to 16:8 allows your body to adapt safely. Avoid extreme fasting protocols like extended water fasts.
Will intermittent fasting interfere with my neuropathy medications?
Fasting can affect the absorption and timing of some medications. Gabapentin and pregabalin are typically taken with food and may need timing adjustments. Duloxetine should be taken with food to reduce stomach upset. Blood pressure medications combined with fasting may cause excessive drops in blood pressure and increase fall risk. Discuss any fasting plans with your doctor and pharmacist to adjust medication timing as needed.
Should I take supplements while intermittent fasting with neuropathy?
If fasting reduces your overall food intake, supplementation becomes more important to prevent nutritional deficiencies that can worsen neuropathy. B vitamins, particularly B12, are essential for nerve health and should be maintained. Discuss with your doctor whether supplements for magnesium, alpha-lipoic acid, or other nerve-supporting nutrients are appropriate during your fasting regimen. Take supplements during your eating window for best absorption.


